8 Complications
Accidents and complications are a part of clinical practice and reality in all aspects of dentistry (Annibali, Ripari, et al. 2009). A primary challenge for practitioners is to provide care to patients with the least degree of risk in an effort to achieve the highest possible functional and esthetic outcome (Dawson, Chen, et al. 2009). Patients entrust clinicians to achieve this using techniques, biomaterials, and evidence-based scientific therapy that are both time- and cost-effective. Long-term research has shown that implant dentistry, when performed with appropriate expertise and risk assessment, can yield significant success rates for replacing missing teeth; however, implant dentistry is not without risk for accidents and complications (Buser, Mericske-Stern, et al. 1997). An accident is defined as an event that occurs during a surgical or restorative procedure, while a complication is a pathologic condition that appears post-operatively. Surgical accidents can affect the soft tissues, blood vessels, nerve trunks, sinuses, and adjacent teeth. Accidents may also involve the creation of dehiscence/fenestration defects; fractured, ingested, or inhaled instruments; and overpreparation of the osteotomy leading to the lack of primary stability (Figure 8.1). Surgical complications may result in mucosal disturbances, loss of osseointegration, technical challenges related to the restoration process, and short-/long-term esthetic and phonetic outcomes (Figure 8.2) (Adell, Lekholm, et al. 1981; Balshi 1989). Early complications following a surgical procedure can result in infections, edema, ecchymosis, hematomas, emphysema, bleeding, flap dehiscences, and sensory disorders. Late complications may consist of perforations of the mucoperiosteum, maxillary sinusitis, mandibular fractures, failed osseointegration, infraboney defects, periapical implant lesion, and peri-implantitis (Figures 8.3–8.5). Clinicians who elect to perform implant surgery must be prepared to confront these various accidents and complications when they occur. Quite often, continuing education courses designed to train dentists to perform implant surgery focus more on the technique aspect of the surgical procedure and spend little if any time on accidents and complications (Mattheos, Albrektsson, et al. 2009). It is for this reason that immediate implant placement should be limited to advanced and master-level surgeons, as the treatment site can frequently present with unanticipated challenges.
Figure 8.1 Panoramic radiograph of implant “lost” into the maxillary sinus.
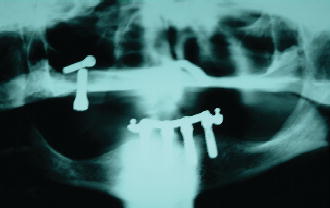
Figure 8.2 Radiograph of implant placed into the root of an adjacent premolar.
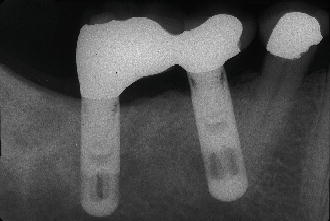
Figure 8.3 Buccal view of an implant replacing tooth #11 resulting in a fistula at the mucogingival junction.
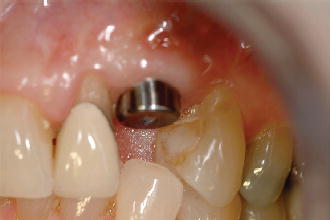
Figure 8.4 Buccal view of implants replacing teeth #24 and #25 resulting in mucositis.
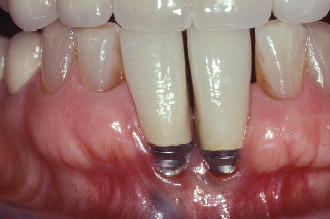
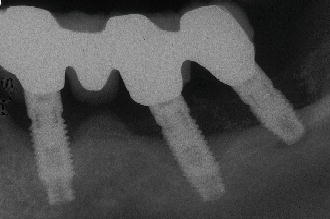
Figure 8.5 Radiograph of implants failing due to peri-implantitis.
As with early, delayed, and late placement, the immediate placement protocol can present the clinician with the aforementioned accidents and complications. A review of the most frequently encountered issues will be described and solutions provided when possible.
NERVE AND BLOOD VESSEL INJURIES
One of the challenges with the immediate placement of dental implants into an extraction socket is obtaining primary mechanical stability. When the morphology of the site is wide, as is frequently encountered with mandibular molar and premolar sites, the osteotomy must provide the stability using intact bone apical to the root apex. It is imperative to have an accurate radiograph (periapical or CT) to locate the position of the inferior alveolar nerve and/or mental nerve. Local anesthetic should be administered as infiltration, not block, and an effort should be made to remain 2 mm coronal to the inferior alveolar nerve during the osteotomy preparation. Failure to do this may result in transient or permanent parasthesia of the mental area.
Blood vessel injuries are frequently encountered in the mandibular molar or incisor areas during the osteotomy procedure. Lingual undercuts of the mandible may not be recognized during the surgery and the lingual plate can become perforated, leading to injury to the lingual artery. This is a potential life-threatening event, and the clinician will require the expertise to address the initial hemorrhage and possible airway management concerns until the patient can be transported to the hospital.
DEHISCENCE/FENESTRATION DEFECTS
Fenestration and/or dehiscence defects are routinely encountered with the placement of immediate dental implants (Figures 8.6 and 8.7) (Zitzmann, Scharer, et al. 1999). The periodontal literature has shown that naturally occurring defects along the facial bone plate are quite common, especially with maxillary and mandibular cuspids (Rupprecht, Horning, et al. 2001). Certainly the fenestration defects are the result of a thin buccal plate and/or prominent root surface, while dehiscence defects may be the result of root/crown angulation toward the labial. Dehiscence defects may also occur due to periodontal disease, treatment of cervical caries, and the presence of a thin phenotype. Both fenestration and dehiscence defects may be the result of surgical trauma that occurs iatrogenically during the extraction or osteotomy process. When extracting a tooth with a thin labial plate, the clinician must attempt to initially use a scalpel blade or periotome to separate the root surface from the attachment fibers. The temptation to luxate the tooth using a buccal-lingual vector with a forceps should be avoided, and instead, a rotational movement as described in a previous chapter should be employed. On very difficult extractions one may wish to section the tooth to lessen the forces upon the labial plate and reduce the possibility of creating a dehiscence defect.
Figure 8.6 Buccal view of fenestration defect following tooth extraction.
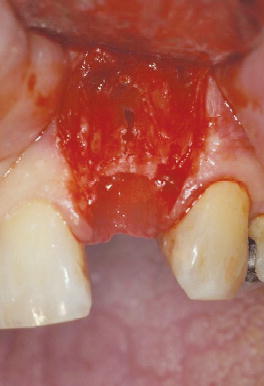
Figure 8.7 Occlusal view of the thin labial boneplate.
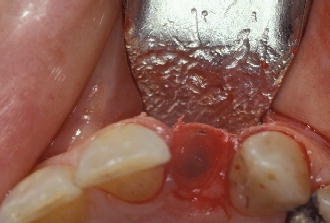
Fenestration defects are more commonly experienced in the maxillary arch/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


