5 Extraction Site Healing
Clinicians who embark on the reconstruction of partially and fully edentulous patients utilizing dental implants must have a thorough understanding of wound healing following the loss of a tooth. It is widely accepted that a three-dimensional alteration of the bone and associated soft tissues occurs following a tooth extraction (Carlsson, Bergman, et al. 1967; Atwood and Coy 1971). This finding implies that the replacement of the lost root with an endosseous dental implant may result in a non-desirable functional or esthetic outcome if the bone architecture is not properly evaluated prior to implant surgery (Figures 5.1 and 5.2) (Iasella, Greenwell, et al. 2003). Knowledge concerning the stages of wound healing following an extraction will help guide the surgeon in the necessary critical thinking required when determining if a site should be treated using an immediate, early, or delayed implant approach (Chen, Wilson, et al. 2004). With this end in mind, numerous “classic” articles have been published using animal research and human biopsies to create a scaffold of knowledge regarding wound healing, bone resorption, regeneration, and remodeling of the extraction socket.
Figure 5.1 Buccal view of poor implant placement due to inadequate bone architecture.
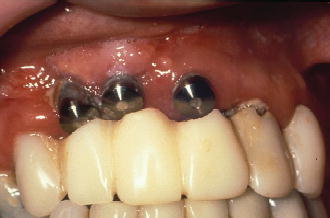
Figure 5.2 Buccal view of final restoration of implants placed into sites with inadequate bone architecture.
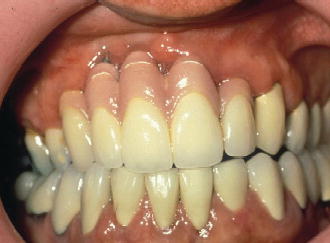
ANIMAL STUDIES
Much of the detailed information regarding wound healing has been derived from animal studies. Animal studies provide us an opportunity to histologically assess a mathematical “time lapse” sequence of events not possible to control with humans. Quite often, these studies provide a control to compare to sites deemed experimental. The control sites typically allow for an unblemished extraction socket to compare to one treated with a bone graft and/or dental implant. An assessment of the literature shows a rather consistent outcome of the histological events that occur following tooth extraction, particularly in the dog model (Cardaropoli, Wennstrom, et al. 2003; Araujo and Lindhe 2005). Following the extraction of a tooth, five stages of healing occur (Amler, Johnson, et al. 1960). Initially, a blood clot forms as a coagulum of red and white blood cells, derived from the circulation. During the second stage, the clot is replaced over a 4- to 5-day period with granulation tissue. During this time, endothelial cells are associated with budding capillaries. From days 14 to 16, the third stage consists of the granulation tissue being replaced by connective tissue. Spindle-shaped fibroblasts, collagen fibers, and a metachromatic ground substance comprise the connective tissue.
Osteoid calcification commences at the apex and lateral walls of the socket during the fourth stage of healing, seen within an additional 7–10 days. By the sixth week, the socket is almost completely filled by bone trabeculae. During this time, maximum osteoblastic activity is occurring but subsides after the eighth week. The fifth stage is characterized by the completion of epithelial closure of the socket, occurring between 24 and 35 days. From weeks 5 to 10, substantial bone fill occurs, being completed at week 16.
Animal studies have also given us insight into the histologic events that occur as the internal and external dimensions of the socket change during wound healing. The information extrapolated from this data has a direct correlation to treatment planning of dental implants, especially relative to the desired prosthetic result compared to implant position. These dimensional changes occurring in the dog model for extraction sites have been described with regards to rate and dimensional direction through histologic observations (Araujo and Lindhe 2005; Araujo, Sukekava, et al. 2006). During the first week of healing, the marginal portion of the lingual boney wall of the socket is markedly wider than the buccal wall (Figure 5.3). Both walls contain large numbers of well-defined bone marrow spaces, with the inner surfaces of the socket walls lined with bundle bone. It has been observed that at week 1, the buccal bone crest is made exclusively of bundle bone, while the lingual crest is comprised of a mixture of cortical bone and bundle bone. During this time, the height of the buccal wall is more pronounced than that of the lingual plate by >1 mm. Histologically, large numbers of osteoclasts are observed along the outer surface of the buccal and lingual crest walls. Also during week 1, the internal portion of the extraction socket is comprised of coagulum, granulation tissues, provisional matrix, and small amounts of newly formed bone, seen in the most apical portion of the socket. At this time sequence, the provisional matrix is the dominant tissue, consisting of fibroblasts, new vessels, and collagen fibers.
Figure 5.3 Histology showing 1 week of healing. Reprinted from Araujo, M. G., and J. Lindhe (2005). “Dimensional ridge alterations following tooth extraction: An experimental study in the dog.” J Clin Periodontol 32(2): 212–218, with permission from John Wiley & Sons, Inc.
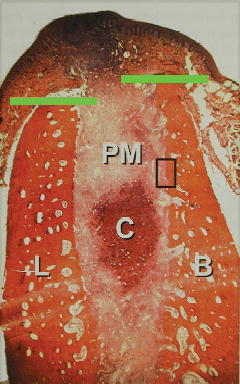
During the second week of wound healing, the crestal region of the lingual bone wall is absent of bundle bone, while the corresponding region of the buccal bone wall continues to have bundle bone present (Figure 5.4). Osteoclasts continue to be observed in the crestal region of both bone walls, as well as areas apical to the crest. As large amounts of newly formed bone are noted in the apical and lateral aspects of the socket, the provisional matrix continues to survive in the central and marginal compartments. The second week is also noted for the absence of the periodontal ligament. The remaining bundle bone is seen in direct continuity of the woven />
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


