7
Additional anaesthetic techniques
In dentistry, infiltration anaesthesia of the maxillary nerve (Chapter 5) is mainly used for anaesthetising the teeth and surrounding tissues of the upper jaw. In the lower jaw, block anaesthesia of the mandibular nerve (Chapter 6) is usually applied. In this chapter, several supplementary anaesthetic techniques are discussed, such as regional block anaesthesia of the maxillary, infraorbital, nasopalatine and mental nerves. The Gow-Gates technique, an alternative to mandibular block anaesthesia, is also described.
7.1 Maxillary nerve block
Blockade of the maxillary nerve induces anaesthesia of half of the maxilla, which enables surgical treatment in the upper jaw and maxillary sinus under local anaesthesia. This regional block can also be used to counteract pain in cases of inexplicable pain complaints. A maxillary nerve block can be achieved via high tuberosity anaesthesia or via the greater palatine foramen. A local anaesthetic with vasoconstrictor is used, applied with an aspirating syringe and a 25-gauge needle (bent at approximately 45 degrees).
7.1.1 High tuberosity anaesthesia
The maxillary nerve leaves the skull through the foramen rotundum. The nerve runs through the pterygopalatine fossa and then on through the orbit as the infraorbital nerve. The infraorbital nerve runs through a canal at the bottom of the orbit and leaves the canal again through the infraorbital foramen.
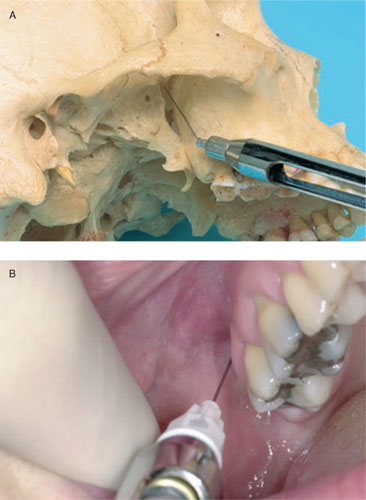
The pterygopalatine fossa is accessible from the mouth. This fossa can be reached with a 35-mm-long 25-gauge needle if the needle is bent to approximately 45 degrees. This bent needle must pass the mucosa behind the zygomaticoalveolar crest, about 1 cm from the alveolar process, and then be directed dorso-medially (Figure 7.1). After aspiration, about one cartridge may be injected. Two to three minutes later, half of the upper jaw will be anaesthetised. In some cases the infraorbital nerve is insufficiently numbed by this technique. Furthermore, there is a chance of injecting into the pterygoid plexus, so that there is a risk of intravasal injection and developing a haematoma.
Figure 7.1 A and B Photos of skull (A) and patient (B) show a high tuberosity anaesthesia. The (bent) needle is inserted from out to in, high in the pterygopalatine fossa, just by the split of the maxillary nerve into the infraorbital and superior alveolar nerves. The injection is given after aspiration.
7.1.2 Greater palatine foramen block
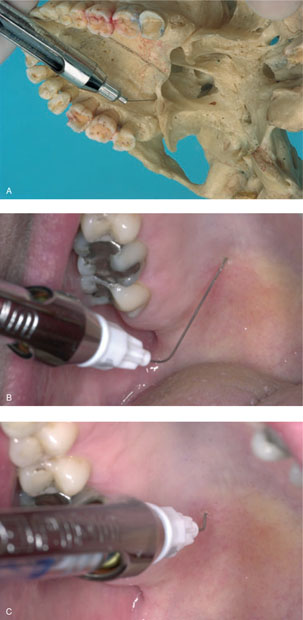
A greater palatine foramen block is used less frequently than high tuberosity anaesthesia, but can be easily carried out intraorally. The greater palatine foramen lies approximately 1 cm palatinally to the M2–M3 region and approximately 0.5 cm in front of the pterygoid hamulus. The direction of the canal is 45 degrees to dorsal in relation to the occlusion plane. The bent needle is carefully inserted into the foramen, and by inserting the needle slowly, the entire length of the needle can be used (Figure 7.2). After aspiration, a half to one cartridge may be injected. Within 2–3 minutes, half of the maxilla will be anaesthetised.
Figure 7.2 A, B and C Photo of skull (A) and photos of patient (B and C) show a maxillary nerve block via the greater palatine foramen. The needle is bent approx. 45 degrees and inserted in the foramen, which is located approx. 1 cm palatinal to the M2–M3 region. The cartridge syringe is held parallel to the occlusion plain of the upper jaw. The needle can now be pushed in carefully. The injection is performed after aspiration.
It is not always easy to find the entrance to the foramen. Moreover, inserting the needle roughly can lead to long-term damage of the nerve. Finally, if the patient has a small maxilla, the anaesthetic fluid may reach the parasympathetic sphenopalatine ganglion so that unintended side effects may occur, such as diplopia (double vi/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


