CHAPTER 6
Swelling
• Pleomorphic salivary adenoma
• Paget’s disease (osteitis deformans)
• Fibroepithelial polyp (focal fibrous hyperplasia, irritation fibroma)
• Drug-induced gingival hyperplasia
• Focal epithelial hyperplasia (Heck’s disease)
• Denture-induced hyperplasia (denture granuloma)
• Pyogenic granuloma (pregnancy epulis)
• Peripheral giant cell granuloma (giant cell epulis)
• Infective warts (verruca vulgaris, condylomata acuminata)
General approach
• Swelling of the orofacial tissues may be due to trauma, infection, immune reactions, or neoplasia.
• Chronic swellings of the oral tissues are usually painless.
• Swelling may be extraoral, intraoral, or at both sites.
• Differentiation of intraoral swelling may be achieved on the basis of the presence of ulceration and the color of the lesion.
The causes of extra- and intraoral swelling are given in Tables 5 and 6.
Table 5 Causes of extraoral swelling
• Viral sialadenitis
• Bacterial sialadenitis
• Sialosis
• Ranula
• Salivary gland tumor
• Squamous cell carcinoma
• Crohn’s disease
• Orofacial granulomatosis
• Paget’s disease
• Fibrous dysplasia
• Acromegaly
Table 6 Causes of intraoral swelling
Pink
• Fibroepithelial polyp
• Drug-induced hyperplasia
• Warts and condylomata
• Focal epithelial hyperplasia
• Crohn’s disease
• Orofacial granulomatosis
• Squamous cell carcinoma
• Salivary gland tumor
• Lymphoma
Red
• Denture-induced hyperplasia
• Pyogenic granuloma
• Giant cell granuloma
• Squamous cell carcinoma
• Scurvy
White
• Squamous papilloma
• Squamous cell carcinoma
Blue
• Mucocele
• Ranula
Yellow
• Sialolith
• Bone exostosis
• Lipoma
Viral sialadenitis (mumps)
ETIOLOGY AND PATHOGENESIS
Mumps represents an acute viral sialadenitis predominantly involving the parotid glands, although other glands may be affected. Infection is caused by a paramyxovirus that is highly infectious and transmitted by saliva. A 2–3 week incubation period precedes the clinical symptoms.
CLINICAL FEATURES
Mumps mostly occurs in childhood but may occasionally develop in adults. The principal manifestations are fever, malaise, headache, chills, and pre-auricular pain with swelling. Approximately 75% of patients have bilateral parotid gland disease (246). The swelling is maximal 2–3 days after the onset of clinical symptoms, with most of the swelling disappearing 10 days later. Since mumps is a systemic infection, other organs can be involved including the gonads, liver, pancreas, and kidneys. Orchitis and oophoritis in adulthood is a serious complication since it can lead to sterility.
DIAGNOSIS
Most cases can be diagnosed on a clinical basis. When there is doubt, the diagnosis can be confirmed by the demonstration of raised serum antibodies to S and V antigens of the paramyxovirus. Antibody to the S antigen disappears shortly after infection but antibody to the V antigen persists and may be used as a marker of previous infection. The virus can also be cultured from the saliva.
MANAGEMENT
Treatment is symptomatic, consisting of rest, fluids, and analgesia (acetaminophen, paracetamol). An effective vaccine given to children has significantly reduced the number of cases of mumps. Aspirin is not recommended in children. Adults who develop gonad involvement should be given in the region of 40 mg of oral prednisolone (prednisone) daily for 4 days, which is then gradually reduced.
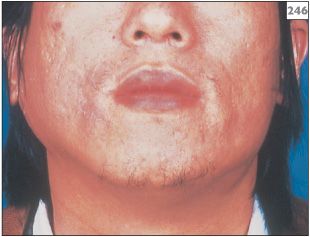
246 Bilateral swelling of the parotid glands in mumps.
Bacterial sialadenitis
ETIOLOGY AND PATHOGENESIS
Any cause of reduced salivary flow can permit the retrograde infection of a major salivary gland with members of the commensal oral microflora. Dehydration following major surgery was formerly an important predisposing factor for bacterial sialadenitis, but improved understanding of fluid balance has almost eliminated this complication. Traditionally, the microorganisms encountered in this infection have been Staphylococcus aureus, Streptococcus viridans, and Streptococcus pneumoniae. However, more recently it has become apparent that strictly anerobic bacteria are also involved.
CLINICAL FEATURES
The affected gland is painful, swollen (247), and tender to touch with a purulent discharge from the duct orifice (248, 249). The overlying skin may be erythematous and the patient will have fever and malaise.
DIAGNOSIS
Diagnosis is made based on the history and clinical findings. Rarely, a child may be found to have suffered repeated episodes of acute sialadenitis in one parotid gland, a condition known as recurrent parotitis of childhood (250). This unusual diagnosis can be confirmed by sialography, which will show multiple sialectasis within the parotid gland (251).
MANAGEMENT
Management should consist of empirical antibiotic therapy with beta-lactamase activity, such as flucloxacillin, clindamycin, or metronidazole. If possible, a sample of pus should be collected from the duct orifice by aspiration. In the acute phase the patient will gain pain relief from provision of an NSAID. A dehydrated patient should be rehydrated and the fluid balance established. Once the acute symptoms have resolved, a sialogram should be performed to determine the presence of any structural abnormality within the affected gland. Each episode of infection in the situation of recurrent parotitis of childhood should be managed individually. Interestingly, this rare condition resolves after puberty.
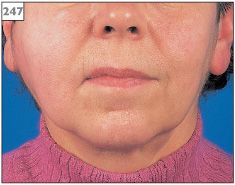
247 Swelling of the right parotid gland.
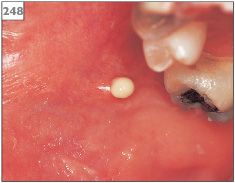
248 Purulent discharge from the parotid duct orifice.
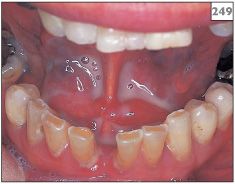
249 Pus draining from the left submandibular gland duct orifice into the floor of the mouth.
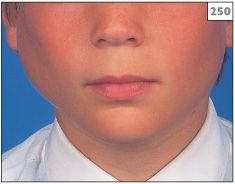
250 Swelling of the left parotid gland of a boy with recurrent parotitis of childhood.
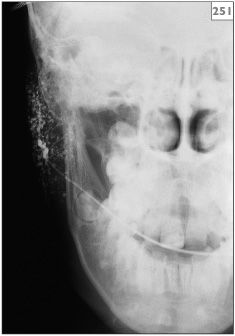
251 Sialogram showing multiple sialectasis characteristic of recurrent parotitis of childhood.
Sialosis (sialadenosis)
ETIOLOGY AND PATHOGENESIS
This condition represents a noninflammatory, non-neoplastic swelling of the major salivary glands, principally the parotid glands. The etiology is poorly understood, although a number of conditions have been implicated in the possible cause. Factors associated with sialosis include alcohol abuse, cirrhosis, diabetes, anorexia, and bulimia.
CLINICAL FEATURES
Sialosis presents with a painless bilateral enlargement of the parotid glands (252, 253).
DIAGNOSIS
Diagnosis is made on the clinical findings and history. Biopsy is not required, although if undertaken it reveals hypertrophy of the serous acini and edema of the interstitial connective tissue. Hematological investigations should be undertaken to exclude other causes of chronic swelling of the parotid glands.
MANAGEMENT
Once diagnosed, no active treatment is required.
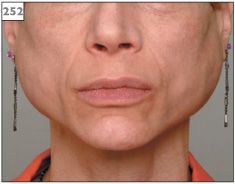
252 Bilateral parotid gland swelling in association with bulimia.
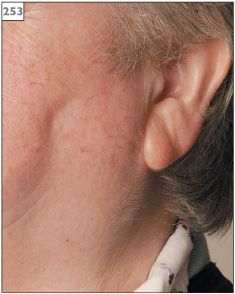
253 Sialosis of the left parotid gland. The ear lobe is characteristically displaced in an upwards direction.
Mucocele and ranula
ETIOLOGY AND PATHOGENESIS
An accumulation of mucus either in the connective tissues or within a salivary duct is clinically termed a mucocele (Chapter 3, p. 54) and encompasses both mucous extravasation phenomenon and mucous retention cysts. The mucous extravasation phenomenon is the result of trauma or transection of a salivary duct, leading to mucus spillage into the connective tissues with resultant granulation tissue response. A mucous retention cyst may be the result of duct obstruction secondary to a salivary stone, scarring, or an adjacent tumor.
CLINICAL FEATURES
Mucocele may develop at any oral site but presents most frequently as a bluish fluid-filled sessile mass just below the mucosa of the lower lip. Blockage of the submandibular or sublingual gland duct may cause a large mucocele in the floor of the mouth, with external swelling. Such a mucocele is sometimes termed a ranula after a suggested resemblance to a frog’s belly and the Latin term for frog (254, 255). A plunging ranula is the result of herniation of the lesion through the mylohyoid muscle and along the fascial planes of the neck. These can present as midline masses in the neck and, rarely, in the mediastinum.
DIAGNOSIS
Diagnosis of mucocele is made on the history and examination. Excisional biopsy including the adjacent minor salivary glands is curative and diagnosis of either extravasation or retention is confirmed by the histopathological findings. Imaging using ultrasound, CT, or MRI of the floor of the mouth and the neck may be needed to determine the extent of a ranula.
MANAGEMENT
Mucoceles are treated by surgical excision to include the lesion and the adjacent minor salivary glands. Aspiration produces no lasting benefit since the adjacent salivary glands will quickly refill the mucocele. The surgical site is frequently left to heal by secondary intention to minimize the chance of recurrence. Cryotherapy may be used to treat mucoceles in children, although there is a possibility of recurrence.
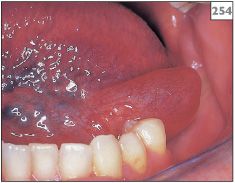
254 Mucocele in the floor of the mouth.
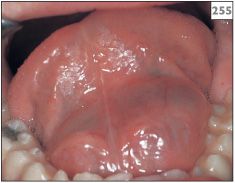
255 Large mucocele (ranula) in the floor of the mouth.
Pleomorphic salivary adenoma
ETIOLOGY AND PATHOGENESIS
Salivary gland tumors are relatively rare and usually present as swelling. The majority (85%) of salivary tumors affect the major glands, with almost 90% of these arising in the parotid gland.
Pleomorphic salivary adenoma (PSA) (also known as pleomorphic adenoma or mixed tumor) is a benign tumor and the most common neoplasm of both the major and minor salivary glands. Approximately 75% of all tumors arising in the parotid gland are PSA. The etiology of PSA is unknown but pathological features suggest that it is derived from the neoplastic transformation of salivary acinar-type cells and myoepithelial cells.
CLINICAL FEATURES
PSA presents as a firm, lobulated mass either extraorally within a major gland (256) or intraorally from minor gland tissue (257). The overlying mucosa or skin appears similar to the adjacent tissues. Lesions are slow growing and painless, ranging in size from a few millimeters to several centimeters. Within the mouth, the majority of these tumors are located in the palate, the buccal mucosa, or the upper lip.
DIAGNOSIS
Diagnosis is established on histopathological examination of biopsy material, which will show bi-layered duct structures composed of neoplastic acinar cells variably mixed with myoepthelial cells and a stroma ranging from hyaline material to cartilage and bone. Imaging studies, such as ultrasound, CT, or MRI, are often necessary to determine the extent of the disease, particularly when PSA occurs within a major salivary gland.
MANAGEMENT
Surgical excision is the treatment of choice. Enucleation is not an acceptable therapy since small fingers of tumor that are located within and outside the tumor capsule are left behind and contribute to recurrence. Incomplete excision is the most important factor related to tumor recurrence. Malignant change, referred to as carcinoma ex-PSA, can occasionally occur in untreated long standing PSA.
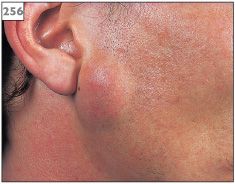
256 Pleomorphic salivary adenoma in the parotid gland.
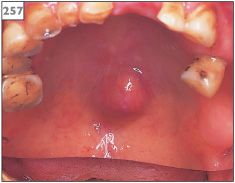
257 Pleomorphic salivary adenoma in the palate.
Adenoid cystic carcinoma
ETIOLOGY AND PATHOGENESIS
Malignant salivary gland tumors are also rare. The etiology of malignant salivary gland tumors is unknown but for some, such as adenoid cystic carcinoma, the tumor is derived from the neoplastic transformation of salivary acinar-type cells and myoepithelial cells. Overall, the most common malignant salivary gland tumor is a mucoepidermoid carcinoma, a tumor with a range of clinical behavior from indolent to clinically aggressive. Adenoid cystic carcinoma accounts for only 25% of carcinomas occurring in the salivary glands but comprises the majority (50–70%) of all neoplasms arising in the minor salivary glands.
CLINICAL FEATURES
Within the mouth, adenoid cystic carcinoma presents most frequently as a firm, painless swelling in the palate (258, 259), possibly with superficial ulceration. When adenoid cystic carcinoma develops in the parotid gland, the fixed discrete swelling is often associated with facial nerve palsy.
DIAGNOSIS
Diagnosis is established by biopsy. Adenoid cystic carcinoma is composed of bilayered duct-like structures in a cribriform pattern. The tumor is unencapsulated showing wide infiltration of adjacent tissues including nerves. Once diagnosed, imaging studies involving CT or MRI are required to determine the extent of the tumor. In the case of large lesions in major glands, such imaging or ultrasound is likely to be performed prior to the biopsy.
MANAGEMENT
Adenoid cystic carcinoma is notoriously difficult to treat successfully. Surgery involving a wide margin is the treatment of choice. In the parotid gland, parotidectomy is performed with the sacrifice of the facial nerve if involved. Postoperative radiotherapy may be used in some situations. Chemotherapy plays little or no role in the management of this condition. The 5-year survival rate is about 70%, although the 15-year survival rate is only 10%. This outcome probably reflects the slow but relentlessly infiltrative growth and perineural spread of this tumor.
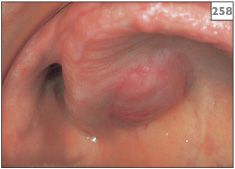
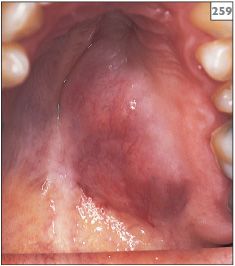
258, 259 Swelling of the palatal tissues due to adenoid cystic carcinoma. The overlying mucosa is normal suggesting that the origin of the lesion is within the underlying tissues.
Squamous cell carcinoma
ETIOLOGY AND PATHOGENESIS
Tobacco and alcohol use remain the two most important risk factors associated with the development of oral SCC (Chapter 2, p. 30).
CLINICAL FEATURES
SCC has no characteristic appearance and can present with a variety of clinical signs including swelling, white patch (Chapter 4, p. 86), red patch (Chapter 5, p. 110), or ulceration (Chapter 2, p. 30). Fixation to underlying tissues is a feature common to all forms. A large SCC within the mouth may produce obvious extraoral swelling (260). If metastasis has occurred, the regional lymph nodes may be palpable or visibly enlarged (261). SCC of the lip can present as a firm swelling that is palpable within the tissues (262–264). Intraorally, SCC can develop as a swelling at any site, although most frequently in the floor of the mouth, the tongue, and the retromolar region (265–267 overleaf). The gingivae (268–270 overleaf). and the buccal mucosa) are relatively rare sites for SCC.
DIAGNOSIS
/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


