Chapter 6
Septal flap
Introduction
The septal flap is a commonly used flap due to its arc of rotation and the quantity of tissue available for use as a lining in nasal reconstruction. In cases where there is a full thickness defect of the nose, the reconstruction of the defect should attempt to restore each of the missing layers and, whenever possible, matching tissues. In these cases, a septal pivot flap or mucoperichondrial flap is exceptionally useful in providing good tip support and a well-vascularized nasal lining for reconstruction after major resection of the nasal tip.1
The use of the septal flap is often carried out in stages. The flap is rotated to reconstruct the defect, but by doing this it obliterates the nasal airway. In the second stage, carried out several weeks later, the nasal passage is opened by separating the mucosa from its pivot point in the septum.
In cases where the defect is limited to the nasal lining, raising the flap is technically more demanding due to the confined space. The challenge centers on diminishing the likelihood of perforations to the mucoperichondrial flap. In these cases, it is recommended that the surgeon be facile with endonasal procedures, preferably with endoscopic harvest.
This nasoseptal flap has become one of the most utilized flaps in the reconstruction of anterior skull base defects. The technique for endoscopic harvest of the flap was described by Hadad and Bassagasteguy in 2006 and is named after them.2 This technique will not be discussed in this chapter.
The septal pivot flap is a modification that transfers both mucosal septal components as well as the interpositioned cartilage. This flap is most commonly used in situations where the anterior nasal tip and columella are missing. These defects are often encountered secondary to trauma, principally gunshot wounds, or due to oncologic resection. These acquired defects pose a significant challenge to the reconstructive surgeon charged with rebuilding the nasal complex.
The septal pivot flap enables the restoration of the projection of the nose as well as the support of the reconstructed nose. When an adequate quantity of the septum and the perfusion is intact, use of this flap obviates the need for alloplastic implants and their associated risk of extrusion.
Anatomy
The anatomy of the nasal septum is simple, yet with several critical nuances that are of significant importance to raising the septal mucoperichondrial and septal pivot flaps.
The septum is composed of cartilage anteriorly and bone posteriorly. The bony part of the septum is the perpendicular plate of the ethmoid bone. The septal mucosa on either side is separated by the cartilage, which is covered by the perichondrium. The septum gives the nose support and is responsible for dorsal as well as tip support and the projection of the nose.
The arterial perfusion to the septum consists of an array of vessels. The anterior portion of the septum (i.e., the cartilage) obtains its blood supply from the septal branch of the superior labial artery. The superior labial artery is a branch from the facial artery and it gives off the septal branch lateral to the philtrum and columella.
Branches of the sphenopalatine artery, mainly the posterior septal branch, perfuse the posterior aspect of the septum. The superior aspect is perfused by branches from the anterior and posterior ethmoidal arteries.3
The survival of the cartilaginous portion of the septum is dependent on the perfusion from the mucoperichondrium. The cartilage can survive as long as one of the mucoperichondrial sides is intact.
A flap of septal mucoperichondrium, either unilateral or bilateral and with or without a cartilage component, will survive if based on a 1.3-mm pedicle located in the zone between the anterior plane of the upper lip and the lower edge of the piriform aperture—the zone containing the septal branch of the superior labial artery.4
Flap harvest
Septal mucosal flap
First stage
- In cases where the septal mucosal flap is being used for lining defects in full-thickness nasal defects, access to the septum is often unimpeded.
- The nasal cavity is packed with Afrin-soaked cotonoids to shrink the mucosa while at the same time diminishing the potential bleeding caused by surgical intervention.
- The area to be incised will be dependent on the amount of tissue needed.
- The superior incision is normally carried out along the plane of the nose and parallel to the planned inferior incision.
- The inferior incision is made about 5 mm above the nasal floor and as far posterior as possible.
- The superior incision is then connected to the inferior incision by dropping a perpendicular incision from superior to inferior incision.
- The flap is then elevated by dissecting between the septal mucosa and the cartilage; care should be taken to not perforate the mucosa.
- The elevation is continued posteriorly, avoiding any trauma to the tissues. The flap is then elevated and rotated to the defect.
Second stage
- Approximately 3 weeks after the first stage surgery, the flap should have enough collateral circulation to tolerate the division of the pedicle without compromise of the transferred tissue.
- The takedown of the flap is achieved by making an incision near the septum along the width of the flap.
- The mucosal end of the flap used to line the nose is inset using chromic gut sutures.
- The septal mucosa is also transferred to the septal area and secured with trans-septal sutures.
- Alternatively, a nostril former or nasal packing can be used to keep the flaps in place until adhesion to the transferred bed.
Figures 6.1 to Figure 6.11 depict the steps in raising the septal mucoperichondrial flap.
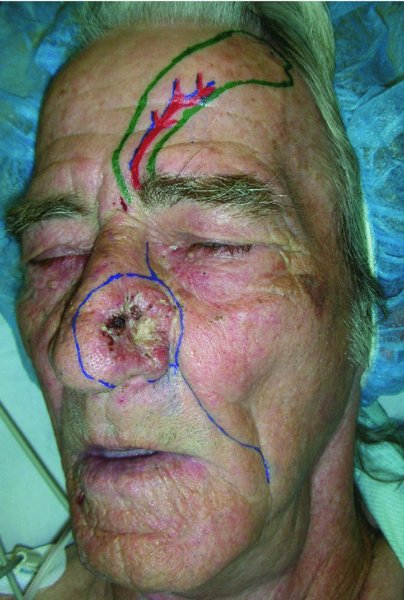
Figure 6.1 Appearance of a large nasal skin cancer with markings for immediate reconstruction.
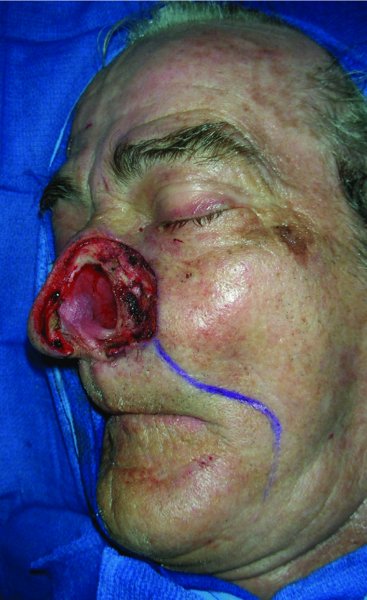
Figure 6.2 View of the resected nasal lesion in the form of a hemirhinectomy.
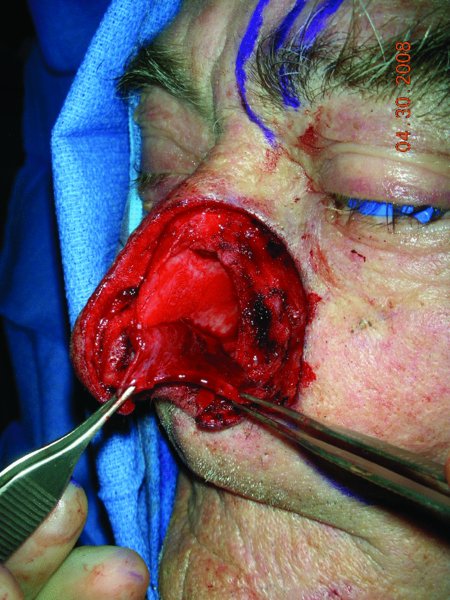
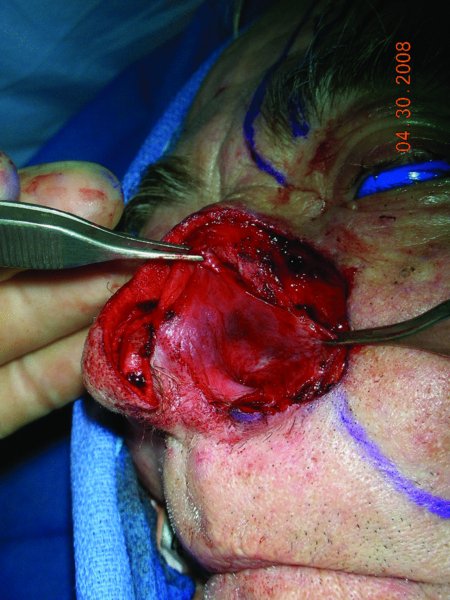
Figure 6.3 Elevated left septal flap.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


