Chapter 14
Submental island flap
Introduction
The submental island flap was first mentioned in the literature by Martin et al., who described this new flap as a good option to reconstruct various defects in the head and neck1. Since this description, the submental island has struggled to gain a strong foothold as a reliable flap in the reconstruction of head and neck defects. Two likely reasons for the slow and reluctant acceptance of this flap into the everyday use by head neck reconstructive surgeons has been the difficult dissection of the flap along the submandibular gland area as well as concern for its use in patients with oral cavity cancers. The latter is due to the belief or fear of potentially transferring nodal disease to the reconstructed site. This concern has not been shown to be valid by the collective experience of most surgeons who routinely use the submental flap.
The submental island flap is a fantastic option for the reconstruction of defects in the head and neck extending from the oral cavity, oropharynx, hypopharynx, maxilla, as well as various sites in the face such as the parotid bed, chin, face, upper and lower lip, and in neck defects.
The main disadvantage of the submental island flap is the dissection of the pedicle near the takeoff of the facial artery and vein as the vessels travel through the submandibular gland. Dissection in this area can be very tedious and a potential site for problems, particularly of the veins leading to venous congestion of the flap.
Overall, this flap is a very reliable option for the reconstruction of small to fairly large defects in the head and neck while still providing the ability to primarily close the donor site. The location of the donor site scar is well hidden, particularly when the patient is standing upright.
Anatomy
The submental artery island flap is a type C fasciocutaneous flap with its dominant pedicle based on the submental artery, which arises approximately 5–6.5 cm from the origin of the facial artery.1 The facial artery has a mean diameter of 2.7 mm at its origin form the external carotid artery. The submental artery emerges from the medial portion of the facial artery 5–7 mm inferior to the mandibular border, 3–5 cm anterior to the mandibular angle and with a mean diameter of 1.7 mm.2 The submental artery arises deep to the submandibular gland and continues forward and medially across the mylohyoid muscle. As it continues its course, the artery gives branches to the submandibular gland, the platysma, digastric and mylohyoid muscles, small branches to the subplatysmal fatty layer, and 1–4 cutaneous perforators.3 These perforators pierce the platysma and terminate in the subdermal plexus connected with the contralateral artery, allowing for skin perfusion of both the ipsilateral and contralateral neck.4 This enables a flap to be raised from the mandibular left angle to the right angle with a width of 7–8 cm and a length of 15–18 cm, a territory of 45 ± 10.2 cm2.5 The submental artery terminates either deep to, superficial to, or within the anterior belly of the digastric and sends branches to the lower lip.6 During flap harvest the ipsilateral anterior belly of the digastric is included, as the artery has been found to lie deep to the muscle in 70% of cases. The pedicle length ranges from 5 to 8 cm giving a significant arc of rotation extending from the medial canthus to the zygomatic arch. The venous drainage is via the submental vein, which has a mean diameter of 2.2 mm. It drains into the facial vein, which has a mean diameter of 2.5 mm. The caliber of the submental vessels, make this flap suitable for microvascular transfer. The sensory nerve supply to this region is via the transverse cervical nerves. Motor innervation is via the cervical branch of the facial nerve. On dissection care must be taken to avoid injury to the marginal mandibular branch of the facial nerve as it can travel a mean of 12 mm away from the submental artery.
Flap harvest
- The first step in the harvest of the submental artery flap is the determination of the amount of skin that can be harvested while allowing for primary closure of the defect. This can be done with a pinch test. The skin inferior to the inferior border of the mandible is pinched to determine the greatest amount of skin which can be taken while allowing for advancement of the remaining neck skin to close to the skin at the inferior border of the mandible.
- Once the skin amount is determined, an elliptical skin island is marked out as needed. The amount of skin can extend laterally to the posterior border of the mandible or the mastoid area.
- If the flap is being raised in conjunction with a neck dissection, the ipsilateral posterior border of the skin island is extended to meet the neck dissection in an apron-type incision.
- A Doppler scan may be used to help determine the trajectory of the pedicle, but this is not necessary.
- Flap raising begins by making the superior skin incision on the distal part of the flap, i.e., on the side away from the pedicle.
- The incision is extended from the skin, the subcutaneous tissue, and to the fascia of the contralateral anterior belly of the digastric. Skin incision is also extended inferiorly towards the ipsilateral aspect of the pedicle.
- Dissection is extended to the midline over the mylohyoid muscle and the ipsilateral anterior digastric muscle.
- The attachment of the anterior digastric muscle is detached from the mandible and it is sectioned inferiorly at the intermediate tendon.
- At this point, dissection is carefully carried out towards the facial artery hugging the inferior border of the mandible where the submental vascular pedicle travels in a transverse horizontal fashion.
- As the dissection approaches the submandibular gland, a subplatysmal flap should be raised to facilitate the inspection and dissection of the pedicle. This portion of the dissection can also be carried out at the beginning of the flap harvest with a circumferential incision and elevation of the subplatysmal flap.
- Taking care to identify the facial vessels and the marginal mandibular branch of the facial nerve, the fascia is elevated superiorly to protect the nerve.
- Dissection in this region approaches the submandibular gland. At this point, dissection should be carried out with a bipolar electrocautery to minimize damage to the vascular pedicle.
- Larger vascular branches of the vascular pedicle should be clipped and divided.
- Once dissection of the pedicle is completed along the submandibular gland, the gland is often removed. At this point, the submental artery and vein are completely dissected to the takeoff at the facial vessels.
Transfer to the oral cavity
- Once the flap pedicle is completely dissected, the flap is ready to be transferred to the oral cavity if that is where the defect is located.
- Prior to the transfer of the pedicle, a tunnel from the neck to the oral cavity must be created.
- The usual transfer to the oral cavity is done by forming a tunnel along the mylohyoid muscle. This dissection can be done from the neck and the tunnel connected to the oral cavity via the resection defect.
- Care should be taken to insure that there is at least ample room to tolerate the pedicle size and so it is not compressed postoperatively as this can interfere with the venous outflow or perfusion.
- Once the tunnel is made, a large Kelly clamp is passed from the oral cavity to the neck. The skin edge of the flap is secured with the Kelly clamp and the flap is gently teased into the oral cavity. Once in the oral cavity, the contour and alignment is oriented for the most effective position and the pedicle in the neck is checked to insure that it is not twisted.
- The flap is then inset and the neck closed over a vacuum drain.
- See Figures 14.1 to 14.10.
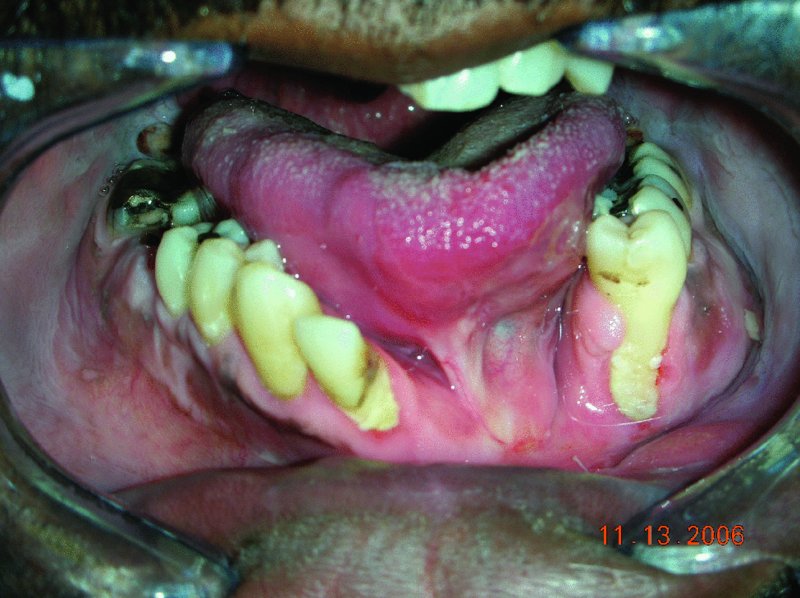
Figure 14.1 Appearance of intraoral scaring in the anterior vestibule secondary to a gunshot/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


