Chapter 13
Cervicofacial advancement flap
Introduction
The cheek is the widest skin expanse of the face and is an important cosmetic and functional unit that provides a platform for crucial midface structures while supporting the lips, nose, and lower eyelids.1 Defects of the cheek region are therefore conspicuous and potentially difficult to reconstruct with minimal evidence of the surgical insult. The first author to describe the cervicofacial flap to tackle complex midface problems was Beare, who in 1969 described the use of this flap for the reconstruction of orbital exenteration defects.2 The cervicofacial flap has also been referred to as the Mustarde flap, or as the cheek Mustarde flap since his publication of the use of the flap to reconstruct large defects in the periorbital region.3 Since then the flap has been described in various forms including a cervicopectoral extension.4–6
Although frequently separated in the literature, and perhaps the lexicon, of reconstructive surgeons, cervicofacial and cervicothoracic (cervicopectoral) flaps represent different degrees of inferior extension for the same flap, allowing flexibility in defect management.7
The advantages of the cervicofacial flap are similar to other local regional flaps in the head and neck in that there is great color match and equal skin texture. The use of this flap enables placement of the scar in an ideal location where it is camouflaged. The use of the cervicofacial flap is made easier in older patients due to the likelihood of redundant tissues and rhytids, which enables the reconstructive surgeon to better hide the final scars.
The use of the cervicofacial or cervicopectoral flap has very few disadvantages. The potential downside of the flap is the increased risk to the branches of the facial nerve if the elevation of the flap is made deeper to the parotidomasseteric fascia. When reconstructing large defects, the superior tip of the flap may develop signs of venous congestion or ischemia and may eventually lead to the loss of that portion of the flap. Some authors have advocated raising the flap deep to the superficial musculoaponeurotic layer to minimize the potential for distal edge ischemia; this is especially recommended in smokers.8
Anatomy
The blood supply to this flap is a random pattern since it is elevated just below the subcutaneous layer. Multiple perforators to the skin arise from the deep facial artery, transverse facial artery, and superficial temporal artery.9 These perforators are sacrificed as the dissection is carried in the subcutaneous layer. A modification of this flap includes the deep plane cervicofacial flap, which carries the dissection below the superficial musculoaponeurotic system (SMAS) in the face and deep to the platysma in the neck. With this design, the flap becomes a myofasciocutaneous flap with an axial blood supply. An anteriorly based flap derives it blood supply from the submental and perforating branches of the facial artery, while a posteriorly based flap receives its supply from perforators of the superficial temporal artery.10–12 An extension of this flap includes a pectoral component, which as a fasciocutaneous flap receives its major supply from the first four internal mammary perforating vessels.13 The venous drainage is mainly through paired vessels, emptying into the anterior and external jugular veins.
Flap harvest
- The head of the patient is rotated towards the contralateral side and the neck is extended to visualize the entire length of the neck.
- The chest is also prepped into the field.
- The anticipated defect is marked and a decision is made on where to base the flap, i.e., anterior or posterior.
- The superior aspect of the flap is extended towards the lateral canthus and slightly superior towards the anterior hairline. The marking is then extended along the pre-auricular region and extended posterior around the earlobe towards the hairline behind the ear and continues inferiorly towards the base of the neck along the anterior aspect of the trapezius muscle.
- If the defect is anticipated to be very large, the extension can be carried just above the nipple areolar complex.
- The patient is prepped and draped in the usual fashion and the resection is carried out.
- The elevation of the flap begins by making the incision along the previously marked flap outline.
- The flap is raised in the subcutaneous plane and extended towards the defect site. In the facial region, the flap is elevated superficial to the superficial musculoaponeurotic system (SMAS).
- As the dissection is carried out below the inferior border of the mandible, the dissection is transitioned below the platysma muscle.
- Flap elevation is stopped once adequate rotation of the flap is achieved to repair the defect with minimal tension.
- See Figures 13.1 to 13.6a, b.
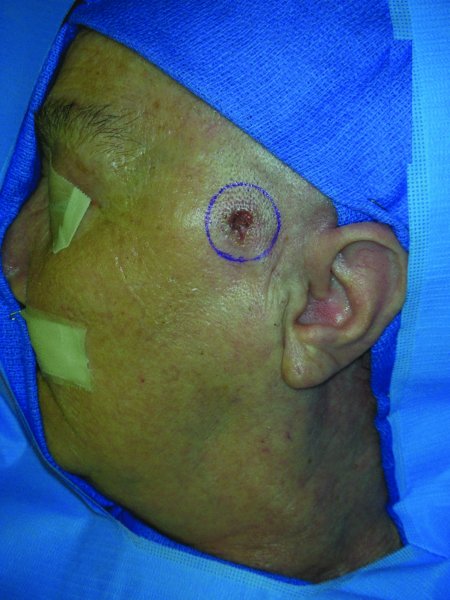
Figure 13.1 Appearance of a left facial lesion with planned resection margins.
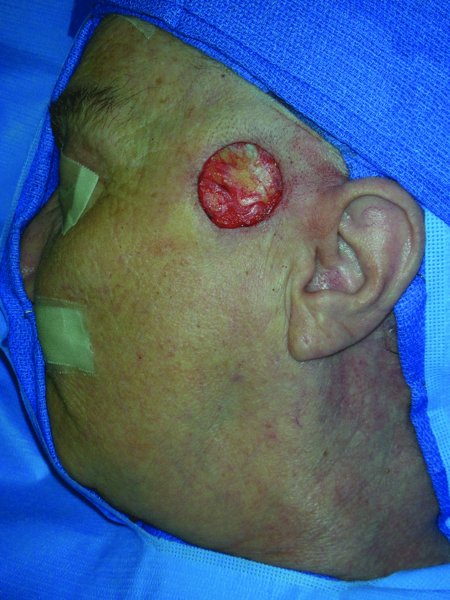
Figure 13.2 Defect after excision of the lesion.
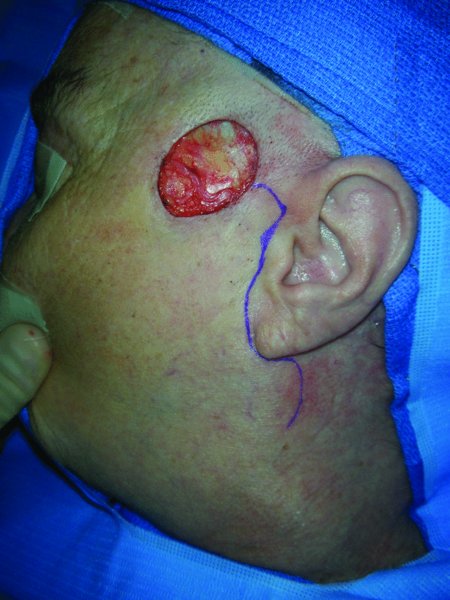
Figure 13.3 Planning for the cervicofacial flap with incision in the preauricular region.
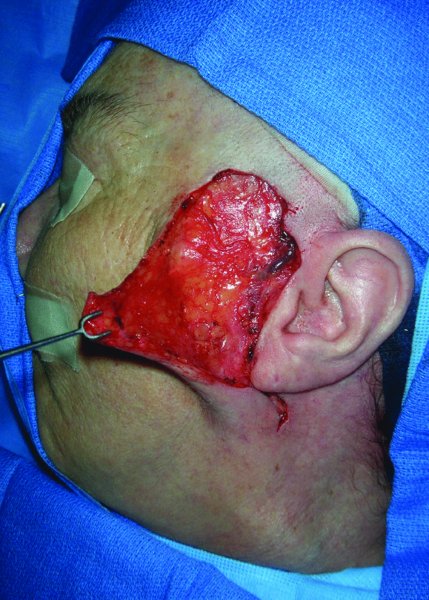
Figure 13.4 Elevation of a facial flap prior to transfer.
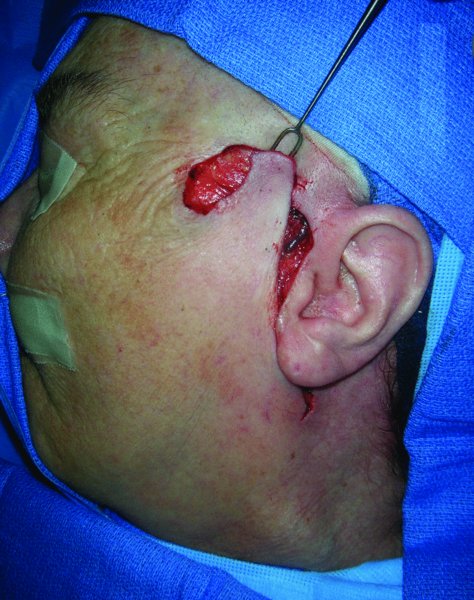
Figure 13.5 Confirmation of the reach of the flap to repair the defect.
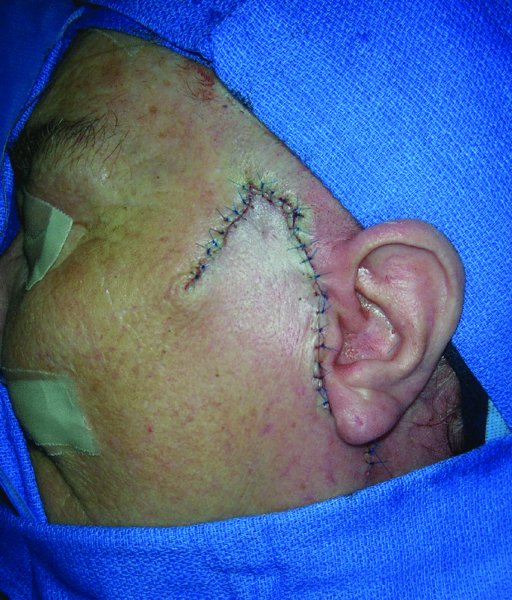
Figure 13.6a Inset of the flap into the defect.
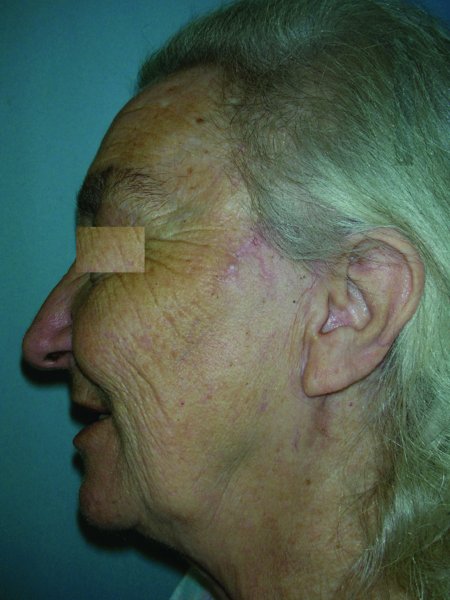
Figure 13.6b Appearance after a few months post-surgery; note the well healed scar.
Extended cervicofacial (cervicopectoral/cervicothoracic) flap
- In cases where the defect is large or for complex defects of the cheek where there is a through-and-through defect, the reconstruction may be carried out using a combination of flaps such as a pedicle pectoralis myocutaneous flap to repair the buccal defect and the extended cervicofacial (cervicopectoral) flap for the skin defect.
- A complex defect can also be reconstructed with a combination of a free flap and a cervicopectoral flap.
- In these cases, the elevation of the cervicopectoral flap is extended inferior to the clavicle and onto the pectoral muscle.
- The plane of dissection in this area should be suprafascial.
- Dissection towards the midline should be deliberate and cautious to avoid the perforators from the internal mammary artery, which serve to aid in the perfusion of the extended flap.
- The flap is advanced to the defect and checked to be sure that adequate tissue can be transferred to repair the defect.
- Often, there is enough redundant tissue that affords the surgeon the ability to contour the flap and place the incisions along the junctions of various subunits. Attention to this detail will render a more pleasing final cosmetic reconstruction.
- The donor site can often be closed primarily after wide undermining.
- If the donor site is unable to be closed primarily even after wide undermining, then a skin graft may be used to repair the remaining open area.
Case #1
A 66/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


