6
Preoperative preparation of the patient for surgery
There are a number of issues to consider in preparing the patient for surgery, including the timing of surgery, improving the physical status of the patient, information for the patient and ensuring that the correct procedure is carried out.
Timing of surgery
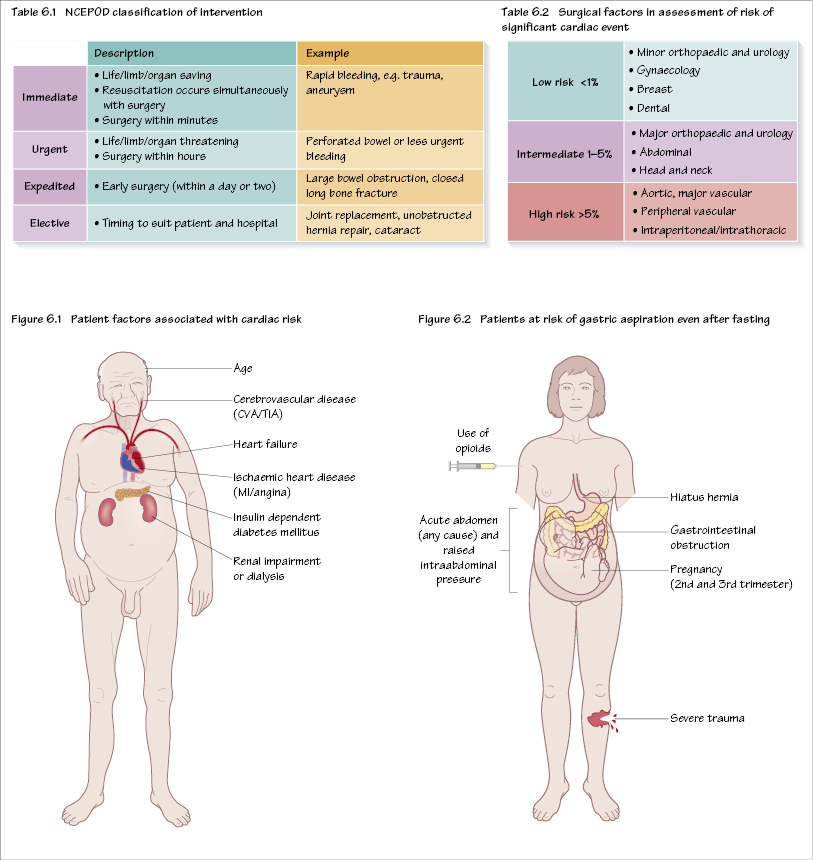
There are various classifications of the urgency of surgery; the most common is the NCEPOD classification (National Confidential Enquiry into Patient Outcome and Death), given in Table 6.1. The anaesthetist has to ensure that the patient is made as well as they can be made prior to surgery. In immediate cases, there will be no time to effect improvement in the patient’s condition beforehand, as resuscitation takes place simultaneously during surgery. Fortunately such cases are quite rare; with most ‘emergencies’ there are a few hours which can be well spent to reduce risk and improve outcome by careful treatment (vascular access, urinary catheter, nasogastric tube, i.v. fluids). With elective patients there is plenty of time to make the patient as well as they can be (e.g. treatment of hypertension or angina). In some cases it may be appropriate to refer the patients for other surgery first (e.g. coronary revascularization or carotid surgery prior to, for example, a joint replacement).
Assessment of risk
Patients may ask about the risks associated with their procedure. Whilst it is not possible to give an exact figure, there are two main areas to consider – the patient (Figures 6.1) and the proposed surgery (Table 6.2). Cardiac risk is the major area that has been studied, as perioperative cardiac events are not uncommon and carry a significant mortality.
There are many general risk-scoring systems; the most well known is the American Society of Anesthesiologists (ASA) grading (Table 6.3), but there are many others including POSSUM (Physiological and Operative Severity Score for enUMeration of morbidity and mortality), APACHE (Acute Physiology and Chronic Health Evaluation) and various others specifically for cardiac risk such the Goldman (1977) and Lee’s modification of this in 1999.
Table 6.3 ASA grading
| ASA grade | Definition | Example |
|---|---|---|
| I | A normal healthy patient | |
| II | A patient with mild systemic disease | Well-controlled hypertension, asthma |
| III | A patient with severe systemic disease | Controlled CHF, stable angina |
| IV | A patient with severe systemic/> |
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


