6 Practical Application of the SAC Classification
Having discussed the structure and determinants of the SAC Classification in earlier chapters, in this section the process of determining an SAC Classification for clinical cases will be demonstrated. A number of case presentations will illustrate how a classification may be derived, and some significant issues that may arise.
6.1 How is a Classification Derived for Specific Case?
A. Dawson, S. Chen
During the Mallorca Consensus Conference, the tables that form the basis of discussions in Chapters 4 and 5 were developed. These outline the normative classifications that would be assigned to a class of similar cases, for example, single tooth replacements in an esthetic site. When determining a classification for a specific case within such a class, users of the classification should start by finding the appropriate case type within these tables (for both the surgical and restorative parts of the classification) and deciding on the normative classification that would apply. These surgical and restorative normative classifications can then be further modified to take account of specific risk factors that apply to the case in question to determine the final classification for that case. As esthetic risk is an important part of both the surgical and restorative classification, the ERA (Esthetic Risk Assessment) from Section 3.2 will need to be determined.
The surgical group at the consensus conference proposed six factors that form the basis of their classification. Thus the surgical normative classification can be found by finding the case type and features of the case in question in the tables in Chapter 4. The restorative process is much more complex in the sense that more factors have the potential to influence the outcome of restorative implant treatments. Consequently, the classification for a specific case will be determined by the “best-fit” that can be derived for that case within the appropriate table in Chapter 5. Other potential complicating factors are then applied. In the restorative tables, more than three factors that have an Advanced or Complex classification would indicate a normative classification of at least Advanced. The process might better be described using a number of real-life cases, and these are detailed below.
6.2 A Straightforward Restorative Case – Replacement of a Maxillary First Molar
S. Chen, A. Dickinson
A 37-year-old female patient was referred for replacement of an upper right first molar (tooth 16). The pre-treatment status of this area is illustrated in Figure 1. The tooth had been endodontically-treated twice over a 5 year period. Two years previously, the tooth had fractured and was then restored with a post-retained crown. The crown had recently loosened and fallen off.
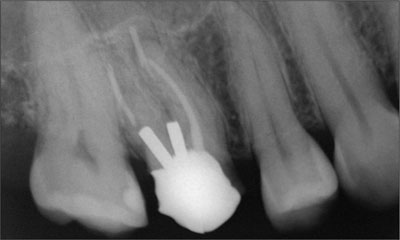
Figure 1. Radiograph of tooth 16 prior to its final failure.
On examination, the tooth had been decoronated with some post and core structure remaining. Two posts were retaining an amalgam core. A periapical area was present over the mesio-buccal root. Normal probing pockets were present around the tooth. The endodontic and restorative prognosis was deemed to be poor and a replacement with an implant-supported crown was recommended. The remaining dentition was healthy. The patient’s general health was good and she was a non-smoker.
The treatment plan was as follows:
-
Extraction of tooth 16, followed by a healing period of 12 weeks to allow partial bone healing and flattening of the sinus floor
-
Implant placement
-
Restoration with a single crown
A surgical SAC assessment was undertaken (Table 1). There were no medical contraindications to treatment and the patient was a non-smoker. The site was not in the esthetic zone. Following extraction of the tooth, it was anticipated that oro-facial bone width would be sufficient to allow an implant with a large endosseous diameter and wide restorative platform to be placed. Bone was expected to reduce in height during the 12 weeks after extraction due to a combination of crestal bone loss and modeling of the bone at the sinus floor. However, it was anticipated that there would be sufficient bone height to allow an 8 mm long implant to be placed. The procedure could therefore be undertaken with minimal anatomic risk. The procedure was determined to have a relatively low level of difficulty, with a low risk of operative and postoperative complications. The surgical SAC Classification was therefore determined to be Straightforward.
| General Factors | Assessment | Notes |
| Medical contraindications | None | |
| Smoking habit | None | |
| Growth considerations | None | |
| Site Factors | Assessment | Notes |
| Bone volume | Sufficient | Possibility that there may not be sufficient bone height following healing after tooth extraction |
| Anatomic risk | Low | |
| Esthetic risk | Low | |
| Complexity | Low | |
| Risk of complications | Low | Risk of perforation of the sinus floor membrane if site over-drilled |
| Loading protocol | Early | The plan was to restore the implant 6 to 8 weeks after placement |
| SAC Classification | Straightforward |
It was recognized that healing after tooth extraction may result in less bone height than anticipated. In this situa-tion, grafting of the sinus floor using the osteotome technique would be required in conjunction with implant treatment. This procedure would have an increased anatomic risk and complexity. The risk of perforation of the sinus membrane was also recognized.
Significant issues in the determination of a restorative SAC Classification are listed in Table 2. In this case, the space available for restoration was ideal, there was low esthetic risk, and risk of complications was low. As such, all of the applicable factors in Table 2 indicate that a classification of Straightforward was appropriate.
| Posterior Single Tooth | Notes | Straightforward | Advanced | Complex |
| Inter-arch distance | Refers to the distance from the proposed implant restorative margin to the opposing occlusion | Ideal tooth height +/- 1 mm | Tooth height reduced by ≥ 2 mm | Non-restorable without adjunctive preparatory therapy due to severe over-eruption of opposing dentition |
| Mesio-distal space (Premolar) | Anatomic space corresponding to the missing tooth +/- 1 mm | Anatomic space corresponding to the missing tooth plus 2 mm or more | Non-restorable without adjunctive preparatory therapy due to severe space restriction ≤ 5 mm | |
| Mesio-distal space (Molar) | Anatomic space corresponding to the missing tooth +/- 1 mm | Anatomic space corresponding to the missing tooth +/- 2 mm or more | Non-restorable without adjunctive preparatory therapy due to severe space restriction ≤ 5 mm | |
| Access | Adequate | Restricted | Access prohibits implant therapy | |
| Loading protocol | To date, immediate restoration and loading procedures are lacking scientific documentation | Conventional or early | Immediate | |
| Esthetic risk | Refer to ERA (Treatment Guide 1) | Low | Moderate | Maxillary first premolars in patients with high esthetic demands |
| Occlusal para-function | Risk of complication to the restoration is high | Absent | Present | |
| Provisional implant-supported restorations | Situations where provisional restorations are recommended | Restorative margin < 3 mm apical to mucosal margin | Restorative margin > 3 mm apical to mucosal margin |
The treatment plan was discussed with the patient. The possibility that treatment could increase in complexity if bone height was less than anticipated was highlighted. The patient then gave her consent to proceed with treatment.
The tooth was extracted without flap elevation, and healing progressed uneventfully. After 12 weeks, the soft tissues had healed with minimal loss of oro-facial dimension of the ridge. Radiographically, partial bone fill had occurred. However, there was greater vertical loss of bone height than originally anticipated. It was estimated that 6 mm of corono-apical bone was available. It was therefore planned to elevate the floor of the sinus using osteotomes to allow an implant with a length of 8 mm to be placed. The patient was advised that this would increase the degree of difficulty of the procedure, and risk of perforation of the sinus membrane. The SAC Classification was reviewed and amended to Complex (Table 3).
| General Factors | Assessment | Notes |
| Medical contraindications | None | |
| Smoking habit | None | |
| Growth considerations | None | |
| Site Factors | Assessment | Notes |
| Bone volume | Insufficient | Sinus floor elevation and bone graft required; sufficient bone height to allow simultaneous implant placement |
| Anatomic risk | High | Involvement of the maxillary sinus |
| Esthetic risk | Low | |
| Complexity | High | Combination of sinus floor elevation using the osteotome technique and implant placement has a high degree of complexity |
| Risk of complications | High | Risk of perforation of the sinus floor membrane |
| Loading protocol | Early | The plan was to restore the implant 6 to 8 weeks after placement |
| SAC Classification | Complex |
Following administration of local anesthesia, full thickness flaps were raised on the facial and palatal aspect of site 16. Intra-operative assessment confirmed sufficient oro-facial bone width to allow an implant with an endosseous diameter of 4.8 mm to be placed. The site was prepared to a depth of 5 mm using twist drills of increasing diameter until the osteotomy was prepared to a diameter of 4.2 mm. The osteotomy was filled with autogenous bone chips that were locally harvested. Osteotomes were used to infracture the cortical bone of the sinus floor. The membrane was checked to verify that no perforation had occurred. An implant with an SLA surface, 4.8 mm endosseous diameter, 8 mm length and 2.8 mm collar (Straumann WN S implant, Straumann AG, Basel, Switzerland) was inserted into the osteotomy. The implant achieved good initial stability and a 2 mm extended healing cap was attached.
The flaps were adapted around the healing cap and closed with simple interrupted sutures. The patient was advised to use a 0.2% chlorhexidine mouth rinse and to refrain from mechanical cleaning of the area for 2 weeks. Healing progressed uneventfully and the implant integrated (Figure 2).
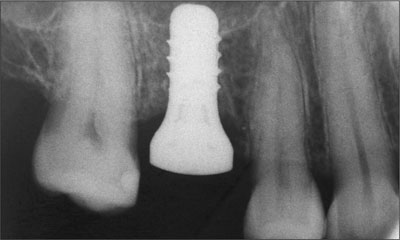
Figure 2. Radiographic appearance of the healing implant.
Restorative procedures commenced eight weeks after surgery. This involved the placement of a solid abutment followed by taking a transfer impression that incorporated recording the position of the implant collar and the abutment. At a subsequent appointment, a cemented crown was placed after confirming fit, occlusal and interproximal contacts, and esthetics. The patient was happy with the final result.
At the most recent review, the peri-implant tissues were healthy with stable bone conditions observed nine years after initial surgery (Figures 3a to 3c).
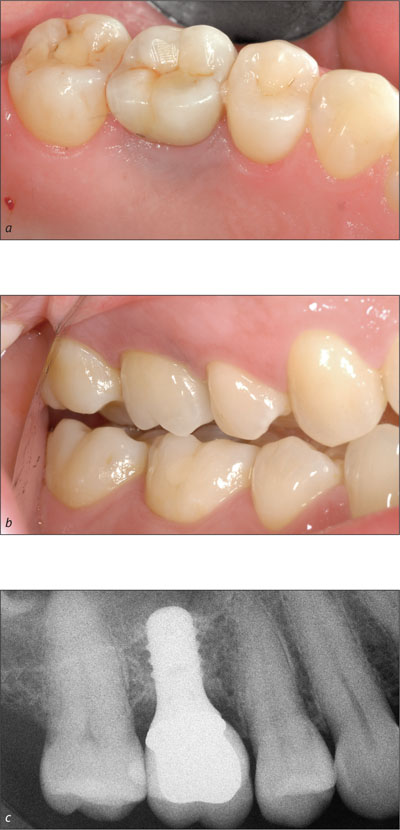
Figures 3a-c. Final restoration in place and radiographic view nine years after surgery.
Comments
This case illustrates the surgical and restorative SAC Classifications for replacement of a single upper molar. Initially, the surgical SAC was regarded as Straightforward. However following extraction of the tooth, the reduced bone volume increased the complexity of the treatment. This contingency was discussed with the patient before commencement of treatment. The restorative phase of treatment remained Straightforward despite the amendment to the surgical classification. The implant was well positioned which allowed restorative treatment to progress as originally planned.
6.3 An Advanced Case – Upper Left Central Incisor Replacement
C. Evans, S. Chen
A healthy 47-year-old female presented for consultation on referral from her general dental practitioner. The patient had noticed some intermittent bleeding after tooth brushing from the facial surface of the tooth 21. No pain or discomfort had been experienced by the patient. The patient had been referred to a specialist endodontist who confirmed the presence of external cervical resorption (Figure 1). The tooth was deemed not restorable and replacement alternatives sought. The patient wished to investigate the option of an implant-supported crown to replace the upper left central incisor.
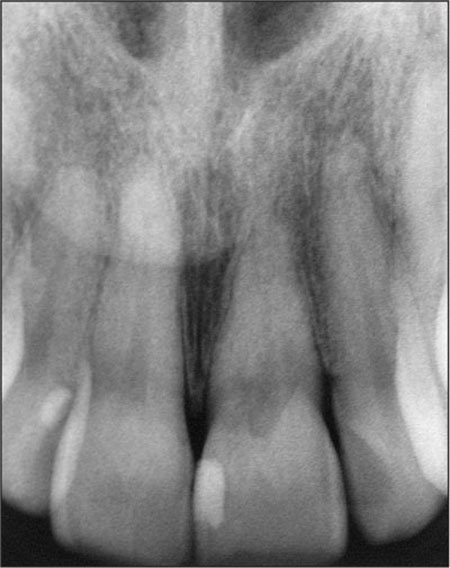
Figure 1. Radiograph of presenting condition of tooth 21.
Clinical examination revealed tooth 21 to have a small mesial resin restoration but otherwise to be unrestored. Close examination revealed the facial surface of tooth 21 to have a resorptive defect that could be easily probed, extending beneath the gingival margin. The cervical enamel was pink in color indicating the loss in dentinal tooth structure that characterizes these lesions (Figure 2). The adjacent teeth were unrestored. A low smile line was present even on wide smiling. The gingival tissue biotype was classified as medium and the tooth shape was square. Esthetic Risk Assessment indicated that the Esthetic Risk was moderate (Table 1).
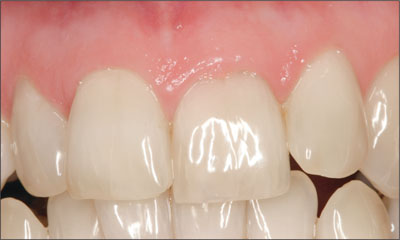
Figure 2. Clinical appearance at presentation, demonstrating pink coloration of the cervical area of tooth 21.
| Esthetic Risk Factor | Level of Risk | ||
| Low | Moderate | High | |
| Medical status | Healthy, co-operative patient with an intact immune system. | Reduced immune system | |
| Smoking habit | Non-smoker | Light smoker (< 10 cigs/day) | Heavy smoker (> 10 cigs/day) |
| Patient’s esthetic expectations | Low | Medium | High |
| Lip line | Low | Medium | High |
| Gingival biotype | Low scalloped, thick | Medium scalloped, medium thick | High scalloped, thin |
| Shape of tooth crowns | Rectangular | Triangular | |
| Infection at implant site | None | Chronic | Acute |
| Bone level at adjacent teeth | ≤ 5 mm to contact point | 5.5 to 6.5 mm to contact point | ≥ 7 mm to contact point |
| Restorative status of neighboring teeth | Virgin | Restored | |
| Width of edentulous span | 1 tooth (≥ 7 mm) | 1 tooth (≤ 7mm) | 2 teeth or more |
| Soft tissue anatomy | Intact soft tissue | Soft tissue defects | |
| Bone anatomy of alveolar crest | Alveolar crest without bone deficiency | Horizontal bone deficiency | Vertical bone deficiency |
There was minimal evidence of parafunctional activity. Tooth 21 had supra-erupted by 0.5 to 1.0 mm compared to the contra-lateral tooth. The gingival margin associated with tooth 21 was irregular and located about 0.5 mm coronal when compared to tooth 11. Crown coloration of the anterior teeth was low in value with strong chroma and a moderate degree of translucency.
Treatment options were discussed with the patient and an implant-supported crown was planned to replace the tooth 21. The case was classified as Advanced. An interim removable partial denture was planned to be used during implant therapy.
Due to the intact nature of the root form and lack of apical infection, the surgical phase of implant treatment was planned to be performed as a Type 1 (immediate placement) protocol. Implant placement was planned to allow direct occlusal screw access of the final restoration. A conventional loading protocol was planned with restoration planned after 3 months of implant healing.
The intention to use a Type 1 placement protocol with a flapless approach indicates a surgical SAC Classification of Complex (Table 2).
| General Factors | Assessment | Notes |
| Medical contraindications | None | |
| Smoking habit | None | |
| Growth considerations | None | |
| Site Factors | Assessment | Notes |
| Bone volume | Adequate | |
| Anatomic risk | Low | |
| Esthetic risk | Moderate | |
| Complexity | High | Immediate placement and flapless approach increases complexity of treatment. |
| Risk of complications | High | |
| Loading protocol | Conventional | The plan was to restore the implant 12 weeks after placement |
| SAC Classification | Complex |
The restorative SAC Classification is determined by reference to the relevant case type table (Table 3). This indicates a classification of Advanced is warranted. Here, the majority of factors applicable to this case fall into the Advanced class, thus indicating this as the appropriate classification.
| Anterior Single Tooth | Notes | Straightforward | Advanced | Complex |
| Maxillomandibular relationship | Refers to horizontal and vertical overlap and the effect on restorability and esthetic outcome | Angle Class I and III |
Angle Class II Div 1 and 2 | Non-restorable without adjunctive preparatory therapy due to severe malocclusion |
| Mesio-distal space (maxillary central) | Symmetry is essential for successful outcome | Symmetry +/- 1 mm of contra-lateral tooth | Asymmetry greater than 1 mm | |
| Mesio-distal space (maxillary laterals and canines) | Symmetry +/- 1 mm of contra-lateral tooth | Asymmetry greater than 1 mm | ||
| Mesio-distal space (mandibular anterior) | Symmetry +/- 1 mm of contra-lateral tooth | Asymmetry greater than 1 mm | ||
| Loading protocol | To date, immediate restoration and loading procedures are lacking scientific documentation | Conventional or early | Immediate | |
| Esthetic risk | Refer to ERA (Treatment Guide 1) | Low | Moderate | High |
| Occlusal para-function | Risk of complication is to the restoration, not to implant survival | Absent | Present | |
| Provisional implant-supported restorations | Provisional restorations are recommended | Restorative margin < 3 mm apical to mucosal margin | Restorative margin > 3 mm apical to mucosal margin |
After minimally traumatic tooth extraction, an implant with an SLA surface (Straumann RN SP implant with an endosseous length of 10 mm, Straumann AG, Basel, Switzerland) was placed in an ideal three dimensional position, to allow direct screw access through the cingulum of the final crown. The implant was placed oro-facially with the shoulder positioned in the Comfort Zone as described by Buser et al. 2004. The implant shoulder was located 2.5 mm apical to the planned mucosal margin (Figures 3a and 3b).
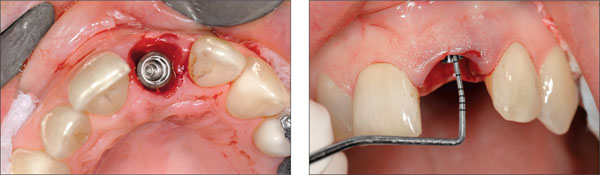
Figures 3a and 3b. Implant positioning relative to adjacent teeth and the gingival margin.
A small connective tissue graft was placed in the facial pouch to augment the facial peri-implant tissue thickness. Implant healing occurred in a partially submerged approach (Figure 4).
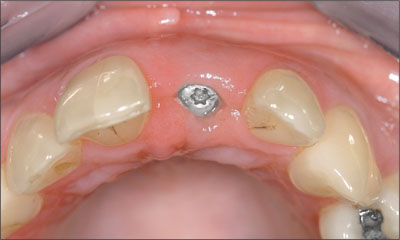
Figure 4. Implant appearance after completion of healing.
Prior to the commencement of restorative procedures, a second surgical procedure was performed to attach a longer healing abutment to facilitate restorative procedures. An idealized soft tissue form was found with excellent soft tissue contours (Figure 5). The decision was made to proceed direct to definitive restoration, without the need to use a provisional crown to develop the transition zone, due to the ideal implant position, ideal soft tissue volume, low lip line and moderate patient expectations.
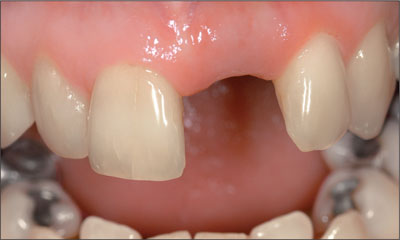
Figure 5. Soft tissue contour after healing.
Implant restoration was commenced with an implant level impression made to allow fabrication of a master cast. A screw retained impression coping was connected to the implant and a periapical radiograph taken to verify complete seating of the impression coping. A synOcta 1.5mm abutment (Straumann AG, Basel, Switzerland) was selected and a preformed gold coping used to fabricate a direct screw-retained, PFM crown, designed with an idealized emergence profile (Figure 6).
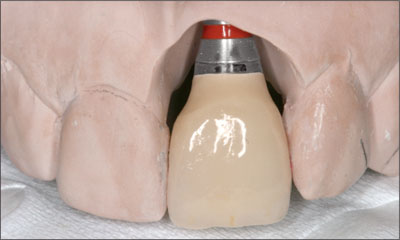
Figure 6. The completed restoration prior to placement.
The definitive abutment was tightened to 35 Ncm and retention screw to 15 Ncm. Initial soft tissue blanching required the emergence profile to be reduced slightly to ensure that soft tissue blanching was minimized (Figure 7) and this completely resolved within 10 minutes. Proximal contact points were placed to be within 5 mm of the bone crest level on the adjacent teeth and periapical radiographs demonstrate complete seating of the restoration (Figure 8).
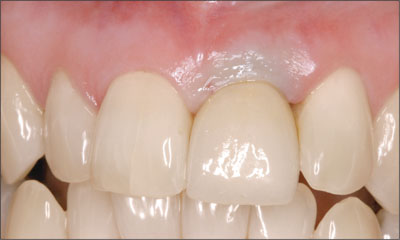
Figure 7. Final restoration at the time of placement. The emergence profile was modified to minimize soft tissue blanching.
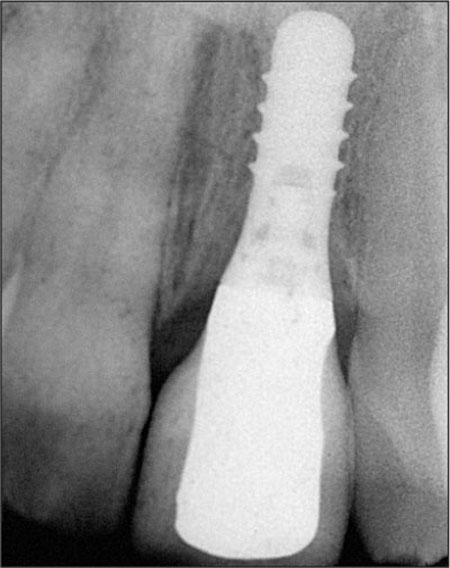
Figure 8. Radiograph of the seated restoration taken at the time of restoration delivery.
The final restoration required a small amount of surface glaze staining to balance restoration coloration under natural lighting conditions.
The final restoration is seen in harmony with the adjacent teeth and soft tissues 18 months after restoration placement (Figures 9a and 9b).
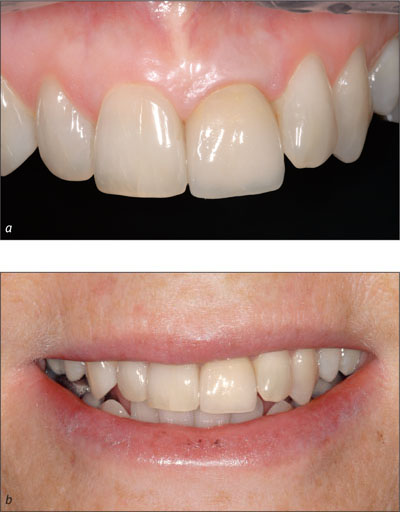
Figures 9a and 9b. Appearance 18 months after restoration placement.
Comments
This case progressed without any significant complication due to good preoperative assessment and planning, and meticulous execution of the treatment plan by skilled practitioners. However, although this is seemingly a simple case, the inherent risks associated with the procedures used, and the complexity of the techniques employed, still indicate that a surgical classification of Complex and a restorative classification of Advanced were appropriate.
6.4 A Complex Esthetic Application – Immediate Implant Placement and Provisionalization
F. Higginbottom, T. Wilson
A 35-year-old patient sought help for a failing central incisor. The patient presented with a damaged central incisor that sustained trauma in her teenage years. The root fracture/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


