5 Classification of Restorative Cases
A. Dawson, W. Martin, U. Belser
5.1 Principles of Restorative Classification
The application of the SAC Classification to restorative cases will follow the general guidelines outlined below. These guidelines will assist in generating the normative classification of a clinical case type. Specific indications and the influence of modifying factors on these case types will be introduced in detail within this chapter.
Clinical cases may be assessed as Straightforward, Advanced or Complex when they meet the following criteria:
Straight forward
-
A non-esthetic site, hence the esthetic risk is minimal.
-
The restorative process is expected to be uncomplicated and involves few steps.
-
The restorative outcome is readily predictable.
-
There is a low risk of complications.
Advanced
-
There is a discernable esthetic risk.
-
The restorative process may have an increased number of steps, but the outcome is predictable.
-
The restorative outcome can be accurately visualized.
-
The risk of complications is low to moderate.
Complex
-
The esthetic risk is moderate to high.
-
The restorative process involves multiple steps, and the treatment plan may need to be re-evaluated as a consequence of the outcome of one or more of these steps.
-
The restorative outcome cannot be readily visualized prior to treatment.
-
The risk of complications is high, and multiple branching contingency plans may be necessary to deal with these issues. The long-term outcome of the restorative process may be compromised by these complications.
-
Detailed coordination, communication, and sequencing of treatment procedures between the restorative dentist, surgeon and laboratory technician are essential for success. Patients must understand and accept the potential for compromised outcomes.
These criteria define the normative classification of case types. In addition, the Esthetic and Restorative modifying factors discussed in Chapter 3 may also apply in the risk assessment of specific cases. The following tables summarize the most significant of these modifying factors for each case type. These factors will be discussed below in the areas where they may have the greatest impact.
In general, factors such as the space available for restoration, the number of missing teeth to be replaced, and the quality and quantity of hard and soft tissues in the area will have an impact on the restorative classification.
5.2 Posterior Single Tooth Replacements
Table 1 summarizes the influence of specific modifying factors on the classification of posterior single tooth replacements. These modifying factors determine the normative classification for case types. These classifications can be adapted to fit specific situations by the restorative and esthetic factors discussed earlier. Users of the classification should look for the normative presentation that best fits their specific case and apply the necessary modifiers to obtain an appropriate SAC Classification.
| Posterior Single Tooth | Notes | Straightforward | Advanced | Complex |
| Inter-arch distance | Refers to the distance from the proposed implant restorative margin to the opposing occlusion | Ideal tooth height +/- 1 mm | Tooth height reduced by ≥ 2 mm | Non-restorable without adjunctive preparatory therapy due to severe over-eruption of opposing dentition |
| Mesio-distal space (Premolar) | Anatomic space corresponding to the missing tooth +/- 1 mm | Anatomic space corresponding to the missing tooth plus 2 mm or more. | Non-restorable without adjunctive preparatory therapy due to severe space restriction ≤ 5 mm | |
| Mesio-distal space (Molar) | Anatomic space corresponding to the missing tooth +/- 1 mm | Anatomic space corresponding to the missing tooth +/- 2 mm or more | Non-restorable without adjunctive preparatory therapy due to severe space restriction ≤ 5 mm | |
| Access | Adequate | Restricted | Access prohibits implant therapy | |
| Loading protocol | To date, immediate restoration and loading procedures are lacking scientific documentation | Conventional or early | Immediate | |
| Esthetic risk | Refer to ERA (Treatment Guide 1) | Low | Moderate | Maxillary first premolars in patients with high esthetic demands |
| Occlusal para-function | Risk of complication to the restoration is high | Absent | Present | |
| Provisional implant-supported restorations | Situations where provisional restorations are recommended | Restorative margin < 3 mm apical to mucosal margin | Restorative margin > 3 mm apical to mucosal margin |
5.2.1 Space for Restoration
The inter-arch space available for restoration, which is the distance from the anticipated restorative margin to the opposing occlusal plane, will have an impact on the complexity of restorative treatment and the likelihood of complications (Figures 1 and 2). This issue may be less critical in bone-level implants where the shoulder of the implant is placed at the alveolar crest. These implant designs will often be accompanied by a wide selection of restorative components that allow for varying restorative margin positions. Implant designs that incorporate a transmucosal collar require planning that compensates for the height of the collar in situations where the inter-arch dimension is limited. In all implant designs, the space for restorative components and the ability to develop an ideal emergence profile are always critical. Restorative challenges are generally not associated with increased inter-arch space. Rather, limited inter-arch space is likely to complicate the process. When restorative space is limited, treatment plans will often include procedures to create ideal space. These procedures may include: adjustments to the opposing dentition, elective endodontics, crown lengthening, full-coverage restorations, orthodontic intrusion, or surgical osteotomies. Alternatively, when anatomy allows (e.g., when the inferior alveolar nerve position is favorable), the surgical plan may be modified to ensure that implants are placed more deeply to allow adequate space for restoration. However, such plans may result in deeply placed restorative margins that will indicate the use of screw-retained restorations.
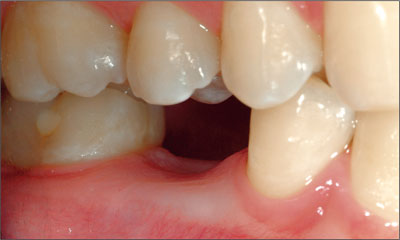
Figure 1. Adequate inter-arch space for replacement of tooth 45.
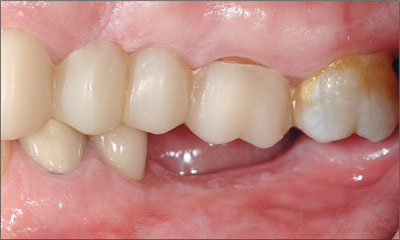
Figure 2. Inadequate inter-arch space for replacement of tooth 36.
Limited or excessive inter-arch space may influence esthetic outcomes, so special consideration must be given to patients who have any esthetic risk. Poor crown length-to-width ratios will have an adverse impact on esthetics. When crowns are too short, surgical management using deeper implant placement and soft tissue reduction techniques may be successful. However, esthetic compromises may still be evident in opposing arches where there is a mismatch in the sizes of restorations and natural teeth. Long crowns are often not easily managed without the assistance of vertical ridge augmentation or the use of tissue-colored porcelain.
The mesio-distal space available for restoration will also have an impact on the treatment regimen. Limited space, more often in premolar sites, may influence implant selection, surgical access, restorative materials and maintenance (Figures 3a to 3c). In patients with esthetic risk, restorative space limitations have an effect on crown proportions and interproximal soft tissue, often leading to an esthetic compromise. Situations with excessive mesio-distal space can also pose esthetic risk, and some form of adjunctive restorative treatment (such as modifying the contour of adjacent teeth with restorations or crowns) may be necessary.
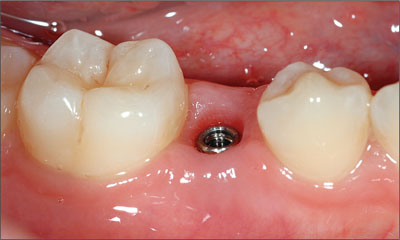
Figure 3a. Post-orthodontic result (tooth 45) with limited mesio-distal space (5 mm) requiring selection of a narrow platform implant.
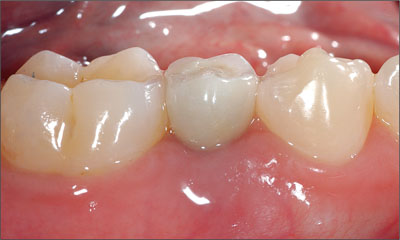
Figure 3b. Limited mesio-distal space (tooth 45), leading to compromised crown proportion and emergence profile when compared to adjacent teeth.
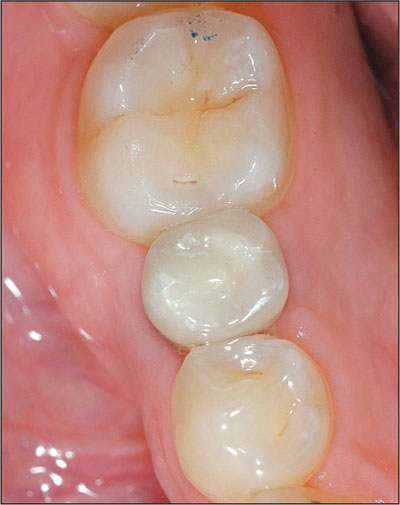
Figure 3c. Limited mesio-distal space (tooth 45), leading to compromised crown proportion and emergence profile when compared to adjacent teeth.
5.2.2 Access
Restricted mouth opening may be a consequence of normal anatomy, temporomandibular joint problems, or other pathological conditions. This may limit the ability of surgeons and restorative dentists to gain access to a potential site for an implant-supported restoration. In general, this is most likely to be problematic in posterior sites, and may preclude implant treatment as an option. As a general rule, greater than 30 mm of inter-ach space is necessary for implant therapy.
5.2.3 Loading Protocol
The Group 3 statements (Loading Protocols) from the Third ITI Consensus Conference (Cochran et al. 2004) recommended against employing immediate loading techniques in single tooth replacements, noting that at the time of the conference there was insufficient evidence to support this procedure as a routine technique in implant dentistry. Generally, this lack of supporting evidence is still an issue, although an increasing number of investigations are being conducted in this area of research. However, should immediate loading (i. e., occlusal loading of the implant via a provisional or definitive restoration within 48 hours of implant placement) be seen as desirable or necessary, it should be noted that this tends to place more stress on the treatment team. A higher level of expertise and logistic coordination are necessary compared to early or conventional loading protocols. Alternatively, immediate restoration (i. e., placement of a provisional restoration with no occlusal load within 48 hours of implant placement) may be utilized in situations where there is a high esthetic risk and/or a desire to maintain intra-arch space. In any event, care must be taken to prevent para-functional non-axial loading of the dental implant.
5.2.4 Esthetic Risk
In most cases, single tooth replacements in posterior sites will have little or no esthetic risk, and consequently are likely to have a normative restorative classification of Straightforward. However, in some situations where patients have high and broad smiles, premolar replacements (and occasionally those for molars) will have an assessable esthetic risk (Figure 4). In these cases, normative restorative classifications of Advanced or Complex may be appropriate.
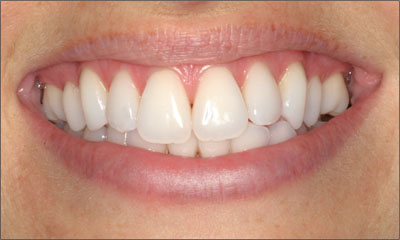
Figure 4. Posterior tooth replacement would include an elevated esthetic risk in this patient with a high, broad smile.
5.2.5 Occlusal Parafunction
Current research suggests that, whereas implant failure is not increased by parafunctional overloading, the risk of technical complications such as screw loosening and fracture, abutment fracture, and loss of veneering materials is positively associated with parafunctional activity (Brägger et al. 2001). Thus, the presence of occlusal parafunction will increase the risk of complications and may make restorative procedures more demanding, and somewhat less predictable. The restorative dentist may need to modify the planned restoration to minimize potential effects of this overloading by using a retrievable restoration, or restorations employing veneering materials that are less prone to fracture, or softer materials that will result in less wear on the opposing dentition.
5.2.6 Provisional Restorations
When the placement of an implant-supported provisional restoration is indicated, the depth of the restorative platform beneath the mucosa will have an impact on the difficulty of this process. Implant shoulders located greater than 3 mm apical to the planned mucosal margin often require screw-retained or customized meso-structures that either eliminate the need for cementation, or move the cement margin to a position where access for removal of excess cement is readily available. Entrapment of cement within the peri-implant tissues can lead to undesirable inflammation, fistula formation, and in extreme situations, bone loss. Therefore, these case types should be considered Advanced.
5.3 Anterior Single Tooth Replacements
Table 1 demonstrates the most important factors in the assessment of single tooth replacements in anterior sites. As mentioned in Section 5.2, these variants will provide basic normative classifications that may need to be further amended based upon the influence of the modifying factors.
| Anterior Single Tooth | Notes | Straightforward | Advanced | Complex |
| Maxillomandibular relationship | Refers to horizontal and vertical overlap and the effect on restorability and esthetic outcome | Angle Class I and III | Angle Class II Div 1 and 2 | Non-restorable without adjunctive preparatory therapy due to severe malocclusion |
| Mesio-distal space (maxillary central) | Symmetry is essential for successful outcome | Symmetry +/- 1 mm of contra-lateral tooth | Asymmetry greater than 1 mm | |
| Mesio-distal space (maxillary laterals and canines) | Symmetry +/- 1 mm of contra-lateral tooth | Asymmetry greater than 1 mm | ||
| Mesio-distal space (mandibular anterior) | Symmetry +/- 1 mm of contra-lateral tooth | Asymmetry greater than 1 mm | ||
| Loading protocol | To date, immediate restoration and loading procedures are lacking scientific documentation | Conventional or early | Immediate | |
| Esthetic risk | Refer to ERA (Treatment Guide 1) | Low | Moderate | High |
| Occlusal para-function | Risk of complication is to the restoration, not to implant survival | Absent | Present | |
| Provisional implant-supported restorations | Provisional restorations are recommended | Restorative margin < 3 mm apical to mucosal margin | Restorative margin > 3 mm apical to mucosal margin |
5.3.1 Maxillomandibular Relationship
The anterior occlusal relationship, most importantly the degree of horizontal and vertical overlap, will influence the restorative difficulty and technical complications after treatment is complete. Space for restorative components can be restricted by these factors, as will be the loading vector on the final restoration. Deep bites with restricted horizontal overlap, such as those found in Angle Class II division 2 cases, are potentially the most problematic due to significant space restrictions as well as to the high potential for unfavorable loading vectors impacting the restorative materials, abutments and screws. The potential for adverse wear on opposing teeth must also be acknowledged. Often, adjunctive orthodontic treatment should be considered if implant-borne tooth replacements are desired (Figures 1a and 1b).
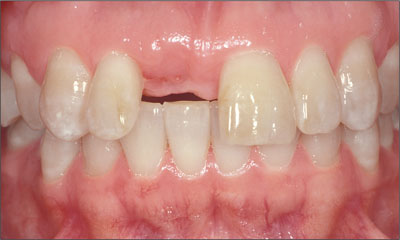
Figure 1a. Excessive vertical overlap, complicating replacement of tooth 11.
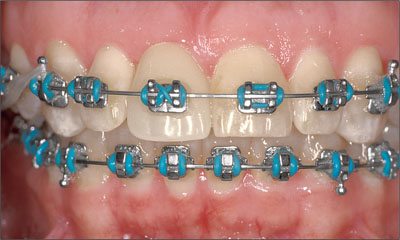
Figure 1b. Orthodontic therapy has been used to improve the vertical and horizontal relationship of the teeth.
5.3.2 Mesio-Distal Space
Symmetry with the adjacent (central incisor) or contralateral (lateral incisor and canine) teeth can be one of the most important determinants of esthetic success in an implant restoration. This may well be a factor even in situations that are deemed to have low esthetic risk due to the smile line, because improper tooth proportions may still be visible. Maxillary central incisor replacements are most critical in this area, as the contralateral natural tooth is immediately adjacent to the implant restoration. Some increase in latitude for width discrepancy can be allowed for lateral incisor and canine replacements which are more distantly related to the comparison tooth. Similar latitude may be applied to lower anterior teeth, as they are less often visible. When the intra-arch space is inadequate, the limitation can have a negative impact on the implant selection, crown proportions and resulting inter-proximal soft tissues, potentially leading to an esthetic compromise (Figures 2a and 2b).
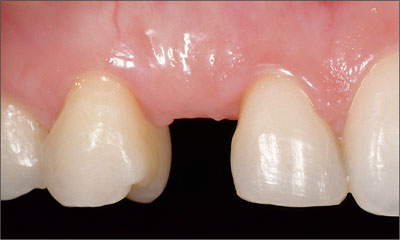
Figure 2a. Inadequate intra-arch space (6 mm) for replacement of tooth 13.
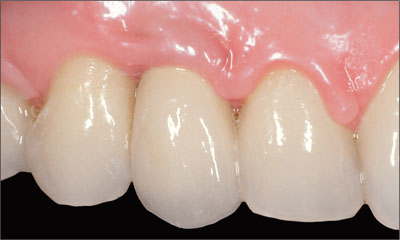
Figure 2b. A compromised peri-implant soft tissue result (tooth 13), even though adjacent tooth modification was performed in an attempt to increase intra-arch space.
In situations with either a high esthetic need or demand, adjunctive orthodontic treatment or restorative intervention involving adjacent teeth may be necessary (Figure 3). This added complexity in the treatment would likely result in a classification of Complex.
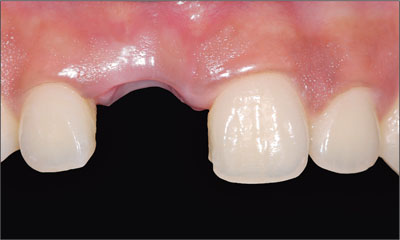
Figure 3. Increased mesio-distal dimension (tooth 11) when compared to the adjacent tooth, necessitating adjunctive treatment to achieve esthetic success.
5.3.3 Loading Protocol
As previously discussed, immediate loading protocols are currently not recommended for single tooth replacements. This is especially significant in the anterior region, where the risk of adverse esthetic outcomes is already an issue in many cases, even when conventional or early loading protocols are used. Additionally, the potential for significant non-axial loading of the implant may be a disadvantage during the healing period. Alternatively, immediate restoration of an implant may help improve the esthetic result by maintaining support of the peri-implant tissues and interproximal contact points at the time of surgery (Figures 4a to 4c). Implants possessing good primary stability in patients with favorable occlusal schemes that protect the provisional restoration during function could benefit from this technique. For these reasons, any immediate restorative procedure on single tooth implants in the anterior segment should be considered Complex.
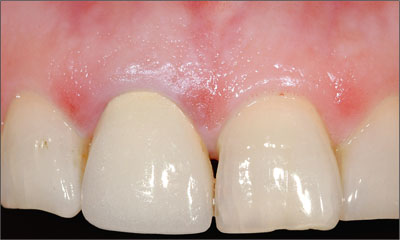
Figure 4a. Sub-osseous fracture of tooth 11 necessitating extraction of the tooth and placement of a dental implant.
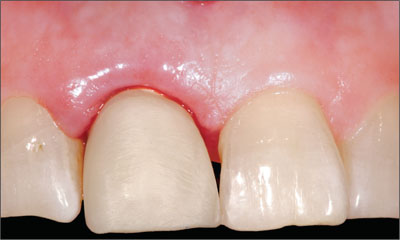
Figure 4b. Immediate implant placement with primary stability allowing for immediate restoration of tooth 11.
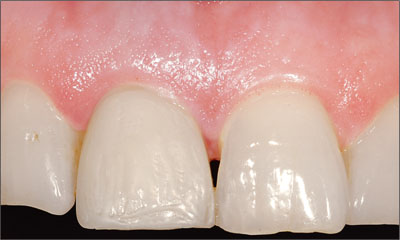
Figure 4c. The seven-day postoperative follow-up highlighting the initial maturation of the peri-implant tissues.
5.3.4 Esthetic Risk
As discussed in Chapter 3, the level of esthetic risk can have a significant impact on the degree of difficulty of implant treatment in esthetic sites, as well as on the potential for adverse outcomes. Symmetry of the implant restoration with the surrounding teeth and tissues with respect to size, shape, color, and contour is crucial for achieving esthetic success. Consequently, issues that may reduce the likelihood of a successful outcome should be identified early in the assessment phase, and the patient advised of the impact that these issues may have on the outcome of treatment. While some anterior sites may be assessed as having low esthetic risk due to a low smile line or low esthetic demand, the majority of implant restorations in the anterior segments assume a moderate to high esthetic risk. Thus these cases will have classifications of at least Advanced. Currently, there is little evidence that allows us to accurately predict the soft-tissue outcome secondary to implant surgery, as well as the long-term stability of the peri-implant soft tissues. Thus, when the esthetic risk is high, and/or the patient’s esthetic demands are high, the treatment regimen should be seen as Complex.
5.3.5 Occlusal Parafunction
As noted previously, parafunctional loading of implant restorations can be associated with an increase in technical complications. In the anterior segment, while the amount of occlusal load is less than in posterior sites, the loading vector is more unfavorable due to a larger lateral component of this force. Overall, the potential for damage to the implant restoration and components such as abutments, screws, and restorative material remains significant in patients who practice a latero-protrusive form of bruxing, or those with excessive vertical overlap.
5.3.6 Provisional Restorations
Provisional implant-supported restorations are indicated in the anterior segment to develop the transition zone (the emergence created from the shoulder of the implant to the mucosal margin) and to prepare the site for the definitive restoration (Figures 5a and 5b). The three-dimensional position of the implant can influence the type of provisional restoration utilized (cemented vs. screw-retained). The depth of the implant shoulder below the mucosal margin and the patient’s tissue biotype will affect the difficulty of the treatment and the predictability of the result. In the case of a deeply placed implant, the soft-tissue management is more demanding and the risk of complications is higher. In such situations, the need for screw retention and tissue shaping through multiple adjustments to the emergence profile of the provisional restoration cannot be overemphasized.
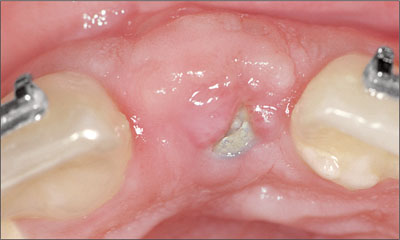
Figure 5a. Semi-submerged implant (tooth 21) requiring the fabrication of a provisional restoration.
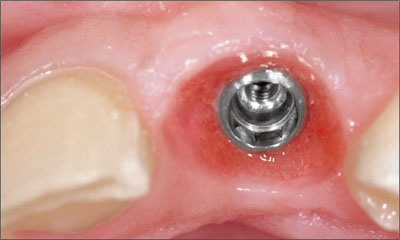
Figure 5b. Shaping of the transition zone accomplished with the provisional restoration over a four-week period.
5.4 Posterior Extended Edentulous Spaces
Table 1 details the factors considered to influence the classification of multiple-tooth replacement restorations in posterior sites. Consideration of these factors, and any other modifiers such as those discussed in Chapter 3, will allow the classification of such cases.
| Posterior Extended Edentulous Spaces | Notes | Straightforward | Advanced | Complex |
| Esthetic risk | Refer for ERA (Treatment Guide 1) | Low | Moderate/High | |
| Access | Adequate | Restricted | Limited access does not allow for implant therapy | |
| Inter-arch distance | Refers to the distance from the proposed implant restorative margin to the opposing occlusion | >8 mm | < 8 mm or >16 mm | |
| Mesio-distal space | Anatomic space corresponding to the missing teeth +/- 1 mm | Anatomic space corresponding to the missing teeth plus 2 mm or more, or space corresponding to a whole number of premolar units | Non-restorable without adjunctive preparatory therapy due to severe space restriction | |
| Occlusion/articulation | Harmonious | Irregular with no need for correction | Changes to existing occlusion necessary | |
| Interim restorations during healing | None needed | Removable/ fixed | ||
| Occlusal para-function | Risk of complication to the restoration is high. | Absent | Present | |
| Loading protocol | To date, immediate restoration and loading procedures are lacking scientific documentation | Conventional or early | Immediate | |
| Cemented (Consensus Statement) | Accessible restorative margin | Sub-mucosal location of restorative margin | ||
| Screw-retained | Multiple non-splinted Implants | Multiple splinted implants |
5.4.1 Esthetic Risk
The replacement of multiple teeth in posterior sites with implant restorations is not usually associated with significant esthetic risk, and such cases can normally be classified as Straightforward. However, in patients with excessively high or broad smiles (see Figure 4 in 5.2.4), these areas can be exposed, leading to a measurable esthetic risk and thus warranting classifications of Advanced or Complex. Edentulous ridges presenting with significant loss of hard and soft tissue contour may require either pre-surgical so/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


