3 Modifying Factors
3.1 General Modifiers
S. Chen, A. Dawson
Normative classifications refer only to standard presentations of a case type. The following factors may modify these classifications, generally through increasing the difficulty of a treatment process:
3.1.1 Clinical Competence and Experience
While it is assumed that clinicians will undertake implant therapy that does not exceed their clinical abilities, it should be noted that the normative SAC Classification for a case type is independent of the clinicians’skill and competence. Thus, a Straightforward case will represent an uncomplicated procedure for both the novice and experienced clinician. On the other hand, a Complex case will be difficult to manage for the novice and experienced clinician alike. In this regard, the difference between the two is that the experienced clinician possesses the skill, competence and knowledge to manage the complex case and to deal with complications should they arise. In contrast, the novice clinician lacks the necessary skill and experience and would be best advised to refer such a case to someone with greater expertise.
3.1.2 Compromised Patient Health
Treatment of patients with compromised health is often more difficult in execution as well as more prone to complications (Table 1). For example, we know that smokers (Strietzel et al. 2007) and patients with uncontrolled diabetes mellitus (Moy et al. 2005, Ferreira et al. 2006) are more likely to have post-operative complications and implant failure and are regarded as at high risk for implant therapy. Other conditions can also have an impact in these areas, and must be assessed during the work-up for each case. These factors may be controlled to allow progression of the treatment, but the treatment process generally requires variations from standard treatment protocols.
| Risk Factor | Remarks |
| Medical |
|
| Periodontal |
|
| Oral Hygiene/Compliance |
|
| Occlusion |
|
3.1.3 Growth Considerations
Implants placed into the jaws of growing individuals represent a significant modifying factor. Experimental studies (Thilander et al. 1992) and clinical case reports in growing patients (Oesterle et al. 1993, Johansson et al. 1994, Westwood and Duncan 1996) have shown that implants act in a similar manner to ankylosed teeth by retarding the growth of the alveolar process in the immediate vicinity of the implant. The net effect is a relative infraocclusion and/or palatoversion of the implant (Figure 1). The clinical presentations of this are not only associated with esthetic issues (mismatch of incisal edges and gingival margins between the implant restoration and the contralateral tooth) but also with functional issues where restorations move into infraocclusion.
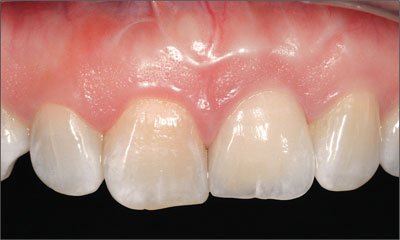
Figure 1. Three years after implant placement, there is a discrepancy in the level of the incisal edges of the implant in the 21 site and the adjacent central incisor due to dento-facial growth.
For these reasons, placement of implants should be postponed in young individuals until craniofacial/skeletal growth is complete (Koch et al. 1996). However, the growth period varies widely in children, and chronological age alone should not be used as a criterion. It has been recommended that a combination of methods be used to determine growth cessation, including serial cephalometric tracings, tooth eruption patterns within the arch (e.g., eruption of the second molar), evaluation of bodily growth in length, and evaluation of hand/wrist radiographs (Op Heij et al. 2003). It should be noted that individuals with a short or long face type may demonstrate further eruption of teeth adjacent to implants after the age of 20 years, posing a risk to esthetic and functional outcomes (Op Heij et al. 2006).
There is evidence that craniofacial growth may never cease completely, but may slowly continue throughout life (Behrents 1985). Over time, adaptive changes in tooth position may affect esthetics and function, requiring modification to or replacement of the implant-supported pros-theses in mature adults (Oesterle and Cronin 2000).
3.1.4 Iatrogenic Factors
Sub-optimal planning, as well as less-than-desirable outcomes in preceding treatment procedures, will often increase the difficulty of implant treatment phases. For example, implant placement into an upper lateral incisor site is more difficult when orthodontic treatment has failed to make sufficient space between the roots of adjacent teeth. Sub-optimal three-dimensional implant placement will also complicate the restorative process (Buser et al. 2004), and likely alter the classification for that particular presentation (Figures 2 to 7).
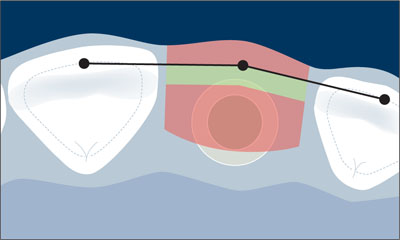
Figure 2. Schematic drawing of the orofacial comfort and danger zones.
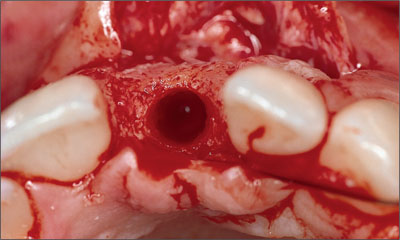
Figure 3. Occlusal view following implant bed preparation with a proper orofacial implant position and an intact facial bone wall.
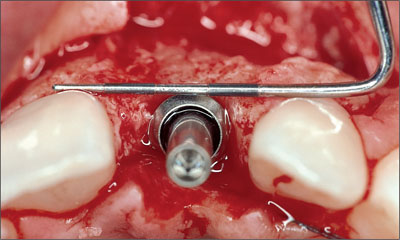
Figure 4. Periodontal probe visualizing the correct position of the implant shoulder in orofacial direction.
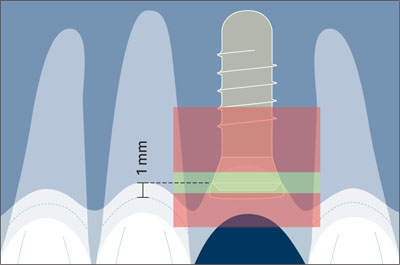
Figure 5. Comfort and danger zones in the coronoapical dimension.
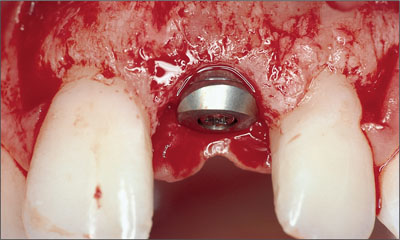
Figure 6. Correct implant placement in a coronoapical direction.
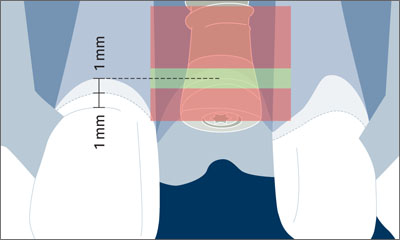
Figure 7. Schematic drawing illustrating the comfort and danger zones in the coronoapical dimension.
3.2 Esthetic Modifiers
S. Chen, A. Dawson
Esthetic issues apply where the implant restoration, and the surrounding mucosal margin, will be visible during normal functional activity or when the patient smiles. Consequently, not all implant treatments will have associated esthetic risk. This series of modifiers has been discussed in detail in “The ITI Treatment Guide, Volume 1: Implant Therapy in the Esthetic Zone – Single Tooth Replacements” (Martin et al. 2007).
Table 1 lists the factors that determine esthetic risk. This Esthetic Risk Assessment (ERA) can be used to determine the risk of a negative esthetic outcome for a particular treatment, thus assisting the clinician in determining the SAC Classification of the case. It should be noted that, by definition, a case for which there is some esthetic risk (i.e. the restoration margin is visible) would have a classification of at least Advanced.
| Esthetic Risk Factor | Level of Risk | ||
| Low | Moderate | High | |
| Medical status | Healthy, cooperative patient with an intact immune system. | Reduced immune system | |
| Smoking habit | Non-smoker | Light smoker (< 10 cigs/day) | Heavy smoker (> 10 cigs/day) |
| Patient’s esthetic expectations | Low | Medium | High |
| Lip line | Low | Medium | High |
| Gingival biotype | Low scalloped, thick | Medium scalloped, medium thick | High scalloped, thin |
| Shape of tooth crowns | Rectangular | Triangular | |
| Infection at implant site | None | Chronic | Acute |
| Bone level at adjacent teeth | ≤ 5 mm to contact point | 5.5 to 6.5 mm to contact point | ≥ 7 mm to contact point |
| Restorative status of neighboring teeth | Virgin | Restored | |
| Width of edentulous span | 1 tooth (≥ 7 mm) | 1 tooth (≤ 7mm) | 2 teeth or more |
| Soft tissue anatomy | Intact soft tissue | Soft tissue defects | |
| Bone anatomy of alveolar crest | Alveolar crest without bone deficiency | Horizontal bone deficiency | Vertical bone deficiency |
The factors listed in the ERA all affect the volume and health of the hard and soft tissues that surround implant restorations, and how these are likely to influence esthetic outcomes. An implant restoration in an esthetically demanding site can be compared to a painting in an art gallery. The surrounding soft tissues, and the bone that supports them, are analogous to the frame surrounding the painting. The overall esthetic effect of this piece of art will be enhanced by a good frame, but can be significantly degraded by a poor one. It is the same with an implant restoration.
3.2.1 Health Status
The impact of medical issues such as health status and smoking relates primarily to the predictability of the healing process. These issues have been discussed previously.
3.2.2 Esthetic Expectations
Patients’ expectations with regard to the esthetic outcome also represent a significant issue in planning esthetic cases. Patients with unrealistic demands or those whose esthetic needs are very high, may be difficult to treat as the esthetic outcome of an implant treatment may not be able to meet these expectations or needs. Patients should be fully advised as to how limitations imposed by the other factors in the ERA are likely to influence their individual outcomes, and this information must be communicated very early in the assessment and planning process. Additionally, treatment modalities other than implants should be considered if these might provide more satisfactory or predictable outcomes.
3.2.3 Smile Line
The level to which the planned implant restoratio/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


