Chapter 6
Periradicular Surgery
Aim
This chapter aims to provide the reader with guidance on case selection and a step-by-step approach to contemporary techniques used in periradicular surgery.
Outcome
Having read this chapter the reader will be aware of contemporary techniques used in periradicular surgery.
Introduction
“Periradicular surgery” is the contemporary term used to describe those surgical interventions the aim of which is to manage disease associated with endodontic and extraradicular apical infection. Disease may present at portals of exit along the length of the root relating to the apical foramen, lateral canals or even iatrogenic perforations. Cases may also involve the periodontium or be concomitant with periodontallesions. Thus the term “apicectomy”, which simply implies removal of the root end, is regarded as an oversimplification for what may be technically challenging surgery involving both periodontal and periapical hard and soft tissues. The term “orthograde” refers to conventional root canal therapy and “retrograde” implies a surgical approach to periapical disease.
In the last five years, significant changes have taken place in technique, armamentarium and materials that render periradicular surgery a more predictable treatment modality. The frequent coexistence of periapical and periodontal infection and the common principles underpinning surgical approaches to managing extraradicular infection require the periodontal surgeon to have knowledge of, and be competent in, periradicular surgery.
Orthograde Retreatment or Periradicular Surgery?
In view of the microbial basis of endodontic disease, treatment efforts (nonsurgical or surgical) must aim to eradicate this infection wherever possible. As the infection is most frequently located within the root canal system, orthograde endodontics is normally the most appropriate initial strategy and should always be carried out in the first instance. When infected canals are treated surgically, the root end restoration will simply seal over such infection and predispose to treatment failure through bacterial leakage (Fig 6-1a–c).
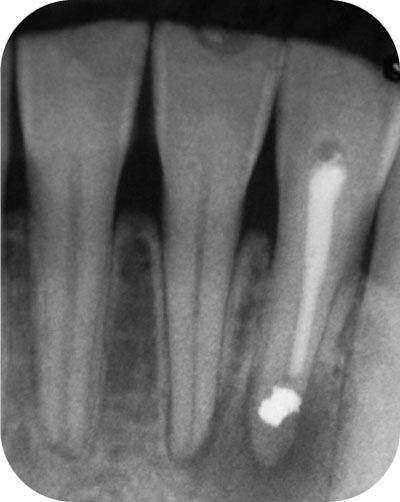
Fig 6-1a Failing surgical endodontic treatment. There is a large periapical radiolucency, an incomplete root resection and an amalgam root-end filling. The root-end filling was not continuous with the root filling.
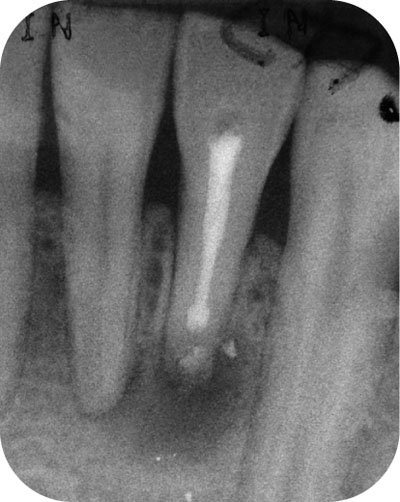
Fig 6-1b Failing surgical retreatment. A second attempt at periradicular surgery, though technically improved, has failed to resolve the apical pathology.
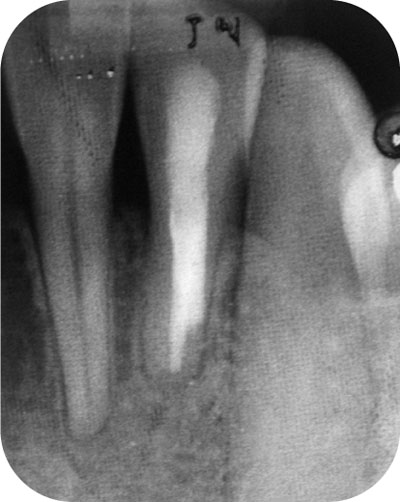
Fig 6-1c Orthograde retreatment and subsequent healing. Thorough exploration revealed a second untreated canal (common in lower incisors). Respect for basic endodontic principles will provide an environment for predictable healing in most cases.
Orthograde endodontic instrumentation and irrigation cannot always render canals free from bacteria owing to the anatomic complexity of the root canal system and the resilient nature of microbial biofilms. In some instances, apical biofilms on the external surface of the root and extraradicular infection have been demonstrated (Fig 6-2). These are clearly not amenable to orthograde root canal treatment. A key decision for the periodontist to make, therefore, is whether the existing orthograde root filling can be improved prior to adoption of a surgical approach.
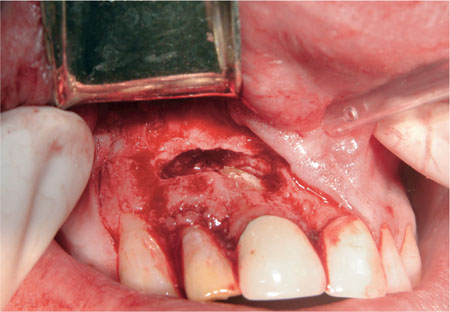
Fig 6-2 A well-organised biofilm is present apically on the external surface of the root of a central incisor. This was independent of any periodontal pocketing.
Case Selection
Indications for Periradicular Surgery
-
If orthograde retreatment is not possible.
-
Where iatrogenic errors, e.g. perforation, necessitate a surgical approach.
-
When retreatment by orthograde approach has failed.
-
If extraradicular reasons for failure are suspected:
-
infection
-
cyst
-
foreign body reaction.
-
-
Where cost/patient convenience precludes dismantling of existing restorations.
-
When previous surgical endodontics has failed owing to technical inadequacy.
Contraindications for Periradicular Surgery
As with any surgical procedure, there are a few absolute contraindications to periradicular surgery. These have been considered in previous chapters.
Holistic Restorative Treatment Planning
When contemplating periradicular surgery, some general considerations should include:
-
stability and prognosis of the remaining dentition
-
presence of untreated or unstable periodontal disease
-
use of an existing denture to which the tooth may be added, without compromising periodontal health.
Tooth-specific Assessment
-
restorability of the tooth
-
quality of existing restorations
-
local periodontal health
-
crown: root ratio
-
quality of endodontic treatment
-
whether the tooth is functional
-
-
tooth angulation.
Site-specific Surgical Contraindications
-
access
-
proximity to structures of anatomic importance
-
maxillary sinus
-
neurovascular bundles, e.g. mental nerve
-
-
bone thickness.
Alternative Treatment Options and their Predictability
-
no treatment
-
retreatment by orthograde approach
-
extraction and replacement with denture, bridge or implant
-
extract and accept resulting space.
Operator-related Factors
-
operator experience
-
time available
-
potential difficulty of case
-
accessibility of specialist endodontic services.
Patient-related Factors
-
cost
-
unrealistic expectations
-
behavioural issues that may compromise surgery or post-operative care.
Pre-surgical preparation
Where periradicular surgery is judged the most appropriate treatment modality, it is convenient to consider management in a number of phases:
-
pre-surgical endodontic treatment
-
informed consent for surgery
-
antimicrobial chemotherapy
-
analgesia.
Presurgical Endodontics
Presurgical orthograde endodontic treatment plays an extremely important role in maximising the success of periradicular surgery. As the vast majority of endodontic disease is related to root canal infection, and reduction of bacterial load through chemomechanical debridement of the canal will influence the success of, or need for, future surgical intervention, successful orthograde treatment may render surgery unnecessary.
Orthograde placement of MTA (mineral trioxide aggregate) cement at the root end may greatly simplify subsequent surgical root-end management. This technique will be discussed with “root-end filling”.
Informed Consent
Informed consent for periradicular surgery, like that for any surgical procedure, needs to include a balanced appraisal of risks and benefits along with other treatment options and their predictability.
The most likely adverse outcome of periradicular surgery is failure, necessitating eventual tooth extraction. Recent studies would suggest that between 37% and 91% of cases can expect healing. However, 80–94% of teeth treated in these studies remained in symptom-free function, even if healing was incomplete. For many patients, this may represent a successful outcome. The risk of leaving potentially infected tissues should clearly be appraised on a case-by-case basis. This would be inadvisable in certain patients, for example those with rheumatic heart disease. The high success rates of implant studies are, in particular, worthy of mention. These “success” rates are most often measured by implant survival. This may include implants with bone loss and peri-implant defects or those with restorations considered to be an aesthetic failure. If one applies similar survival criteria to surgical endodontic treatment, “success” may be comparable with, and certainly more cost-effective than, implant therapy.
The risk of gingival recession also merits particular mention. Often periradicular surgery involves tissues in the aesthetic zone and is performed around crowned teeth. Subsequent recession may lead to exposure of unaesthetic crown margins. This is particularly important where the patient has a high smile line. Whilst contemporary flap designs will minimise this risk (see later), this should be discussed with the patient as part of the informed consent process.
Analgesia and antimicrobial chemotherapy have been discussed in Chapter 1.
The Surgical Phase
-
analgesia
-
flap design, incision, reflection and retraction
-
root-end identification, osteotomy and curettage
-
root-end resection
-
crypt control
-
root-end preparation
-
root-end obturation
-
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


