Chapter 3
Surgical Management of Gingival Overgrowth
Aim
To provide a brief overview of the aetiology of gingival overgrowth, and describe the principles of and techniques for its surgical management.
Outcome
Having read this chapter, the reader should be aware of the contemporary surgical techniques used for the surgical management of gingival overgrowth. It is hoped that the reader will understand which types of gingival enlargement are amenable to surgical treatment and be aware of alternative key management strategies. The principal causes and non-surgical management of gingival overgrowth have been discussed in detail in Chapters 5 and 6 of book 43/44 in this series (Periodontal Medicine – A Window on the Body) and are beyond the scope of this chapter.
Introduction
Gingival overgrowth, gingival hyperplasia, gingival enlargement and gingival hypertrophy are terms that are used interchangeably (and incorrectly) in the literature. The term gingival overgrowth will be used for the remainder of this chapter.
Gingival overgrowth has numerous causes. These include:
-
plaque-induced inflammatory swelling
-
drug therapy
-
systemic illness
-
genetic disorders
-
other specific physiologic states.
Inflammatory changes within the gingival tissues may cause enlargement of the gingivae without apical migration of the junctional epithelial attachment. Probing depths increase as a consequence and a “false pocket” is formed. Local plaque accumulation may, in fact, allow progression to chronic periodontitis and formation of true pocketing if left untreated.
Box 3-1 lists types of gingival overgrowth that may require surgical management.
Box 3-1 Types of gingival overgrowth that may require surgical management
Hereditary gingival fibromatosis
Drug-induced gingival overgrowth
Inflammatory gingival overgrowth due to plaque accumulation secondary to:
orthodontic appliances
dentures
mouth breathing
incompetent lip seal
dental crowding
Gingival epulides
fibrous epulis
vascular epulis
giant cell epulis
Drug-induced Gingival Overgrowth
Gingival overgrowth is a well-documented and unwanted side effect, associated principally with the calcium channel blockers, phenytoin and ciclosporin (Table 3-1). The tissue enlargement begins as a painless, beadlike enlargement of the interdental papilla and can extend to involve the buccal and lingual gingival margins. The enlargement is usually generalised but the maxillary and mandibular anterior teeth are frequently the most severely affected.
| Drug Type | Uses |
| Calcium channel blockers |
|
| Phenytoin |
|
| Ciclosporin |
|
Drug-induced gingival overgrowth has two components:
-
A fibrous component which is caused by the drug (Fig 3-1).
-
An inflammatory component which is induced by plaque (Fig 3-2).
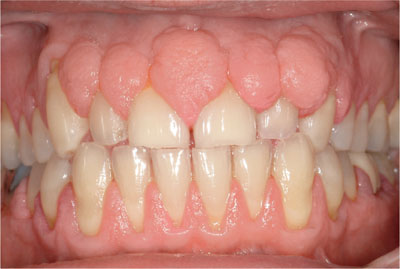
Fig 3-1 Fibrous overgrowth in a patient medicated with ciclosporin.
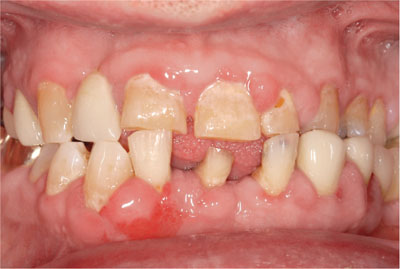
Fig 3-2 Drug-induced gingival overgrowth in a patient medicated with nifedipine. Tissues appear more vascular because of poor plaque control.
Treatment of drug-induced overgrowth and prevention of recurrence can be challenging, and the primary course of action is to attempt to remove the causative agent (drug) from the patient’s medical regime. Medical management by drug substitution is, however, not always possible in patients with severe and poorly controlled epilepsy or hypertension.
Inflammatory Gingival Overgrowth
Provision of an orthodontic appliance, especially a fixed appliance, often has a tendency to favour the accumulation of plaque around the gingival margins. This inflammation is usually transient and does not lead to attachment loss. As a result, hyperplastic tissue can lead to false pocketing around brackets and bands. This usually resolves following debonding and improvement in plaque control; surgical intervention is rarely necessary.
Low-grade, chronic irritation from an ill-fitting denture may result in an inflammatory fibrous overgrowth at the denture border. Treatment involves relieving over-extended areas of the denture. If the enlargement does not resolve, simple surgical excision is often required with subsequent provision of a new denture.
Gingival overgrowth is often seen in patients who mouth-breathe. In mouth-breathers there is increased lip separation and decreased coverage of the teeth by the upper lip (Fig 3-3). Thus there may be a decrease in saliva, which reduces the natural cleansing (plaque removal) processes. This, in turn, may contribute to increased plaque levels and subsequent gingival inflammation.
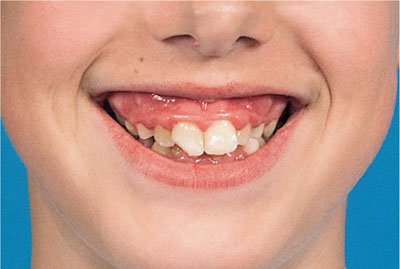
Fig 3-3 A mouth breather. Note the gingival overgrowth and high lip line.
In a crowded dentition plaque control can be more difficult, leading to plaque retention and gingival overgrowth (Fig 3-4).
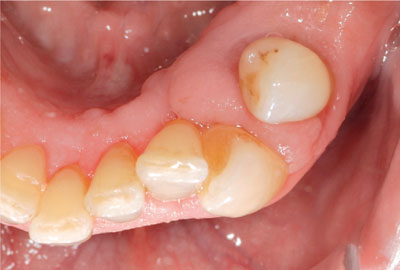
Fig 3-4 Dental crowding with gingival overgrowth. This has resulted in distal movement of the left mandibular first pre-molar.
Epulides
Epulides are benign localised enlargements of the gingival tissues that usually develop following irritation by subgingival plaque, retained by calculus or ledges on restorations. The true epulides include:
-
pyogenic granuloma (pregnancy epulis) (Fig 3-5)
-
fibrous epulis (fibroepithelial polyp)
-
giant cell epulis.
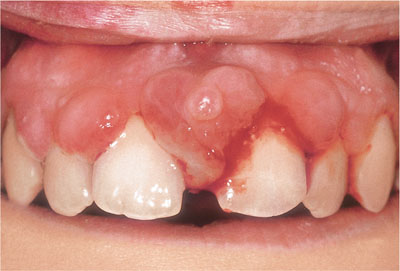
Fig 3-5 Pregnancy epulis. The tissue is highly vascular and bleeds readily.
The aetiology and non-surgical management of epulides are covered in book 43/44 in this series and are beyond the scope of this chapter. Surgical excision is by gingivectomy. Prior to excision biopsy it is important to determine whether the lesion base is sessile (broad-based) or pedunculated (narrow stem). A pedunculated lesion is more straightforward to excise but more likely to have a vascular supply, and therefore it may be more haemorrhagic. Preoperative radiographs are also essential to exclude the risk of intraosseous involvement (see later).
Hereditary Gingival Fibromatosis
Hereditary gingival fibromatosis (HGF) is a rare, benign familial condition. It is characterised by proliferative, fibrous overgrown gingivae, usually of a normal colour, firm consistency and with abundant stippling. It typically develops as an isolated disorder but can be a feature of other syndromes and is inherited as an autosomal dominant or recessive condition.
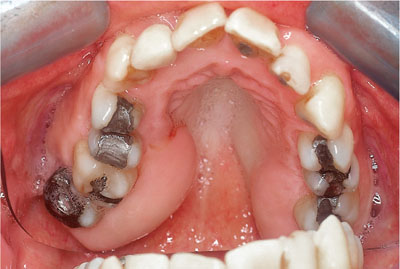
The severity of HGF varies between patients and ranges from minor localised gingival enlargement to involvement of buccal and lingual attached gingival tissues in both the mandible and the maxilla. It typically affects the maxillary tuberosity (Fig 3-6) and mandibular retromolar regions (Fig 3-7).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses