Chapter 6
Acute Presentations of Chronic Oro-Facial Pain Conditions
Introduction
Pain is a highly subjective experience and has been defined as occurring when and where the patient says it does. Pain is defined by the International Association for the Study of Pain as ‘an unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage’. It is difficult to determine a cut-off point for when acute becomes chronic pain but estimates vary from 3 to 12 months. Chronic pain conditions affecting the oro-facial region can originate from any of the multitude of tissue types present in the head and neck: vascular, nervous, muscular, bony and cartilage, amongst others.
Chronic pain conditions must start at a chronological point. They can start either insidiously, or suddenly with an acute limitation of everyday function due to the severity and urgency of the pain experienced. In the latter case, patients may present ‘acutely’ to the dental practitioner. The presentation of their complaint may be complicated by the rich sensory oro-facial peripheral innervations. Messages from the peripheral nociceptors can diverge or converge, and therefore, pain may be reported, felt and perceived, to be related to teeth or other oral structures, but may originate from another anatomical site.
The aim of this chapter is to outline the characteristics and initial management of the more common chronic oro-facial pain conditions that might present acutely to a dental emergency clinic. It is not intended to be a complete manual for the management of chronic oro-facial pain. Suggestions for further reading in the field and supportive references for the text are given at the end of the chapter.
Oro-facial pain history
Patients may describe oro-facial pain using a rich variety of terms but unfortunately the terms chosen do not always distinguish between the differing origins of the pain. What will nearly always be communicated is the particularly high intensity of oro-facial pain. The aim of this section is to give an overview of a brief oro-facial pain history and highlight some of the symptoms and characteristics of the commonly presenting chronic oro-facial pain conditions. Throughout the section it is important to bear in mind that as pain is subjective these classical descriptors, or signs, are not true in every case.
There are two issues of overriding importance to consider when taking an oro-facial pain history. The first is to ensure that the practitioner establishes a degree of empathy with the patient with regard to their complaint. The second is to establish that their complaint has legitimacy and ensure an attempt is made to provide a diagnosis, even if provisional, by the end of the consultation. A good, empathic oro-facial pain history and provisional diagnosis may have almost therapeutic effects on the level of stress and anxiety patients with oro-facial pain will experience, often due to a long and complex journey through the health service.
The history-taking format follows that described in Chapter 2. That is, to begin with the chief or presenting complaint, proceeding through the history of the presenting complaint, medical history, social history, dental history and then move onto examining the patient, remembering of course that the examination actually starts when the patient first enters the room.
Patients with oro-facial pain may report two or more interlinked chief complaints but describe them as a single complaint. If it is felt that this is the case, it is important to discuss this with the patient and clarify whether or not there are two or more definite, separate, issues/diagnoses, or that they are indeed one complaint. This will help to make taking the history of the presenting complaint easier and create less confusion in the clinician and patients’ minds. It may also make diagnosis and treatment easier. If there are indeed multiple complaints, this should be made clear in the notes by enumerating the complaints so that anyone reading the notes can quickly reference and relate findings and diagnoses to complaints.
In the history of the presenting complaint, the practitioner should specifically examine the characteristics of the pain(s) (see also Chapter 2) and as a minimum enquire about the following:
- Location, radiation and referral: Ask the patient to take one finger and point to where the pain starts, then ask them to show with that single finger where it radiates or refers to.
- Onset and duration: Specifically, how frequently is the pain occurring, or is it constant? If it is constant, are there acute exacerbations against a background of constant pain?
- Quality of pain. Ask the patient to describe the type of pain they are experiencing, e.g. stabbing, burning, aching, etc.
- Magnitude: Ask on a scale of 1–10, 10 being the worst imaginable pain, firstly where would they rank their pain generally, and secondly where would they rank it today?
- Relieving and precipitating factors.
- Diurnal and seasonal variation.
- Brief sleep history:
- Do they sleep well or do they wake excessively early?
- Does the pain wake them from sleep?
- Does the pain stop them getting to sleep?
- Is the pain worse when they wake up?
- Effects of the pain on their everyday lives: Gently and tactfully attempt to gain an understanding of the impact the pain is having on the patient’s everyday life, e.g. their job, close relationships etc. This is important, as patients with oro-facial pain can need social support with their everyday lives until the pain is controlled. Without appropriate social support from their closest family and friends, the pain may worsen in certain conditions due to increased stress and anxiety.
- Surgical therapy prior to the pain: Recent dental, medical and surgical therapy prior to this pain.
- Previous experience: Experience of this type of pain and previous treatment for it. Within this, ask the patient to list the treatments in chronological order and detail how effective they found the treatment. It is also useful to note the doses of medications they have tried previously and any side effects. Some patients may find this very difficult, and if this is the case, their family doctor or dentist should be consulted for further details.
- Systemic symptoms: When pain occurs, e.g. lacrimation, rhinorrhoea, dizziness, palpitations, weakness, nausea, vomiting, photo- or phonophobia.
- Systemic well-being: Recent weight loss, lymphadenopathy elsewhere in the body, sensory or motor deficits elsewhere, pain elsewhere in body.
If the pain history is somewhat unclear, then the use of a pain diary by the patient over a week or two might help clarify matters. This diary can be as simple or as complex as the clinician desires, some good examples can be found in the literature. It may be best to refer the patient at this stage to a specialist clinic so that the pain diary can be reviewed.
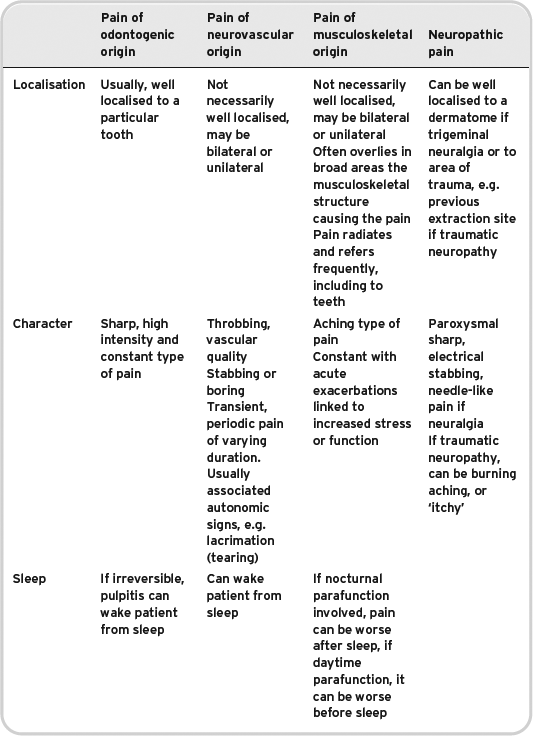
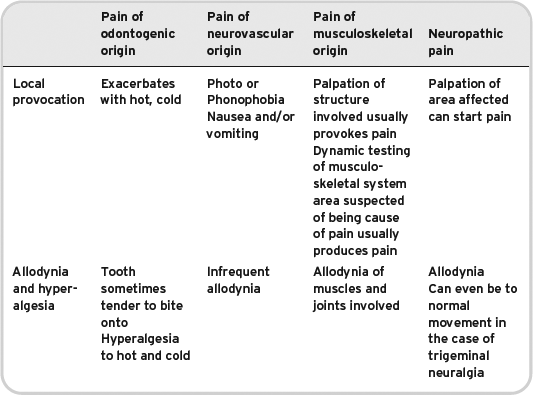
Characteristics of pain from different tissue types do differ slightly, but as one would expect there can be a large amount of crossover. To further complicate things, it is also possible to have two types of pain occurring simultaneously, or to have one type of pain exacerbating another type of pain for example, acute pulpitis exacerbating a temporomandibular disorder. Table 6.1 gives a summary of the characteristics of pain occurring from different tissue types in the oro-facial region, but as explained in the preceding sentence it is a guide rather than absolute.
Table 6.1 Characteristics of chronic oro-facial pain.
The medical history should be taken as described previously in Chapter 2, with special attention given to anything discovered in the enquiries made in the history of presenting complaint. The social history is as standard, but it may be possible at this stage to try and build an understanding of the work-life stressors and events the patient may be experiencing that may be contributory to the pain. The dental history for a patient with oro-facial pain should focus on any treatments that occurred prior to the pain, and any treatments performed for the pain.
Examination of patients with oro-facial pain
The examination should be conducted extra-orally and intra-orally as described in Chapter 2. Of specific importance in the extra-oral examination of a patient with oro-facial pain are:
- General appearance and demeanour.
- Any facial grimaces, or tics associated with pain.
- Palpation of the masticatory musculature. All muscles should be thoroughly palpated from insertion to origin to see if this palpation reproduces the patient’s pain. If the patient reports any tenderness or restriction in the neck, consideration should also be given to palpating the sternocleidomastoid muscle, posterior intrinsic muscles of the neck and trapezius.
- Palpation (auscultation) and observation of the range of movement of temporomandibular joint (TMJ), specifically examining for clicks, crepitus, deviation or restricted translation of the joint.
- Measurement of the range of movement of the TMJ (parentheses indicate normal values range):
- Protrusive (6–8 mm)
- Excursive (6–8 mm)
- Opening (40–50 mm)
- Palpation of temporal arteries.
- Lymph node examination.
- Salivary gland examination via palpation (bimanual for submandibular).
- Palpation of maxillary air sinuses extra-orally.
- Cranial nerve examination. Disturbances in cranial nerve function should always be taken seriously and fully investigated by an appropriate specialist. (See Chapter 2).
- Auriscopy (otoscopy) can be carried out if competent to do so. If not competent simply, visually inspect the auricle and the visible part of the external auditory meatus and make arrangements for someone competent to conduct an aural examination, if necessary.
- Consideration can be given to a neurological examination if competent to do so and signs and symptoms dictate.
Of specific importance in the intra-oral examination of the patient are:
- Provocation testing of any dental structures implicated by the patient’s history, e.g. palpation of ridge, percussion, or Tooth sleuth® testing of teeth.
- Thorough mucosal screening including visualisation of the oropharynx.
- Examine the patient’s occlusion. Specifically examine for gross occlusal discrepancies, e.g. a crown high in the occlusion or an overerupted tooth. If competent to do so and if it is indicated conduct a full occlusal examination including noting shim stock contacts, excursive guidance, and non-working side/working side interferences.
Red flag signs and symptoms
Patients and clinicians are justifiably concerned when acute oro-facial pain presents. Pain can often mean damage or disease. This is not always true, but there are a number of ‘red flag’ signs and symptoms associated with pain presenting oro-facially that every clinician should be aware of and take prompt action over, either by instituting expedient investigation and treatment, or seeking an urgent specialist opinion. These red flags are included in Table 6.2.
Table 6.2 Red flag signs and symptoms.
| Headache | Worrisome characteristics (SSNOOP – American Headache Society):
Systemic disease or symptoms, e.g. weight loss/gain, malaise, lymphadenopathy Secondary headache risk factors, e.g. previous history of malignancy Neurological signs or symptoms, e.g. unexplained weakness or cranial nerve dysfunction Onset abrupt – ‘thunderclap’ Older (>50 yr) and new onset headache Previous headache history or progression. First ever headache of huge severity or very sudden progression to this level Specific features of headache:
|
| Ear and nose and throat signs or symptoms | Recurrent epistaxis Anosmia Persistent nasal obstruction or purulent discharge Objective hearing loss Lymphadenopathy |
| Oral and maxillofacial signs and symptoms | Near absolute trismus precluding careful oral examination Erythroplakia, erythroleukoplakia, leukoplakia or frank ulceration of oral mucosa Cranial nerve dysfunction especially in cranial nerves five or seven Previous head and neck carcinoma Pre-auricular masses Young onset (<40 yr) trigeminal neuralgia, especially females |
Again, it must be remembered that these ‘red flags’ are not absolute. They are, however, useful to guide clinicians and if present they should be investigated and an explanation sought for them.
Special investigations for oro-facial pain
A thorough history and clinical examination will often give sufficient information to make a (clinical) diagnosis in oro-facial pain. Occasionally, the clinician will need to perform specific imaging to help exclude pathology. Dependent on the clinical presentation such imaging may include the following:
- Plain radiographs: As indicated and justified by the history and examination.
- Cone beam computed tomography of teeth: To examine features of teeth, or pathology associated with them that plain dental radiography cannot identify.
- Computed tomography of the head and neck: To exclude head and neck malignancy mimicking an oro-facial pain condition, e.g. sudden onset near absolute trismus of unknown cause in an elderly patient.
- Magnetic resonance imaging (MRI) of the head: To exclude vascular compression of the trigeminal nerve root, multiple sclerosis, or intra-cranial pathology such as tumours at the cerbellopontine angle.
It is inadvisable to perform investigations simply because of a request from a patient, especially if there is no clinical indication to do />
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


