Other conditions
Actinic prurigo (AP) A chronic, pruritic skin disease caused by an abnormal reaction to sunlight.
Amelogenesis imperfecta A rare genetic defect of enamel formation due to mutations in AMELX, ENAM, and MMP20 genes, with a wide variety of patterns. All teeth are equally affected, as are other family members. Diagnosis is from clinical features (Fig. 57.1, Table 57.1). Fluorosis, tetracycline staining, dentinogenesis imperfecta and oculodentodigital dysplasia may need to be differentiated. Management requires restorative dental care.
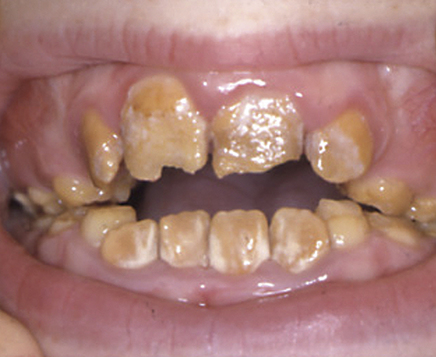
Table 57.1
| Type | 1 | 2 | 3 | 4 |
| Name | Hypoplastic | Hypocalcified | Hypomaturation | Hypomaturation with taurodontism |
| Defect | Matrix | Calcification | Maturation | Mixed – between types 1 and 3 |
| Enamel thickness and colour | Thin, hard, pitted or grooved | Normal thickness, softer and liable to attrition Discoloured white to brownish-yellow, and darkening with age |
Normal thickness, softer and liable to attrition | Variable |
| Radiographic features | Normal enamel density | Enamel similar to dentine | ||
| Inheritance | AD, AR or x | AD or AR | AD, AR or x | AD |
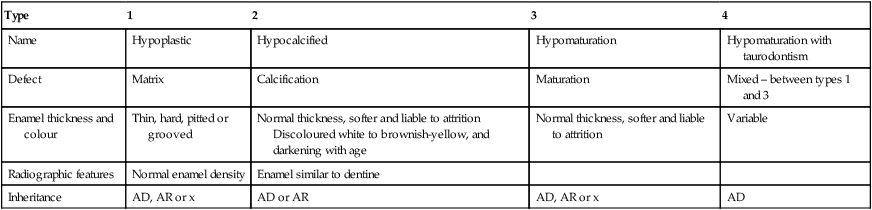
AD = autosomal Dominant, AR= autosomal recessive, X = X-linked
Diagnose from biopsy; blood picture; raised ESR, CRP or PV and marrow biopsy; serum proteins and electrophoresis; urinalysis (Bence–Jones proteinuria: Ch. 56); skeletal survey for myeloma. Manage by chemotherapy (melphalan, corticosteroids or fluoxymesterone).
Angiomyoma A rare benign hamartoma involving blood vessels and muscle.
Cheek biting (morsicatio buccarum) Common and seen in adults mainly, especially anxious patients, and those with other psychologically related disorders, e.g. temporomandibular pain–dysfunction syndrome, it is also rarely caused by self-mutilation, seen in psychiatric disorders, learning disability, Lesch-Nyhan syndrome (Ch. 56) and some rare syndromes with insensitivity to pain. Abrasion of the superficial epithelium leaves whitish fragments on reddish background. The lesions are invariably restricted to the lower labial mucosa and/or buccal mucosa near the occlusal line on one or both sides.
Congenital epulis A rare reactive process seen on the alveolus of a neonate.
Cyst A pathological cavity having liquid, semi-liquid or gaseous contents. It is frequently, but not always, lined with epithelium. Cysts of the jaws mostly arise from odontogenic epithelium, and are relatively common lesions (Ch. 45). Non-odontogenic developmental cysts are uncommon and were said to form from entrapment of epithelium during the fusion of embryological processes, but this embryological concept has now been discarded. The lining of these cysts is either stratified squamous epithelium or pseudostratified ciliated columnar (respiratory) epithelium. Non-odontogenic cysts include the following:
 Nasopalatine or incisive canal cysts: derived from the vestigial oronasal ducts. They may occur either within the nasopalatine canal, or in the soft tissues of the palate at the opening of the canal, grow slowly, and may discharge into the mouth giving a salty taste. Radiological examination shows a well-defined, rounded ovoid or occasionally heart-shaped defect in the anterior maxilla. Nasopalatine cysts must be distinguished from a normal large anterior palatine fossa which may be up to 7 mm in diameter, and from radicular cysts associated with the maxillary incisors. These cysts should be enucleated and seldom recur.
Nasopalatine or incisive canal cysts: derived from the vestigial oronasal ducts. They may occur either within the nasopalatine canal, or in the soft tissues of the palate at the opening of the canal, grow slowly, and may discharge into the mouth giving a salty taste. Radiological examination shows a well-defined, rounded ovoid or occasionally heart-shaped defect in the anterior maxilla. Nasopalatine cysts must be distinguished from a normal large anterior palatine fossa which may be up to 7 mm in diameter, and from radicular cysts associated with the maxillary incisors. These cysts should be enucleated and seldom recur.
 Nasolabial cysts: soft tissue cysts found within the nasolabial fold. They are lined by respiratory epithelium, and if allowed to grow may distort the upper lip and alar base. Treatment is by simple excision.
Nasolabial cysts: soft tissue cysts found within the nasolabial fold. They are lined by respiratory epithelium, and if allowed to grow may distort the upper lip and alar base. Treatment is by simple excision.
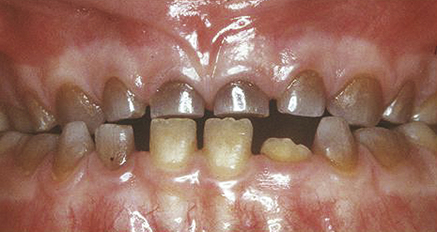
Dentinogenesis imperfecta A rare autosomal-dominant disorder in which the dentine is abnormal in structure and, hence, translucent (Fig. 57.2), and poorly attached to enamel. All teeth are affected, but primary teeth are more severely affected than permanent teeth. In the permanent dentition the teeth that develop first are generally more severely affected than those that develop later. The teeth:
 may vary in colour from grey to blue or brown
may vary in colour from grey to blue or brown
 enamel is poorly adherent to the abnormal underlying dentine and easily chips and wears
enamel is poorly adherent to the abnormal underlying dentine and easily chips and wears
 crowns are bulbous with pronounced cervical constriction and the roots are short
crowns are bulbous with pronounced cervical constriction and the roots are short
 fracture easily (there is progressive obliteration of pulp chambers and root canals with secondary dentine)
fracture easily (there is progressive obliteration of pulp chambers and root canals with secondary dentine)
There are three types of dentinogenesis imperfecta:
 Type I (associated with osteogenesis imperfecta): most severe in deciduous dentition; bone fractures; blue sclerae; progressive deafness; caused by mutations in one of several genes.
Type I (associated with osteogenesis imperfecta): most severe in deciduous dentition; bone fractures; blue sclerae; progressive deafness; caused by mutations in one of several genes.
 Type II (hereditary opalescent dentine): defect equal in both dentitions; caused by mutations in the DSPP gene. A few families with type II have progressive hearing loss in addition to dental abnormalities.
Type II (hereditary opalescent dentine): defect equal in both dentitions; caused by mutations in the DSPP gene. A few families with type II have progressive hearing loss in addition to dental abnormalities.
 Type III (Brandywine type – first identified in Brandywine, Maryland, USA): associated with occasional shell teeth and multiple pulpal exposures; caused by mutations in the DSPP gene.
Type III (Brandywine type – first identified in Brandywine, Maryland, USA): associated with occasional shell teeth and multiple pulpal exposures; caused by mutations in the DSPP gene.
 mucocutaneous disorders, usually. Most gingival involvement in the vesiculobullous or skin diseases (dermatoses) is related to lichen planus or pemphigoid, but pemphigus, dermatitis herpetiformis, linear IgA disease, chronic ulcerative stomatitis and other conditions may need to be excluded. Most of these conditions are acquired, but a few are congenital with a strong hereditary predisposition, such as epidermolysis bullosa
mucocutaneous disorders, usually. Most gingival involvement in the vesiculobullous or skin diseases (dermatoses) is related to lichen planus or pemphigoid, but pemphigus, dermatitis herpetiformis, linear IgA disease, chronic ulcerative stomatitis and other conditions may need to be excluded. Most of these conditions are acquired, but a few are congenital with a strong hereditary predisposition, such as epidermolysis bullosa
 chemical damage, such as reactions to sodium lauryl sulphate in toothpastes
chemical damage, such as reactions to sodium lauryl sulphate in toothpastes
 reactions to mouthwashes, chewing gum, medications and dental materials
reactions to mouthwashes, chewing gum, medications and dental materials
The treatment of desquamative gingivitis consists of:
 minimizing irritation of the lesions
minimizing irritation of the lesions
 specific therapies for the underlying disease where available
specific therapies for the underlying disease where available
 local or systemic immunosuppressive or dapsone therapy, notably corticosteroids.
local or systemic immunosuppressive or dapsone therapy, notably corticosteroids.
Corticosteroid creams used overnight in a soft polythene splint may help.
Dilated pupils (mydriasis) Can be caused by parasympathetic lesions affecting the third nerve, Holmes–Adie syndrome (Ch. 56), Horner syndrome (Ch. 56), anticholinergic drugs (e.g. atropine or similar drugs), sympathomimetic drugs (e.g. adrenaline, cocaine). Users of cocaine or crack cocaine may thus have dilated pupils.
 behavioural problems (including theft)
behavioural problems (including theft)
 oral lesions typically are those of these conditions or neglect of hygiene.
oral lesions typically are those of these conditions or neglect of hygiene.
Exfoliative cheilitis (tic de levres) An uncommon condition affecting the lip vermilion, characterized by continuous production and desquamation of unsightly, keratin scales which, when removed, leave a normal lip beneath (Fig. 57.3). The aetiology is unknown, but some cases may be factitious.
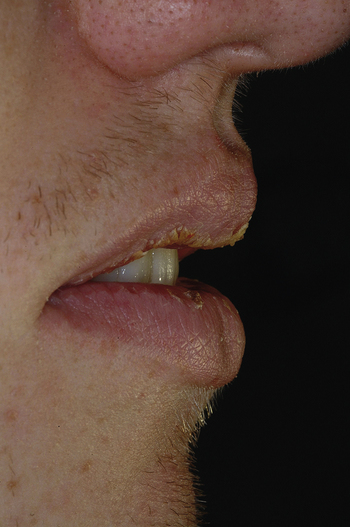
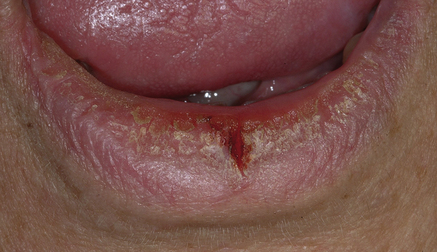
Fissured lip Lip fissures may appear especially where there is exposure to adverse environments (Fig. 57.4), or where the lip swells as in Down syndrome (Ch. 56) or cheilitis granulomatosa (Ch. 46).
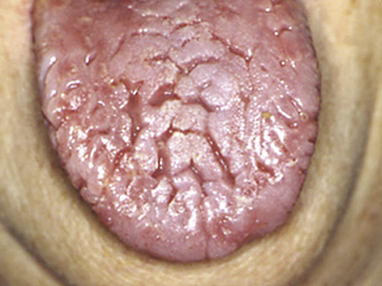
Fissured (plicated or scrotal) tongue An extremely common genetic condition, the dorsum has deep irregular fissures, but is normally papillated (Fig. 57.5). A fissured tongue may also be seen in Down syndrome or Melkersson–Rosenthal syndrome (Ch. 56). There are associations with erythema migrans in particular. The diagnosis is usually clear cut. The lobulated tongue of Sjögren syndrome (Ch. 50) must be differentiated.
 Mildest form: white flecks or spotting or diffuse cloudiness.
Mildest form: white flecks or spotting or diffuse cloudiness.
 More severe form: yellow-brown or darker patches.
More severe form: yellow-brown or darker patches.
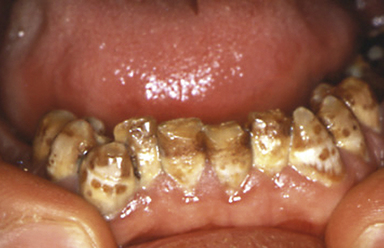
 Most severe form: yellow-brown or darker patches, sometimes with pitting (Fig. 57.6).
Most severe form: yellow-brown or darker patches, sometimes with pitting (Fig. 57.6).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses





















