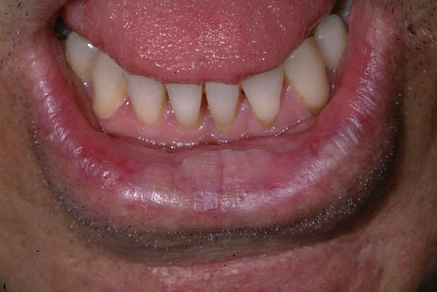
Actinic cheilitis (solar cheilosis)
CLINICAL FEATURES
Actinic cheilitis is most common on the lower lip, with sparing of the oral commissures. In the early, acute stages, the lip may be red and oedematous, but after months or years (chronic cheilitis) may become dry and scaly and wrinkled with grey to white changes. Lesions may appear as a smooth or scaly, friable patch or can involve the entire lip later, becoming palpably thickened with small greyish white plaques (Fig. 26.1). Eventually, warty nodules may form, which may evolve into OSCC.
DIAGNOSIS
A careful history and a biopsy are indicated (Table 26.1). Lupus erythematosus and lichen planus must also be considered in the differential diagnosis.
Table 26.1
Aids that might be helpful in diagnosis/prognosis/management in some patients suspected of having solar cheilosis*
| In most cases | In some cases |
| Biopsy | Dermatological opinion |
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses