46
Luting Techniques
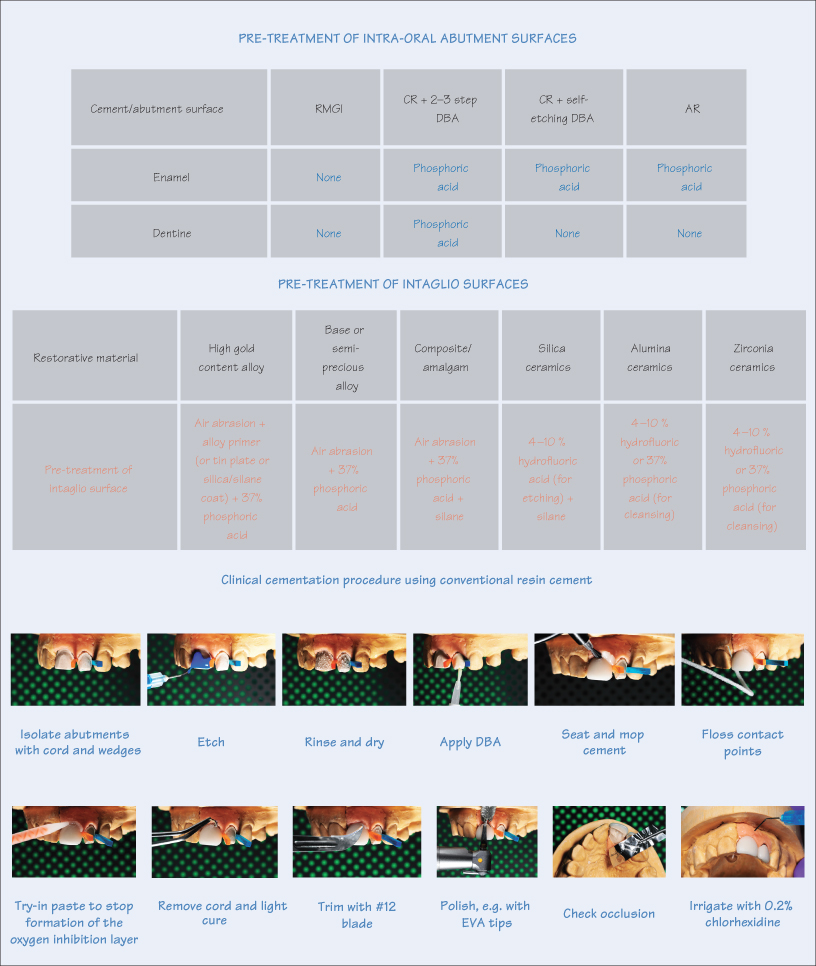
The performance of any cement depends on clinical factors, pre-treatment of the indirect restoration intaglio surface, and the intra-oral abutment. The cementation technique is both time-consuming and exacting, and any omissions will compromise the durability and long-term survival of the restoration.
Clinical Factors
Clinical performance of cements is influenced by:
- Operator variables – mixing, dispensing and loading cement, accounting for more than 50% of all risk factors;
- Tooth preparation design – ideal 8° convergence angle and adequate resistance form;
- Material properties – accounting for approximately 5% of risk factors;
- Location of tooth – anterior or posterior;
- Patient factors – oral hygiene.
Pre-Treatment of Intra-Oral Abutment
Pre-conditioning of the intra-oral abutment starts by removing the temporary cement, which is accomplished mechanically using hand instruments, rotraty plastic burs (OptiClean, KerrHawe SA, Switzerland) air abrasion, pumice paste or ultrasonic devices. Total removal is essential to avoid compromising the bond strength between the natural tooth substrate (or artificial abutment, e.g. intraradicular post/cores or implant abutments) and the definitive cement.
The next stage is isolation, either with rubber dam or intrasulcular gingival retraction cords. An arid environment is essential for resin-based cements, but less critical for RMGI. Rubber dam is the ideal choice for cementing inlays in posterior teeth, but is unsuitable for anterior teeth since the retaining metal clamps can potentially traumatise the gingival margin, leading to recession, especially on anterior teeth with thin periodontal biotypes. Gingival retraction cord, dry or impregnated with an astringent, not only allows visualisation of the abutment margins, but also acts as a physical barrier to avoid excess cement entering the delicate gingival sulcus. However, retraction cord may be inappropri/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


