MAIN OROFACIAL PROBLEMS
TEETH
Trauma
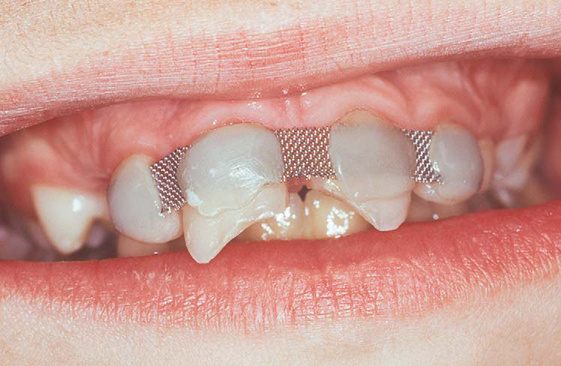
Trauma is common in severe learning disability, severe epilepsy and in abused and vulnerable individuals (Figs 4.1, 4.2). Learning disabilities, cognitive impairment, delirium (common among the acutely ill/frail elderly), and dementia (occurring in as many as 50% of institutionalised elderly) represent serious barriers to trauma and pain assessment. Management of trauma in these special needs groups should involve a coordinated team approach, where carers, and other health care professionals, such as general medical practitioners, may be able to assist in ensuring the correct diagnosis is made and appropriate treatment is offered.
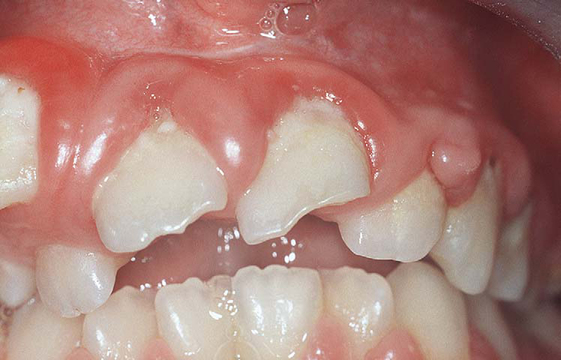
Tooth wear
Attrition (Fig. 4.3) is common (especially in males), where the diet is very coarse, where there is bruxism, or where the teeth are defective, as in dentinogenesis imperfecta or Ehlers–Danlos syndrome. Furthermore, tooth wear may be more common in individuals with intellectual disabilities. Restorative procedures may be needed, including composites and advanced restorative techniques.
Caries
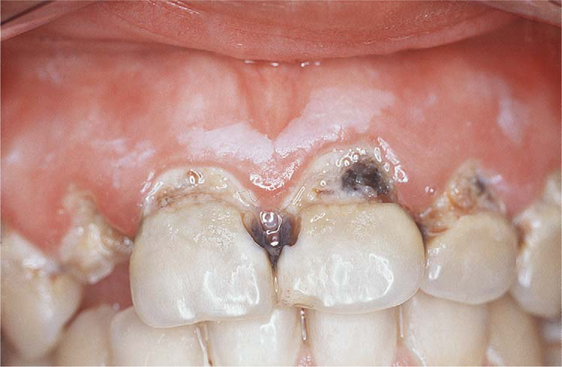
Higher levels of dental caries may be present in some individuals with special needs (Fig. 4.4), with the level of risk dependent on a complex interrelationship between socioeconomic factors and access to oral health care, concurrent illness and its treatment. Examples of factors which may increase caries risk include:  xerostomia due to Sjögren’s syndrome, radiotherapy, or secondary to the use of tranquilisers or other psychoactive anticholinergic drugs
xerostomia due to Sjögren’s syndrome, radiotherapy, or secondary to the use of tranquilisers or other psychoactive anticholinergic drugs  medications containing sugar
medications containing sugar  special diets, including those that require frequent snacking
special diets, including those that require frequent snacking  poor motor control of the cheeks, lips and tongue
poor motor control of the cheeks, lips and tongue  dysfunction in the arms and hands
dysfunction in the arms and hands  general debilitation/poor motivation due to concurrent illness or chronic depression.
general debilitation/poor motivation due to concurrent illness or chronic depression.
Erosion
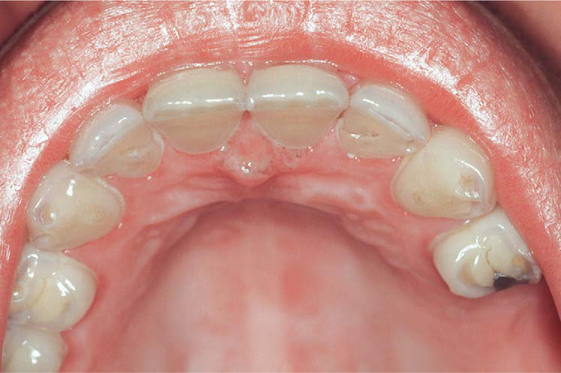
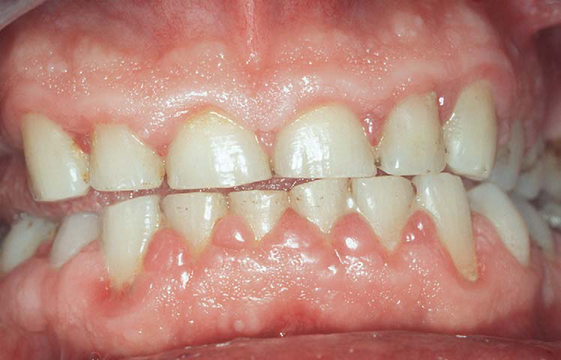
Frequent exposure to acidic substances may result in the loss of enamel from the tooth surface by chemical erosion (Fig. 4.5). Erosion may be the result of intrinsic or extrinsic sources of acid.
PERIODONTIUM
Salivary glands
Drooling
 Behavioural approaches where appropriate, such as ‘anti-drooling lessons’.
Behavioural approaches where appropriate, such as ‘anti-drooling lessons’.
 Physiotherapy approaches, such as a modified Andreasen monobloc appliance, Innsbruck Sensory Motor Activators and Regulators (ISMARs) or the Castillo–Morales technique where a palatal appliance encourages lip and tongue control.
Physiotherapy approaches, such as a modified Andreasen monobloc appliance, Innsbruck Sensory Motor Activators and Regulators (ISMARs) or the Castillo–Morales technique where a palatal appliance encourages lip and tongue control.
 Orthodontics may be indicated if incompetent lips are a possible cause.
Orthodontics may be indicated if incompetent lips are a possible cause.
 Antisialogogues may be of some benefit and include:
Antisialogogues may be of some benefit and include:
• Atropinics such as benztropine or benzhexol which are theoretically useful to control sialorrhoea, although many, such as scopolamine (hyoscine) or ipatropium bromide, are of little practical value because of adverse effects. However, transdermal scopolamine using dermal patches has been shown to be effective within 15 minutes, and lasts up to 72 hours. Itching under the patch and flushing appear to be the main adverse effects.
• Glycopyrrolate, a quaternary ammonium compound with anticholinergic effects, has minimal side effects to the central nervous system because it penetrates the blood–brain barrier poorly yet has a long-lasting antisialogogue effect. Oral glycopyrrolate 0.4 mg 3× daily is effective in many adults with sialorrhoea though it may cause some flushing and urinary retention.
• Antihistamines are sometimes used. Propantheline bromide 15-30 mg may be effective but is contraindicated in glaucoma, myasthenia gravis and bowel or bladder obstruction. Methantheline is an alternative.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


 gastro-oesophageal reflux, which may be due to sphincter incompetence, increased gastric pressure (due to obesity) and increased gastric volume
gastro-oesophageal reflux, which may be due to sphincter incompetence, increased gastric pressure (due to obesity) and increased gastric volume  vomiting (due to pregnancy, eating disorders)
vomiting (due to pregnancy, eating disorders)  rumination.
rumination. dietary acids, such as carbonated beverages, alcoholic drinks and citrus foods
dietary acids, such as carbonated beverages, alcoholic drinks and citrus foods  medication such as vitamin C and iron preparations, ecstasy, anti-asthmatic medication and excessive aspirin
medication such as vitamin C and iron preparations, ecstasy, anti-asthmatic medication and excessive aspirin  some mouthwashes and saliva substitutes that are also acidic
some mouthwashes and saliva substitutes that are also acidic  environmental contact with acids as part of work or leisure activities.
environmental contact with acids as part of work or leisure activities.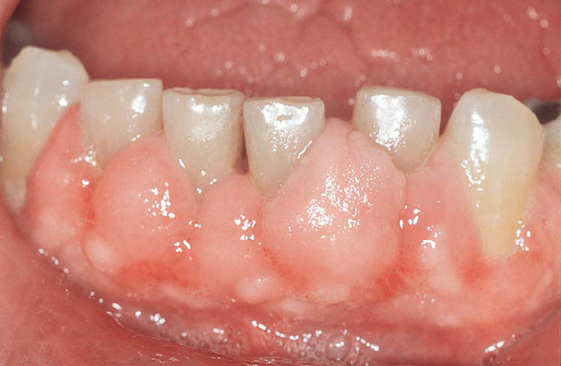
 food
food  local factors such as teething or oral inflammatory lesions
local factors such as teething or oral inflammatory lesions  physiological factors such as menstruation or early pregnancy
physiological factors such as menstruation or early pregnancy  digestive origin, both functional (motility disorders and oesophageal spasm) and organic pathology (ulcers, hiatus hernia)
digestive origin, both functional (motility disorders and oesophageal spasm) and organic pathology (ulcers, hiatus hernia)  medications (those with cholinergic activity such as pilocarpine, tetrabenazine, clozapine or bethanecol)
medications (those with cholinergic activity such as pilocarpine, tetrabenazine, clozapine or bethanecol)  nasogastric intubation.
nasogastric intubation. neuromuscular dysfunction: as a result of muscular
neuromuscular dysfunction: as a result of muscular poor lip seal and malocclusion, usually linked to learning disability
poor lip seal and malocclusion, usually linked to learning disability  abnormal head position as seen in progressive bulbar palsy
abnormal head position as seen in progressive bulbar palsy  pharyngeal or oesophageal obstruction, such as by a neoplasm.
pharyngeal or oesophageal obstruction, such as by a neoplasm.
