Diagnosis and treatment planning
A diagnosis of irreversible pulpitis was reached for the 36.
What were the potential treatment options for the patient?
- Leave alone.
- Root canal treatment.
- Extraction.
The patient was keen to retain her tooth. Therefore, it was decided to confirm the restorability of the tooth prior to proceeding with root canal treatment.
Treatment
The existing composite restoration was removed under local anaesthetic and rubber dam, and the restorability of the tooth was confirmed. However, achieving complete anaesthesia proved to be difficult, and it was not possible to proceed with pulp extirpation at that visit. The tooth was dressed with a sedative (antibiotic and steroid) dressing, and another appointment scheduled. At the second appointment, a ‘direct’ inferior alveolar nerve block (IANB) (3% mepivicaine ‘plain’) was given together with a second ‘higher’ IANB (4% articaine; 1 in 200,000 epinephrine). After a 10 minute wait for the onset of anaesthesia, an additional intra-osseous injection (4% articaine; 1 in 200,000 epinephrine) was given. This provided suitable anaesthesia, and treatment was commenced.
The root canals were identified and instrumented, thus eliminating possible difficulties with anaesthesia at subsequent visits. The tooth was dressed with calcium hydroxide, and the patient scheduled to return in 2 weeks. At the third visit, her symptoms had completely resolved, and gaining anaesthesia did not present any problems. The root canal treatment was successfully completed (Figure 4.3.2a). At the 12 month review, the patient was asymptomatic and the tooth was functional (Figure 4.3.2b).
Figure 4.3.2 (a) Post-operative periapical radiograph of molar 36, (b) periapical radiograph of the 36 taken at 12 months. The tooth is functional and radiographically the periapical tissues are within normal limits.
(a) 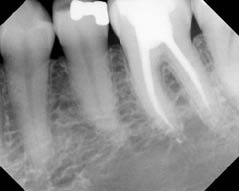 (b)
(b) 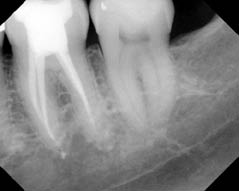
Discussion
A stressful aspect of endodontic treatment, for both clinician and patient, is when it proves impossible to painlessly instrument the root canal system. When this occurs, the clinician is struggling to be in control of the clinical situation and a successful treatment outcome is jeopardized. This case highlights the difficulties in achieving predictable pulpal anaesthesia in teeth with irreversible pulpitis, particularly in lower molars.
It is essential to appreciate the neurophysiology of the pulp to understand why anaesthesia may be difficult to achieve.
What nerve fibres supply the pulp?
The trigeminal nerve supplies the teeth and the oral structures with sensation. This nerve consists of three divisions: the ophthalmic, maxillary and mandibular. The maxillary and mandibular divisions supply sensation to the maxillary and mandibular teeth respectively. In the dental pulp, the primary afferent pain-conducting (nociceptive) nerve fibres are A∂ and C fibres (Table 4.3.1). These nerve fibres (axons) have peripheral nerve endings in the dentine-pulp complex and the periodontal ligament. The cell bodies of the primary afferent axons are found in the trigeminal ganglion, and the central nerve endings of the primary axons synapse with second order neurones in the trigeminal sensory nucleus within the brain stem.
Table 4.3.1 A summary of the differences between A∂ and C fibres
| A∂ fibres | C fibres | |
| Sensation | Sharp/pricking | Dull aching pain |
| Stimulating factors | Mainly noxious mechanical stimuli | Mechanical, thermal, chemical |
| Myelin sheath | Yes | No |
| Conduction speed | Fast (10 m/sec) | Slow (1 m/sec) |
| Transportation of neuropeptides via axoplasm | No | Yes |
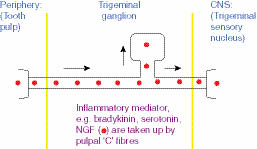
In severe pulpal inflammation, chemical mediators of inflammation such as bradykinin, serotonin and nerve growth factor (NGF) are produced in the dental pulp. These are taken up by the pulpal termini of unmyelinated C fibres and transported within the axoplasm, up to the cell body in the trigeminal ganglion and onwards to the central termini of the axons in the trigeminal sensory nucleus (Figure 4.3.3). The transportation of the neuropeptides is slow, in the order of 1–2 mm per day. These neuropeptides induce endogenous neuropeptide production (e.g. substance P, calcitonin gene related peptide) within the cell body of C fibres in the trigeminal ganglion. The endogenous neuropeptides are then ’exported’ away from the ganglion to the peripheral axon termini and centrally to the trigeminal sensory nucleus (Figure 4.3.4). These changes occur over several days and greatly increase the ‘barrage’ of nociceptive information arriving at the trigeminal sensory nucleus from the inflamed pulp. This may explain the time taken for the characteristic symptoms (an irreversible pulpitis) to develop.
Figure 4.3.3 At the trigeminal ganglion, the chemical mediators of inflammation induce the production of neuropeptides within the cell body of the C fibre. These neuropeptides are then exported from the ganglion, in both a retrograde manner, to the peripheral terminus in the pulp, and in an anterograde manner, to the trigeminal sensory nucleus.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


