Chapter 39 Mandibular Donor Block Bone Grafts: Symphysis and Ramus
INTRODUCTION
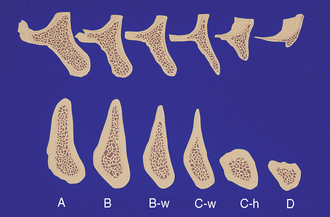
Treatment plans in implant dentistry in the 1980s often used existing bone volume to determine the location and type of implant abutment. In abutment bone (Division A), root forms were inserted; in bone of moderate width (Division B), blade implants were placed; and in inadequate height of bone (Division C-h), subperiosteal implants were the treatment options (Figure 39-1). Today, the final prosthesis type and design is first determined, followed by the ideal implant position, number, and size. Often the bone available is inadequate to perform the ideal, predictable treatment and build a proper foundation. As a consequence, bone grafting has become a more frequent modality to achieve long-term success.
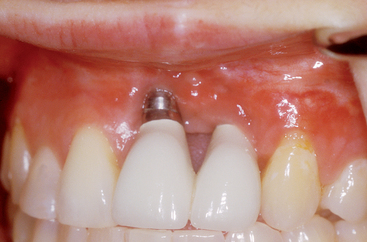
In addition to the biomechanical and functional needs of a prosthesis, there are often esthetic considerations. Bone grafting is often necessary to place the implant in the proper location for an ideal esthetic result. The soft tissue drape often needs enhancement in the esthetic zone. The bone foundation sets the tone for the soft tissue drape (Figure 39-2). Therefore when ideal crown contours (FP-1) and soft tissue are desired, bone augmentation is often an important aspect of the treatment.
As a result of biomechanical-based foundations and esthetic desires, a primary diagnostic consideration for implant prostheses is the available bone in the edentulous span. The placement of endosteal dental implants requires adequate bone volume at the desired locations for ideal prosthetic support. If inadequate bone exists, several surgical techniques may be used to reconstruct the deficient ridge for implant placement. The number of key factors present and the geometry of a bony defect are important considerations in the selection of a modality for ridge augmentation.1 The fewer the number of remaining bony walls, the greater the need for osteopromotive techniques. Although allografts and guided bone regeneration techniques have been used predictably in slight-to-moderate bone regeneration (primarily for inadequate width), these methods have limitations and have been found to produce less favorable results in the treatment of larger bone deficiencies.2–13 Autologous cortical/trabecular bone grafts may be considered the gold standard in the repair of moderate to severe alveolar atrophy and bone defects.14–28
The use of iliac crest autologous bone blocks with osteointegrated implants was originally presented in the literature by Bränemark et al.29 and is now a well-accepted procedure in oral and maxillofacial rehabilitation. Although the iliac crest is often used in major jaw reconstruction for implants,30–34 it has the disadvantages of higher costs, alteration of ambulation, and the need for hospitalization and general anesthesia.35
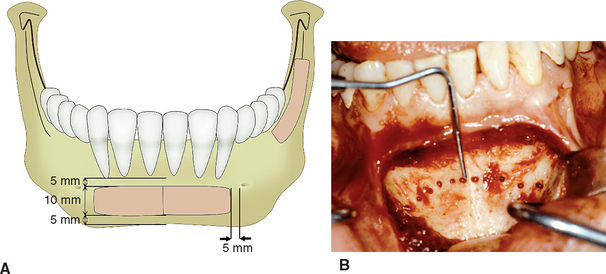
Mandibular symphysis donor site grafts were originally published to correct intraoral birth defects, such as cleft palates.36,37 Misch et al. extended the indications with mandibular symphysis and ramus block bone grafts for use of endosteal dental implants in 1992 (Figure 39-3).38 In the repair of more localized alveolar defects, cortical bone grafts from the mandible offer several benefits.20,38–41 The obvious advantage of intraoral versus extraoral donor grafts is their convenient surgical access. The proximity of donor and recipient sites can reduce operative and anesthesia time, making them ideal for outpatient implant surgery. There is no cutaneous scar associated with extraoral donor sites. In addition, patients report minimal donor site discomfort, and these areas may offer a decreased morbidity from graft harvest compared with extraoral locations.19,20,38–45
Bone harvested from the maxillofacial region appears to have inherent biological benefits for augmentation. Research suggests that this may be attributed to the embryologic origin of the donor bone.43,46–51 The majority of bones in the skeleton are of endochondral origin (from a cartilaginous precursor). With the exception of alveolar bone, the maxilla and body of the mandible develop intramembranously, whereas the condyles develop by endochondral bone formation.52 Experimental evidence has shown that grafts from membranous bone show less resorption than endochondral bone.46,47,49,53–56 Although cancellous grafts revascularize more rapidly than cortical grafts,14 cortical membranous grafts revascularize more rapidly than endochondral bone grafts with a thicker cancellous component.48,57
Early revascularization of membranous bone grafts has been suggested as an explanation for the improved maintenance of graft volume.48,56–58 Another hypothesis is that bone of ectomesenchymal origin, such as the mandible, has a better potential for incorporation in the maxillofacial region because of a biochemical similarity in the protocollagen of the donor and recipient bone.60 However, more recent research suggests that grafted bone, independent from its embryogenic origin, will mimic the properties of the recipient bone.60 The inductive capacity of cortical grafts is explained by their higher concentration of bone morphogenetic proteins,61–63 and bone from the maxillofacial skeleton contains increased concentrations of growth factors, which may lead to a greater capacity for bone repair and graft retention.64 Another hypothesis is that the improved survival of craniofacial bone grafts is simply caused by their three-dimensional structure.65,66 Because these grafts have a thicker cortical layer, they resorb more slowly.53,54,57,67
An emphasis has been placed on the transplantation of viable osteoprogenitor cells from trabecular marrow grafts.18 The concept has been that the majority of osteoblasts are present in trabecular bone. Because these cells are responsible for the formation of new bone, it is logical that trabecular grafts are advantageous. However, because of the significant resorption associated with corticocancellous block grafts from endochondral donor sites, these have lost favor in the treatment of mandibular continuity defects and ridge augmentation for soft tissue-borne prostheses.16,18,55–57,68,69 It has been observed by Misch and others that the cortical/trabecular blocks harvested from the ilium have greater bone volume after initial healing compared with inlay trabecular grafts.57 In addition, when endosteal implants are inserted within the first year, the bone is maintained long term. It appears the microarchitecture of the bone graft (cortical versus trabecular) and implant insertion to stimulate the bone is more important than whether the bone graft is from endochondial or mesenchymal origin.
Mandibular donor bone grafts, which are primarily cortical bone, exhibit little volume loss and show good incorporation at short healing times.57 There are more mature bone cells (osteocytes) in the cortical bone, more growth factors, including insulin-like growth factors 1 and 2, and more bone morphogenetic protein. As important, the cortical bone acts like a barrier membrane and prevents resorption of the graft site. This permits the blood vessels from the host bone to invade the graft and bring osteoblasts into the graft along the sides of the invading blood vessels.
The cortical bone has more growth factors to encourage blood vessel growth from the host bone, including transforming growth factors. There are at least 50 known growth factors in this category (which includes bone morphogenetic proteins). Vascular endothelial growth factor is also present, which contributes to new blood vessel growth. Implant placement shortly after graft incorporation has a stimulating effect on the bone, maintaining the augmented bone volume and preventing further loss.70–73 In addition, the dense structure of the cortical portion of the graft offers the benefit of improved implant stability during placement and healing and may even improve interfacial stress transmission upon implant loading.74–76
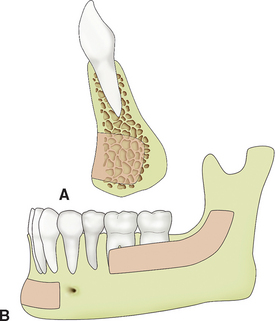
Over the years, intraoral cortical/trabecular block bone grafts have been used for residual bone augmentation prior to implant placement with extremely favorable results.19–23,25,26,38–45,77–92 Block-type grafts may be harvested from the residual ridge, mandibular symphysis, body, or ramus area (Figure 39-4). Donor grafts may be harvested from the symphysis region of the edentulous mandible while placing implants in the region, provided there has been minimal atrophy. Implant placement in the lower jaw is then limited to the available bone superior to the graft harvest or postponed until healing of the donor site has occurred. The amount of bone available in many cases is limited only by the imagination of the surgeon. However, a common mistake in comprehensive treatment planning is to overestimate the volume of attainable bone graft from intraoral donor sites. It is prudent to consider extraoral donor sites for grafting alveolar defects, when more than a four-tooth span must be augmented (especially when height augmentation is required).
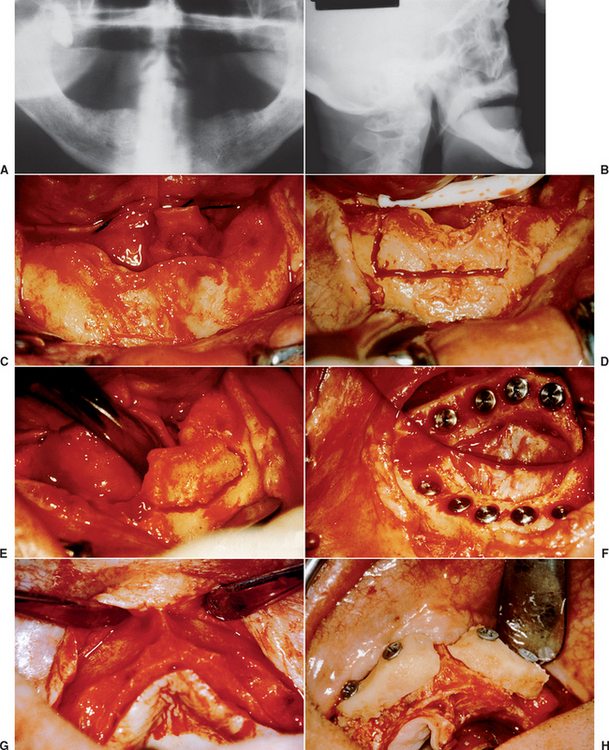
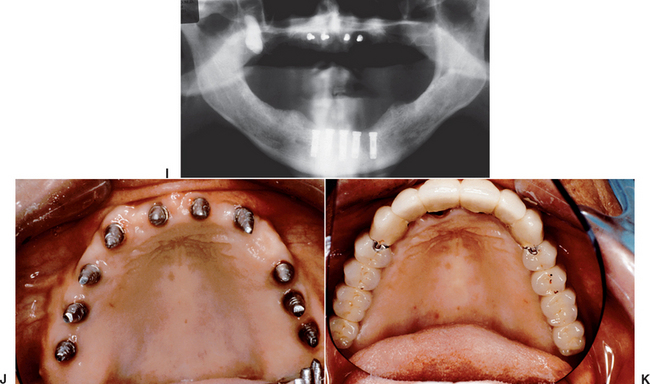
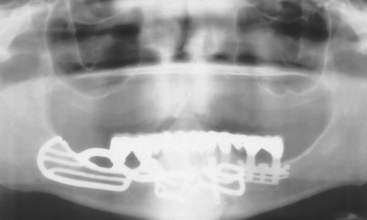
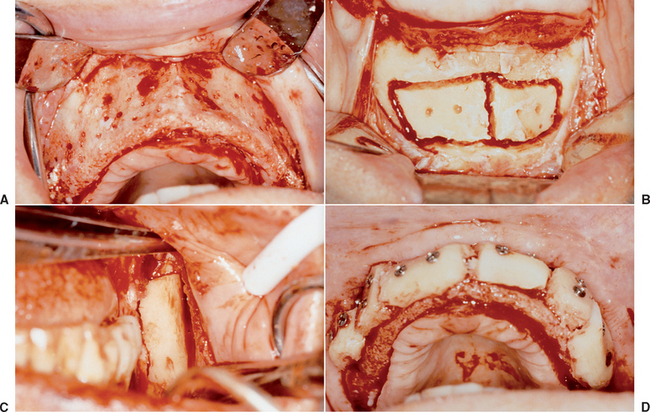
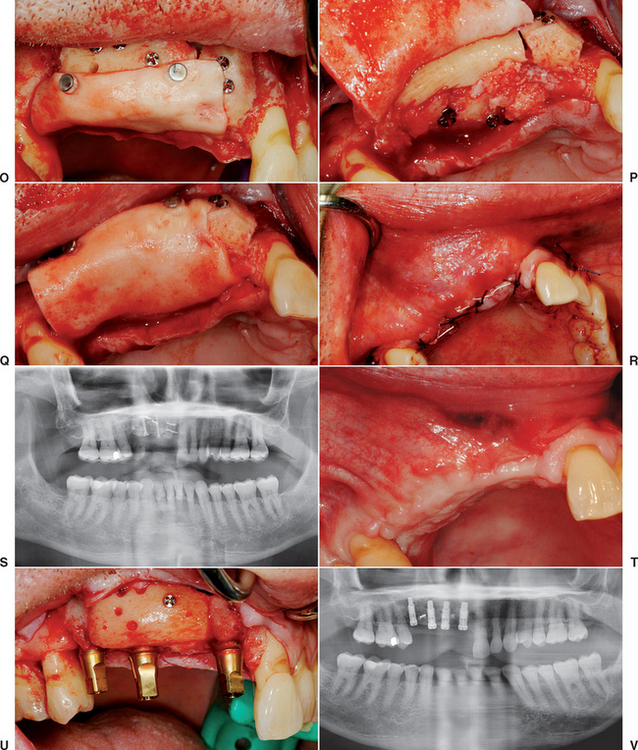
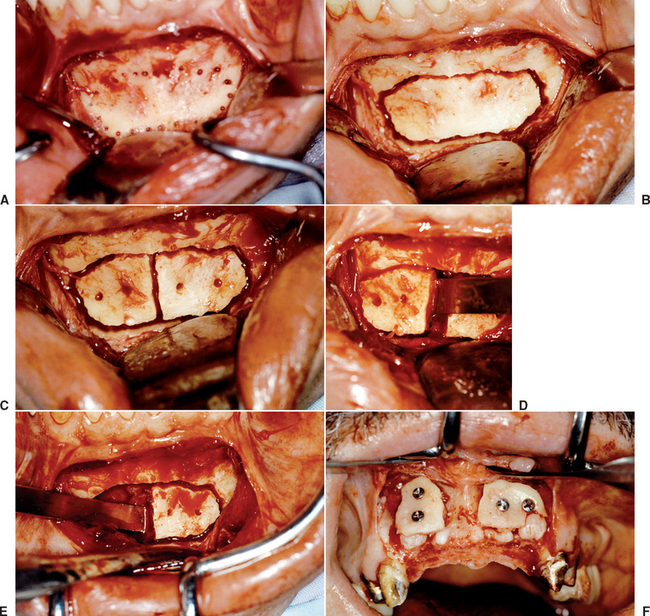
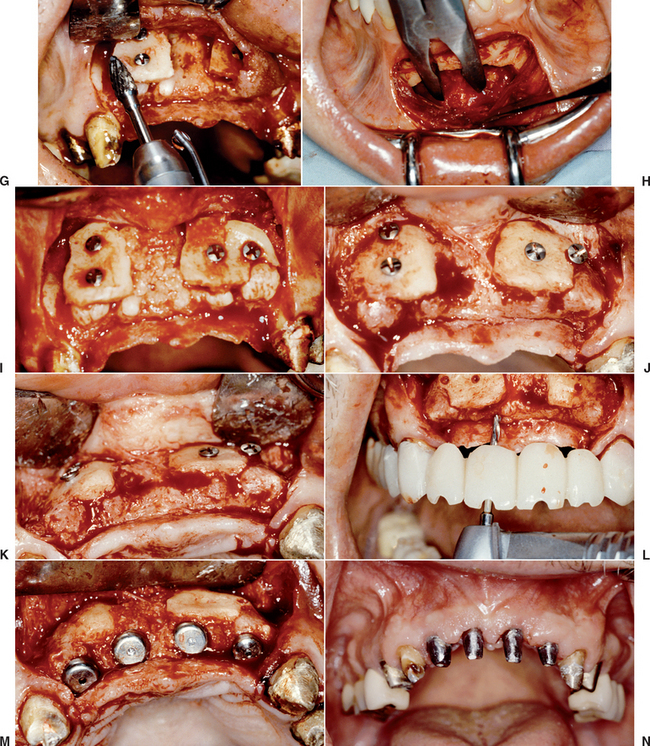
Figure 39-4 A, A panoramic radiograph of an edentulous maxilla and mandible (except for an impacted molar). B, A lateral cephalogram of the patient in Figure 39-3, A. The anterior maxilla and mandible is Division B bone volume. C, The soft tissue in the mandibular symphysis is reflected. D, A block of bone is outlined as a donor graft from the crest of the ridge. E, A second bone block is harvested from the crest. F, After osteoplasty, anterior implants are placed in the mandible. G, The maxillary anterior recipient ridge is exposed and decorticated. H, The two blocks are fixated to the anterior maxilla. I, An immediate postoperative radiograph of the mandibular implants and maxillary block grafts. J, After sinus grafts and impacted molar removal, 10 implants were inserted into the grafted maxilla. K, A fixed prosthesis was delivered to the maxillary arch.
PREOPERATIVE EVALUATION OF HOST SITE
A comprehensive evaluation of the host graft site is necessary for planning of the surgery. This includes the graft size, esthetic concerns, soft and hard tissue topography, and the periodontal and endodontic health of the adjacent teeth.38,93,94 The host site may be evaluated in width, height, and length. The most predictable bone augmentation sites require only the width dimension and extend for only one tooth. This provides mesiodistal lateral walls of bone, an apical wall, and a medial wall of host bone. A one-tooth span provides ease of soft tissue manipulation and minimal risk of incision line opening. Tooth-borne transitional restorations are easily fabricated. The donor bone harvest permits a complete fill of the region with an autograft. The least predictable bone graft sites are more than four teeth in length and require more than 5 mm of height and width of bone because the host site has primarily one wall of bone at the base and incision line complications, transitional prosthesis, inadequate autograft from the donor site combine to increase the overall risks.
The mesiodistal size of the host graft site with an intraoral harvest is most often four adjacent teeth or less in length and only deficient in width. However, in some larger mandibles with multiple harvest sites, a full-arch maxilla may be augmented in width (Figure 39-5). The mesiodistal size for a host site that requires height and width with an intraoral harvest is most often two adjacent teeth or less in length, although a span of four adjacent teeth may be restored with multiple harvest sites.
In esthetic areas, an emphasis must be placed on not only providing adequate osseous volume, but also developing a soft tissue profile for the final implant restoration.93 When the soft tissue region is in the esthetic zone, an increased height and thickness of keratinized mucosa before the bone graft is of benefit. A connective tissue graft is a common method to increase the desired tissue over the graft site before bone grafting. The soft tissue of the recipient site must then be completely healed for several months before bone graft surgery. Removal of foreign bodies, soft tissue surgery, or tooth extractions should be completed at least 12 weeks before bone grafting. This period allows vascularization and mature elastic fibers to be present in the soft tissue before the bone augmentation process and reduces the risk of incision line opening. Soft tissue surgical procedures may be planned in conjunction with implant placement or implant stage II uncovery when the soft tissue drape is out of the esthetic zone.
The width and height requirements for augmentation will influence the donor site selected from the mandible. As a general rule, when more than 4 mm of width is desired (C-w bone volume), the mandibular symphysis is the most common donor site. A mandibular ramus is selected as a donor site when the bone graft width is less than 4 mm (Division B to B-w bone volume). When an augmentation for height is required, the most common site is the mandibular symphysis and includes its cortical inferior border (Figure 39-6).
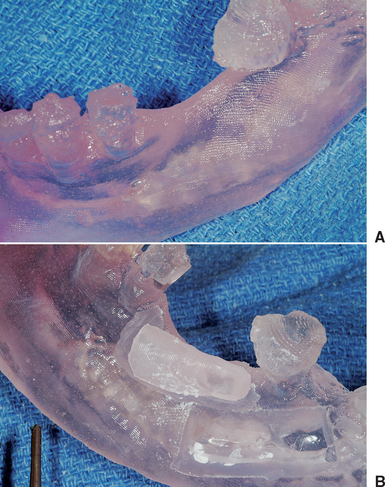
The initial radiographic examination of the host site may include periapical, panoramic, or lateral cephalometric views and computed tomography (CT) scans. A lateral cephalometric view is useful in determining the anteroposterior (A-P) (width) dimension of the anterior mandible at the midline when an augmentation for width is required from this donor site. CT with reformatted images are most useful in preoperative planning and ridge mapping for both the host site and the donor site (Figure 39-7).95–97 Mounted casts are also a benefit to allow the clinician to evaluate the ridge morphology in relationship to the adjacent teeth and opposing dentition. A diagnostic wax-up of the reconstructed ridge and restored dentition is advantageous in determining the graft width and position requirements and analyzing the occlusion. It is also used for fabrication of templates for CT, graft positioning, and implant surgery.38,41,95,96 A CT model may also be generated to study the three-dimensional (3D) aspect of the host site. A mock surgery may be performed of the donor site, and this CT model may also be used to help recontour the donor bone graft to fit the model prior to the intraoral fixation (Figure 39-8).
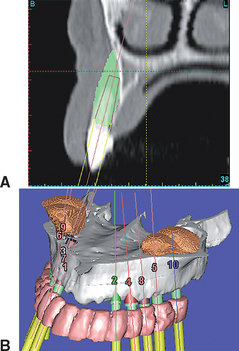
Figure 39-7 A computed tomography scan may be used to evaluate the host site volume required for proper rehabilitation.
Surgery
Preparation of Host Site
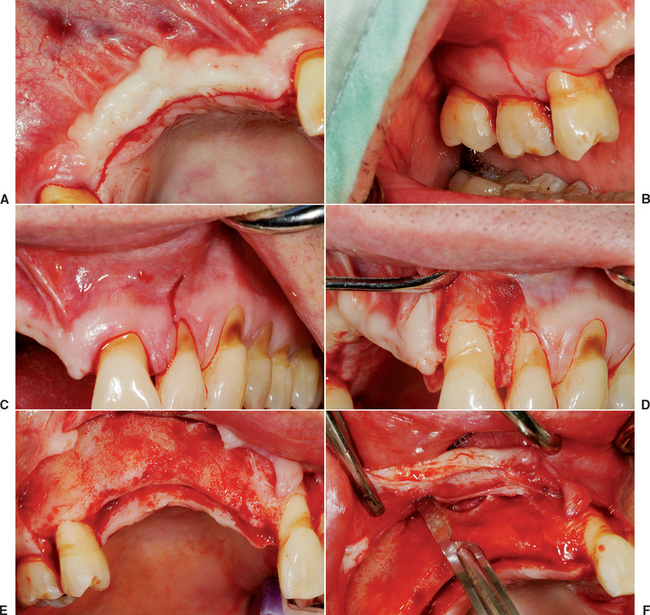
The concepts presented in the chapter on keys for bone grafting are incorporated into every step of the bone block grafting procedure. Incisions to surgically expose the recipient site are usually made within attached, keratinized tissue. The crestal incision in the edentulous host site is most often to the lingual aspect of the ridge, especially in the maxilla. This provides more keratinized tissue facially and reduces the risk of sutures tearing through the tissue if edema occurs after surgery, which results in incision line opening (Figure 39-9, A). When a block bone graft is anticipated, the vertical primary incisions usually are made one tooth distal to the tooth adjacent to the defect and include the distal interdental papilla. This provides a broader flap, which aids in primary closure and reduces incision line opening. The vertical release incision extends to the mucogingival junction (MGJ), not beyond. The soft tissue reflection of the flap distal to the graft site is a split-thickness reflection to aid the initial soft tissue healing and reduce incision line opening (see Figure 39-9, B to D).
The submucosal space technique was first described by Misch to cover large block bone grafts from the iliac crest. This procedure reflects a full-thickness flap over the graft site and at least 5 mm above the height of the MGJ. The periosteum and tissues 5 mm above the MGJ remain on the bone and are not reflected. The facial flap is then lifted and 3 to 5 mm above the depth of the MGJ and a scalpel incises through the periosteum 1 to 2 mm deep, parallel to the crestal incision and extends over and beyond the vertical release incision. After the incision is made through the periosteum, pointed tissue scissors (Metzenbaum) may be introduced into the periosteal incision for 10 to 15 mm or more, parallel to the surface mucosa with the blades of the scissors closed, so the facial flap thickness is 3 to 5 mm. The tissue scissors are then opened, and this blunt dissection of the tissue allows the muscles to be separated from the flap and creates a submucosal space. With the periosteum, tissues and muscles attached to the bone on one side and a 3- to 5-mm-thick facial flap on the other side, the facial flap may now advance the depth of the submucosal space, 10 mm or more. This dramatically increases the ability to advance the soft tissue flap over a block graft (see Figure 39-9, E to I).
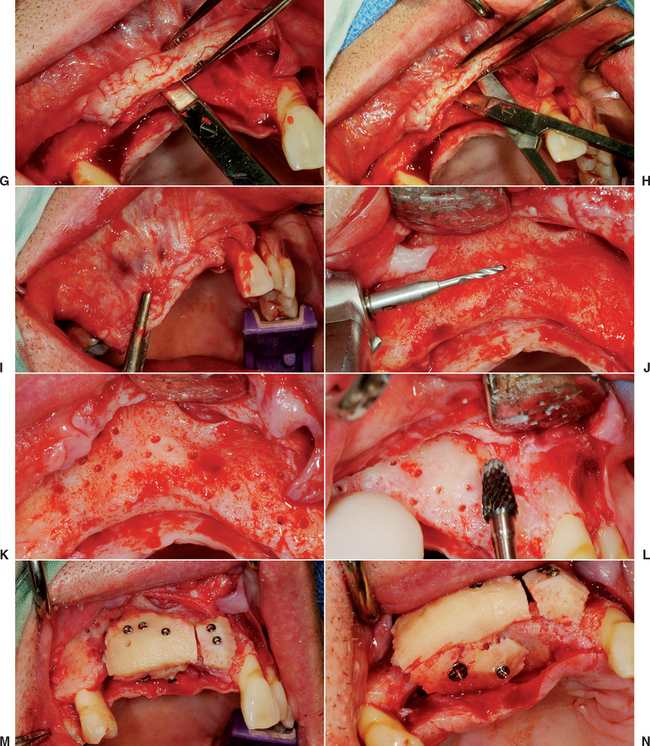
The next step in the preparation of the host site is perforation of the lateral and crestal aspects of the host bone with a small-diameter drill, equal to or smaller than the drill size that corresponds to the bone screws used to fixate the donor bone (1.4 mm diameter). The holes are 3 to 5 mm apart in the entire area of the desired augmentation (Figure 39-9, J, K). The perforations in the bone are created under copious amounts of saline at 2500 rpm and penetrate both the facial and lingual plates of bone in the region of the graft, especially when augmentation is desired on both sides of the residual ridge. This procedure increases the availability of osteogenic cells, accelerates revascularization, increases the regional acceleratory phenomenon (RAP), and improves graft union.97–99 The drill sites perforate the lingual plate. So that the fixation screw does not bottom out and strip the host bone and the dense, a cortical lingual plate ensures that the bone screws secure the bone block during the initial healing period. The host site is also recontoured with a large, pear-shaped carbide bur to improve the graft-to-recipient congruency. Ideally, the donor bone block should be slightly recessed in the host bone 1 to 2 mm, surrounded by a bony margin (Figure 39-9, L). After the block bone graft harvest and fixation, the tissues are approximated for primary closure (Figure 39-9, M to S). After a healing period of 4 to 6 months, the implants may be inserted (Figure 39-9, T to V).
MANDIBULAR SYMPHYSIS DONOR SITE
The ideal goal of a donor block harvest is to obtain sufficient bone, so the entire bone defect/augmentation dimensions are composed of the block autograft. The mandibular ramus donor site has several advantages over a symphysis donor, including: easier graft harvest, less postoperative discomfort, less neurosensory complications, less incision line opening, less anesthesia, more profound local anesthesia with fewer drugs, and less concern of changes in facial morphology. As a consequence, it is the harvest site of choice, when possible.
The mandibular symphysis exhibits a slight curved triangular shape in the midline, and this morphology is often well suited for reestablishing the arch form in maxillary anterior ridges.100–104 The average interforaminal distance is greater than 4 cm; therefore bone deficiencies requiring larger intraoral grafts may be managed with the symphysis as a donor site. In most cases, sufficient block grafts may be harvested from the symphysis for deficiencies in width involving a span up to four teeth or sites involving up to three teeth that require gains in both vertical height and width.*
The average dimension of an anterior mandible between the foramina is 44 mm, with black males having the greatest distance, followed by white males, black females, and white females having the least available donor bone between the foramen.108 A general rule is to stay at least 5 mm mesial to the mental foramen on each side for a donor bone harvest. Because the average mesiodistal dimension for an implant is 7 mm, a 35-mm bone length between a 45-mm mental foramen length would be necessary for five teeth. In a study by Montazem et al.,101 dentate cadaver mandibles were harvested from the mandibular symphysis. When two symmetric blocks were measured from each site, the average was 21 × 10 × 7 mm, the largest was 25 × 13 × 9 mm, and the smallest measured 21 × 6.5 × 6 mm.101
Surgical Harvest
Anesthesia
Surgical access to the symphysis is obtained via a crestal incision, vestibular incision, mid-keratinized tissue incision, or sulcular approach, depending on the anatomy. Most often mandibular anterior teeth are present above the donor site.109 The vestibular approach is used when there is 4 to 8 mm of keratinized tissue height around the lower anterior teeth, when subgingival crown margins are present in the area, when dehiscent roots are suspected, when root coverage is part of the history, or when sulcus depths around the mandibular anterior teeth are greater than 4 mm deep. In these situations, reflection of the soft tissue around the anterior teeth may result in tissue recession and root exposure soft tissue healing.
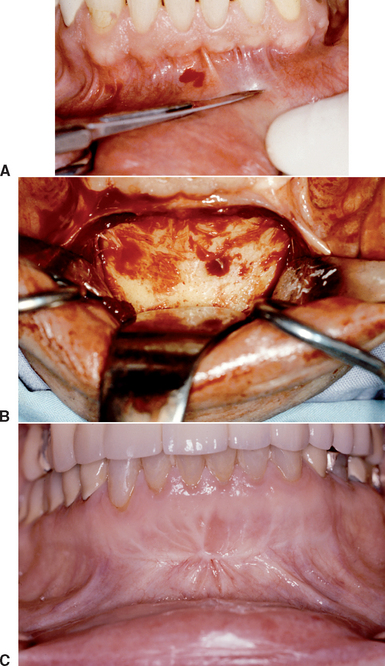
The vestibular incision is made in the mucosa at least 1 cm beyond the mucogingival junction and extends to each distal region of the canines. An inferior vertical release is made for approximately 10 mm between the canine and first premolar. Therefore this incision is anterior and above the mental foramen. A full-thickness mucoperiosteal flap is reflected toward the base of the mandible to the level of the pogonion, leaving themost inferior aspect of the periosteal attachment of the mentalis muscle intact (Figure 39-10).
The vestibular incision has the most intraoperative bleeding and the highest risk of incision line opening, but the least risk of soft tissue changes around the teeth and root exposure after healing. It also creates easier access to the chin. It is the easiest incision line to suture. Limiting the distal extent of the vestibular incision to the canine tooth area will reduce the incidence of mental nerve paresthesia.38,39,44
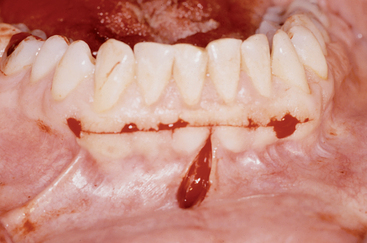
An incision is made within the mandibular anterior keratinized tissue when it is 9 mm or greater in height. This condition is rarely observed. However, when present, this is the incision line of choice, because it reduces intraoperative bleeding, eliminates the risk of root exposure after healing, and soft tissue healing conditions are ideal. The incision is made from the distal of each canine and a vertical release is made 10 mm in front of and above the mental foramen (Figure 39-11).
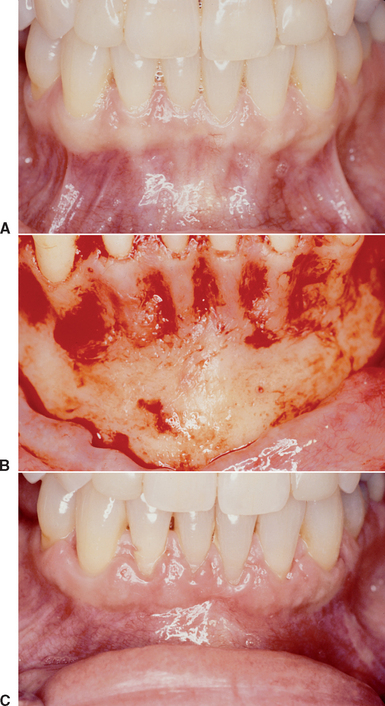
A sulcular incision is made when there is less than 4 mm of keratinized mucosa in height around the lower anterior teeth. These conditions are associated with a high mucogingival junction and high muscle attachments. Under these conditions, incision line opening is a greater risk. This is especially observed when the mentalis muscle is large and parafuctional forces of this region exist. The sulcular incision carries the least risk of incision line opening after healing, but has an increased risk of root exposure after soft tissue healing. It is also the most time consuming for suturing (Figure 39-12).
Symphysis Donor Harvest (for Division B-w to C-w)
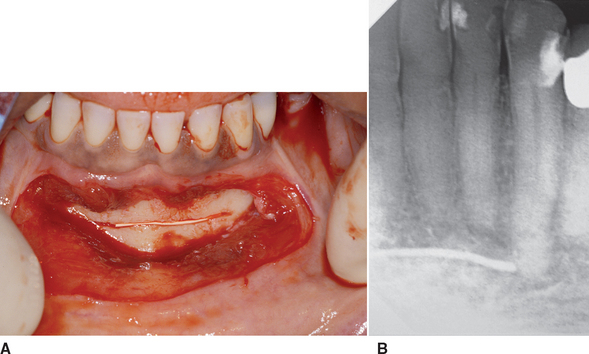
After the symphysis is exposed, the osteotomy for graft harvest is planned. The dimensions of the block are determined by the size of the bone defect. The osteotomies may be performed with a surgical fissure bur (557, 702) or oscillating saw. This is usually done under copious sterile irrigation with a 1:1 to 1:5 contraangle or straight hand piece. The most superior bone cut is made first, because the position of this border is less flexible. The superior osteotomy is ideally made at least 5 mm below the root apices. The angulation of this cut is perpendicular to the cortex to prevent injury to the roots. The depth of the osteotomies should be at least through the outer cortex and to the opposite cortical plate. Perforation of the lingual cortex may inadvertently occur, but it is not encouraged. The osteotomy may slope below the longer canine roots when more mesiodistal distance is necessary for the host site (Figures 39-13 and 39-14).
In most cases, the inferior cortex of the mandible is maintained unless a block graft for vertical augmentation is harvested. When adequate size permits, the inferior cut is 5 mm or more above the inferior border. The inferior margin has a cut perpendicular or angled upward, so the block harvest may be lifted out of the jaw with an osteotome. This also may protect the inferior portion of the mandible from fracture during the harvest, because more cortical bone along the inferior border is maintained (Figure 39-15, A). The vertical cuts are made in relation to the topography needs of the host site and may extend 5 mm in front of the foramen, when necessary. A larger mesiodistal dimension harvest rarely fits the host site in one piece. Instead, two blocks of bone are usually easier to mortice into place. In addition, two blocks of bone are easier to harvest than is one long block. Therefore most often the blocks are divided into 15- to 17-mm-long pieces and three vertical cuts are often made to trim the block harvest (see Figure 39-15, A to C).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses