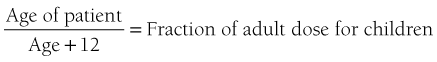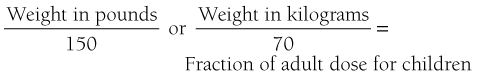chapter 35 The Pediatric Patient
McDonald RE, Avery DR, Dean J: Dentistry for the child and adolescent, ed 8, St Louis, 2004, Mosby.
FACTORS INFLUENCING PATIENT RESPONSE
The dentist sets the behavior standard in the office. Kimmelman1 has stated that firmness with kindness and a soft, clear voice is an asset in dealing with children. The dress of the dentist is important: White uniforms may provoke negative feelings in younger patients, whereas colorful uniforms (commonly worn today as pastel scrubs or scrubs with designs) evoke a more positive response. With universal precautions (gloves, glasses, and masks being standard of care), explanations and role-playing with the child to make him or her comfortable with our safety garb are suggested.
The time of day at which the appointment is scheduled may have bearing on a child’s behavior, especially the younger child. Interference with a child’s sleep or eating habits should, if possible, be avoided. The young child accustomed to a midday nap may be irritable if he or she is in the dental chair instead of bed at that time. Younger patients are most easily managed early in the day. This is also true for the apprehensive adult patient (see Chapter 4). The basic concepts presented in the stress-reduction protocols are of great importance in managing the pediatric patient. The length of the appointment should not exceed the child’s attention span. Younger patients are less able to tolerate longer appointments than are older, more mature children. Most children are able to tolerate 30- to 45-minute appointments with little difficulty.2
BEHAVIORAL EVALUATION OF THE PEDIATRIC PATIENT
Even though there are innumerable factors that interact to influence a child’s behavior in the dental office, the dentist must still be able to evaluate the patient’s ability to cope with the planned treatment. A number of systems have been developed to aid in classification of a child’s behavior and the potential for successful dental treatment. Two of the most commonly used systems are the Frankl Behavior Rating Scale3 and the system devised by Wright.4
In the Frankl system the observer (dentist) places the child’s behavior into one of four categories:
Johnson has stated that the Frankl scale appears to be closely related to the attitude of the parent toward dentistry.5
Wright’s classification presents three major groups: (1) cooperative, (2) lacking cooperative ability, and (3) potentially uncooperative behavior, with multiple subgroups. Wright has stated that most dentists, either consciously or subconsciously, categorize the behavior of children into one of these groups. These classifications permit the dentist to more readily determine the appropriate means of overcoming the management problems presented by the patient4:
DETERMINING THE NEED FOR SEDATION
The decision to use sedation should be made only following consideration of several factors:
Parental attitudes must be taken into account when considering the use of sedation. Unfortunately, the use of sedation in dentistry has periodically received negative publicity, a factor that has conditioned some parents against the use of these techniques in their children. The desires of the parent should always be considered when formulating the patient’s treatment plan; however, the dentist must always be the one to make the final decision. Several pediatric deaths have occurred in part because of the dentist’s desires to accommodate the parent’s wishes that all the dental treatment be completed at one visit. Though the administration of sedatives to a child patient at home, before leaving for the dental office, is discouraged, the parent’s ability to follow prescribing instructions must be determined if the dentist is considering doing this. When any doubt exists, the child should be scheduled early, with the drug administered by the dentist in the dental office.6
Alternative modes of treatment should be considered. Which technique of sedation is most likely to be effective in this patient? Many dentists develop the disturbing practice of using the same technique (and in some cases the same drugs and dosages) on all patients. Consideration in selection of the technique and drugs involves multiple factors, including the degree of cooperation of the patient and the patient’s medical history (i.e., allergies and illnesses). There is no one technique of sedation that will be effective in all patients. Indeed, in pediatric dentistry the failure rate for sedation is considerably greater than that seen in adults. Trapp has stated that a failure rate of 20% to 40% is not unusual unless the dentist is administering general anesthesia.7 Recent experience with pediatric sedation has demonstrated a 40% to 50% failure rate with oral sedation but a 5% failure rate with IM/IV sedation. As a general rule, the younger the patient the higher will be the failure rate of sedation techniques. The greater the number of techniques available to the dentist, the greater the likelihood of a successful outcome.
GOALS AND TECHNIQUES
Kopel has stated that sedation in the pediatric patient should be used to “train” or “retrain” the patient in an understanding of dental procedures and their importance.8 He continues by listing the following goals of pediatric premedication (sedation):
There is no simple answer to the question of proper drug dosage. Many factors act to complicate drug selection and drug action in children. In addition, the desired level of drug action varies considerably from patient to patient and from dentist to dentist. The most reliable factor in predicting adequate drug effect is a patient’s previous clinical experience with the drug in question. Once a drug has been administered to a patient, subsequent dosages can be modified according to this initial response. This is termed titration by appointment.5 Although previous clinical experience can provide guidelines leading to safer and more effective drug administration, it is still necessary to determine a safe and effective drug dose for a first appointment.
Drug package inserts (DPI) provide prescribing information concerning pediatric dosages. However, many drugs introduced for the management of pain and anxiety in recent years have not undergone adequate clinical trials in children to permit recommendations concerning pediatric dosage. Conversely, many of these drugs provide only adult dosage forms or indicate that “information [in children] is inadequate to establish dosage.” Wilson,9 in a review of the 1963 Physicians’ Desk Reference, found that 62% of listed drugs were not indicated for pediatric use, whereas an additional 16% were without recommendation for pediatric dosage. This number has steadily increased in recent years.
MONITORING
Monitoring of the sedated patient is discussed in Chapter 5. As important as monitoring is for all sedated patients, in the pediatric patient monitoring is possibly of even greater significance. Because of the relative lack of communication available between the dentist and the very young, precooperative or the handicapped patient, one of the most important means of communication—verbal—is often not present. In addition, because of the inability to titrate drugs administered orally, intramuscularly, or intranasally, the possibility of a relative overdose developing is somewhat enhanced. Constant monitoring of the patient is essential.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses