Chapter 33 Communication
Section A Patient Communication
Relevance to Esthetic Dentistry
Communication is probably more relevant to esthetic dentistry than other areas in that patients are now more aware of what can be done esthetically for their smile. They come to the dental office and say, “I want this smile,” often showing photographs from magazines. The dental professional then must translate that into a determination of how to satisfy the patient’s want in a way that will mesh with the patient’s actual needs. One of the most attractive things about a person is his or her smile; the ultimate fashion accessory is an attractive smile (Figure 33-1). Communication is essential so that the dentist understands what the patient wants and the patient understands what he or she needs and what the dentist can do.
Key Terms to use in Verbal and Written Communications
Several words can be used in verbal and written communications that will encourage patients to seek esthetic dental procedures (Box 33-1). For example, when talking with a patient about whitening, it is easy to use many of these words to help the patient better understand about the procedure, as follows:
Verbal Communications
Telephone Communications
How one answers the telephone creates the initial impression for the patient or prospective patient. The person answering the telephone should maintain a very upbeat voice that indicates that the person is smiling and happy to have received this call (Figure 33-2). An appropriate beginning is to say:
This conveys to the patient a warm, sincere welcome and indicates this is the right office.
“Thanks for calling. May I have your name?”
“Thank you, Mr Smith, for calling our office. How may I be of service to you?”
The key thing is to personalize one’s communication by using the caller’s name.
Follow-up to the First Call
The follow-up call is made only if time permits before the patient’s appointment.
What to Expect in the Dental Visit
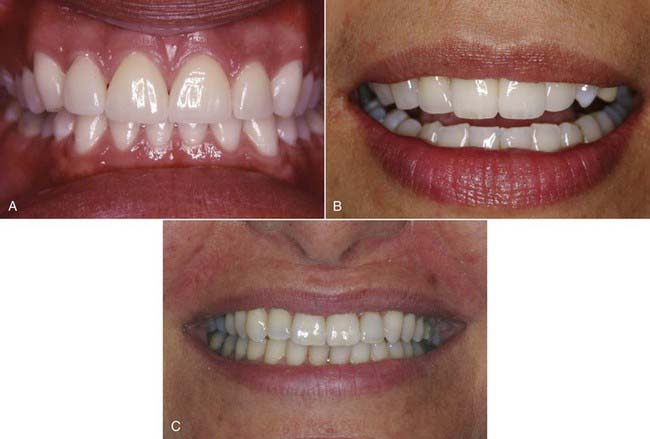
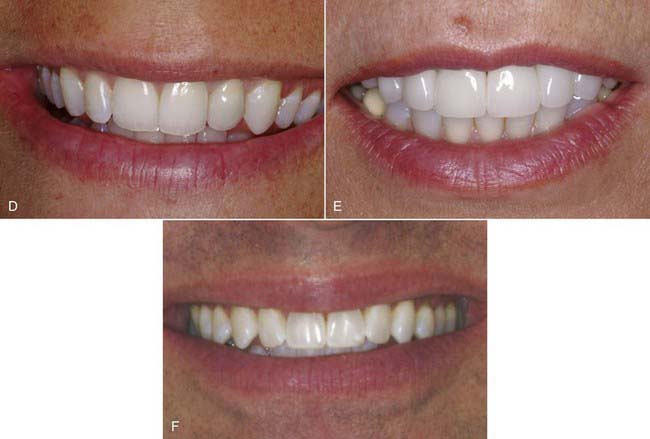
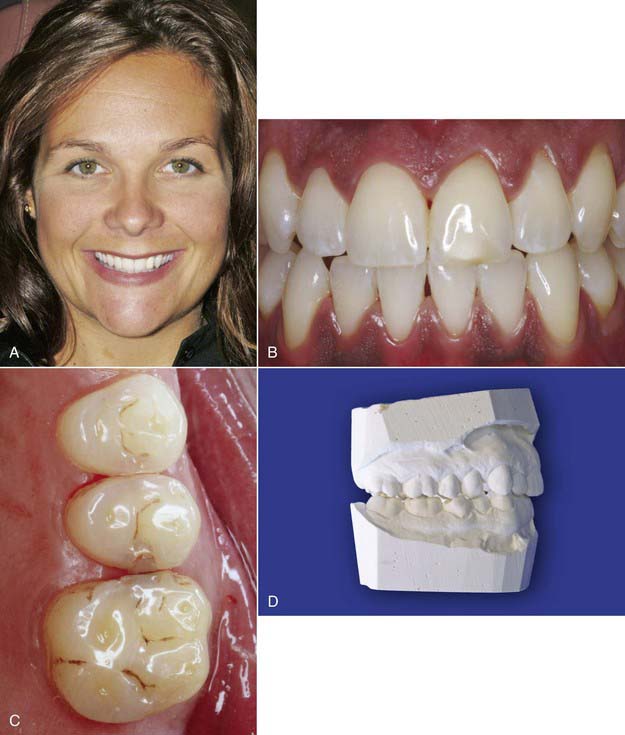
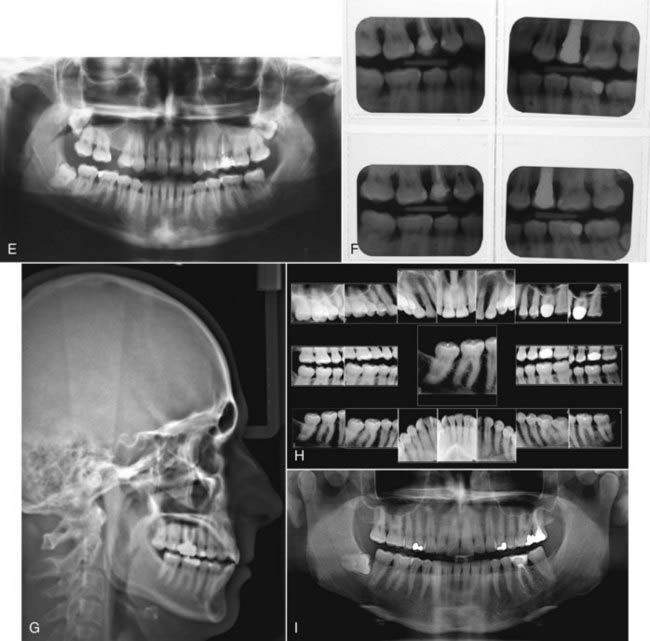
Typically the patient is told what to expect either on the phone, depending on the length of the conversation, or at the initial visit. First, it is important to meet with the patient, whether this is done by the dentist or the staff. With a new patient, the current procedure is to take full face and intra-oral photographs (Figure 33-3, A to C). Also, study impressions and models of the teeth may be made (Figure 33-3, D), and there may be a need for radiographs (Figure 33-3, E to I). Depending on how the staff and office are set up, a complete diagnostic work-up may be performed. Some of these tasks are handled by the dentist; some fall to the dental hygienist or auxiliary staff. The patient is fully informed of everything that will be done before the initial visit.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses