Chapter 15 Direct Veneers
Section A Direct Composite Bonding
Emanuel Layliev, Jeff Golub-Evans
Brief History of the Development and Evolution of the Direct Composite Bonding Procedure
Relating Anterior Function and Esthetics
The typical reason a patient requires the placement of direct composites in the anterior include normal wear and tear, occlusal disturbances, aggressive tooth brushing, or eating too much crunchy food. To create the proper look cosmetically, it must first be determined what has made such treatment necessary. It is important to evaluate the patient’s habits and normal function. This will reveal occlusal problems, perhaps abrasion, nutritional problems, erosion, or bruxism. The wear is evaluated to identify its cause, and then treatment possibilities and precautions are planned (Box 15-1). The goal is to avoid such wear in the future or at least minimize the threat of repetition. This involves evaluating what has happened to the individual’s teeth, and to the opposing dentition (e.g., the lower arch) to ensure that a better profile, shape, and position can be created for those teeth. Various modalities such as Invisalign (Align Technology, Inc., San Jose, California), bonding, or enameloplasty may be employed.
Innovative Elements
Treatment Considerations
Case 1
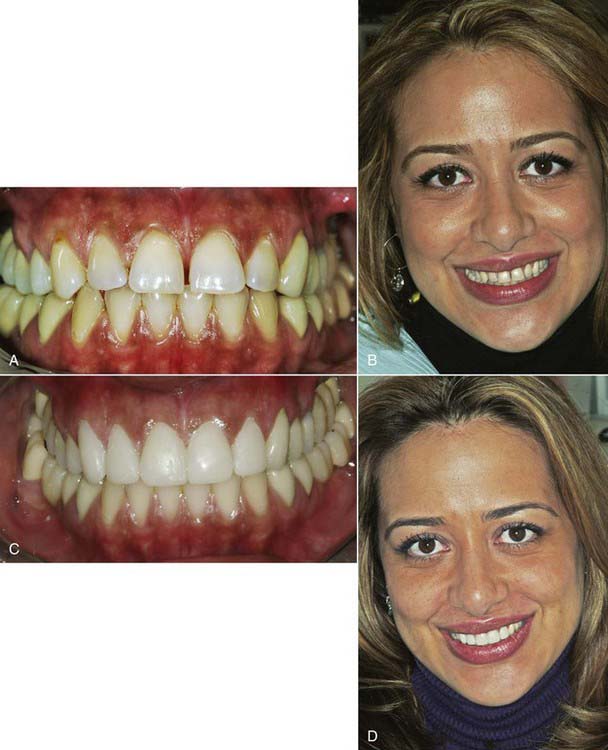
A female patient had short and narrow upper anterior teeth with space present interproximally. She was unhappy with her appearance (Figure 15-1, A and B). A treatment plan was established to include bonding the maxillary anteriors, canine to canine, while the rest of her upper dentition involved crown and bridgework. The end result portrays teeth that met her esthetic and functional expectations, and made her look attractive, and complemented her appealing facial features (Figure 15-1, C and D). The procedure took about 4 hours to complete and was done in a single sitting. She returned for a follow-up about 2 weeks later to make sure her gingiva were healthy, the bonding intact, and the esthetics up to her expectations.
Section B Transitional Bonding
Relevance of Transitional Bonding to Esthetic Dentistry
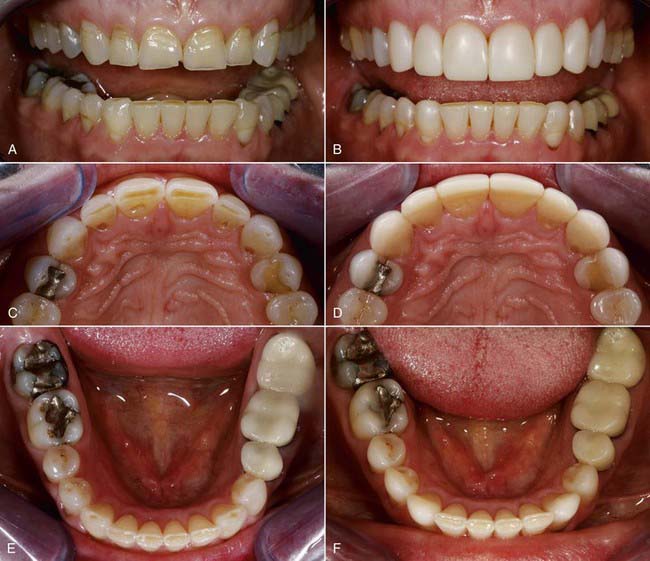
Transitional bonding allows practitioners to make major or minor changes in occlusion and esthetics with little or no reduction of tooth structure (Figure 15-2). With this approach it is possible to address cases with various esthetic problems, and, perhaps more important, health issues can often be treated. Examples include wear from bruxing; loss of occlusal tooth structure from erosion, decay, or fractures; and numerous teeth missing. Such situations may cause a decrease in vertical dimension leading to esthetic and functional problems. Restoring teeth that have worn down or are developmentally small so that the teeth are long enough or large enough to look more attractive without opening the bite could create a very deep overbite or other negative change. By increasing the vertical dimension one can often compensate for that.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses