Angioedema
INTRODUCTION
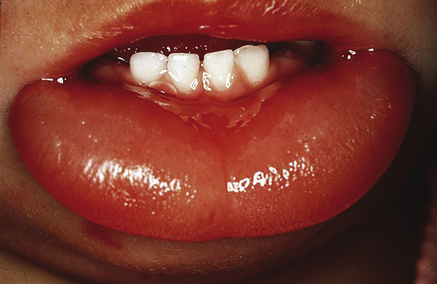
This is a potentially lethal condition. Angioedema manifests with rapid development of oedematous swelling of the lip(s), tongue and oral or facial swelling (Fig. 32.1). This can be life-threatening as oedema may also involve the neck and hazard the airway. The swelling in angioedema is usually relatively transient and the skin does not scale.
ALLERGIC ANGIOEDEMA
INCIDENCE
Allergic angioedema is common – far more common than HANE.
AETIOLOGY AND PATHOGENESIS
Allergic angioedema is a type 1 hypersensitivity reaction that may be induced by:
CLINICAL FEATURES
 The acute oedema, which appears < 2 h of antigen exposure, can cause pronounced itchy labial and periorbital swelling, and can involve any oral site, but when oedema involves the tongue and neck and extends to the larynx, it can cause rapidly fatal respiratory obstruction.
The acute oedema, which appears < 2 h of antigen exposure, can cause pronounced itchy labial and periorbital swelling, and can involve any oral site, but when oedema involves the tongue and neck and extends to the larynx, it can cause rapidly fatal respiratory obstruction.
 Acute allergic oedema usually develops along with urticaria (‘hives’) and may be associated with anaphylactic reactions.
Acute allergic oedema usually develops along with urticaria (‘hives’) and may be associated with anaphylactic reactions.
DIAGNOSIS
Angioedema is diagnosed clinically and from a history of atopic disease and/or exposure to allergen, and sometimes by allergy testing (prick test), but only where there are appropriate resuscitation facilities and an emergency kit containing injectable adrenaline at hand. Mast cell tryptase levels may be raised. Hereditary angioedema (HANE) may need to be excluded – HANE has low C4, but normal C3 levels, and absence of C1-INH activity (Table 32.1).
Table 32.1
Aids that might be helpful in diagnosis/prognosis/management in some patients suspected of having angioedema*
| In most cases | In some cases |
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses












