3
Orthodontic Diagnosis and Treatment Planning: Collaborating with Medical and Other Dental Specialists
Summary
Orthodontists – as specialists – are expected to be proficient in diagnosing anomalies of the face, teeth, and jaws, as well as identifying any coexisting deviations in physiological functions and systemic pathologies. As a member of the healthcare provider system, an orthodontist should have sufficient knowledge to recognize and record the etiology of a presenting malocclusion, which may be the result of a variety of systemic or local aberrations. This means any anomalies of anatomy, physiology, and the various medical conditions that may directly or indirectly influence the orthodontic diagnosis, treatment plan, mechanotherapy, or the prognosis of the case should be taken note of. In addition, the existing oral health conditions and problems with the dentition, ranging from quality and quantity of dentition, morbidity associated with childhood trauma, dental caries, and/or periodontal diseases, which might require close collaboration with a variety of dental specialists, should be recorded. This chapter aims to deal with these issues and provide a framework for interaction and collaboration with medical and dental specialists, based on a holisitic approach to orthodontic diagnosis and treatment planning. The goal is to help the reader develop an aptitude to communicate with a variety of healthcare specialists to undertake, reconsider, stop, or reschedule orthodontic treatment with due precaution.
Introduction
Success in any healthcare profession depends largely on accurate diagnosis, formulation of appropriate treatment goals, and their precise implementation. Currently, patients with orthodontic needs span across a wide range of age groups, personalities, social strata, and ethnic backgrounds, with varying levels of expectations (Abu Alhaija et al., 2010). Additionally, the increasing number of adult patients means that the present-day orthodontist is faced with an array of systemic (van Venrooy and Proffit, 1985; Patel et al., 2009) as well as local conditions (Basdra et al., 2001; Altug-Atac and Erdem, 2007) that may affect both the general as well as oral health status of the individual. It is now accepted that ‘It is no longer appropriate to deny elective dental or medical care to patients with diagnoses that have historically been associated with poor outcomes’ (Sonis, 2004). The recent medical and dental advances have made it possible for many patients with significant medical and dental disorders to be successfully managed in the orthodontic office (Lux et al., 2005), provided the orthodontist has a sound knowledge base and is keen to interact with other medical and dental professionals (Patel et al., 2009).
An orthodontic graduate first needs to be a good oral diagnostician and a good physician, before becoming a good orthodontist. We, as orthodontists, often make a diagnosis after taking a short medical history, complemented by a physical examination concentrating only on facial appearance (in general) and occlusion (local) alone. This approach, which is more appropriately termed ‘regional diagnosis’, reveals the existing malocclusion but lacks an overall perspective, and, in this process, the bigger picture of the medical, psychological, and pathological processes occurring elsewhere in the body gets ignored. This approach makes proper recognition of existing systemic conditions, and their effects on orthodontic treatment, difficult, if not impossible to comprehend. In our ‘play safe’ approach, many of us end up refusing treatment to patients who could be treated successfully with suitable precautions and professional interaction with the other medical/dental specialists. To rectify this approach, it is recommended to include a module on diagnosis and management of medical conditions in orthodontic training programs, with sufficient exposure in clinical settings in multispecialty hospitals. This will allow development of an attitude that encourages a more professional approach when interacting with our medical and surgical colleagues, while recognizing and realizing our responsibilities and limitations. Up-to-date knowledge of medical problems should be aimed for, so that proper communication protocols can be followed while referring patients to other medical and dental colleagues.
The Other Side of the Story
Since oral health can have a significant impact on the general health, dental health is often a great concern for the medical fraternity (George et al., 2010; Yasny, 2010). Mutual referral systems are useful in these situations, with medical personnel – including specialists – referring patients with dental and oral health-related problems to the dental specialists with greater zeal, provided the specialists on both sides are confident about and comfortable while interacting with each other. We should recognize that none of us can possibly treat all the diseases of the human body. Thus, a ‘two-way interaction’ is important for providing a better level of healthcare.
Orthodontic Diagnosis from a Broad Perspective
From a mere tooth-moving specialty, orthodontics has emerged to become a branch of dentistry with deep scientific and evidence-based perspectives of its biomechanical principles. Often, clinicians remain preoccupied with the mechanotherapeutic features of various appliances and philosophies, ignoring the fact that teeth are a part of larger, intricately linked biological systems of the body which influence the response of teeth to mechanical stimuli.
Every patient is unique, with metabolic traits that are individually specific to him or her (Sidell and Kaminskis, 1975; Morrison et al., 1992; Bartley et al., 1997) even though all humans have similar basic anatomical, physiological, and biochemical features. It must be appreciated that treatment is being delivered not to an artificial set of typodont teeth, but rather to vital tissues – which have the capacity to respond differently to the same treatment protocol under the same physiological conditions in different individuals (Ren et al., 2003; McConkey, 2004; Williams, 2008), altered physiological conditions in the same individual (Brambilla et al., 1981), and in various pathological conditions (Salerno et al., 1982; Verna et al., 2000).
The craniofacial complex can be considered as an organization of many small organ systems and components, such as the dentoalveolar structures, the nervous system, the muscular system, the soft tissue matrix, and the air passages. These structures are so intricately interlinked that disturbances in the physiology, anatomy, or function of any one component structure are bound to cause an imbalance in the whole of the craniofacial complex. This understanding should be clearly reflected in orthodontic diagnosis and treatment planning.
Concurrently, a thorough knowledge of subjects such as anthropology, genetics, growth and development, nutrition, psychology, endocrinology, and kinesiology can help us gather critically important data regarding the various aspects of general health and disease. Along with this knowledge, the use of advanced biochemical, microbiologic, and radiologic investigative procedures can help to optimally diagnose a malocclusion, thus reducing the chances of treatment failure. In brief, a comprehensive approach toward diagnosis and treatment planning helps in categorizing patients according to their general health status and biological limitations, and increases the probability of a successful treatment outcome.
The First Interaction with the Patient
The initial examination is the most overlooked step as far as orthodontic diagnosis is concerned. Planning for an orthodontic examination should begin even before the patient visits the orthodontic office, through careful screening via telephonic conversation with trained office personnel, or alternatively, through electronic mailing of the patient’s knowledge of their medical history to the orthodontic office prior to the scheduled appointment. This preliminary review will often highlight important medical conditions such as endocrine, hematological, cardiac, renal, hepatic, pulmonary, and allergic disorders, as well as dental health-related conditions. Such information is important for the orthodontist to prepare for the appointment, and plan various investigative procedures and anticipated referrals in advance, which can translate into increased efficiency and reduced time required for the screening and risk assessment of the patient. This strategy should ultimately lead to increased patient satisfaction and higher confidence levels, and lesser chances of complications later during therapy.
Comprehensive diagnosis and treatment planning should start at the time of the first interaction with the prospective patient (Kharbanda, 2009). The very short ‘look-see’ examination is no longer considered adequate with the increasing number of patients with medical problems seeking orthodontic treatment. At the first visit, the orthodontist should enquire about the problems and the expectations of the patient and parents from orthodontic treatment (Figure 3.1), and concurrently perform an appraisal of the patient’s psychological profile, as treating patients with unrealistic expectations or with extreme mood fluctuations may result in an unhappy ending (Al-Omiri and Alhaija, 2006). Following this initial scrutiny, a systematic procedure of examination should be followed, starting with the craniofacial region. If the examination or the previous medical history indicates the presence of an underlying pathology or abnormality, further investigations in the form of referrals and advanced diagnostic tests should be undertaken (Figure 3.2).
Figure 3.1 (a–d) A 12-year-old girl with severely compromised vision attended with her parents for protrusion of her upper teeth and poor dental esthetics. She had a Class II malocclusion with bimaxillary protrusion and severe discoloration of the dentition due to fluorosis. Radiographic examination also revealed an inverted and unerupted mesiodens. The diagnosis and treatment plan in such a case must include evaluation of expectations of patient and parents in view of the reduced vision of the girl, who may not fully appreciate the benefits of the improved esthetics following orthodontic treatment and correction of the discolored anterior teeth. It is also pertinent to elicit the intensity of concern in the patient and parents towards the discoloration and protrusion as well as the motivational factors with regard to treatment.
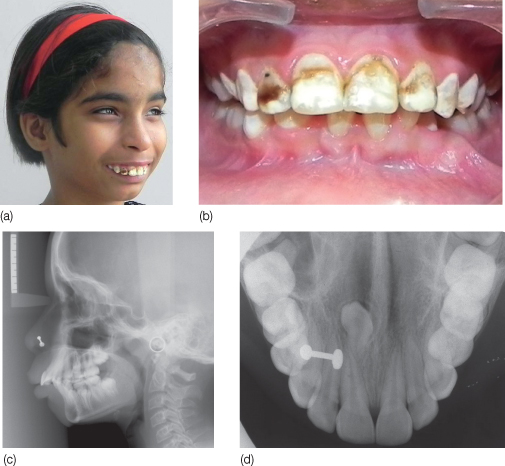
Figure 3.2 A 12-year-old girl with congenital strawberry angioma on the left side of her face reported for orthodontic consultation. A strawberry angioma of the face may be associated with disorders such as encephalotrigeminal angiomatosis (which is associated with epilepsy of the contralateral cerebral hemisphere). Hence, presence of such a lesion warrants further investigations to rule out such disorders. Angiomas of the face may extend into the oral cavity as well or they may occur as an isolated lesion within the oral cavity. These lesions are known to bleed excessively following episodes of trauma associated with extraction, injection of local anesthesia and even trauma from orthodontic appliances.

The Importance of the Medical History in the Orthodontic Diagnosis and Treatment Planning
Many patients today would already be taking short-or long-term medications, which may influence paradental tissue remodeling (Krishnan and Davidovitch, 2006) and consequently, tooth movement. Drugs such as steroids, when taken for long periods, as in chronic asthma or for immunosuppression, may predispose teeth to iatrogenic root resorption following application of a mechanical stimulus (McNab et al., 1999). In certain instances, for example, in the presence of sexually transmitted diseases such as human immunodeficiency virus (HIV) infection or syphilis, the patient may hesitate to give a complete and realistic history. Thus, it becomes the prerogative of the treating doctor to sufficiently evaluate the patient, both prospectively and retrospectively, to obtain a detailed health history during the first visit and/or the subsequent visits. In this regard, the orthodontist and office personnel should be able to judge from the mannerisms, attitude, and the current health condition of the patient whether further investigations and/or precautions are warranted before and/or during treatment.
A detailed medical history is an extremely useful tool for evaluating the existing health status of an individual, and identifying any medical disorders that he/she may have. Diseases of chronic duration, those of severe intensity, those affecting bone metabolism, and those altering the inflammatory pathways have a particularly important bearing on the orthodontic treatment plan (Sonis, 2004; Patel et al., 2009). Besides nutritional imbalances, developmental disorders, and skeletal malformations, chronic diseases, liver dysfunctions, renal impairments, cardiac and pulmonary anomalies, and erosive joint diseases can all impact physiological growth, and thus, orthodontic treatment (Table 3.1).
Table 3.1 Common causes of short stature
Table adapted from: Lifshitz (2007); Crocetti, Barone (2004); Fujieda, Tanaka (2007); Matfin (2009).
| 1. Intrauterine growth retardation (low birth weight): a) Sporadic b) Syndromic 2. Chronic diseases and disturbances of organ systems: 3. Nutritional disturbances: 4. Endocrinologic disorders: 5. Chromosomal aberrations: 6. Skeletal disorders: 7. Inborn errors of metabolism: 8. Psychosocial dwarfism (functional) 9. Chronic drug intake: 10. Normal variation of growth: |
Chromosomal Aberrations and Embryologic Defects Including Deformities of the Orofacial Complex – Where Do Orthodontists Stand in Their Diagnostic Approach?
Development of craniofacial structures is largely determined by the cells of the neural crest, which give rise to the branchial arches during embryonic development. In the 4th week of intrauterine life, the mandibular arch (also the hyoid and glossopharyngeal arches) forms discrete processes, which form the future maxilla and mandible. While the paired mandibular processes merge with each other in the midline by the 4th week, the maxillary process continues to contribute to the formation of the secondary palate, the upper jaw and lateral portions of the upper lip (Sperber et al., 2001). The period between the 6th and 12th week of intrauterine life is considered to be critical for craniofacial development (Finkelstein, 2001), and anomalies during this period result in a variety of craniofacial defects (these are covered in greater detail in Chapters 7–9). Most of the congenital disorders result from unknown causes. However, in the light of newer research, many of the unknown causes have been identified, and now multifactorial etiology is considered the commonest cause of congenital defects, whereas isolated genetic defects have been described in 10–30% of cases (Kumar, 2008). Genetic inheritance can follow a variety of patterns, from simple mendelian inheritance to complex polygenic traits with variable penetrance and expression across generations. In order to accurately diagnose the etiology of the condition and the inheritance pattern, the orthodontist has to identify the role of genetics and delineate it from the environmental influences. Familial comparisons, pedigree analysis, and sometimes, simple cephalometric analysis, may be valuable tools in identifying and differentiating the role of genetic aberrations in the causation of these conditions.
Orthodontists often encounter conditions resulting from embryonic developmental defects, such as cleft of lip and palate, hemifacial microsomia, maxillofacial dysplasias, vertical facial clefts, and micro/macrognathia. Being an active member of the craniofacial team, it is the responsibility of the orthodontist to be able to recognize the basic features of a congenital growth anomaly or a genetically linked syndrome. A thorough extraoral and intraoral examination can reveal vital information of an underlying syndrome/congenital deformity, (Table 3.2 and Figure 3.3). Facial features such as sparse hair on the head, frontal bossing, depression of the nasal bridge, telecanthus, low-set ears, typical epicanthal folds, coloboma, defects of the external ear, and facial clefts are characteristic features seen in many craniofacial syndromes. It is important to note that many craniofacial deviations may be associated with systemic alterations, such as osteogenesis imperfecta with dentinogenesis imperfecta, or craniofacial clefts, in association with velocardiofacial and Aperts syndrome.
Table 3.2 Syndromes affecting face and jaws associated with Class II/Class III malocclusion
| Condition | Features | Etiology |
| Class II | ||
| Hemifacial microsomia (Goldenhar syndrome) | Unilateral dysplasia of the ear, hypoplasia of mandibular ramus, cardiac and renal abnormalities | Most cases sporadic; few familial instances; pedigrees compatible with autosomal dominant and recessive transmissions |
| Pierre Robin complex | Micrognathia; cleft palate and glossoptosis. This condition may occur as an isolated malformation complex or part of a broader pattern of abnormalities | Heterogeneous |
| Treacher Collins syndrome | Dysplastic low-set ears; downslanting palpebral fissures; micrognathia | Genetic/autosomal dominant |
| Class III | ||
| Apert syndrome | Craniosynostosis proptosis hypertelorism; downslanting palpebral fissures; symmetric syndactyly of hands and feet | Genetic/autosomal dominant |
| Crouzon syndrome | Craniosynostosis; maxillary hypoplasia accompanied by relative mandibular prognathism; shallow orbits; proptosis | Genetic/autosomal dominant |
| Achondroplasia | Short-limbed dwarfism; enlarged head; depressed nasal bridge; lordosis; high palate | Genetic/autosomal dominant |
| Syndromes associated with mandibular prognathism | ||
| Basal cell nevus (Gorlin syndrome) | Macrocephaly; frontal and parietal bossing; prognathism; multiple jaw cysts; multiple basal cell carcinomas; bifid ribs | Genetic/autosomal dominant |
| Klinefelter syndrome | Mandibular prognathism; skeletal disproportion; gynecomastia; small testicles | Commonly 47, XXY karyotype XXXY and XXXXY also occur |
| Osteogenesis imperfecta | Fragile bones; blue sclera; deafness; mandibular prognathism | Autosomal dominant (common type) |
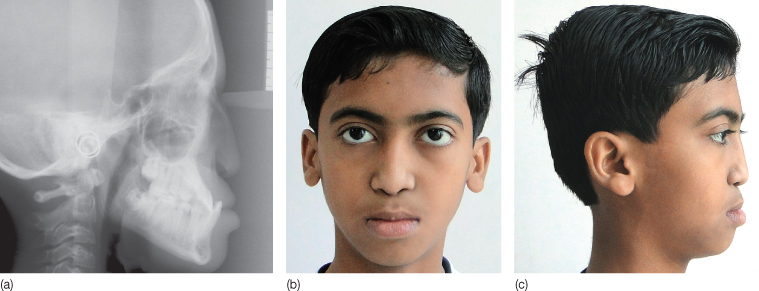
Figure 3.3 a-c Binder syndrome. This 11-year-old boy, who attended the orthodontic clinic for fixed appliance treatment, had a flat midface due to a retrognathic maxilla, broad flat nose, horizontal nostrils, short columella, and an apparent lack of nasal bridge. The radiograph confirmed a short anterior cranial base, small cranial base angle, reduced sagittal depth of nasopharynx, hypoplasia of the anterior nasal spine, downward inclination of the nasal bones and extremely reduced sagittal maxillary length. The patient was diagnosed as having Binder syndrome after consulting with the oral medicine department, the differential diagnosis of which includes acrodysostosis and Stickler syndrome. Additional investigations may be required for differential diagnosis of the case from other similar conditions.
In sum, an orthodontist should be able to identify severe conditions, and make appropriate referrals to medical specialists and/or the craniofacial and genetic centers, while managing the lesser severe ones themselves, without inflicting further trauma on the psychological status of the already burdened patient.
Acute and Chronic Infections (systemic and local)
Various systemic diseases, and those locally affecting the craniofacial complex, have the propensity to contribute to the etiology of malocclusion, directly or indirectly, in both the prenatal and postnatal stages. Chronic systemic infections such as tuberculosis, hepatitis, nephritis, and HIV may indirectly contribute to a malocclusion by causing disruption in systemic growth during childhood. Acute perinatal infections such as the TORCH complex (Toxoplasmosis, Other infections, Rubella, Cytomegalovirus, Herpes simplex) can lead to congenital deformities in the offspring, including craniofacial clefts. Diseases such as congenital syphilis, apart from systemic alterations, can lead to an array of orofacial malformations such as saddle nose, depressed nasal bridge, and hypoplasia of the molars and incisors.
Late natal or acute childhood infections can cause temporary cessation of tooth development, which may be evident as enamel hypoplasia. In other instances, infections from distant foci, acute or chronic, may disseminate via blood, and lodge into one of the jaw bones, leading to osteomyelitis (Fabe, 1950; Carek et al., 2001), and consequent destruction of the bone architecture and/or growth disturbance. Involvement of the temporomandibular joint (TMJ), due to similar reasons, or from local spread of infections from adjacent structures, as in mastoiditis (Hadlock et al., 2001) or otitis media (Semlali et al., 2004; Prasad et al., 2007), can lead to arthrosis, adhesions, and regressive changes within the joint, which may affect growth and function of the mandible, resulting in malocclusion. The role of tonsillitis and rhinitis in the etiology of mouth breathing and development of adenoid facies, cannot be overemphasized.
Many infectious bacterial, fungal, parasitic, and viral diseases require utmost consideration to prevent nosocomial transmission of the disease. Minor problems, such as aphthous ulcerations, aerobic and anaerobic infections of the oral cavity, may be effectively managed by the well-trained orthodontist. However, since many systemic infectious diseases, such as infectious mononucleosis, mumps, measles, tuberculosis, HIV, and leukemia may also have similar oral manifestations, it becomes extremely important to differentiate local lesions from lesions that are signs of major systemic conditions to allow timely intervention and management by trained personnel. In such situations, the orthodontist should collaborate with the physician to avoid the risks associated with spread of disease and complications that may arise during orthodontic treatment.
Deficiency States and Malnutrition
Craniofacial and dental development is profoundly influenced by the availability of essential nutrients. Malnourished children tend to become disabled, incapable of resisting a disease or withstanding its onset and progress. Animal studies have demonstrated that in rats fed on a low-calcium and vitamin D-deficient diet, increase in body weight is impaired and the craniofacial dimensions are reduced (Engström et al., 1982a,b). There is no general agreement whether growth retardation during early infancy in humansis reversible in later years. Research findings on children surviving protein calorie malnutrition (PCM) have shown that severe malnutrition early in life affects their post-malnutrition growth, with reduced height and head size (Krueger 1969; Alvear et al., 1986). Other epidemiological studies have shown that catch-up growth subsequent to malnutrition compensates for previous growth retardation, and results in normal stature of previously malnourished children (Garrow and Pike, 1967; Graham and Adrianzen, 1972). Dreizen et al. (1967) stated that chronic undernutrition in the presence of nutritional or metabolic disease slows down the rate of skeletal maturation, delays the onset of menarche, and retards the epiphyseal fusion period.
These research findings may have diagnostic implications, wherein children with Class II malocclusion with nutritional deficiency, in general, could present with smaller physical and craniofacial dimensions. Those with unusual smaller dimensions may need to be discussed with a pediatrician and a nutritionist for their nutritional requirements, which might have a bearing on the quality of the response to functional appliance treatment as well as on the tissue response during orthodontic tooth movement. Similarly, vitamin deficiency, such as vitamin C (Litton, 1974) or D (Collins and Sinclair, 1988) deficiency, may affect the remodeling response of the periodontal ligament and the alveolar bone to orthodontic forces. For a detailed description on how nutritional factors influence orthodontic diagnosis and treatment planning, and how an orthodontist should obtain nutrition data from patients, see Chapter 5.
Endocrinological and Metabolic Anomalies in the Etiology of Malocclusion
The endocrine system is an intricate network that is regulated at various levels by human physiological processes. This system is responsible for regulation of the metabolic processes throughout the body, controlling the growth and differentiation of various parts of the skeleton. Hence, disruption of any part of this system may lead to widespread alterations of the human physiology, resulting in metabolic, anatomical, and/or growth-related disturbances. Although a disturbance in virtually any part of the endocrine system would be expected to have orthodontic implications, disorders of the pituitary, thyroid, parathyroid, and pancreas are of particular interest to the orthodontist. In many instances, an alert dental professional may be the first person to suspect a systemic anomaly (Cohen and Wilcox, 1993; Vitral et al., 2006; Gosau et al., 2009), leading to the diagnosis of an underlying endocrinological disorder.
The Pituitary Gland
The physical and mental development of a child is controlled to a great extent, apart from other genetic and nutritional factors, by the pituitary and the thyroid glands (Setian, 2007). Pituitary hormones control the functioning of various other endocrine glands, as well as the linear growth of the skeleton. Consequently, disturbances of the pituitary function (and that of hypothalamus) are associated with alteration of function of most other endocrine glands. Deficiency of growth hormone, one of the many hormones produced by the pituitary, is associated with reduced stature and reduced growth and development of the craniofacial complex (manifesting as a retrognathic maxilla and mandible) and shortened cranial base length (Cantu et al., 1997; Van Erum et al., 1998). Interestingly, it has been reported that dental age may not be retarded in growth hormone deficiency states (Van Erum et al., 1998). The use of hormone replacement therapy, in conjunction with orthodontic treatment for growth modulation highlights the importance of interactive care (Davies and Rayner, 1995; Hwang and Cha, 2004). On the other hand, growth hormone excess, which usually occurs secondary to a somatotrophic pituitary adenoma (Matfin 2009), causes gigantism in childhood and acromegaly in adults. Any child or an adult who presents with unexplained gain in height and/or mandibular prominence should be suspected for gigantism (Yagi et al., 2004), and should be referred to an endocrinologist for further investigations and management. It is important to know that although gigantism/acromegaly typically occurs in isolation, it may be associated with other pathological endocrine conditions such as multiple endocrine neoplasia (MEN) (Yagi et al., 2004; Accurso and Allem, 2010), McCune–Albright syndrome (MAS), neurofibromatosis and the Carney complex (Eugster and Pescovitz, 1999). See Chapter 11 for a detailed description of these conditions.
The Thyroid Gland
Euthyroid state is essential for normal mental and skeletal development and maturation, and adult bone maintenance (Harvey et al., 2002; Murphy and Williams, 2004). A hypothyroid state during pregnancy and early childhood results in various developmental disturbances and defects, including neurological deficits. Hypothyroidism (Figure 3.4) during pregnancy and in early childhood causes mental retardation, growth arrest, delayed bone maturation, and epiphyseal dysgenesis (Rivkees et al., 1988; Bassett et al., 2007). In older children and adolescents, however, mental deficits may not be marked, but the delay in skeletal maturation is evident. Orofacial alterations include enlargement of the tongue (Wittmann, 1977), delayed tooth eruption, tendency for mouth breathing, Class II malocclusion due to a retruded mandible, short posterior facial height, and anterior open bite (Shirazi et al., 1999), all of which contribute to the development of malocclusion.
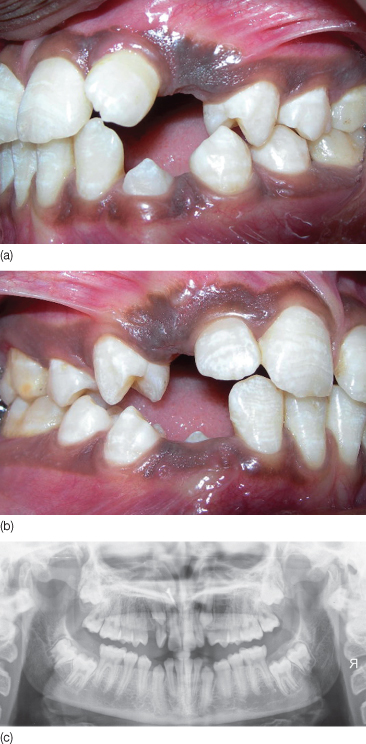
Figure 3.4 Intraoral views and radiographs of an 18-year-old girl diagnosed with hypothyroidism show delayed eruption of multiple teeth.
In contrast, juvenile thyrotoxicosis leads to accelerated growth and advanced bone age, but it also induces short stature due to premature fusion of the growth plates as well as craniosynostosis (Bassett et al., 2007). In adults, thyrotoxicosis accelerates bone loss, causing osteoporosis (Murphy and Williams, 2004), and even minor disturbances of thyroid status increase the risk of fractures (Bassett et al., 2007).
At the present time, owing to early recognition of thyroid deficiency states, the classic manifestations of thyroid disease may not be evident in all individuals with thyroid disorders. Also, subclinical thyroid disease is being diagnosed more frequently in clinical practice in young and middle-aged people, as well as in the elderly, with a reported prevalence of 4–10% in the adult population (Canaris et al., 2000; Hollowell et al., 2002). Subclinical hyper- and hypothyroidism may have repercussions on the cardiovascular system and bone, as well as on other organs and systems (Biondi and Cooper, 2008). Hence, the clinician has to be vigilant and informed to be able to suspect or diagnose an underlying thyroid disease. For example, a lack of response to functional appliance treatment in a case of skeletal Class II malocclusion after a reasonable period of time and excellent patient cooperation may be because of an underlying growth hormone or thyroid disorder. The literature supports the view that thyroid hormone replacement therapy results in rapid catch-up growth (Rivkees et al., 1988; Teng et al., 2004). It has been suggested that orthodontic treatment should be combined with hormone replacement therapy for optimum results (Verna et al., 2000).
Pancreas
Diabetes mellitus, a disorder of carbohydrate, protein, and fat metabolism due to absolute or relative deficiency of insulin, is one of the commonest metabolic disorders. The disorder, especially when poorly controlled, leads to widespread changes such as nephropathy, neuropathy, retinopathy, and vascular disease, as well as cardiovascular and cerebrovascular complications, among other possibilities (Vernillo, 2001). Uncontrolled diabetes predisposes to severe and rapidly progressive periodontal disease, osteoporosis, and increased propensity to infections, all of which can be factors in the etiology of malocclusion. It can also lead to alteration in the timing of tooth eruption, causing accelerated development until about 10–11 years of age, and delayed development after that (Adler et al., 1973; Orbak et al., 2008). In addition, diabetes is also associated with an exaggerated inflammatory response during normal tooth eruption (Orbak et al., 2008), xerostomia, burning mouth syndrome, candidiasis, delayed and abnormal wound healing, diminished salivary flow, and salivary gland enlargement. A child or adult with symptoms of dry mouth/burning sensation, ketone smell from the mouth, unusual intensity of periodontal breakdown, inflamed gingivae with pockets should raise the suspicion of underlying diabetes mellitus (Lamster et al., 2008).
Neuromuscular Disorders in the Etiology of Orthodontic Problems
The influence of neuromuscular harmony on dental development, occlusion, and functions such as mastication, deglutition, speech, and respiration is well established. Animal studies have confirmed alteration in the craniofacial skeletal structures secondary to loss of muscle tone (Babuccu et al., 2009; Tsai et al., 2010). Consequently, any degenerative or inflammatory disorder affecting the neuromuscular system can have significant influence on growth and remodeling of the dentofacial structures. Disorders such as chronic seizures, hemiparesis, and cerebral and cranial nerve palsies can cause alterations in the muscle tone, leading to imbalance of forces and consequent adaptation of the skeletal structures (Fong et al., 2003), including the craniofacial skeleton, with subsequent development of a malocclusion (Cascino et al., 1993; Trujillo et al., 2002; Portelli et al., 2009).
Seizure disorders, which are one of the most common neurological disorders with an incidence of 1–3% (depending on age) (Annegers, 1997), can result in orofacial trauma (Sheller, 2004) and asphyxiation because of appliance aspiration during an episode of seizures. Patients with chronic seizures may manifest body asymmetry (Fong et al., 2003), including forehead and facial structures (Tinuper et al., 1992), altered mental status and poor oral hygiene, while patients on long-term drug therapy may show gingival hyperplasia (Sheller, 2004) and bone mineral loss (Sheth, 2004). Moreover, hypercementosis, root shortening, anomalous tooth development, delayed eruption, and cervical lymphadenopathy have also been documented in patients with seizure disorders (Johnstone et al., 1999). Since orthodontic appliances often consist of a variety of metal fixtures, they have the ability to alter or distort the signals produced by magnetic resonance (MR) and computed tomography (CT) machines (Sadowsky et al., 1988; Sheller, 2004). Hence, in patients with suspected organic lesions causing seizures who may require MR imaging or CT scanning, the presence of an orthodontic appliance may act as an impediment in the imaging process, which needs to be considered while planning the treatment.
An Overview of Systemic Disturbances in Relation to Orthodontic Treatment Planning
Although the discussion of each disease or organ system is beyond the scope of this chapter, this section will briefly highlight the diseases affecting major organ systems and their implications for orthodontic diagnosis and treatment planning.
Psychiatric Disorders
A majority of patients attending an orthodontic clinic are children and young adults at various stages of maturation, with rapid and drastic changes taking place, both in their minds and bodies. These patients are prone to the development of psychological/psychiatric disorders. It is reported that up to 14–20% of American children and adolescents may develop psychiatric disorders (Cassidy and Jellinek, 1998). In addition, adults going through difficult phases of life may also develop psychiatric problems. It is, therefore, imperative that the orthodontist be well conversant with psychology as well as any abnormal behavior which might point towards a psychiatric disorder or substance misuse.
The psychiatric disorders most commonly encountered by the orthodontist are either major depressive disorder (MDD) or attention deficit hyperactivity disorder (ADHD) (Neeley et al., 2006a). Any history, sign, or symptom that points toward a psychiatric disorder or a sudden or unusual change in a patient’s behavior during treatment requires discussion with the parents and the family physician, who may consider consultation with a clinical psychologist/psychiatrist. In addition, patients with ADHD may be under treatment with amphetamines such as methylphenidate, which predisposes them to xerostomia, dysphagia, sialoadenitis, stomatitis, bruxism, and growth disturbances (Elia et al., 1999). These possibilities have important orthodontic implications as non-compliance with maintenance of oral hygiene, instructions in placement of elastics at home, difficult behavior during orthodontic procedures, and missed appointments can lead to treatment failure. Therefore, pretreatment evaluation of the patient must include questions about prior or current illness and medication. Any treatment plan should include a discussion with the treating psychiatrist, as discussed in Chapter 4.
Substance misuse is also a significant problem among adolescents with a reported prevalence of up to 40% among tenth graders in the USA (Neeley et al., 2006b). Intravenous drug users may have diseases that are transmitted through blood, such as HIV infection (Leukefeld et al., 1990) and Hepatitis B (Gillchrist, 1999). A suspected case may need to be referred to a medical specialist after consultation with a psychologist.
Diseases of the Respiratory System
Diseases of the respiratory system can be broadly divided into those affecting the upper and the lower airways. Diseases of the upper airway can be an outcome of anatomical, physiological, or pathological restrictions of airway space in the nose, pharynx, and the larynx. Chronic restriction of the nasal airway due to sinusitis, tonsillitis, adenoiditis, and allergic rhinitis leads to mouth breathing, and further to the classic adenoid facies as well as a change in the craniofacial flexure. Disorders of the lower airway, such as asthma, chronic bronchitis and other chronic pulmonary diseases increase the breathing effort and affected cases may display orofacial changes similar to those seen with mouth breathing, apart from consequences related to impaired general health due to low oxygenation of the blood. Moreover, children with severe asthma may be using oral or inhaled steroids, which may cause a reduction in the salivary flow (Laurikainen and Kuusisto, 1998), predispose to oral candidiasis, and increase risk of root resorption (Davidovitch and Krishnan, 2009). A proper consultation with a pulmonologist is deemed essential while treating these patients, so that any complications that may develop in due course during orthodontic treatment can be effectively managed.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


