3
Oral medicine and pathology
- Viral infections
- Oral ulceration
- White patches and premalignant lesion of the oral mucosa
- Oral cancer
- Soft tissue swellings of the oral mucosa
- Cysts of the jaws
- Conditions of the salivary glands
- Oral manifestations of systemic disease
- Common causes of facial pain
- Disorders of the temporomandibular joint
- Developmental tooth anomalies
- Tooth wear
Introduction
As dental care professionals (DCPs), hygienists and therapists will encounter the oral mucosa and the underlying supporting tissues as well as the teeth on a daily basis. They are therefore in a unique position to detect disease which may be either local or systemic in origin. In some cases detection may be life saving, in others recognition of the disease may affect the treatment plan, in yet others the patient may seek reassurance or an explanation of its implications. It is therefore important to have a thorough understanding of the causes and the clinical presentation of the common and important oral diseases and their effects upon both the treatment and the patient.
Viral infections
Unlike bacteria which are composed of single cells and capable of independent growth, viruses are composed of small nuclear fragments surrounded by a protein coat. They are unable to divide or replicate on their own and in order to survive must gain access to and live inside cells. Once inside they use the host cell’s own synthetic processes to reproduce and, in the process, often destroy the host cell. In other cases the host will destroy the virally infected cell in order to eliminate the virus. It is this cellular destruction that is responsible for many of the clinical features of viral infections affecting the oral cavity.
The time taken for the virus to infect the host, replicate and for cellular damage and hence clinical symptoms to occur may be anything from 3 to 21 days and is known as the incubation period. Most severe viral infections last between 10 and 14 days, after which time the host has mounted an effective immune response and the infection resolves. Other less virulent infections may last only a few days. In general viral infections affect younger age groups, and viral infections occurring in older age groups raises the possibility of underlying immunosuppression.
The common viral infections affecting the oral cavity are:
- Herpes simplex: primary and secondary.
- Herpes zoster: primary and secondary.
- Hand, foot and mouth.
- Herpangina.
Of these, infections caused by herpes simplex are the most common and important.
Primary herpes (primary gingivoherpetic stomatitis)
This is caused by herpes simplex virus type 1, which is transmitted in saliva, and it is usually children and young adults who are affected. The following features help in the diagnosis:
- The patient will complain of feeling unwell.
- They usually have a fever and enlarged lymph nodes in the neck (cervical lymphadenopathy).
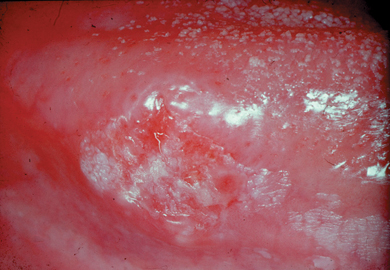
- Painful blisters known as vesicles develop on the gingiva, palate, buccal mucosa and tongue and these are fragile and burst to form superficial ulcers covered in grey–white slough (Figure 3.1). The surrounding tissues are red (erythematous) and the lips may appear swollen and blood encrusted.
- In some cases the patients will be unable to eat or drink.
Figure 3.1 Young adult with primary herpes. Numerous small ulcers covered by a white slough and with erythematous margins are present on the labial mucosa.
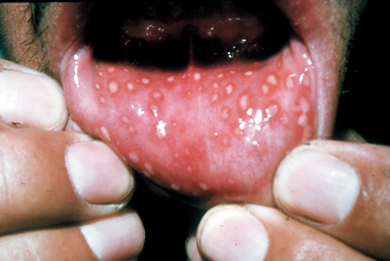
Patients are highly infectious and isolation and bed rest are advised. Most treatment is symptomatic and the disease is self-limiting, resolving in about 10–14 days. The diagnosis is made on clinical features. If antiviral agents are given early enough, they may shorten the course of the disease (see also Chapter 12, p. 261).
Although primary herpes may be very severe, in many instances the disease is subclinical and the patient will have no signs and symptoms.
Secondary herpes (cold sores)
In approximately a third of patients, the herpes virus remains dormant in the ganglion of the trigeminal nerve. It is reactivated by a number of agents including sunlight, stress and menstruation, and travels down the trigeminal nerve to form characteristic vesicles, which burst and crust over, on the lips. The lips may become swollen and the lesions are known as cold sores. They often recur in the same position and are preceded by a tingling or prodromal phase. Treatment with antiviral agents at this stage may significantly shorten the course of the disease which otherwise lasts 10–14 days. The patient is infectious during this time and dental treatment should be avoided.
Varicella zoster viral infection (chicken pox)
This is also caused by a herpes virus and is a common disease of children. It rarely affects the oral cavity but occasionally small ulcers may be seen in addition to the itchy, vesicular, crusting rash which occurs on the skin. The incubation period lasts up to 21 days and the disease 10–14 days. Like herpes simplex, the varicella zoster virus may also lie dormant in the trigeminal ganglion and upon reactivation forms a characteristic rash along the distribution of the nerve. This may occur on the face or rarely in the oral cavity. Such lesions are painful and may cause scarring.
Hand, foot and mouth and herpangina
These two infections are both caused by the coxsackie A virus and are relatively mild diseases usually affecting children. In both infections the lesions are characterised by vesicles, which break down to form shallow ulcers.
- In hand, foot and mouth disease almost any part of the oral mucosa may be affected together with the hands and the plantar surfaces of the feet.
- In herpangina the lesions may affect the soft palate, tonsils and pharynx and the patient usually complains of a sore throat.
- In both conditions lesions resolve within a few days.
Oral ulceration
The oral mucosa is composed of stratified squamous epithelium, which covers and protects the underlying connective tissues from the oral cavity. An ulcer is formed when there is a break or defect in the epithelial covering and the underlying connective tissue is exposed to saliva and microorganisms of the oral cavity. This results in an acute inflammatory response and the surrounding connective tissue becomes reddened and inflamed. The surface of the ulcer is covered by a white–grey slough.
There are many causes of oral ulceration but the two most common types are those caused by trauma and idiopathic aphthous ulceration. An important although rarer cause is malignancy and this is discussed in more detail in the section on oral cancer.
Traumatic ulceration
There are many causes of trauma in the oral cavity and these include mechanical, chemical and thermal.
Mechanical trauma may be caused by:
- Sharp cusps.
- Orthodontic appliances.
- Ill-fitting dentures.
- Teeth (biting lips or cheeks).
Diagnosis of this type of ulceration is usually not difficult and the position, shape and size of the ulceration should correspond to the suspected cause. Once this is removed the ulceration usually starts to heal within 10 days. If healing does not occur then other causes of ulceration should be suspected.
Chemical ulceration is relatively uncommon but may be caused by drugs and other oral preparations taken by the patient. Aspirin tablets placed in the oral cavity adjacent to a painful tooth may cause this type of ulceration.
Thermal injury is relatively common and is caused by the ingestion of very hot food or drinks. The oral cavity heals quickly and without scarring and thermal injury rarely causes a diagnostic problem.
Aphthous ulceration (recurrent aphthous stomatitis)
Aphthous ulcers are relatively common and affect younger rather than older individuals. Their characteristic feature is recurrence and typically they start in childhood and tend to decrease in frequency with age. The cause of aphthous ulceration is not known but there is a family history in about 45% of patients, indicating there may be a hereditary disposition. Other predisposing factors which have been implicated include stress, trauma and menstruation. In some cases aphthous ulceration is associated with iron-deficiency anaemia and treatment of the deficiency may result in resolution.
Three different clinical types have been identified: minor aphthae, major aphthae and herpetiform ulcers.
Minor aphthae
This is the most common type of ulceration and has the following characteristic features:
- Ulcers are typically small, about 2–5 mm across, oval and covered by a grey slough. The surrounding mucosa may be erythematous (Figure 3.2).
- In some patients the ulcers may be multiple.
- They affect the non-keratinised mucosa, i.e. the lateral border of tongue, floor of mouth, buccal mucosa and lips, and last about 10–14 days.
- The ulcers may be very painful and anecdotal evidence suggests that the pain increases towards the end of the 14-day period.
- The time interval for recurrence is variable.
Treatment is symptomatic if all possible underlying causes have been excluded.
Figure 3.2 Minor aphthous ulcer on the labial mucosa.
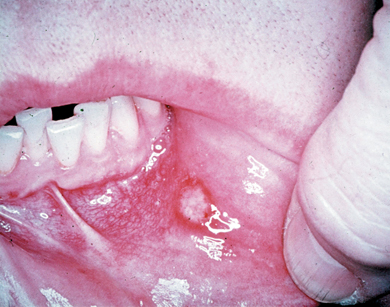
Major aphthae
These ulcers are not as common as minor aphthae and differ in the following ways:
- They are larger and usually greater than 5–10 mm in diameter.
- They are often multiple and affect keratinised as well as non-keratinised mucosa; the lips, cheeks and soft palate are common areas.
- They last between 4 and 6 weeks and may be very painful.
- They may also heal with scarring.
Other causes of ulceration
A malignant ulcer caused by a squamous cell carcinoma is an important cause of oral ulceration. However, it has very characteristic features that help in the diagnosis and these are discussed below in detail. Ulceration following breakdown of vesicles is a feature of viral lesions affecting the oral cavity and also certain autoimmune blistering disorders, such as pemphigus vulgaris, but these latter conditions are rare.
The differential diagnosis and distinguishing features of oral ulceration are shown in Table 3.1.
Table 3.1 Differential diagnosis of ulceration of oral mucosa.
| Type of ulcer | Clinical features |
| Traumatic: mechanical | Position of ulceration corresponds to suspected cause (dentures, teeth, orthodontic appliance) and disappears when cause removed |
| Idiopathic: minor aphthous ulceration | Recurrent, young individuals, painful, small lesions, lips, floor of mouth. Lasts 10–14 days |
| Neoplastic: squamous cell carcinoma | Long duration, non-healing ulcer, no obvious cause, raised rolled margins, firm/hard to touch. High-risk sites include floor of mouth, lateral tongue, retromolar area |
| Infective: herpes simplex | Preceded by vesicles, characteristic distribution on gingivae and palate, patients systemically unwell, lasts 10–14 days |
| Autoimmune conditions: pemphigus vulgaris, pemphigoid | Blisters which break down to give ulcers and erosions. Affects older individuals. Skin lesions with pemphigus vulgaris |
White patches and premalignant lesions of the oral mucosa
In health the oral mucosa is pale pink, but pathological changes may result in white patches. In many instances this is brought about by changes in the keratinisation of the epithelium; for example, the cheeks are normally non-keratinised but if epithelium becomes keratinised they will appear white clinically. There are many causes of white patches on the oral mucosa and the most important are discussed below. The differential diagnosis and distinguishing features are shown in Table 3.2.
Table 3.2 Differential diagnosis of white patches affecting the oral mucosa.
| Type of white patch | Clinical features |
| Frictional keratosis | Position of lesion corresponds to cause (dentures, teeth, orthodontic appliance) and disappears when cause is removed. Common on cheeks, lateral border of tongue |
| Lichen planus | Bilateral reticular lesions affecting the cheeks, lateral tongue, gingivae. Skin lesions. Other clinical types. No obvious cause |
| Lichenoid reactions to drugs | Similar clinical appearance to lichen planus but associated with drugs |
| Lichenoid reactions to amalgam restorations | Unilateral on tongue or cheeks adjacent to large amalgam restoration. Resembles lichen planus |
| Leukoplakia – homogeneous | Smooth or undulating white patch, any site. Not associated with trauma or any other obvious cause |
| Leukoplakia – non-homogeneous | Irregular white patch. May have a raised, nodular or irregular surface and or show variations in colour with red areas. Highest risk of malignant change |
Frictional keratosis
White patches may occur in response to chronic trauma and are known as frictional keratosis. Such lesions are common on the buccal mucosa in a linear pattern adjacent to the teeth and this is known as an occlusal line. They may also be seen on the tongue or other intraoral sites and are often caused by:
- Chronic biting.
- A sharp cusp.
- An over-extended denture.
- An orthodontic appliance.
In order to make a diagnosis of frictional keratosis the source of the trauma must be identified and the position of the white patch should correspond to the trauma. If this is not the case then other causes of a white patch should be considered and these are discussed in more detail below.
Lichen planus
Lichen planus is a relatively common disorder, which may affect the skin as well as the oral mucosa. Middle-aged women are affected more than men and in most cases the disease is symptomless. However, some patients may complain of roughness or discomfort on eating spicy foods. Typically it is characterised by:
- Reticular, white, interlacing lines or striations which occur bilaterally on the buccal mucosa and tongue and occasionally the lips (Figure 3.3).
- Sometimes the free and attached gingivae may be affected and appear fiery red.
- Other patterns of disease may be seen: the white patches may be plaque-like rather than reticular or sometimes the mucosa appears erythematous and may show areas of erosion or ulceration. In these cases diagnosis may be more difficult.
- Skin lesions may be present on the wrists and shins and appear as violet papules.
Figure 3.3 Lichen planus affecting the buccal mucosa. Note the lace-like white striations on the cheeks.
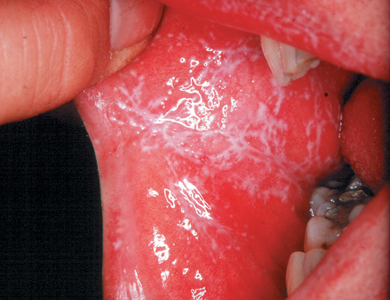
The histological changes in lichen planus show that the epithelium is keratinised, leading to the white striations seen clinically. In addition there is a band of lymphocytes beneath the epithelium which is associated with destruction of the lower epithelial layers. This and other observations have led to the belief that lichen planus is the result of a cell-mediated immune reaction. What precipitates this reaction is unknown.
Lichenoid reactions
Lesions that resemble lichen planus clinically may be caused by drugs and also dental materials. Lichenoid drug reactions are often caused by:
- Antihypertensive drugs taken for high blood pressure.
- Oral hypoglycaemic drugs taken for diabetes.
Lichenoid drug reactions start after commencement of drug therapy and resolve when the drug is withdrawn. Such lesions are usually bilateral and very difficult to distinguish from lichen planus unless a careful medical and drug history is taken.
Reactions to amalgam restorations are also common but in these cases lesions affect one side of the mouth only and are present on the mucosa in the contact area of amalgam. Quite often it is the buccal mucosa and lateral borders of the tongue that are affected. Removal of the restoration usually results in resolution of the lesion.
Leukoplakia
White patches that have no obvious cause and do not fall into any of the other diagnostic categories of white patches are known as leukoplakia. They are important lesions because a small proportion have a higher risk of turning malignant (i.e. developing into squamous cell carcinoma) than does normal mucosa. Leukoplakia is therefore a premalignant lesion and identification of the ‘high-risk’ leukoplakias is important for the patient and dental care professional.
The clinical appearance of leukoplakia is very variable and they have been grouped into homogeneous and non-homogeneous types.
Homogeneous leukoplakia
- The lesions appear similar throughout and are usually flat, white patches, but some may have a regular undulating surface (Figure 3.4).
- This type of leukoplakia has a negligible risk of turning malignant.
Figure 3.4 Homogeneous leukoplakia affecting the gingival margin and palate.
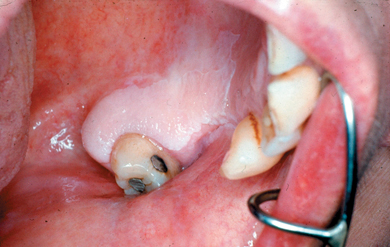
Non-homogeneous leukoplakia
- The lesions may show variations in the surface contour; they may be nodular or spiky.
- They may show variations in colour with red areas interspersed with white areas (Figure 3.5).
- It is within this group that the highest risk of malignant transformation occurs (Axell et al., 1996) and indeed some may be malignant from the onset.
Figure 3.5 Non-homogeneous leukoplakia occurring on the lateral border of tongue. Note the variation in colour: red areas interspersed with white areas.
The site of the leukoplakia is also important in determining the risk, as certain areas have a high risk of malignant change. These sites are the lateral border of the tongue, floor of the mouth and the retromolar area.
Aspects of the patient’s social history are also important as the risk of malignancy increases in patients who smoke and drink. There is also an increased risk in patients who take betel quid and in these patients the leukoplakia is often found on the buccal mucosa.
Pathological changes in leukoplakia
It is often difficult, if not impossible, to determine the risk of malignant transformation in leukoplakia by clinical examination alone and for this reason biopsies are often performed on such lesions, i.e. a small piece is removed and sent for histopathological examination. From a histopathological point of view the risk of malignant transformation is related to how abnormal the individual epithelial cells appear (atypia) and the extent to which this is present throughout the thickness of the epithelium. These changes together are referred to as dysplasia which is graded as mild, moderate and severe. The highest risk of malignant transformation lies within lesions showing severe dysplasia and these are usually removed surgically. Patients with lesions showing mild or moderate dysplasia may be kept under review.
Oral cancer
Oral cancer refers to cancers which arise in the oral cavity including the lips, tongue, mouth, oropharynx and hypopharynx as well as other ill defined sites. Almost 90% are squamous cell carcinoma which is a malignant neoplasm that arises from the oral epithelium.
Epidemiology of oral cancer
Oral cancer is the sixth most common cancer worldwide with an estimated 405 000 new cases per year. Two thirds of these are in developing countries (Cancer Research UK). The highest incidence (i.e. rates of oral cancer per 100 000 population) is found in parts of South-East Asia, and in Bangladesh, Sri Lanka and Pakistan it is the most common cancer in men. In Europe the highest incidence in men is found in France and Hungary.
The following points are important in the epidemiology of oral cancer in the UK:
- There were 5410 new cases of oral cancer diagnosed in the UK in 2007 (Cancer Research UK) and the incidence has increased by 50% for both men and women since 1989.
- The highest incidence of oral cancer in the UK is found in Scotland and this correlates with higher rates of tobacco and alcohol consumption.
- The majority of new cases occur in individuals over the age of 40 years with a peak incidence between 60 and 70 years.
- Men are affected more than women but the incidence in women is rising.
- The incidence is rising in younger individuals particularly the 40–60-year-old age groups. It is thought this is due to changes in alcohol consumption rather than an increase in tobacco consumption (Hindle et al., 2000) but one study has shown that a significant proportion of young patients have no risk factors (Llewellyn et al., 2003).
- The percentage of people who survive 5 years after diagnosis of oral cancer (all sites) is in the region of 50%.
- The survival figures vary depending on the site of the cancer. Almost all patients with cancer of the lip survive 5 years but the percentage of people who survive 5 years with cancer of the posterior parts of the mouth is very low.
Aetiology of oral cancer
The causes or aetiology of oral cancer are complex. There is little evidence for a strong genetic predisposition to oral cancer and environmental factors appear to be important. The risk of developing oral cancer is increased in individuals who smoke, use smokeless tobacco in the form of snuff or betel quid and is further increased in those who drink and smoke together. There is some evidence that in a small subset of patients human papillomavirus infection may play a role.
The following points should be noted:
- The most commonly affected sites are the lateral border of the tongue, floor of mouth and the retromolar region and about 80% of cancers in the Western world occur in these sites. This is related to alcohol consumption and smoking, two important risk factors in the development of oral cancer. It is thought that the carcinogens (chemicals that cause cancer, which are present in tobacco), dissolve in saliva and pool in these regions of the mouth.
- Alcohol itself is not carcinogenic (i.e. it does not contain carcinogens) but it potentiates the effects of carcinogens by increasing the permeability of the oral mucosa.
- In South-East Asia many cases of oral cancer are caused by betel quid chewing and occur on the cheeks adjacent to where the quid is placed. Studies have shown that immigrant populations from South-East Asia in the UK continue this habit and have a higher risk of developing oral cancer (Farrand et al., 2001; Warnakulasuriya, 2002).
- Cancer on the lower lip is caused by sunlight and is prevalent in fair-skinned individuals with outdoor occupations or lifestyles.
- A diet low in fresh fruit and vegetables is a risk factor for the development of oral cancer.
Pathology of oral cancer
In health the oral epithelium forms a continuous layer on the surface of the mucosa but in oral cancer the epithelium proliferates excessively due to genetic changes and eventually the epithelial cells grow down into the underlying connective tissue. This is known as invasion and is a characteristic feature of malignancy (Figure 3.6). The tumour cells continue to divide and invade and will spread into and destroy the underlying tissues which will then feel hard and not function properly. Tissues affected in this way may include skeletal muscle, salivary glands and bone. Tumour cells will also invade lymphatic vessels and spread to the cervical lymph nodes in the neck. This process is called metastasis.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


