Chapter 3
Occupational health and immunisation
PROVISION OF OCCUPATIONAL HEALTH
In this chapter, we will examine building a culture of safety, pre-employment health assessments, immunisation, exposure-prone procedures (EPPs) and health clearance, all of which contribute to staying healthy in the dental practice. In the working environment, members of the dental team are exposed to a number of hazardous substances such as natural rubber latex and disinfectants as well as microbial pathogens.
So, if you want to stay healthy in the dental practice then the first stage is to identify where the major occupational health hazards might lie.
Risk activities in dentistry that relate to occupational health include:
- Sharps injuries and exposure to blood-borne virus (see Chapter 4)
- Respiratory infections from inhaling contaminated aerosols from dental unit waterlines, e.g. Legionnaires’ disease and Pontiac fever, exacerbation of asthma by endotoxins and Gram-negative bacteria (see Chapters 6 and 9)
- Exposure to respiratory aerosols and secretions from infected patients, e.g. tuberculosis (TB), influenza, varicella, measles, rubella (see Chapter 6)
- Eye and skin infections, e.g. herpetic whitlow, impetigo, conjunctivitis (see Chapter 5)
- Hypersensitive reactions affecting skin and respiratory system, e.g. natural rubber latex, methyl methacrylate, glutaraldehyde (see Chapter 6)
- Mercury toxicity (see Chapter 10)
- Exposure to irradiation (outside the remit of this book)
Health and safety law requires the dentist to implement necessary measures to protect all members of the dental team and patients from such risks as far as is reasonably practicable.
BUILDING A CULTURE OF SAFETY
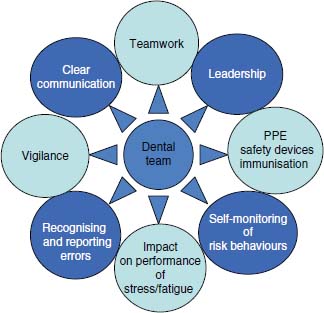
One of the main strategies for combating transmission of infection from person to person within the practice is to develop a culture of safety. Safe working practices, compliance with infection control policies, reporting injuries and near misses and effective management form the backbone of a dental practice safety culture. Personal protective equipment (PPE; see Chapter 6), sharps safety devices, immunisation and post-exposure prophylaxis (see Chapter 5) provide the protective defences against transmission of infection. Figure 3.1 illustrates how all these factors could come together to create a culture of safety within the dental practice.
This approach requires a commitment from the whole dental team if it is to be successful. Everyone in the dental team including students and trainees has an important contribution to make. Some of the steps the dental practice can take to create a safety culture are shown in Table 3.1.
Accidents such as sharps injuries will occur in the practice, however well it is run, but it is important to try and understand why an accident or a near miss occurred to prevent it from happening again. Mistakes and accidents tend not to be random mishaps but to fall into recurrent patterns, referred to as error traps. The same set of circumstances can provoke similar errors or accidents regardless of the member of staff or student who is involved. To be effective, cross-infection prevention necessitates looking beyond the simple explanation that it was someone’s fault and attempt to answer the much harder question as to ‘why’ the error occurred in the first place. There is seldom a single reason. Breakdowns in the practices infection control management and defences can arise from two main causes:
- Active failures
- Latent conditions
Figure 3.1 How the dental team can work together to build a safety culture.
Table 3.1 Steps involved in creating a practice safety culture
| A safety culture is created through: |
|
Active failures are unsafe acts committed by frontline people in direct contact with the patient. Their impact is usually instantaneous and breaches the integrity of the practice ‘defences’. In many cases, such acts have a causal history that extends back in time. The case scenario examples given below show how active and latent failures can combine and stack up with serious long-term consequences:
Example of an active failure: During a surgical extraction on a patient with hepatitis B the suture needle is covered by a bloody swab and both are discarded into a waste sack. The needle punctures the plastic and the cleaner receives a sharps injury when she empties the pedal bin.
Example of a series of latent failures: The cleaner had not been vaccinated against hepatitis B. She was a temporary cleaner from an agency and was covering for the practices regular cleaner who was on holiday. Nobody at the agency or the dental practice had checked if she was vaccinated against hepatitis B. Three months later she was diagnosed with hepatitis B. She worked at night after the practice had closed and had not reported the accident. As there was no record of the incident in the accident book, she was unable to prove where she acquired the infection from and was unable to make an insurance claim to which she would have been entitled.
Table 3.2 Where latent failures could occur in dental practice
| Poor design of surgery and equipment |
| Ineffective training |
| Inadequate supervision |
| Ineffective communications |
| Uncertainties in roles and responsibilities |
Whereas latent failures arise from decisions made on the design, procedures and management within the practice (see Table 3.2) or may relate to decisions taken outside the dental practice by third parties, such as equipment and instrument manufacturers, or government health authorities. Latent or delayed failures can remain dormant for many years until they combine with active failures and other local triggers to create an opportunity for an accident. If the dental practice’s infection-control policy and ‘defences’ function as intended, the results of the unsafe act are caught and the effects limited. If not, the accident could have tragic and long-term consequences (see the examples above). To prevent latent failures causing repeated incidents they require proactive rather than reactive responses on behalf of the dental team.
A way of highlighting active and latent failures in the dental practice is to use root cause analysis. Staff and students working on the ‘frontline’ are usually in the best position to identify issues and solution. The aim of a root cause analysis is to determine:
- What happened?
- Why did it happen?
- What can you do to prevent it from happening again?
ORGANISING STAFF HEALTH IN YOUR PRACTICE
Pre-employment health assessment
All new employees in the dental practice (including trainees, students, part-time and agency staff) should undergo a pre-employment health assessment which includes checking their vaccination history, flagging up any additional pre-employment vaccines they require based on a risk assessment of the duties they will be performing in the post, e.g. does the person have direct or close clinical contact with the patient. Do they perform EPPs?
Everyone working in the practice has a duty of care towards the patients, which includes taking reasonable precautions to protect them from communicable diseases. This can be achieved by appropriate immunisation against vaccine-preventable diseases. But immunisation should never be regarded as a substitute for safe working. Immunisation directly protects the individual and indirectly protects their family and friends, colleagues and vulnerable patients. Preventing communicable infections, e.g. influenza, promotes efficient running of the dental practice and reduces disruptions caused by the staff absent on sick leave.
Immunisation programme and staff health records
The dentists as employers need to be able to demonstrate that they have an effective employee immunisation programme in place. It is normally recommended that the practice nominates a person to coordinate the administration of staff health and the reporting and recording of accidents and near misses within the practice. The practice should keep a confidential record of health clearance records including hepatitis B antibody test results and occupational immunisation schedules. Include an alerting system in the records as this helps ensure that the records are contemporary and that all members of the dental team are up to date with booster vaccinations, although it is strongly recommended that immunisation programmes are managed by the local occupational health services. The following information will need to be recorded:
- Sharps injuries, accidents and incidents and near misses
- Pre-employment health clearance
- Date for booster vaccination
We know that underreporting of a sharps and a splash injury is common. It is helpful if the health coordinator in the dental practice understands the reasons why injuries are not reported or recorded and addresses barriers to reporting that apply in their own practice.
Failure to report accidents or near misses is due to:
- Fear of being accused of negligence
- Fear of being labelled accident prone
- Reputation with peers
- Conflict of loyalty to patient or practice (bear silent witness)
- Fear of subsequent medical treatment (sharps injuries)
- Lack of understanding of purpose of accident reporting
A wise man said, ‘To err is human’. High-risk industries with the potential for disastrous accidents such as nuclear power and airlines are pioneers in the field of industrial safety. Their excellent safety record is based on a nonblame approach, with the emphasis firmly on prevention, not punishment. Both industries have found this to be the best method to encourage reporting of incidents and near misses by their staff.
IMMUNISATION REQUIREMENTS FOR DENTISTRY
In the UK, it is recommended that all health care staff are up to date with routine vaccinations against tetanus, diphtheria, polio, and measles, mumps and rubella (MMR; Salisbury et al., Immunisation Against Infectious Disease – ‘The Green Book’, 2006). Clinical staff and students who have direct contact with patient or body fluids will require additional vaccinations for hepatitis B, TB (BCG vaccine) and varicella (if non-immune) (see Table 3.3). Annual vaccination in the autumn against seasonal influenza is strongly recommended for all members of the dental team. Increasing attention is being directed towards improving influenza vaccination uptake rates in all health care personnel. Antiviral drugs are available for the treatment of seasonal influenza, but in the UK, NHS doctors are permitted to prescribe the drugs only when the number of cases per week exceeds a Department of Health specified threshold. Avian flu and pandemic influenza are discussed in/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses