Chapter 3
ABCDE: Recognition and treatment of the acutely ill patient
INTRODUCTION
It is important to have a systematic approach to an acutely ill patient and to remain calm (Greenwood, 2009). The Resuscitation Council (UK) (2012) recommends undertaking a systematic clinical assessment following the ABCDE approach: pre-empting a medical emergency would allow appropriate help, e.g. ambulance, to be called, hopefully before the patient deteriorates or collapses. As well as monitoring the patient’s vital signs, e.g. respiratory rate, pulse and blood pressure it is also important to be alert to the presence of chest pain (see Chapter 6), a common pre-cardiac arrest symptom (Resuscitation Council (UK), 2012).
The aim of this chapter is to understand the principles of recognition of the acute ill patient following the ABCDE approach.
CLINICAL SIGNS OF ACUTE ILLNESS AND DETERIORATION
The clinical signs of acute illness and deterioration are usually similar regardless of the underlying cause, because they reflect compromise of the respiratory, cardiovascular and neurological functions (Nolan et al., 2005). These clinical signs are commonly:
- Tachypnoea (respiratory rate > 20/min): a particularly important indicator of an at-risk patient (Goldhill et al., 1999) and is the most common abnormality found in acute illness (Goldhill and McNarry, 2004);
- Tachycardia (heart rate > 100 beats per minute);
- Hypotension (usually a systolic blood pressure < 90mmHg);
- Altered consciousness level (e.g. lethargy, confusion, restlessness or falling level of consciousness) (Resuscitation Council (UK), 2012; Jevon and Ewens, 2012).
The identification of the clinical signs of acute illness (together with the patient’s history, examination and appropriate investigations) is central to objectively identifying patients who are acutely ill or deteriorating (Buist et al., 1999). However, these clinical signs of deterioration are often subtle and can go unnoticed. It is therefore important to assess the patient following the systematic ABCDE approach.
THE ABCDE APPROACH
The Resuscitation Council (UK) (2012) has issued guidance on the recognition and treatment of the sick patient following the logical and systematic ABCDE approach:
- Airway;
- Breathing;
- Circulation;
- Disability;
- Exposure.
When assessing the patient, undertake a complete initial assessment, identifying and treating life-threatening problems first, before moving on to the next part of assessment. The effectiveness of treatment/intervention should be evaluated, and regular reassessment undertaken. The need to call for an ambulance should be recognised and other members of the multidisciplinary team should be utilised as appropriate so that patient assessment, instigation of appropriate monitoring and interventions can be undertaken simultaneously.
Irrespective of their training, experience and expertise in clinical assessment and treatment, all dental professionals can follow the ABCDE approach; clinical skills, knowledge, expertise and local circumstances will determine what aspects of the assessment and treatment are undertaken.
GENERAL PRINCIPLES OF THE ABCDE APPROACH
The general principles of the ABCDE approach to assessing the acutely ill patient are as follows:
- The ABCDE approach should be followed when both assessing and treating the patient.
- Life-threatening problems, once identified, should be treated before moving on to the next part of the assessment.
- If there is further deterioration, reassessment should be performed, starting with the airway.
- The effects of any treatment administered should be evaluated.
- The need for extra help, e.g. calling 999 for an ambulance, should be considered.
- All the members of the dental team should be involved, allowing essential tasks such as collecting emergency equipment and oxygen or calling 999 for an ambulance to be undertaken simultaneously.
- Effective organisation and communication within the dental team are paramount.
- The initial aim of treatment is to keep the patient alive, prevent deterioration and ideally achieve clinical improvement; hopefully this will buy time while awaiting expert help and more definitive treatment.
- The ABCDE approach can be used by dental professionals irrespective of their training, expertise and experience in clinical assessment or treatment; individual experience and training will determine which aspects of assessment are undertaken and which treatments are administered.
- Basic interventions, e.g. laying the patient flat or administering oxygen, are often all that are required.
Source: Resuscitation Council (UK) (2012)
THE ABCDE APPROACH TO THE SICK PATIENT
Safety
Ensure the environment is safe and free of hazards and follow infection control guidelines, e.g. wash hands, put on gloves if necessary.
Communication
Talk to the patient and evaluate his response: a normal response, indicates he has a clear airway, is breathing and has adequate cerebral perfusion; the inability to complete sentences could indicate extreme respiratory distress. An inappropriate response or no response could indicate an acute life-threatening physiological disturbance (Gwinnutt, 2006), e.g. inability to complete sentences in one breath is a severe adverse sign in a patient having an asthmatic attack (British Thoracic Society, 2008).
Patient’s general appearance
Note the patient’s general appearance, his colour and whether he appears content and relaxed or distressed and anxious.
Senior help
It is important to call for help at a very early stage – this includes anything from other members of the dental team to calling for an ambulance (Greenwood, 2009). Request help from the senior dental practitioner. During the assessment process, consider whether it is necessary to call 999 for an ambulance.
Oxygen, emergency equipment/drugs
Ask a colleague to fetch the oxygen and other emergency equipment/drugs if required.
Monitoring devices
If one is available, attach a pulse oximeter (see principles of pulse oximetry section later) (Resuscitation Council (UK), 2012).
Airway
Assessment of airway
During the assessment of the airway, it is important to quickly establish if it is obstructed and treat it effectively. Look, listen and feel for the signs of airway obstruction. Partial airway obstruction will result in noisy breathing.
- Gurgling: indicates the presence of fluid, e.g. secretions or vomit, in the mouth or upper airway; usually seen in a patient with altered level of consciousness who is having difficulty or is unable to clear his own airway.
- Snoring: indicates that the pharynx is being partially obstructed by the tongue; usually seen in a patient with altered level of consciousness lying in a supine position.
- Stridor: high-pitched sound during inspiration, indicating partial upper airway obstruction; usually due to either a foreign body or laryngeal oedema.
- Wheeze: noisy musical whistling type sound due to the turbulent flow of air through narrowed bronchi and bronchioles, more pronounced on expiration; causes include asthma and chronic obstructive pulmonary disorder (COPD).
- Complete airway obstruction can be detected by no air movement at the patient’s mouth and nose. Paradoxical chest and abdominal movements (‘see-saw’ movement of the chest) may be observed and, if not rapidly treated, central cyanosis will develop (late sign of airway obstruction).
Treatment of airway obstruction
Airway obstruction is a medical emergency. If untreated, it can lead to hypoxia/hypoxaemia (low oxygen levels in the blood), which can damage the brain, kidneys and heart; cardiac arrest and even death could ensue (Resuscitation Council (UK), 2011).
If the patient has airway obstruction, whether partial or complete, treat the underlying cause if possible. In most situations, simple interventions are sufficient to clear the airway. For example:
- Perform head tilt, chin lift to open the airway in an unconscious patient (see Chapter 10).
- Suction the pharynx if there is blood or vomit in it.
- Consider inserting an oropharyngeal airway to help keep a patent airway in an unconscious patient (see Chapter 10).
- Perform back slaps and abdominal thrusts as necessary if there is foreign body airway obstruction (see Chapter 10).
- Administer oxygen 15 l/min via a non-rebreathe mask (Figure 3.1) (see Chapter 10) (Jevon and Ewens, 2012).
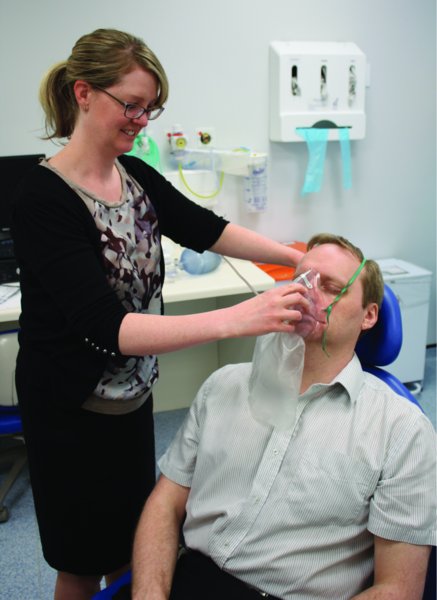
Figure 3.1 Administering high concentration of oxygen via a non-rebreathe mask.
Breathing
Assessment of breathing
During the assessment of breathing, it is important to quickly diagnose and treat any life-threatening breathing problems, e.g. acute asthma (Resuscitation Council (UK), 2012). Follow the familiar ‘look, listen and feel’ approach to assess breathing:
- Count the respiratory rate: normal respiratory rate is 12–20 beats per minute (Resuscitation Council (UK), 2012). Tachypnoea (fast respiratory rate) is usually the first sign that the patient has respiratory distress. It is an indicator of illness, that the patient may deteriorate and that medical help is required (Resuscitation Council (UK), 2012). Bradypnoea (slow respiratory rate) is an ominous sign and could indicate imminent respiratory arrest; causes include drugs, e.g. opiates, and fatigue.
- Evaluate chest movement: chest movement should be symmetrical; unilateral chest movement suggests unilateral pathology, e.g. pneumothorax, pneumonia, pleural effusion.
- Evaluate the depth of breathing: only marked degrees of hyperventilation and hypoventilation can be detected; hyperventilation may be seen if the patient is having a panic attack (Ford et al., 2005).
- Note the oxygen saturation (SaO2) reading (if available): the normal reading is usually 97–100%. A low SaO2 could indicate respiratory distress or compromise.
- Listen to the breathing: normal breathing is quiet. Rattling airway noises indicate the presence of airway secretions, usually due to the patient being unable to cough sufficiently or unable to take a deep breath in. The presence of stridor or wheeze indicates partial, but significant, airway obstruction (see Assessment of airway section above).
Treatment of compromised breathing
If the patient has compromised breathing it is paramount to provide prompt effective treatment. In addition, during the initial assessment of breathing, it is essential to diagnose and effectively treat immediately life-threatening conditions, e.g. acute severe asthma (Resuscitation Council (UK), 2012). If the patient has compromised breathing:
- Position the patient in an upright position to help maximise chest movement; if he is in the dental chair, he may find it helpful to sit on the side of the chair with his legs down and feet touching the floor.
- Administer high concentration of oxygen via a non-rebreathe mask (Figure 3.1) (see Chapter 10) (Jevon and Ewens, 2012); If possible treat the underlying cause. In the dental practice the most likely cause of compromised breathing that could be treated is asthma, i.e. administer beta agonist inhaler (see Chapter 4).
Circulation
Assessment of circulation
- Count the pulse (radial or carotid): a weak pulse suggests a poor cardiac output. In a vasovagal attack, the pulse is slow; in anaphylactic shock the pulse is fast.
- Check the colour and temperature of the hands and fingers: signs of cardiovascular compromise include cool and pale peripheries.
- Measure the capillary refill time (CRT): holding a fingertip at the level of the heart, apply sufficient pressure for 5 seconds to cause blanching of the skin, and then release (Figure 3.2). Normal CRT is less than 2 seconds; a prolonged CRT could indicate poor peripheral perfusion, though other causes can include cool ambient temperature, poor lighting and old age (Resuscitation Council (UK), 2012). A prolonged capillary refill time may be seen in anaphylaxis.
- Measure the blood pressure: a systolic BP <90 mm Hg suggests shock.
- Establish if the patient has chest pain: central crushing chest pain is suggestive of a heart attack (see Chapter 5).
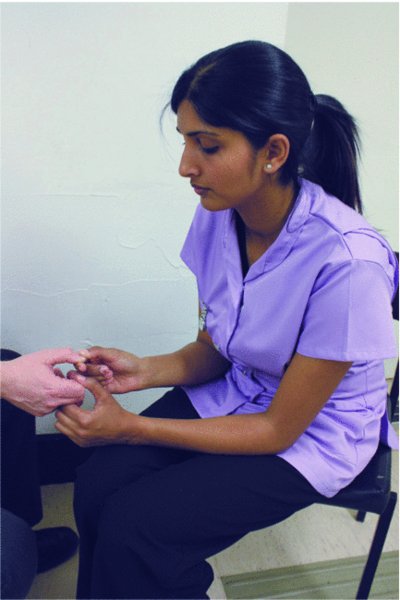
Figure 3.2 Measuring capillary refill time.
Treatment of a problem with circulation
The treatment of a problem with circulation will depend on the cause:
- Low blood pressure due to a vasovagal episode or simple faint: lay the patient flat with the legs raised (often, no other treatment is required) (see Chapter 5).
- Anaphylactic shock: lay the patient flat with the legs raised (unless this compromises breathing), administer high concentration of oxygen and administer adrenaline, wh/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


