29
Anaesthesia and diabetes
Diabetes mellitus in patients undergoing major surgery poses a number of serious problems for the anaesthetist, particularly insulin-dependent diabetes. It is an independent predictor for serious postoperative complications such as perioperative myocardial infarction, renal failure, infections, mortality as well as length of hospital stay. In obstetrics, mothers with diabetes have a much higher incidence of stillbirth and congenital malformations. In addition, in the intensive care unit, for patients with and without diabetes, tight glycaemic control reduces both morbidity and mortality.
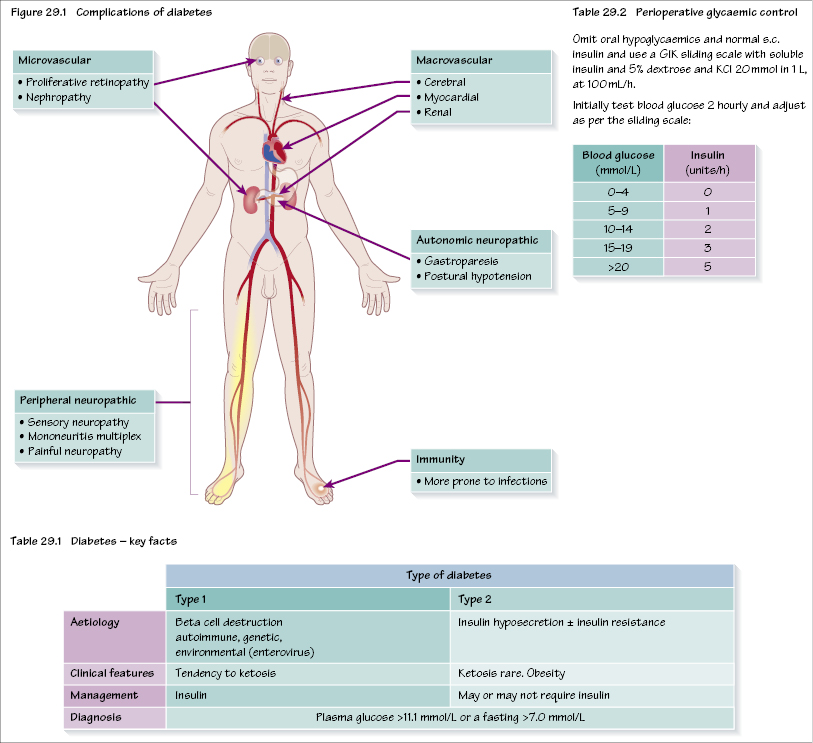
The key features of diabetes are shown in Table 29.1 and some of the major complications in Figure 29.1.
The essence of managing diabetes is to ensure good glycaemic control with rapid return to normal diet and medication. In addition, because of the potential for associated problems, especially vascular disease, patients need to be monitored for complications of this, such as myocardial ischaemia. Moreover, poor glycaemic control may precipitate diabetic ketoacidosis (DKA) or hyperosmolar non-ketotic coma (HONK), both of which carry a significant mortality. Many of the endocrine changes that occur following major surgery (e.g. increase in catecholamines, cortisol and glucagon) may increase blood glucose further (and indeed many patients without diabetes can have high blood glucose following major surgery).
General management of blood glucose in patients with diabetes
Good glycaemic control may involve a good preoperative diet and weight loss, and perioperative insulin.
Insulin
This is required in the treatment for Type I diabetes. In addition, patients with Type 2 diabetes undergoing major surgery may need insulin.
There are three types of insulin:
- soluble insulin (rapid onset and short duration of action);
- intermediate duration of action;
- longer duration of action.
The latter two are insoluble as they are mixed with protamine or zinc to delay absorption, and can only be given subcutaneously. Patients are normally converted to soluble insulin preoperatively.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


