Chapter 28 Perioesthetics
Section A Periodontal Esthetics and Periodontal Plastic Surgery
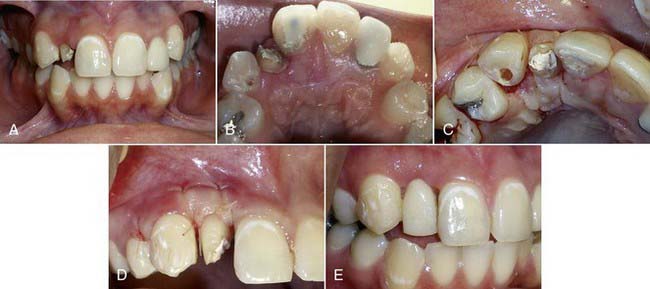
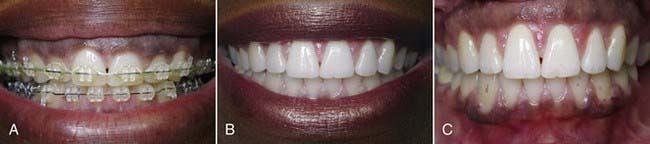
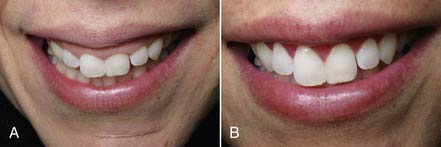
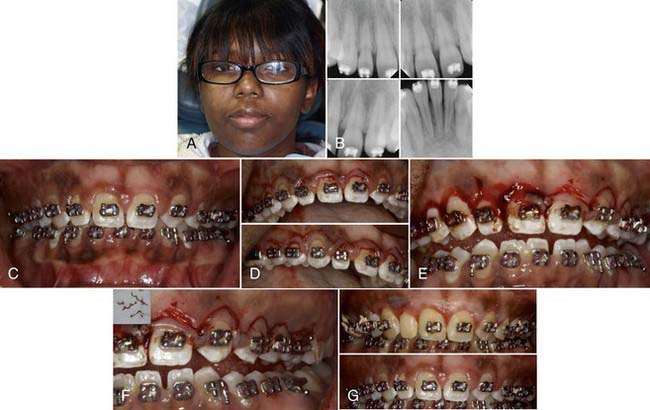
Clinical Cases
American Academy of Periodontology. Local delivery of sustained or controlled release antimicrobials as adjunctive therapy in the treatment of periodontitis. J Periodontol. 2006;77:1458.
Drisko CL, Cochran DL, Blieden T, et al. Position paper: Sonic and ultrasonic scalers in periodontics. Research, Science and Therapy Committee of the American Academy of Periodontology. J Periodontol. 2000 Nov;71(11):1792-1801.
Fedi PF, Vernino A, Gray J. The periodontic syllabus, ed 4. Philadelphia: Lippincott Williams & Wilkins; 2000.
Lindhe J, Lang NP, Karring T. Clinical periodontology and implant dentistry, ed 5. Oxford: Blackwell Munksgaard; 2008.
Misch CE. Contemporary implant dentistry, ed 3. St Louis: Mosby Elsevier; 2008.
Newman M, Takei H, Klokkevold P, Carranza F. Carranza’s clinical periodontology, ed 11. St Louis: Saunders-Elsevier; 2011.
Suzuki JB, Misch CE, Brunstein D, Mortilla LD. Contemporary implant dentistry, ed 3. St Louis: Mosby-Elsevier; 2008. pp 1073-1088
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses