CHAPTER 20
Soft Tissue Injuries
Jason Jamali, Antonia Kolokythas, and Michael Miloro
Department of Oral and Maxillofacial Surgery, College of Dentistry, University of Illinois Chicago, Chicago, Illinois, USA
Stensen’s Duct Repair
A means of reestablishing parotid salivary flow through a damaged or severed Stensen’s duct (parotid duct).
Indication
- Traumatic transection of Stensen’s duct
Contraindications
- Partial transaction with adequate salivary flow through the orifice of Stensen’s duct
- Intervention may be delayed in the medically compromised or unstable patient.
Anatomy
Parotid duct (Stensen’s duct): The anticipated course of the parotid duct is predicted by drawing a line from the tragus of the ear to the mid-portion of the upper lip. Stensen’s duct originates from the anterior portion of the parotid gland and continues anteriorly toward the anterior border of the masseter muscle. At the level of the masseter muscle, the duct courses medially piercing through the buccal fat pad and buccinator muscle before terminating at its papilla orifice within the buccal mucosa adjacent to the maxillary second molar. The length of the duct is approximately 7.0 cm. Both the zygomatic and buccal branches of the facial nerve may cross the path of Stensen’s duct.
Parotid Duct Repair Technique
- A thorough clinical examination is performed to evaluate facial nerve function as parotid duct injuries frequently occur in conjunction with facial nerve injuries.
- The patient is placed under general anesthesia within an operating room. Short-acting paralytics are used to allow for further facial nerve stimulation with a nerve stimulator during the procedure. The patient is prepped intraorally and extraorally and draped to allow for full exposure of the facial wounds.
- The facial wounds are debrided and irrigated with light pressure. Pulsatile irrigation is deferred in cases where the facial nerve is exposed or damaged.
- Exploration of the wound is commonly performed with magnification (loupe vs. operating microscope).
-
The duct is cannulated intraorally via the orifice of Stensen’s duct with an IV angiocatheter (Figure 20.5, Case Report 20.2), or a 16-gauge epidural catheter. Lacrimal probe dilation is typically necessary to enlarge the duct to accommodate a catheter (Figure 20.2, Case Report 20.1 and Figure 20.4, Case Report 20.2).
- Saline or propofol (TEVA Pharmaceuticals, North Wales, PA, USA) is injected through the cannula while the wound is observed for leakage. Toluidine blue has been used in the past, but typically it obscures the remainder of the field for repair.
- If present, the location of transection is confirmed, and an attempt is made to identify and cannulate the proximal end of the duct over the same cannula placed transorally, obturating the distal portion of the duct. A blue background may be placed for visual enhancement of the surgical field.
- Primary anastomosis is performed over the cannulated ends of the duct using nonresorbable nylon (9-0, 10-0) or silk (7-0, 8-0) sutures.
- For large segmental defects of the duct, microsurgical repair with interposition grafting may be considered. Donor veins include the facial vein, the saphenous vein, and veins from the forearm.
- Distal ductal injuries may be treated through a fistulization procedure where the cannulated duct proximal to the injury is diverted intraorally and sutured to the buccal mucosa, creating a new orifice.
- Proximal injuries closer to the duct and those with extensive parenchymal damage may be treated with ligation of the proximal stump. Salivary flow may be decreased using anticholinergic medications or low-dose radiation to the gland.
- After definitive treatment of ductal discontinuity, the parotid capsule is closed in order to minimize sialocele formation. If extensive parenchymal damage is present, a drain is placed and sewed to the anterior skin edge of the wound.
- The wound is irrigated and closed in layers, and a pressure dressing is applied for 48 hours.
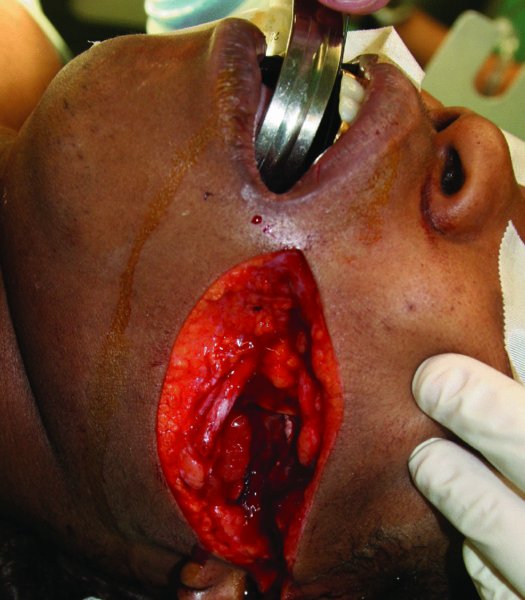
Figure 20.1. Deep facial laceration involving the parenchyma of the parotid gland.
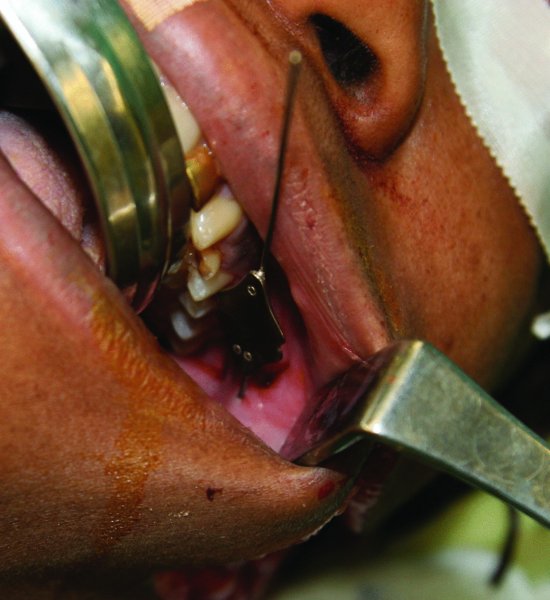
Figure 20.2. Complete cannulation of the parotid duct with a lacrimal probe confirmed no involvement of the parotid duct in this injury.
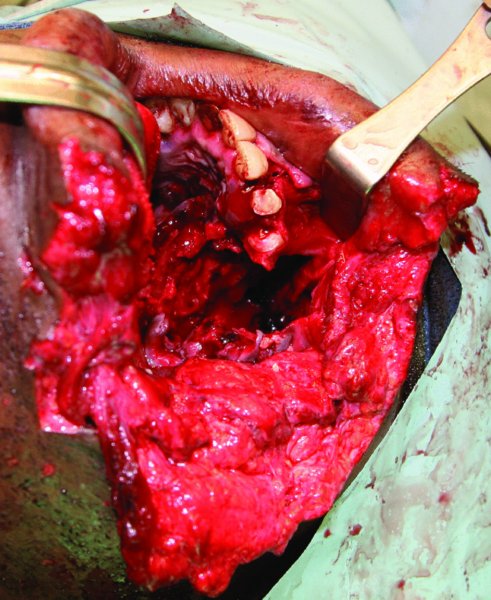
Figure 20.3. Extensive hard and soft tissue injuries to the parotid region.
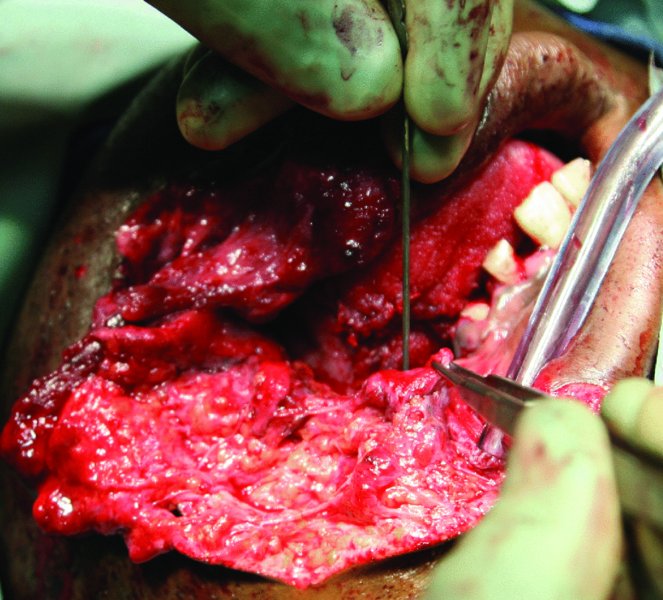
Figure 20.4. Lacrimal probe used to identify and dilate the proximal aspect of the parotid duct.
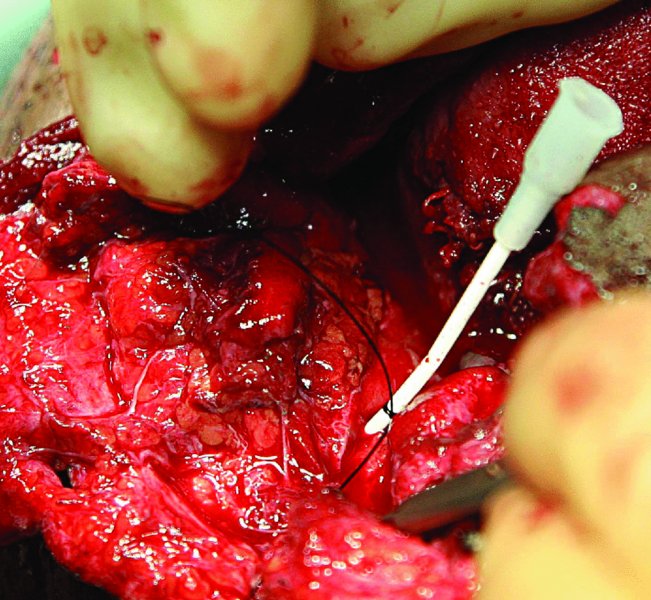
Figure 20.5. The proximal end of the duct is cannulated with an angiocatheter. The distal end of the parotid duct could not be located due to the extensive soft tissue injuries. The catheter was sewn into the intraoral buccal mucosa to create a new orifice.
Postoperative Management
- Pressure dressings are removed after 48 hours.
- If present, drains are removed after 1 week.
- The intraoral stent or catheter is removed after 2 weeks.
Complications
- Sialocele and salivary fistula formation: May result from unidentified or incompletely repaired ductal injury, extensive parenchymal gland damage, or failure to adequately close the parotid capsule. Early management involves opening the anterior aspect of the wound and placing a drain, pressure dressings, repeat aspirations, anti-sialagogues, and anti-cholinergic medications. Late management includes botulinum toxin injections, tympanic neurectomy, parotidectomy, and low-dose radiation therapy.
- Salivary gland hypofunction: In the event that parotid injury or ductal repair results in decreased salivary flow, artificial salivary substitutes, sialogogues, or cholinergic medications may be used to augment saliva production.
- Facial nerve deficits: These should be followed with neurosensory testing in cases in which facial nerve function has been demonstrated to be intact, and only transient deficits are expected (neurapraxia and axontotmesis). With transaction injuries of the facial nerve (neurotmesis), repair is indicated.
Key Points
- All deep facial lacerations involving the parotid gland should have the parotid duct cannulated in order to evaluate the integrity of Stensen’s duct (Figure 20.2, Case Report 20.1).
- Ductal injuries overlying the masseter muscle are most amenable to repair, whereas intraparenchymal ductal injuries are difficult to identify and repair. Distal ductal injuries may be treated with fistulization or redirection of the duct intraorally within the buccal mucosa.
- The choice of ductal repair is dependent upon the location of injury and the ability to identify both proximal and distal ends of the parotid duct.
- Delayed repairs may be complicated by sialocele formation and scar formation. Immediate primary repair is preferred.
- Sialography may be used preoperatively to diagnose ductal injury. Sialography may also be used postoperatively to evaluate and monitor the status of the repair and function of the parotid gland.
- Damage to the facial nerve must be ruled out with penetrating injuries to the parotid region.
- All hard and soft tissue injuries require meticulous debridement and closure, with special emphasis placed on aligning the vermilion border of the lip if involved.
References
- Demian, N. and Curtis, W., 2008. A simple technique for cannulation of the parotid duct. Journal of Oral and Maxillofacial Surgery, 66, 1532–3.
- Lewkowicz, A.A., 2002. Traumatic injuries to the parotid gland and duct. Journal of Oral and Maxillofacial Surgery, 60, 676–80.
- Liang, C., 2004. Reconstruction of traumatic stensen duct defect using a vein graft as a conduit: two case reports. Annals of Plastic Surgery, 52, 102–4.
- Lim, Y.C., 2008. Treatment of an acute salivary fistula after parotid surgery: botulinum toxin type A injection as primary treatment. European Archives of Otorhinolaryngology, 265, 243–5.
- Steinberg, M.J., 2005. Management of parotid duct injuries. Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, and Endodontology, 99, 136–41.
- Sujeeth, S., 2011. Parotid duct repair using an epidural catheter. International Journal of Oral and Maxillofacial Surgery, 40, 747–8.
- Van Sickels, J.E., 2009 Management of parotid gland and duct injuries. Oral and Maxillofacial Surgery Clinics of North America, 21, 243–6.
- Von Lindern, J.J., 2002. New prosepects in the treatment of traumatic and postoperative parotid fistulas with type A Botulinum toxin. Plastic and Reconstructive Surgery, 109, 2443–5.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


