20
Medical Emergencies
I. General Principals of Emergency Medical Care
Medical emergencies are best prevented. Regardless of prevention approaches, emergencies occur in dental practice, and preparation enhances the dental team’s ability to recognize patient distress and react immediately to the emergency. Obtaining adequate perioperative pain, fear, and anxiety control plays an important role in preventing escalation of the stress response into an emergency situation.
- Obtain written and interview dialog health history or updates at each visit.
- Obtain vital signs at initial and recall exams and prior to use of local anesthetic or surgical procedures, or more frequently as health history dictates.
- Make needed treatment modifications, including use of stress and anxiety management protocols.
- Recognize early signs of patient distress and address the cause to prevent escalation, including terminating dental treatment if needed.
Preparation includes dentist and staff training and maintaining in the office basic airway rescue and monitoring equipment and basic emergency medications.
The likelihood of a competent and timely initial emergency response in the dental office is enhanced by the dental team receiving annual medical emergency education updates. Team participation in mock medical emergency drills in the office, were members actually rehearse the roles they would play in responding to potential emergency scenarios, can create a safer dental office environment.1–3 Emergency response scenarios that are routinely practiced by the dental team in a nonemergency situation, will come more naturally, without the initial panic typically generated by the emergency, should the emergency situation arise with a real patient where response times and professional decision making can matter between life and death or morbidity.
- Learn to identify signs of patient distress related to the most common medical emergencies in the dental office.
- Maintain current basic life support (BLS) certification for all office staff.
- Attend continuing education courses in emergency medicine.
- Conduct periodic office “mock” emergency drills.
- Post the telephone number of the emergency medical response service (e.g., 911) near each telephone.
- Maintain an updated emergency drug kit and automated external defibrillator equipment, where required by state law, and have staff demonstrate the knowledge to properly use all items.
- Portable oxygen cylinder (E size) with regulator (see Fig. 20.1)
- Supplemental oxygen delivery devices (nasal cannula, non-rebreathing mask with oxygen reservoir, nasal hood)
- Bag/valve/mask device with oxygen reservoir (see Fig. 20.2)
- Oropharyngeal airway (adult sizes 7, 8, 9 cm)
- Magill forceps
- Automated external defibrillator
- Stethoscope
- Sphygmomanometer with adult small, medium, and large cuff sizes
- Wall clock with second hand
Figure 20.1 Portable oxygen cylinder with regulator and nasal cannula and nonrebreathing mask in plastic attached of handle of cart.

Figure 20.2 Bag/valve/mask.

- Positive pressure/demand valve:
- Full mask permitting 100% O2 delivery
- Bag/valve/mask device:
- Full mask permitting delivery of 21% O2 ambient air, or enriched O2 if attached to an E cylinder (25–90% O2)
- Pocket mask:
- Face mask that permits mouth-to-mask ventilation, providing 16% O2 (exhaled air)
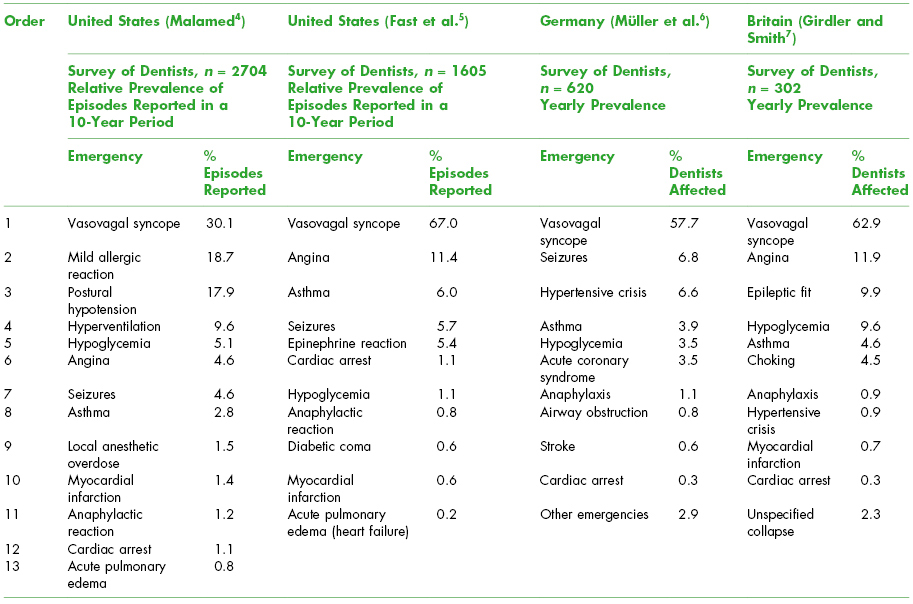
As shown in Table 20.1, surveys of dentists indicate that vasovagal syncope, affecting most dentists, is the most commonly reported emergency episode in dental offices.4–7 Other common emergencies include angina/acute coronary syndrome, mild allergic reactions, seizures, postural hypotension, asthma, hypoglycemia, hyperventilation, hypertensive crisis/epinephrine reaction, choking/airway obstruction, myocardial infarction, local anesthetic overdose, anaphylaxis, and cardiac arrest.4–7
Table 20.1. Frequency of Occurrence of Medical Emergencies in Dental Practices, Based on Dentist Surveys
When the emergency medical service (EMS) first responders are called to the office, the dental team should be prepared to quickly and efficiently relay information about the patient, the emergency situation, and the efforts made to manage the condition.
- Presumed diagnosis (e.g., “possible myocardial infarction”)
- Patient information (e.g., “Mr. Smith is a 63-year-old male with a history of angina, currently experiencing chest pain not relieved by sublingual nitroglycerin. He is conscious, with blood pressure of 161/93 and heart rate of 88 beats per minute.”)
- Current patient supportive care (e.g., “The patient is supine and has received three sequential sublingual nitroglycerine tablets, followed by 325 mg chewed aspirin. The patient is receiving 4 L of oxygen by face mask.”)
- Location of office where emergency responders need to report (e.g., “Dr. Sweet’s dental office on the ground floor suite 100 at 495 East Avenue at the corner of East Avenue and Northern Boulevard.”)
- Phone number from which the call is being made (The dental staff caller should stay on the line with EMS until they have arrived at the office. Giving the phone number allows EMS responders to contact the office should the line be inadvertently disconnected.)
II. Emergency Drugs and Use
Emergency drugs that the dentist knows how to use should be readily available.1 While there is no universal agreement as to which drugs should be included in the basic kit, most agree upon inclusion of a positive pressure oxygen delivery system, 1:1000 injectable epinephrine, injectable histamine-blocker-diphenhydramine, nitroglycerine sublingual tablet or spray, bronchodialator-albuterol, aspirin, glucose-sugar packet, and aromatic ammonia as shown in Table 20.2.1,2 Emergency kits should be routinely maintained with replacement of soon to expire medications. Dentists should consult their state laws and liability insurance carrier to ascertain if there is a mandated list of emergency drugs and equipment that they must have available at the office.2 Increasingly, states are requiring dental offices to have an automated external defibrillator (AED) on-site and have staff trained in its use.
Table 20.2. Basic Emergency Drugs for the Dental Office
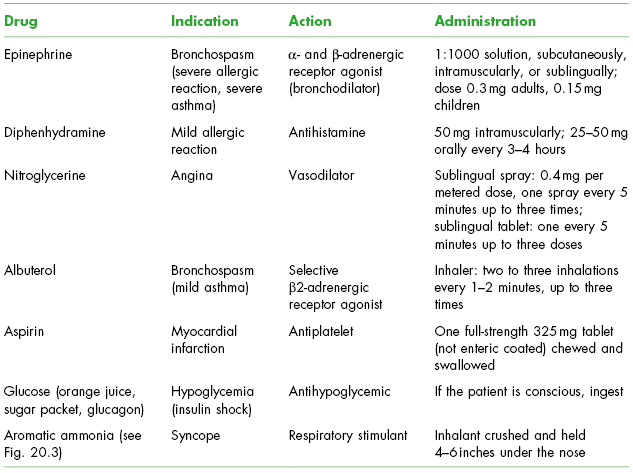
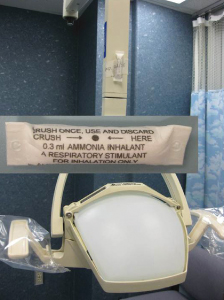
Figure 20.3 Crushable ammonia inhalant (close-up, see insert) affixed to each operatory overhead light for ease of access. Tape holding stimulant is marked with expiration date. Aromatic ammonia spirit crushed and held 4 inches from the nose, acts as a respiratory stimulant for syncope treatment by causing peripheral irritation of the sensory receptors in the nasal mucous membranes. Avoid use in patients with known respiratory disease.
Depending on the dentist’s level of training in management of medical emergencies, types of procedures and techniques, levels of sedation offered, and special needs of the dental office, additional emergency drugs such as naloxone, flumazenil, midazolam, morphine, nitrous oxide, hyd/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


