Chapter 2
Understanding and respect: caring for patients with special needs
Liana Zoitopoulos
Aim
The aim of this chapter is to explain the meaning of the term special needs and to address the special considerations required and issues raised when caring for patients with special needs.
Outcome
The chapter should lead to an understanding of what is meant by the term patients with special needs, and the importance of respecting each patient’s individuality while taking into account the whole team that cares for such patients.
The mark of a civilised society is the way it treats its disabled people.
Introduction
Definitions
Disability is defined as ‘an anatomical, physiological or psychological loss or reduction in functional ability’. Impairment is defined as ‘a disadvantage or restriction of activity due to a disability’.
The term special needs is commonly used to describe people who, because of a disability, are unable to perform some, many or all of the functions of everyday living. The terms special needs, disability, impairment and special care are all used to describe people who for a variety of reasons are in need of additional care. These terms will be used throughout this chapter.
Changing views of people with disability and special needs through time
Society has viewed disabled people in very different ways over the centuries. For example, babies born with disabilities in ancient Sparta were deemed potentially unfit to live. Legend has it that they were left exposed on the inhospitable slopes of Mount Taygetos and only collected and taken home if they survived the night. Other sources say that they may have been thrown off a cliff. This attitude to those with impaired function seems to have been common in ancient times, although equally there are examples of people with disability achieving high office even then. In more recent times, the Victorians constructed buildings and transport systems that were impossible to access or use by many physically disabled people. Although lunatic asylums provided asylum for the mentally ill, there was also a perception that such institutions were required to separate those with mental illness from the community.
Often, the general population is ignorant about disability. People do not know how to behave and what is required of them when they are in the company of disabled persons. This is perhaps a reason why disabled people have tended to be excluded and isolated from mainstream general activities. They have also tended to be stigmatised. For example, in many cultures it remains difficult for parents to talk about having a disabled child. These are some of the reasons why disabled people have been placed in closed institutions, making integration with the rest of society difficult, if not impossible. There are many such examples even today. In parts of Europe, disabled children have been abandoned in institutions with very little care and no education whatsoever. Some countries still isolate people if they are infected with the human immunodeficiency virus (HIV) or have mental incapacity or illness. This has typically resulted in isolation and loss of dignity.
In the UK, even as recently as the late 20th century, society has tended to isolate disabled people, including those with mental illness. Disabled people were made dependent and institutionalised and to some extent this is still true. This approach, however, began to change towards the end of the last century when the move towards integration and empowerment of disabled people was initiated.
Of course, the creation of disabled entrances for buildings, although seemingly enabling inclusion, reinforces the impression that disabled people require special measures. More enlightened countries have placed a legal duty on those constructing public buildings to make them readily accessible to all through common entrances. Essentially, we have to decide whether the able-bodied and the disabled are two separate groups or part of the spectrum of humanity. The latter view, that those with disability are entitled to equal treatment, has been aided in the UK by the following legislation.
Disability Discrimination Act 1995
A person has a disability for the purposes of the Disability Discrimination Act if s/he has a physical or mental impairment which has a substantial and long-term adverse effect on his/her ability to carry out normal day-to-day activities. The Disability Discrimination Act 1995 requires that providers must:
-
take reasonable steps to change policies, practices and procedures which make it unreasonably difficult or impossible for disabled people to use their services
-
take reasonable steps to remove or alter physical features which could be a barrier to disabled people using their services
-
provide the service in an alternative way if the removal of such barriers is impossible
-
consider access to a service in broad terms that includes access to information about a service (e.g. information available as audio, large print and so on).
Disability Discrimination Act 2006
The 2006 modification of the original Disability Discrimination Act was designed to extend the rights for disabled people. It provided protection against discrimination for people using public services and it created new legal responsibilities for local authorities, agencies and other public bodies.
Mental Capacity Act 2005
The Mental Capacity Act, which came into full operation in October 2007, aims to protect people who cannot make decisions for themselves because of a learning disability, mental health condition or any other reason. It provides clear guidelines for carers and professionals about who can take decisions in which situations.
The Mental Capacity Act intends to protect people who lose the capacity to make their own decisions. It will:
-
allow anyone, while they are still able, to appoint someone (e.g. a trusted relative or friend) to make decisions on their behalf in the event that they lose the ability to do so; the nominated individual can make decisions on the person’s health and personal welfare where previously such an appointment only covered financial matters
-
ensure that decisions that are made on the person’s behalf are in their best interests and it provides a checklist of things that decision makers must work through
-
introduce a code of practice for people such as healthcare workers who support people who have lost the capacity to make their own decisions.
The above changes in attitude and legislation have made at least the UK a far better place for disabled people. There is, however, still a long way to go.
Provision of oral care for disabled people
The branch of dentistry which tends to deal with the majority of disabled patients is known as special care dentistry (SCD). Its role has been defined in the UK by the Joint Advisory Committee for Special Care Dentistry as ‘the improvement of oral health of individuals and groups in society who have a physical, sensory, intellectual, mental, medical, emotional or social impairment or disability or, more often, a combination of a number of these factors’.
SCD covers a diverse client group with a range of disabilities and complex additional needs. It must deal with people living at home, in long-stay residential care or in secure units, in addition to the homeless. It requires a holistic approach that is specialist led to meet the complex requirements of people with impairments.
During the journey from receiving a referral to providing oral care for a patient with special needs to completing their care, it must always be kept in mind that there are two distinct types of patient to consider. SCD provides simple dental care for patients with complex comorbidities, or complex dentistry for patients with more straightforward problems (Fig 2-1). Finally, some patients seen by the SCD team are in the transition period between paediatric and adult services, when it is easy for them to be lost in the system.
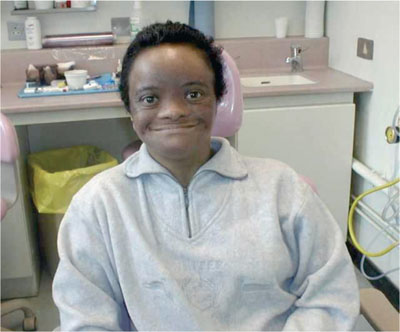
Fig 2-1 Intellectually impaired patient with simple dental needs.
There are several types of impairment seen in the patient population dealt with by special care clinicians:
-
physical disability
-
medical disability
-
intellectual disability
-
mental illness
-
sensory disability
-
people who are anxious or phobic.
Such individuals have special needs and their dental needs are no exception. The following text discusses these groupings in more detail.
Physical disability
There is a wide range of conditions which ma/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


