16
Restoration of Endodontically Treated Teeth
Endodontically treated teeth are usually weak because of loss of tooth structure due to caries restorations, access cavity preparation, and necessary and unnecessary flaring of the root canal in the cervical area of the teeth. Also, loss of moisture in the dentin of these teeth allegedly results in a decreased resilience which has been associated with increased likelihood of fracture. Often so much of the coronal tooth structure is lost that it becomes necessary to use the root to obtain the required retention for a restoration, usually in the form of a root canal post. Thus, endodontically treated teeth may present with two main problems when a restoration is considered, i. e., a reduced strength of the remaining tooth structure and how to obtain the necessary retention for the restoration.
Strengthening of Endodontically Treated Teeth
Intracoronal Restorations
A root canal post is sometimes used with the purpose of strengthening a nonvital tooth. This is inappropriate. The preparation of a post space will significantly weaken a tooth, and no known method of restoration will strengthen the tooth sufficiently to match its previous resistance to fracture.
Thus, a post space should not be prepared in an endodontically treated tooth if this is not absolutely necessary and a root canal post should only be used when needed for retention of a coronal restoration.
The most effective method to strengthen endodontically treated teeth in most clinical situations is to use an acid-etch resin technique to create a bond between the resin in the access cavity and the dentin of the cavity walls. The root filling is removed to a level 1–2mm below the entrance to the root canal, and the access cavity is meticulously cleaned with small burs; if a eugenol-containing cement has been used the cavity is washed with alcohol. The alcohol is removed with a spray of water and air and the dentin is dried and etched with 37% phosphoric acid for 60 seconds. This removes the smear layer of the dentin as well as the highly mineralized peritubular dentin surrounding the dentinal tubules, leaving a clean dentin surface with wide open dentinal tubules (Fig. 16.1). The dentinal tubules are now used for retention of the resin restoration. The access cavity is dried and dehydrated to such a degree that the water in the dentinal tubules is removed. This can readily be done in a nonvital root filled tooth. A lightly filled resin is then applied to the cavity walls, and by means of careful use of compressed air and “condensation” with cotton pellets is forced to penetrate into the open dentinal tubules. This results in numerous (hundreds of thousands) resin tags inside the dentin (Fig. 16.2). When a filled resin then is used to complete the restoration, it not only fills the cavity, but will, because of the resin tags in the tubules of the cavity walls, “hold the tooth together” and increase its strength significantly (Fig. 16.3). Studies have shown that teeth that are restored in this way have almost the same resistance to fracture as intact teeth. If a metallic restoration is required, the orifice areas of the root canals and the pulp chamber are acid-etched and restored with resin as described above. The gold inlay or the amalgam filling is then placed in the tooth with the resin as the base (Fig. 16.4). This combined restoration has a strengthening effect the same as if the entire cavity were restored with the acid-etch resin technique. The type of composite resin used in these intracoronal restorations is of little consequence for the strength of the tooth since it is the lightly filled resin that penetrates the dentinal tubules or, for that matter, the enamel pits if portions of the enamel are included in the retentive area. The acid-etch resin technique may be used with advantage in all endodontically treated teeth where an intracoronal restoration is planned either to completely restore the tooth or to fill the pulp chamber and part of the cavity, leaving enough space for a final metallic restoration.
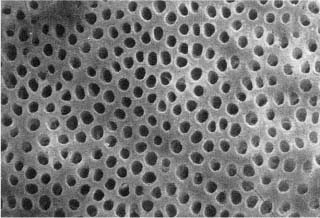
Fig. 16.1 Scanning electron micrograph of an acid-etched dentin surface. The lumina of the dentinal tubules may effectively be used for retention of resin restorations.
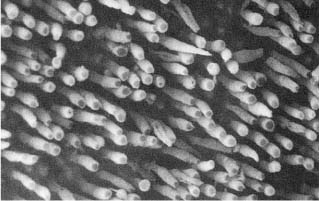
Fig. 16.2 Scanning electron micrograph of resin–dentin interface. The tooth has been dissolved with nitric acid and sodium hypochlorite, exposing the tags of resin that were inside the dentinal tubules. A restoration retained in this way will greatly strengthen the tooth and increase its resistance to fracture.
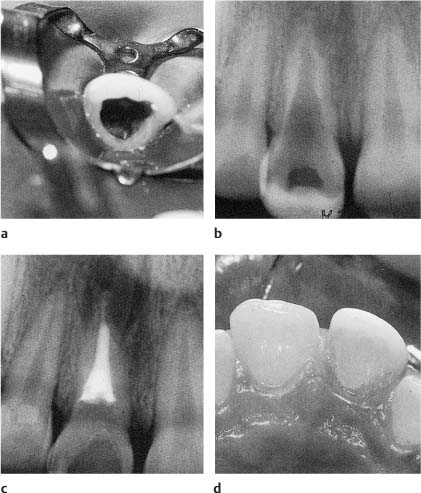
Fig. 16.3
a, b Clinical and radiographic view of a maxillary incisor severely weakened by caries of an endodontic ac/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses