Lumps and swellings in the jaws
INTRODUCTION
Jaw swelling is less commonly due to odontogenic causes (unerupted teeth, infections, cysts or neoplasms) (Box 16.1).
Jaw swelling may occasionally be caused by non-odontogenic inflammatory or neoplastic disorders, or metabolic or fibro-osseous diseases (Box 16.2).
Metastasis to the mouth is rare but is typically to the jaws, especially the posterior mandible.
CHERUBISM
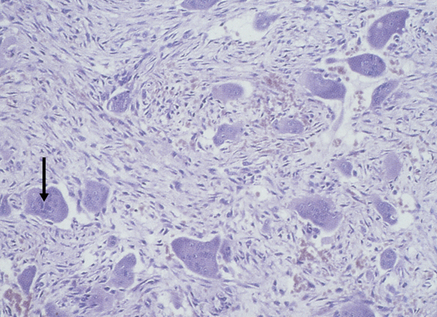
Cherubism is a rare genetically determined jaw disease, which closely resembles fibrous dysplasia except for the autosomal dominant inheritance (but variable expression) and association with chromosome 4p and mutated gene SH3BP2 which codes for a c-abl-binding protein. Painless symmetrical enlargement at the angles of the mandible and in the maxilla leads to the typical ‘cherubic’ facial appearance. Cherubism presents at 2–4 years of age, lesions growing progressively until puberty when they arrest or regress. Expansion of the alveolar bone results in irregular spacing and premature loss of teeth and possibly disturbances to a developing dentition. Imaging shows well-defined multilocular radiolucencies in the mandible, but maxillary lesions are less clearly defined. Blood chemistry is normal, although there may a raised alkaline phosphatase during active growth periods. Histologically, the lesions consist of loose vascular connective tissue with numerous multinucleated giant cells and, as in fibrous dysplasia, there is fibrous replacement of bone (Fig. 16.1). Other fibro-osseous lesions and giant cell lesions of bone (giant cell granuloma, hyperparathyroidism, giant cell tumours) should be excluded. Treatment of cherubism is as for fibrous dysplasia (see also Noonan syndrome, Ch. 56).
EXOSTOSES
Bony proliferations in other sites are considered to be usually either trauma-induced inflammatory periosteal reactions (exostoses), or true neoplasms (osteomas). Unless such a bony prominence is specifically located, is pedunculated or is associated with an osteoma-producing syndrome such as Gardner syndrome (Ch. 56), there is no way to differentiate exostosis from osteoma, even histopathologically.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses