16
Class III Malocclusion—The Evidence on Diagnosis and Treatment
Introduction
Class III, division 1 is characterized [in both lateral halves of the dental arches] by mesial occlusion [that] is slightly more than one half the width of a single cusp on each side, but in cases that have been allowed to develop—and these cases are always progressive—the mesial occlusion becomes greater, even to the full width of a molar, or more.
Edward Hartley Angle, 1907
Angle’s Classification
Angle’s description of Class III malocclusion (Figure 16.1), also known as mesioclusion, in its symmetrical (division 1) and asymmetric (subdivision) patterns focuses not only on the occlusion between the teeth but also on individual variation. Angle describes “considerable crowding, especially in the upper arch, and lingual inclination of the lower incisors and canines.” Although Angle’s classification has been used for over 100 years around the globe, his assumptions on etiology and diagnosis of the malocclusion lack definitive evidence. These assumptions include the relation of mandibular incisor retroclination to lower lip pressure “in the effort to close the mouth and disguise the deformity” and his only explanation for the etiology of Class III, the enlarged tonsils associated with the “habit of protruding the mandible” to afford “relief in breathing.”
Figure 16.1 Class III, subdivision 1, according to Angle.
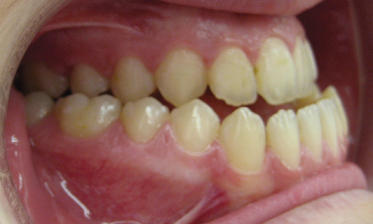
Angle assigns the “proportion” of Class III occurrence among 1000 malocclusions: Division—Bilaterally mesial (34/1000); subdivision—unilaterally mesial (8/1000). The incidence thus amounts to 4.2%, nearly similar to the reported incidence in American children in the 1970s (3%, Kelly, Sanchex & Van Kirk 1973) and 1990s (3.2%, Brunelle, Bhat & Lipton 1996; Proffit, Fields & Moray 1998; Proffit 2000). Higher incidences are reported among Asian populations.
General Characteristics
Angle’s observation on incisor retroclination preceded the age of cephalometrics, which demonstrated a corresponding proclination of maxillary incisors, reflecting dentoalveolar compensation by maxillary and mandibular incisors to an underlying skeletal discrepancy characterized by maxillary retrognathism, mandibular prognathism, or both.
Sometimes the incisal compensation is expressed with incisal edge-to-edge rather than crossbite, yet it is compatible with molar mesioclusion and an underlying Class III pattern. Variations and gradients of severity include the complex differentiation between macrognathism and prognathism in reference to the skeletal bases and between alveolar and skeletal bases. Therefore, the mosaic arrangement of the “parts” requires careful diagnosis, albeit the evidence of tailoring treatment modalities to specific diagnoses is not fully available. This shortcoming is related in great part to the availability of limited approaches to treatment and the inability of treatment to affect the cranial and facial skeletal parts compared to the relatively easier handling of dental components.
In a retrospective study of mesioclusion that comprised a group of Class II malocclusions, we investigated the underlying craniofacial morphology. Critical conclusions included (Figure 16.2) the following:
1. The prevalence of maxillary retrognathism is more than previously thought because its occurrence is more severe (SNA = 78.04 degrees ± 4.04 degrees; norm = 82 degrees ± 2 degrees) than mandibular prognathism (SNB = 81 degrees ± 2 degrees; norm = 80 degrees ± 2 degrees), the angles SNA and SNB yielding differences of 4 degrees and 1 degree from the respective norms.
Figure 16.2 Graphic representation of anterior crossbite, superior-posterior tip of the palatal plane (ANS-PNS) relative to horizontial (H), and high position of sella (S) relative to nasion (N) leading to reduced angle between SN and H. The morphological pattern may result from the transfer of forces generated by the anterior crossbite through the maxilla to the level of the cranial base. Findings on Class III craniofacial morphology also indicate: more reduction of SNA than SNB relative to their respective average values, and smaller saddle angle (N-S-Ar or N-S-Ba) in comparison with Class II morphology. Ar, articulare; Ba, basion.
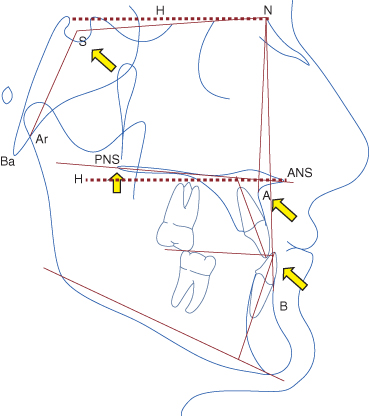
2. A more cephalad position of the anterior cranial base is underscored by a higher position of sella relative to nasion, concomitant with the previously described decrease in the saddle angle (nasion-sella-basion).
3. A previously unreported superior-posterior tip of the palatal plane.
4. Possibility of environmental induction of mesioclusion: an anterior crossbite, not necessarily related to genetic factors but sustained by mandibular forward positioning caused by occlusal interferences, habits, or to improve breathing, may induce forces that produce maxillary retrognathism that otherwise would not exist and affect the palatal tip through the occlusion (in a manner similar to the action of a headgear; Figure 16.3).
Figure 16.3 Treatment with straight-pull headgear inserted in tubes attached to maxillary first molars resulted in downward (clockwise) rotation of the palatal plane around a center (red circle) nearly 4 cm (on average) posterior to PNS. Rotation in the same direction would occur from the sustained effect of an anterior crossbite but probably with a center of rotation more anteriorly located.
(Vertical changes in mandible are not represented. Data from Efstratiadis et al. 2005.)
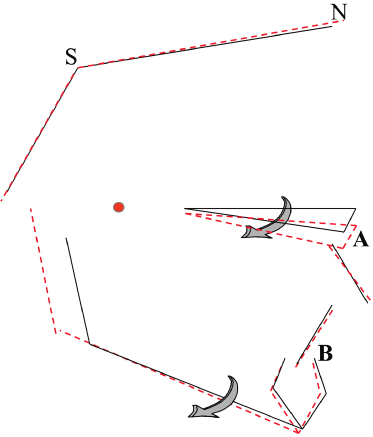
5. The thickness of the soft tissue envelope, which may differ from one region to another, can compensate or exacerbate the regional diagnosis.
Three-dimensional imaging of the craniofacial system has not yet generated new knowledge of Class III morphology to enable more accurate diagnosis, the aim of which is to formulate a corresponding individualized treatment approach.
Pseudo Class III
Pseudo Class III is also called functional crossbite, mandibular displacement, or positional malrelationship (Moyers 1988) because the mandible shifts forward after initial interference, often on canines or more posterior teeth. Compared with Class I malocclusion, pseudo Class III is characterized by retroclined maxillary incisors, retrusive upper lip, decreased midface length, and increased maxillary-mandibular difference (Rabie & Gu 2000; Ngan 2006). Because of closer to normal skeletal features, maxillary and mandibular incisors do not show the typical compensatory inclinations, facilitating resolution of the malocclusion by orthodontic means. In “true” Class III, functional forward shift may coexist with the underlying skeletal discrepancy.
Diagnostic Considerations
Available evidence on the development of Class III suggests the assessment of references used for more accurate cephalometic diagnosis. Maxillary and mandibular positions are commonly gauged by the angles SNA and SNB. The position of sella can induce misinterpretation of data if not corrected to the natural head position “true” horizontal. A high sella relative to nasion would yield smaller SNA and SNB values when corrected, thus less maxillary and mandibular prognathism; a low position of sella would have opposite consequences (Figure 16.4). Regarding SNB specifically, the deeper the overbite or the more anterior functional positioning of the mandible, the greater the SNB angle, thus the inference of more mandibular prognathism. Accurate appreciation of SNB would require “bite opening” or “rotating” the image of the mandible on the tracing to near normal overbite (20%–30%). Such exercise is further rationalized with anterior (functional) mandibular displacement, particularly in the diagnosis of pseudo Class III. These issues are not accounted for in research on Class III malocclusion.
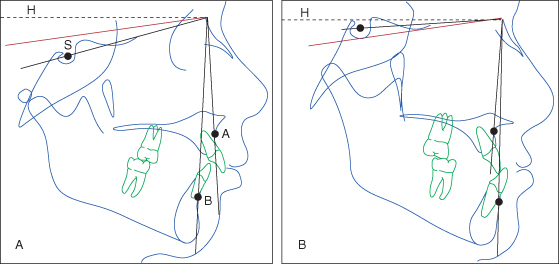
Figure 16.4 Variation in the position of sella (S) relative to nasion (N) results in an upward (cephalad) or downward (caudad) inclination of the SN reference line and consequently an overestimate and underestimate of the jaws’ anteroposterior positions (SNA and SNB).
(A) Lateral cephalometric tracing of a boy 10 years, 5 months old with a Class II, division 1, malocclusion. The inclination of the SN line to the horizontal affects the values of SNA and SNB and the interpretation of sagittal jaw relationship. While the difference in ANB = 8 degrees (norm: 2–3 degrees), SNA = 80 degrees (norm: 82 degrees) and SNB = 72 degrees (norm: 79–80 degrees), suggesting that the sagittal discrepancy is caused by a retrognathic mandible. However, the cant of SN to the horizontal recorded from the natural head position is 15 degrees instead of the norm of 8 degrees (7–9 degrees). When the difference of 7 degrees (15 degrees minus 8 degrees) is added to the values of SNA and SNB to correct for the SN inclination, the angular measurements become SNA = 80 degrees + 7 degrees = 87 degrees; SNB = 72 degrees + 7 degrees = 79 degrees, yielding the correct diagnosis of maxillary prognathism and “normal” mandibular position.
(B) Lateral cephalometric tracing of a boy 14 years, 10 months old with Class III malocclusion with ANB difference of −3 degrees, seemingly relating a normally positioned maxilla (SNA = 82 degrees) and a prognathic mandible (SNB = 85 degrees). Yet, correction of the SN cant to horizontal from an acute 4 degrees to the average of 8 degrees decreases the SNA angle to 78 degrees (82 degrees − 4 degrees), and the SNB angle to 81 degrees (85 degrees − 4 degrees), adjusting the diagnosis to maxillary retrognathism
(Ghafari 2006, Ghafari et al. 2007a).
Etiology of Class III Malocclusion
Class III is often associated with the image of mandibular prognathism (Figure 16.5). The role of genetics and environment in establishing the size and position of the craniofacial components is complex and not yet fully unraveled.
Figure 16.5 Mandibular prognathism is best illustrated in the inherited prognathism within the Habsburg dynasty. Charles II of Spain, the “pathetic victim” of Habsburg inbreeding.

Environmental factors are increasingly recognized as potential determinants of at least individual malocclusions. King, Harris & Tolley (1993) reported the potential environmental influence on and lower genetic components of craniofacial size and form, a finding that would suggest the possibility of minimizing or avoiding the full expression of Class III, despite its ranking as the first most likely deformity to run in families (Proffit 2007). Our research findings and enunciation of the concept of developmental or “intragrowth” orthopedics support the effect of the environment (sustained early anterior crossbite) potentially affecting the position of the maxilla (Figure 16.6; Ghafari 2004). Development and/or severity of the maxillary retrognathism may be generated by functional forces initiated by mandibular anterior position and transferred through the occlusion, particularly in instances of deep overbite maintained during a long period of growth (Ghafari & Haddad 2005).
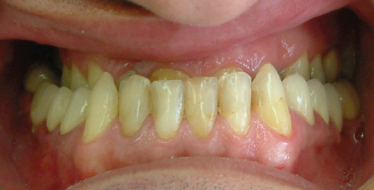
Figure 16.6 Class III malocclusion with maxilla fully embedded within prognathic mandible (see other views in Figure 16.12).
Nasal obstruction also induces a forward position of the mandible that helps clear the airway and reduce mouth breathing (Macari & Ghafari 2006). This theory was Angle’s only explanation for the etiology of Class III, beginning before or around the time of eruption of the first permanent molars and “always associated at this age with enlarged tonsils.” Angle further stated his “conviction” that other etiologic factors are of minor importance and that early treatment of the “throat” and correction of the molar occlusion and its retention for a few months would eliminate the problem. Angle also assigned Class II development at least partially to mouth breathing (1907). Angle’s hypotheses are not supported by definitive evidence, yet the suggested mechanism should be valid for at least a proportion of patients.
Based on our research findings, we postulate that a Class III malocclusion underlined with mandibular prognathism is mainly genetic in nature, whereas a mesioclusion associated with maxillary retrognathism is the result of environmental induction (which may include the restraining effect of an inherited macro and/or prognathic mandible as a primary or secondary factor of inhibiting maxillary forward growth). This premise implies the proper selection of a “true” Class III in researching the genetics of Class III. Such studies should not include maxillary retrognathism, at least not without the presence of a prognathic mandible with increased mandibular size by one standard deviation or more.
Foundations and Variations of Treatment
“[Class III malocclusions are] by far the worst type of deformities the orthodontist is called upon to treat, and when they have progressed until the age of sixteen or eighteen, or after the jaws have become developed in accordance with the malpositions of the teeth, the case has usually passed beyond the boundaries of malocclusion only, and into the realm of bone deformities, for which, with our present knowledge, there is little possibility of affording relief through orthodontic operations.”
Edward Hartley Angle, 1907
How different is the state of the art of treatment of Class III malocclusions over a century after this writing by the definer of the deformity? As the statement implies, treatment is considered differently in growing and adult patients.
Early Treatment
Treatment Approach
With increasing emphasis on repositioning the maxilla rather than the mandible in orthognatic surgery (Proffit, Turvey & Phillips 1996), the focus on maxillary orthopedics in the early treatment of the malocclusion is not surprising. Chin cups to restrain mandibular growth have largely been replaced by face masks (reverse headgears) to protract the maxilla, often with rapid palatal expansion. The rationale for expansion is to minimize the resistance of bony buttresses around the maxilla, splint the maxillary teeth, and correct a posterior crossbite when present. In the primary dentition, fixed palatal expanders or other appliances, such as the Porter arch and quad helix, may be used to achieve expansion. When no expansion is needed, passive appliances (e.g., Nance holding arch) are used.
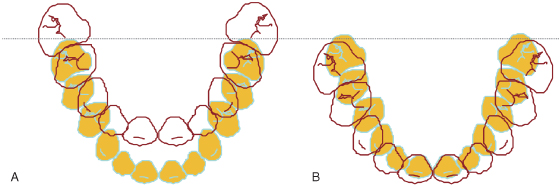
An important clinical observation is warranted: unless a posterior crossbite exists, palatal expansion is not needed for transverse occlusal correction. An anticipated forward positioning of the maxillary dentition relative to the mandibular teeth produces an increased maxillary width (Figure 16.7). Therefore, many practitioners use the face mask without palatal expansion. However, long-term studies are based on the combined use of these appliances and on treatment in the mixed dentition. Most treatment regimens in the primary dentition are based on expert opinion or case reports or series.
Figure 16.7 (A) Maxillary arch (white) in normal transverse relation with mandibular arch (orange) in Class III malocclusion. (B) When arches are approximated into normal Class I relationship, maxillary width increases relative to mandibular breadth at the level of molars and premolars. The opposite is true in Class II malocclusions.
Existing Evidence
Because of the need for long-term evaluation of early treatment and a lower incidence of Class III malocclusion within Caucasian populations, long-term studies of Class III treatment are limited. Research including the highest level of evidence indicates the following conclusions:
Treatment Timing: Treat Early for More Effect
The available evidence emphasizes the efficiency of early treatment, however, more because of its potential effect relative to late treatment. Based on bone age assessment, Suda et al. (2000) determined “more pronounced” treatment effects in younger children. In a meta-analysis, Kim et al. (1999) concluded that protraction face mask therapy is effective in growing patients but to a lesser degree in those older than age 10 years.
Accordingly, treatment in the primary dentition should be more efficient, and some supporting authors have hypothesized potential effect on the cant of the cranial base or saddle angle (Delaire 1980; Deshayes 2006) that would enhance more posterior positioning of the glenoid fossa and thus less prognathic mandible. Advocating optimal treatment timing for face mask therapy in the deciduous or early mixed dentition, Ngan (2006) cites the benefits to include favorable sutural response, elimination of any functional discrepancy between centric occlusion and centric relation, and improvement in facial profile and self-esteem.
Another reason for early treatment that requires focused research is its potential to reduce the worsening of the developing dentofacial dysmorphology. Given the increased severity in maxillary retrognathism if sustained by a forward mandibular position, the sooner the anterior crossbite is eliminated, the closer to normal development would be the dentofacial complex, especially maxillary development. Consequently, future treatment may be reduced to only orthodontic treatment (tooth alignment or compensation of dental inclination over bone) or limited orthognatic surgery (only mandibular surgery or if both jaws are involved, one instead of multiple-piece maxillary surgery).
Treatment Modality: Palatal Expansion May Not Be Required and Chin Cup Success Is Questionable
Palatal expansion is often indicated, particularly in the presence of maxillary constriction and crowding. In a meta-analysis, Kim et al. (1999) reported similar protraction with or without expansion, though the average treatment duration was longer without expansion. While protraction combined with an initial period of expansion was thought to provide more significant skeletal effects (Kim et al. 1999), such as greater forward movement of point A (Baik 1995), the need for expansion absent a transverse discrepancy (skeletal/dental crossbite) was not supported by the results of a prospective randomized clinical trial (Vaughn et al. 2005). The authors evaluated face mask treatment with and without palatal expansion in children at mean initial ages of 7.4 and 8.1 years, respectively, compared with an observation group (6.6 years). The treatment modalities produced equivalent dentofacial changes. Other authors concurred (Tortop, Keykubat & Yuksel 2007). Varied modalities have been advanced that comprise bonded splints with bite blocks for expansion or the addition of adjunct appliances, further demonstrating the variability of approaches to the same strategy. No evidence is available on more or less effectiveness over the basic strategy.
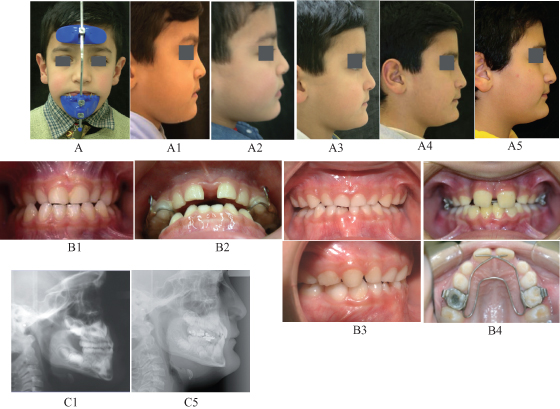
Our observations regarding palatal expansion and face mask in the primary dentition, with overcorrection and removable retention, include the possibility of emergence of the permanent incisors in retroclination, although skeletal changes seem more stable (Figure 16.8). Research is needed on this particular regimen. Thus, the use of a Porter arch or quad helix appliance might be sufficient to correct the anterior crossbite in the primary dentition, with a possible combination of palatal expansion with face mask in the mixed dentition.
Figure 16.8 Treatment of Class III malocclusion (ANB = 1.5 degrees; incisors edge to edge) in 5-year-old boy with primary dentition, using a combination of palatal expander and face mask (A). Photographs of profile (A1–A5), occlusion (B1–B4), and cephalographs (C1, C5) illustrate changes at different times: 1, initial; 2, 17 days after initiation of treatment; 3, 14 months; 4, 3 years, and 5, 6 years. Note the following details: (B2) diastema is the result of palatal expansion with bonded appliance over primary canines and molars; overjet is overcorrected. (B3) Following interrupted retention of phase 1 results, retroclination of primary incisors, though not in crossbite at time T3; (B4) permanent incisors developed in upright and retroclined position are proclined with Porter arch to develop positive overjet at time T4.
A chin cup was initially thought to reduce the growth of a prognathic mandible. Although animal studies indicated the possibility of altering condylar growth (Petrovic, Stutzmann & Oudet 1975; Copray, Jansen & Duterloo 1985; Vardimon et al. 1994), clinical research reveals initial changes within the skeleton that were rarely maintained during pubertal growth (Sugawara & Mitani 1993). The face mask includes a chin cup component (Figure 16.8). The separate effect of the chin cup versus maxillary protraction is not known and would be difficult to determine. The chin cup may have an additive influence, maximizing the effect of the protraction, and/or mandibular rotation.
Mandibular headgear was used in Class III treatment, followed by fixed appliances with long-term improvement that contrasted with lack of self-improvement in corresponding controls (Baccetti et al. 2009). The results show compensatory changes that might be achieved with fixed appliances that would distalize the mandibular teeth. More research is required to explore such approaches.
Treatment Is Better Than No Treatment
Pangrazio-Kulbersh et al. (2007) reported that continued anterior growth after protraction is removed was greater than in control subjects. In a cohort study, they compared protraction treatment with surgical correction 7 years posttreatment, along with a corresponding control group. The authors found a “striking” general similarity between the protraction and surgical groups, suggesting that appropriate orthodontic treatment may avoid surgery.
Overtreatment Is Better for Stability of Results
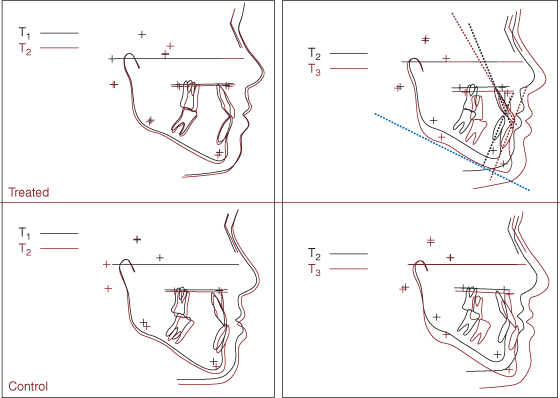
“Aggressive overcorrection of Class III appears advisable.” Westwood et al. (2003) made this conclusion from a cohort study of the long-term effects of Class III treatment with rapid maxillary expansion and face-mask therapy followed by a second phase of treatment with preadjusted edgewise fixed appliances (average of 27 months). Between both treatment phases, patients wore a removable maxillary “stabilization plate.” In a few instances, phase 2 followed phase 1 immediately. The authors evaluated the stability of maxillary protraction in 34 patients at pretreatment (average age: 8 years, 3 months) and posttreatment (14 years, 10 months) compared with matched untreated controls. The treated patients had a more favorable skeletal change than control subjects in whom the mesioclusion was maintained (Figure 16.9). However, a close evaluation of the published illustrations reveals compensatory proclination of maxillary incisors and maintenance of retroclination of mandibular incisors, supported by the reported use of Class III elastics with fixed appliances.
Figure 16.9 Top row: Changes from superimposed cephalographs of treated patients between baseline (T1) and end of phase 1 (T2) (10 months), and between T2 and posttreatment (T3) (5 years, 7 months). Bottom row: Superimposition of cephalographs of matched control subjects at corresponding observation periods, T1–T2 (14 months) and T2–T3 (6 years).
Adapted from Westwood et al. (2003).
More research is needed that accounts for the various variables of a complex, multifactorial issue, namely age, nature of correction (skeletal vs. dentoalveolar), residual maxillary growth, and mandibular growth. The Cochrane database systematic review remains at the level of a protocol (Harrison et al. 2002).
The Difficulty of Forecasting Growth and the Dilemma of Overcorrection
The major problem with early treatment of mesioclusion with underlying skeletal discrepancy is the inability to precisely forecast its development. The orthodontist tries to anticipate the growth spurt to minimize its effect (e.g., favoring maxillary growth or mandibular rotation to counteract additional mandibular growth). Unlike Class II malocclusions, in which mandibular growth helps treatment, further mandibular growth in Class III is not balanced by concomitant maxillary growth. The maxilla grows at a slower rate than the mandible and ceases forward growth nearly 2 years before the mandible (Cortella, Shofer & Ghafari 1997).
The combination of maxillary expansion and face mask is advocated with overcorrection, i.e., increase of overjet, which results from both the maxillary protraction (with a side effect of counterclockwise rotation) and mandibular clockwise rotation (Figure 16.10). Given the inaccuracy of growth forecasting, the amount of overjet overcorrection cannot be determined precisely, leading to one of these possibilities:
1. Mandiblular forward growth equals the amount of overcorrection; then, the present compensatory incisor angulations are maintained; or
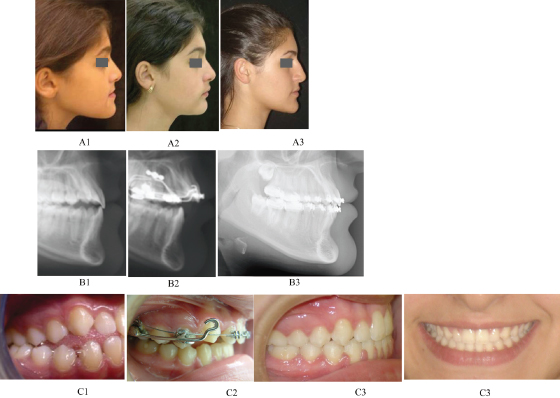
Figure 16.10 Profile photographs (A1–A3), lateral cephalographs (B1–B3), and occlusal views (C1–C3) of female 10 years, 9 months old, who was treated with maxillary expansion and protraction face mask in phase 1 to an overcorrected overjet. The records were taken at pretreatment (A1, B1, C1), 6 months (A2, B2, C2), and 6 years (A3, B3, C3) from treatment start. After an extended period of retention that lasted beyond the adolescent growth spurt, fixed appliances were used to achieve the well-interdigitated neutroclusion (C3). The overcorrection was performed to anticipate either mandibular growth equal to the amount of overcorrection, in which instance pretreatment mandibular incisor angulations would have been maintained, or mandibular growth less than the amount of overcorrection, in which instance the mandibular incisors would be proclined for the remainder of overjet correction. The actual outcome was a “middle” situation: the mandibular incisors ended up more proclined than pretreatment, and the facial profile more orthognathic than the original concave outline. Although the treatment avoided orthognathic surgery, it lasted a long time because appliances were kept beyond a late-occurring adolescent growth spurt. Note improvement (reversal of steps) in relation between upper and lower lips.
2. The mandible grows less than the amount of overcorrection; thus the mandibular incisors are proclined for the residual overjet correction.
In addition, the results must be retained and reevaluated throughout the period of growth, leading to longer treatment, particularly if started in the primary dentition and revisited in the mixed and later the permanent dentitions.
Class III malocclusions with prognathic, particularly macrognathic mandibles often require a surgical correction that is delayed until after or toward the end of mandibular growth (skeletal ages of 16–18 years in females, 18–20 years in males). Yet, early treatment may reduce the severity of the malocclusion by minimizing associated problems such as crowding of the maxillary arch. Left uncorrected, this problem may require later tooth extractions (usually premolars) that contract the maxillary arch, possibly necessitating maxillary surgical widening.
In many instances, parents pressure the orthodontist to start early correction of a noticeable mesioclusion. Early treatment becomes questionable when the patient ends up undergoing surgery at an older age. All the diagnostic and therapeutic components must be weighed carefully in the individual patient. Research should determine valid long-term options.
Adult Treatment
Orthodontic Options
Randomized studies are not available for nonsurgical (camouflage) treatment of mesioclusion with skeletal discrepancy in nongrowing or adult patients. However, case reports indicate that surgery may be avoided with a combination of mandibular rotation and compensatory inclination of teeth over basal bones. To this basic rationale may be added the extraction of premolars for further incisor retroclination or the distal movement of mandibular molars, possibly requiring the extraction of third molars, followed by the retraction of the more anterior teeth (Figure 16.11). This approach contributes to the correction of posterior transverse maxillary-mandibular relations.
Figure 16.11 (A) P/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


