CHAPTER 14. Tongue disorders
Patients are also aware that doctors traditionally look at the tongue. As a result, they look at their own and as a consequence sometimes worry about insignificant changes or think normal features, such as the foliate papilla, are a cause for concern.
THE SORE TONGUE
There are several clinical types of sore tongue (Box 14.1).
Box 14.1
Clinical types of sore tongue
• Ulcers (of any type) involving the tongue
• Glossitis (red and sore tongue)
• The sore, physically normal tongue
• Geographical tongue (erythema migrans)
Ulceration of the tongue
The tongue may be involved in, or even the predominantly affected site of, various types of stomatitis such as herpes simplex or, more frequently, lichen planus (see Figs 13.10 and 13.11). The tongue may also be the site of solitary ulcers, particularly carcinoma which, when far back, may be difficult to see. The lateral borders are affected and carcinoma of the dorsum of the tongue is exceptionally rare.
When there are definable lesions of these kinds, diagnosis is usually straightforward and depends on clinical examination and sometimes biopsy.
Glossitis
Glossitis is the term used for the red, smooth and sore tongue particularly characteristic of anaemia. These features are a combination of signs (redness and smoothness) and a symptom (soreness) which are not always associated. Tongues can be sore in the absence of visible changes or smooth but asymptomatic from a variety of causes (Box 14.2).
Box 14.2
Important causes of glossitis
• Anaemia
• Vitamin B group (especially B 12) deficiencies
• Candidosis
Iron deficiency and pernicious anaemia are the main causes (Fig. 14.1). Women are more frequently affected. Detailed haematological examination is essential. These investigations are important, as a fall in haemoglobin level may lag behind other changes. Thus, there may be glossitis, haematological signs of a deficiency state, but a haemoglobin level within normal limits. Abnormalities of the red cells may be seen in a stained film, but the red cell MCV (mean corpuscular volume) is frequently a useful guide. Serum levels of iron and ferritin, B 12 or folate (as the case may be) are depressed. When abnormalities such as these are found, specific treatment quickly relieves the symptoms.
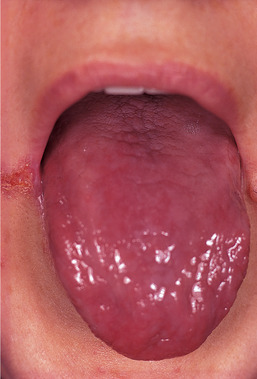 |
| Fig. 14.1
Glossitis in iron-deficiency anaemia. The tongue is smooth, due to atrophy of the papillae, and is red and sore. Anaemia is the commonest diagnosable cause of glossitis and must always be looked for by haematological examination.
|
Glossitis with angular stomatitis is characteristic of riboflavin deficiency and sometimes of nicotinic acid deficiency, but these are rare. The diagnosis of vitamin deficiency should not be made on oral signs alone in an otherwise healthy patient. These B group vitamins are frequently given in an attempt to relieve sore tongue but are virtually invariably ineffective. Their ineffectiveness makes it clear that deficiency of these vitamins is not the cause.
Candidosis can cause the tongue to be red, sore and oedematous. This is typical of acute antibiotic stomatitis (Fig. 14.2) and often then associated with angular stomatitis and other features of candidosis. This condition is rarely seen now that antibiotics are used less indiscriminately than in the past and topical oral antibiotics have now been discredited for oral infections. In Sjögren’s syndrome, the tongue becomes red and acquires a cobblestone texture (see Fig. 18.12).
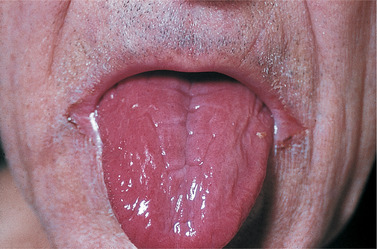 |
| Fig. 14.2
Glossitis in antibiotic stomatitis. The tongue is red, smooth and sore as in anaemic glossitis, but the appearance is partly due to inflammatory oedema. Similar changes affect the rest of the mucosa and other features of candidosis, such as thrush, are often present.
|
Lichen planus can produce a smooth tongue due to atrophy of the papillae (particularly late in longstanding disease), but there is then no soreness and typically no erythema. There is often a bluish-white sheen to the surface of the tongue and other signs of lichen planus may be seen in other parts of the mouth (Fig. 14.3).
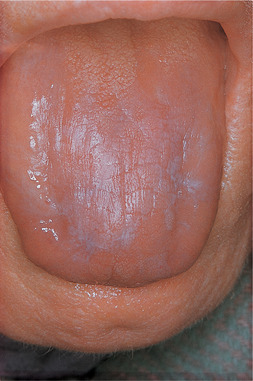 |
| Fig. 14.3
Smooth tongue due to lichen planus. This is a late change due to longstanding disease. The tongue is smooth due to atrophy of the papillae, but has a faint silvery sheen. There are usually no symptoms at this stage.
|
The sore, physically normal tongue
This type creates the most difficult problems. The symptoms are frequently psychogenic, but it is essential to exclude organic disease, particularly a haematological deficiency.
Haematological deficiencies. Soreness can precede visible, physical changes (Fig. 14.4). The haemoglobin is frequently within normal limits, but there are other abnormalities as described earlier. Treatment of the deficiency quickly relieves the symptoms.
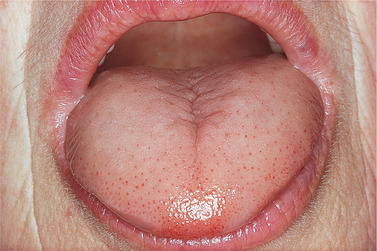 |
| Fig. 14.4
A normal-looking but persistently sore tongue in a doctor’s wife who had had repeated but inadequate haematological investigations which failed to detect early pernicious anaemia.
|
Psychogenic disorders. Soreness of the tongue frequently appears to be psychogenic and is sometimes termed ‘burning mouth syndrome’. Some regard it as a variant of atypical facial pain and it is discussed in Chapter 34.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


