CHAPTER 29. Gastrointestinal and liver disease
GASTRO-OESOPHAGEAL REFLUX AND GASTRIC REGURGITATION
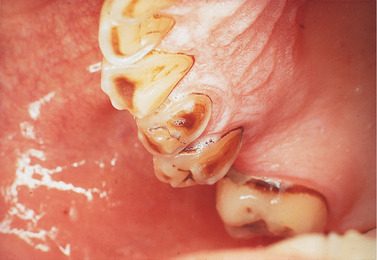
Gastro-oesophageal reflux (‘heart burn’) is a common type of dyspepsia. Smoking, excessive alcohol consumption, obesity, frequent stooping and over-large meals are frequent precipitating factors. If allowed to persist, damage to the oesophageal lining can result, but protein pump inhibitors, such as omeprazole, are highly effective in controlling it. Since there is no significant regurgitation of gastric acid there are no adverse dental effects. By contrast, chronic vomiting of gastric acid contents, due to such causes as hypertrophic pyloric stenosis, can lead to erosion of the palatal aspect of the anterior teeth particularly (Fig. 29.1). This type of dental erosion is an important diagnostic sign of self-induced vomiting in bulimia.
 |
| Fig. 29.1
Erosion of the palatal surfaces of the upper teeth due to repeated vomiting.
|
COELIAC DISEASE
Coeliac disease is one of the most common genetic disorders and is an important cause of malabsorption. It is due to a form of hypersensitivity to gluten in flour. The disease is frequently asymptomatic and it may not be recognised until adult life as a result of its complications. It can also have a great variety of effects. In addition to malabsorption, stunting of growth, fatty diarrhoea and abdominal pain or discomfort are typical consequences. The malabsorption can lead to vitamin and mineral deficiencies resulting in anaemia or bleeding tendencies, as discussed below.
Dental aspects
Anaemia can have a variety of oral effects such as glossitis or recurrent aphthae as discussed in Chapter 22. Up to 5% of patients with coeliac disease may have recurrent aphthae, even in the absence of anaemia.
CROHN’S DISEASE → Summaries pp. 324, 409
Crohn’s disease and ulcerative colitis are types of inflammatory bowel disease which may have common symptoms but which are otherwise distinct entities. Crohn’s disease is of unknown aetiology. It most frequently affects the ileocaecal region, causing thickening and ulceration. Symptoms vary with the severity of the disease, but effects can include abdominal pain, variable constipation or diarrhoea and, sometimes, obstruction and malabsorption. Repeated bowel resections may ultimately be needed. Joint pain can also be troublesome.
Dental aspects
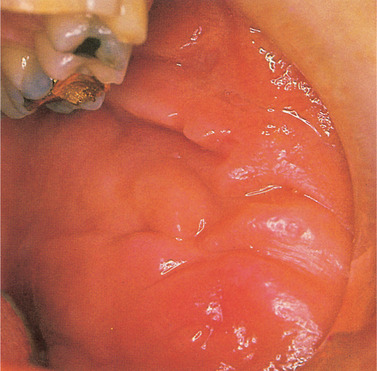
Cobblestone mucosal swelling and ulceration (Fig. 29.2, Fig. 29.3 and Fig. 29.4), particularly when associated with abdominal symptoms, can lead to the diagnosis of Crohn’s disease (Box 29.1). Occasionally, oral lesions precede gastrointestinal symptoms by a long period.
 |
| Fig. 29.2
Crohn’s disease. Soft nodular hyperplasia of the oral mucosa is a typical feature and, in this case, was associated with facial swelling and intermittent diarrhoea.
|
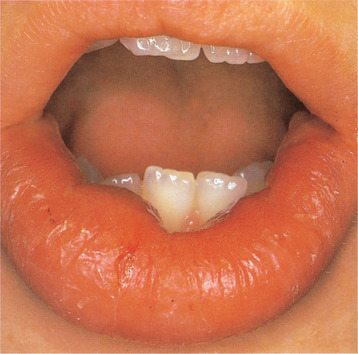 |
| Fig. 29.3
Crohn’s disease. Gross labial swelling and intraoral mucosal proliferation with typical histological changes led to the finding of extensive intestinal involvement.
|
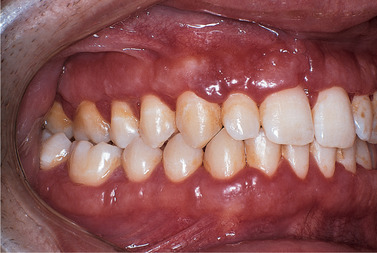 |
| Fig. 29.4
Crohn’s disease. The gingivae are hyperplastic and irregular and erythematous. These changes are obvious, but more subtle signs are easily missed. The appearances are identical to those in sarcoidosis in the gingivae.
|
Box 29.1
Typical orofacial features of Crohn’s disease
• Diffuse soft or tense swelling of the lips, or mucosal thickening
• Cobblestone thickening of the buccal mucosa, with fissuring and hyperplastic folds
• Gingivae may be erythematous and swollen
• Sometimes, painful mucosal ulcers, linear or resembling aphthae
• Mucosal tags in sulcuses sometimes present
• Glossitis due to iron, folate or vitamin B 12 deficiency can result from malabsorption
Histologically, there is formation of non-caseating granulomas resembling those in the intestine. The granulomas are typically small, loose and with few multinucleate giant cells. They are often deep in the corium and may be difficult to find. A biopsy may need to extend unusually deeply (Fig. 29.5, Fig. 29.6 and Fig. 29.7). In the absence of symptoms, sigmoidoscopy and colonoscopy will show the degree of bowel involvement. However, in the absence of symptoms, many gastroenterologists prefer to leave patients in peace until they should develop because of the lack of entirely satisfactory treatment even when symptoms develop. Under such circumstances, mucosal Crohn-type granulomas may be mistaken, for a time at least, for orofacial granulomatosis (see below).
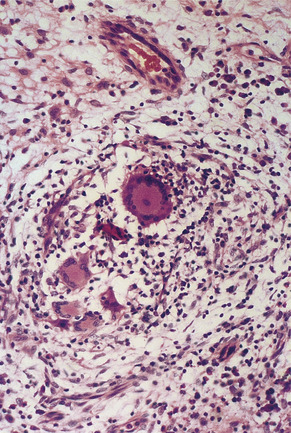 |
| Fig. 29.5
Crohn’s disease. The granulomas are frequently isolated and loose in texture with scanty peripheral lymphocytic infiltrate, as here.
|
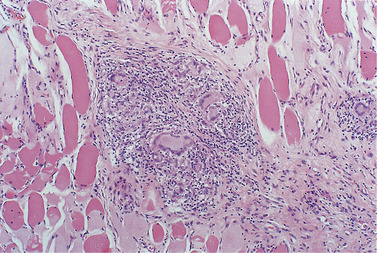 |
| Fig. 29.6
Crohn’s disease. The granulomas are frequently deep in the mucosa and widely dispersed. Here granulomas are present in muscle, showing the importance of adequate biopsy depth.
|
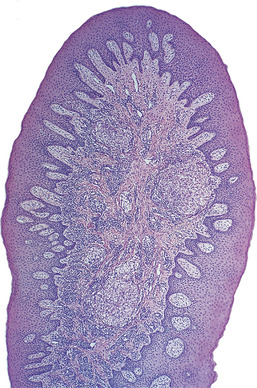 |
| Fig. 29.7
Crohn’s disease. A hyperplastic tag of gingiva contains several large round granulomas.
|
Management
Oral symptoms may resolve when intestinal Crohn’s disease is controlled with, for example corticosteroids, sulfasalazine or mesalazine. Alternatively, oral lesions may respond to oral sulfasalazine or to intralesional injections of a corticosteroid.
OROFACIAL GRANULOMATOSIS → Summaries pp. 324, 409
The term orofacial granulomatosis applies to swellings of such sites as the gingivae or lips (Fig. 29.8) due to granulomatous inflammation (Fig. 29.9), but not caused by any of the recognised diseases. Some of these patients develop Crohn’s disease or sarcoidosis later, but many others remain otherwise healthy or have subclinical bowel disease.
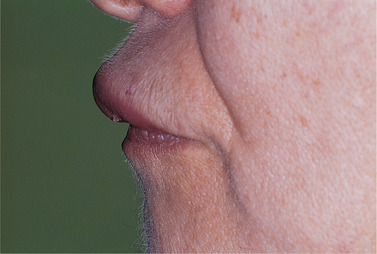 |
| Fig. 29.8
Orofacial granulomatosis. There is conspicuous swelling of the upper lip with eversion of the vermilion border. The lip is thickened and tense.
|
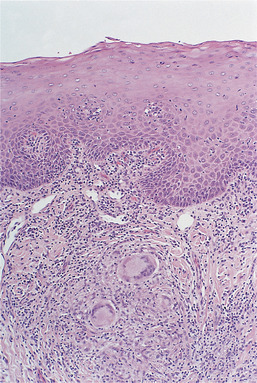 |
| Fig. 29.9
Orofacial granulomatosis. Below the epithelium is a patchy inflammatory infiltrate and scattered granulomas containing large multinucleate giant cells.
|
In some, the granulomatous reaction appears to result from common food additives such as cinnamon or tartrazine. Such causes can only be confirmed by an exclusion diet which, if faithfully maintained, may greatly lessen the swellings. Otherwise, intralesional corticosteroids may help.
When no cause can be found, regular follow-up should be maintained to ensure that any underlying condition, such as Crohn’s disease or sarcoidosis, is recognised at an early stage.
The term ‘orofacial granulomatosis’ should not incidentally be confused with midfacial granulomas which are lethal diseases (Ch. 28).
MALABSORPTION SYNDROMES
Malabsorption syndromes (Box 29.2) can cause haematological deficiencies which can contribute to development or exacerbation of recurrent aphthae, glossitis or other symptoms.
Box 29.2
Important causes of malabsorption syndrome
• Coeliac disease
• Crohn’s disease
• Resection of stomach or ileum
• Pancreatic insufficiency
• Liver disease (failure of bile secretion into the gut)
• Some parasitic and other chronic gut infections
ULCERATIVE COLITIS
Ulcerative colitis is a disease of the large intestine causing inflammation and ulceration. Patients are typically between 15 and 50 years. The main effect of the bowel lesions is intractable diarrhoea with blood, mucus and pus in the stools. Abdominal pain, fever, anorexia and weight loss are seen in severe cases. Development of psychiatric symptoms is a not surprising feature of this distressing and disabling disease.
Serious complications are dilatation and perforation of the bowel (toxic megacolon) and, in longstanding cases, carcinoma of the bowel. Resection of the bowel will eliminate this risk and is curative.
Dental aspects
Anaemia can have its usual effects on the oral mucosa. Rarely, chronic ulceration (pyostomatitis gangrenosum) or multiple intraepithelial microabscesses (pyostomatitis vegetans) develop. As a result of such ulceration and complications such as skin lesions and arthralgia, there may be confusion with Behçet’s disease.
FAMILIAL POLYPOSIS COLI
Polyposis of the of colon is a feature of Gardner’s syndrome comprising multiple osteomas of the jaws, polyposis coli with a high malignant potential and, often, other abnormalities such as dental defects and epidermal cysts. It is inherited as an autosomal dominant trait.
The osteomas of the jaws are typically multiple and may be ranged along the alveolar ridge, along the borders of the mandible or form endosteal radiopacities. However, the importance of this syndrome is that most of those affected die of bowel cancer by the age of 50. Though some members of the family do not have polyposis coli, the finding of multiple osteomas of the jaws should prompt examination for bowel disease.
PEUTZ–JEGHERS SYNDROME
In this disorder, pigmented macules, particularly oral, are markers for intestinal polyposis (see Fig. 21.5). Polyps may develop throughout the gastrointestinal tract and, in the small bowel, can cause recurrent abdominal pain and minor intestinal obstruction. Follow-up of the original family for 38 years and other cases has shown that cancer of the colon is an important complication, but the risk for breast and gynaecological cancers is also high.
PSEUDOMEMBRANOUS COLITIS
Diarrhoea with passage of blood and mucus in the stools and sometimes fragments of necrotic bowel mucosa (pseudomembrane) is typically a complication of usually prolonged antibiotic therapy particularly with clindamycin or lincomycin. It is due to proliferation of Clostridium difficile resistant to these antibiotics. Pseudomembranous colitis particularly affects the elderly and debilitated, some of whom have died as a result. Treatment with metronidazole or oral vancomycin is usually effective.
It does not appear that this disease can follow a single dose of clindamycin given for the prevention of infective endocarditis.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


