INTRODUCTION
PULPAL IRRITANTS
EFFECT OF DENTAL CARIES ON PULP
EFFECT OF TOOTH PREPARATION ON PULP
• Pressure
• Heat Production
• Vibrations
• Remaining Dentin Thiclaless
• Speed of Rotation
• Nature of Cutting Instrument
EFFECT OF CHEMICAL IRRITANTS ON PULP
• Factors Influencing the Effect of Restorative Materials on Pulp
PULP PROTECTION PROCEDURES
• Pulp Protection in Shallow and Moderate Carious Lesions
• Pulp Protection in Deep Carious Lesions
MATERIALS USED FOR PULP PROTECTION
• Varnish
• Adhesive Sealer
• Liners
• Bases
METHODS OF PULP PROTECTION UNDER DIFFERENT RESTORATIONS
• Amalgam
• Restorative Resins
• Glass Ionomer Cements
• Cast Gold Restorations
INTRODUCTION
By definition, pulp is a soft tissue of mesenchymal origin residing within the pulp chamber and root canals of teeth.
Some important features of pulp are as follows (Fig.13.1):
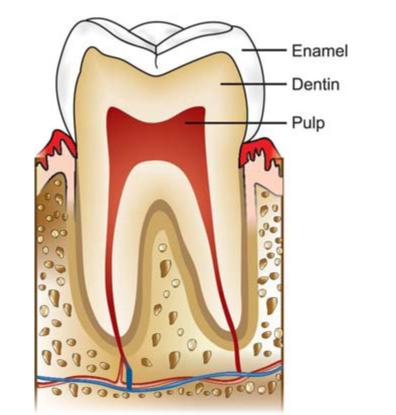
Fig. 13.1: Diagrammatic representation of dental pulp
•Pulp is located deep within the tooth, so defies visualization.
•It gives radiographic appearance as radiolucent line.
•Pulp is a connective tissue with several factors making it unique and altering its ability to respond to irritation.
• Normal pulp is a coherent soft tissue, dependent on its normal hard dentin shell for protection and hence, once exposed, extremely sensitive to contact and temperature but this pain does not last for more than 1-2 seconds after the stimulus removed.
• Since pulp is totally surrounded by a hard tissue, dentin which limits the area for expansion and restricts the pulp’s ability to tolerate edema.
• The pulp has almost a total lack of collateral circulation, which severely limits its ability to cope with bacteria, necrotic tissue and inflammation.
• The pulp possess unique cells the odontoblasts, as well as cells that can differentiate into hard-tissue secreting cells that form more dentin and/or irritation dentin in an attempt to protect itself from injury.
PULPAL IRRITANTS
Various pulpal irritants can be :
• Bacterial irritants: Most common cause for pulpal irritation are bacteria or their products which may enter pulp through a break in dentin either from:
– Caries (Fig. 13.2)
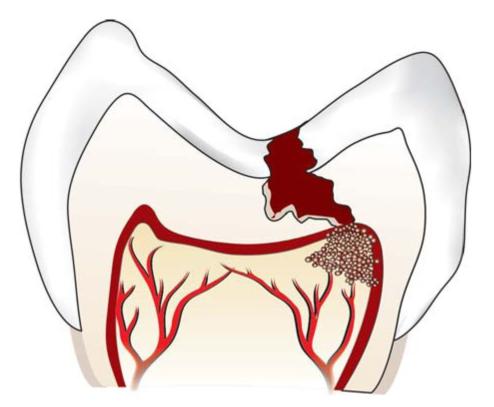
Fig. 13.2: Bacteria from caries resulting in pulpal irritation
– Accidental exposure
– Fracture
– Percolation around a restoration
– Extension of infection from gingival sulcus
– Periodontal pocket and abscess (Fig. 13.3)
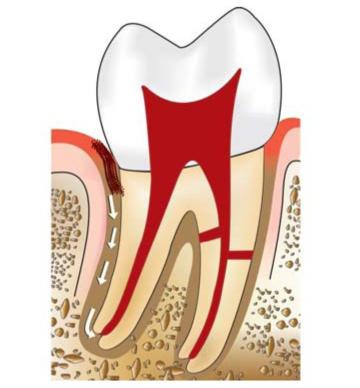
Fig. 13.3: Involvement of pulp via periodontal pocket
– Anachoresis (Process by which microorganisms get carried by the bloodstream from another source localize on inflamed tissue).
• Traumatic
– Acute trauma like fracture, luxation or avulsion of tooth
– Chronic trauma including parafunctional habits like bruxism.
• Iatrogenic: Various iatrogenic causes of pulpal damage can be:
– Thermal changes generated by cutting procedures, during restorative procedures, bleaching of enamel, microleakage occurring along the restorations, electrosurgical procedures, laser beam, etc. can cause severe damage to the pulp, if not controlled.
– Orthodontic movement
– Periodontal curettage
– Periapical curettage
– Use of chemicals like temporary and permanent fillings, liners and bases and use of desiccants such as alcohol.
• Idiopathic
– Aging
– Resorption-internal or external.
EFFECT OF DENTAL CARIES ON PULP
Dental caries is the most common route for causing irritation to the pulp. Dental caries is localized, progressive, decay of the teeth characterized by demineralization of the tooth surface by organic acids, produced by microorganisms. From the carious lesion, acids and other toxic substances penetrate through the dentinal tubules to reach the pulp. The following defense reactions take place in a carious tooth to protect the pulp:
1. Formation of reparative dentin.
2. Dentinal sclerosis, i.e. reduction in permeability of dentin by narrowing of dentinal tubules.
3. Inflammatory and immunological reactions.
The rate of reparative dentin formation is related to rate of carious attack. More reparative dentin is formed in response to slow chronic caries than acute caries. For dentin sclerosis to take place, vital odontoblasts must be present within the tubules. In dentin sclerosis, the dentinal tubules are partially or fully filled with mineral deposits, thus reduce the permeability of dentin. Therefore, dentinal sclerosis act as a barrier for the ingress of bacteria and their product (Fig. 13.4).
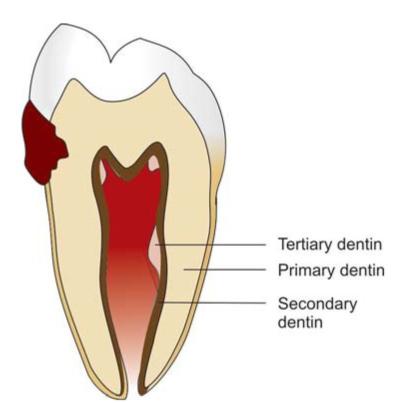
Fig. 13.4: Formation of irritation dentin in response to caries
EFFECT OF TOOTH PREPARATION ON PULP
Factors affecting response of pulp to tooth preparation
1. Pressure
2. Heat production
3. Vibrations
4. Remaining dentin thickness
5. Speed of rotation
6. Nature of cutting instruments.
Pressure
The pressure of instrumentation on exposed dentin characteristically causes the aspiration of the nuclei of the odontoblasts or the entire odontoblasts themselves or nerve endings from pulp tissues into the dentinal tubules. This will obviously stimulate odontoblasts, disturb their metabolism and may lead to their complete degeneration and disintegration. This can occur by excessive pressure of hand or rotary instruments, especially in decreased effective depths.
Heat Production
Heat production is the second most damaging factor. If the pulp temperature is elevated by 11°F, destructive reaction will occur even in a normal, vital periodontal organ. That “heat” is a function of;
1. Revolutions per minute (RPM), i.e. more the RPM more is the heat production. In deep penetrations of dentin without using coolants, e.g. pin holes, the cutting speed must not exceed 3,000 rpm.
2. Pressure: It is directly proportional to heat generation. Whenever, the RPM’s are increased, pressure must be correspondingly reduced.
3. Surface area of contact: It is related to the size and shape of the revolving tool. The more the contact between the tooth structure and revolving tool, the more is the heat generation.
4. Desiccation: If occurring in vital dentin, can cause aspiration of the odontoblasts into the tubules. The subsequent disturbances in their metabolism may lead to the complete degeneration of odontoblasts. Coolant sprays should be used even in nonvital or devitalized tooth structures, since the heat will burn the tooth structures.
Vibrations
Vibrations are measured by their amplitude or their capacity and frequency (the number/unit time). Vibrations are an indication of eccentricity in rotary instruments. The higher the amplitude, the more destructive may be the response of the pulp.
In addition to affecting the pulp tissues, vibration can create microcracks in enamel and dentin.
Remaining Dentin Thickness
Remaining dentin thickness (RDT) between the floor of the tooth preparation and the pulp chamber is one of the most important factor in determining the pulpal response. This measurement differs from the depth of tooth preparation since the pulpal floor in deeper preparation on larger teeth may be far from the pulp than that in shallow preparations on smaller teeth.
Remaining dentin thickness (RDT)
• In human teeth, dentin is approximately 3 mm thick
• Dentin permeability increases with decreasing RDT
• RDT of 2 mm or more effectively precludes restorative damage to the pulp
• At RDT of 0.75 mm, effects of bacterial invasion are seen
• When RDT is 0.25 mm, odontoblastic cell death is seen.
The amount of remaining dentin underneath the tooth preparation plays the most important role in the incidence of a pulp response. Generally, 2 mm of dentin thickness between the floor of the tooth preparation and the pulp will provide an adequate insulting barrier against irritants (Fig. 13.5). As the dentin thickness decreases, the pulp response increases. It is seen that response of cutting occurs only in areas beneath freshly cut dentinal tubules not lined with reparative or irregular dentin. In presence of reparative dentin only minimal response will occur.
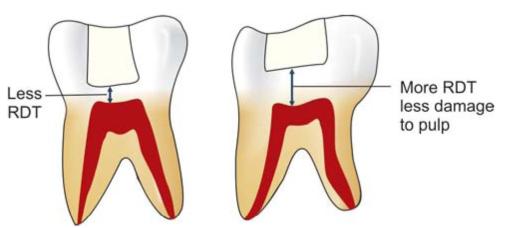
Fig. 13.5: As dentin thickness decreases, the pulp response increases
Speed of Rotation
Ultra high-speed should be used for removal of enamel and superficial dentin. A speed of 3,000 to 30,000 rpm without coolant can cause pulpal damage. It should be kept in mind that without the use of coolant there is no safe speed. High speed without coolant can produce burning of dentin, which in turn affect the integrity of the pulp.
Nature of Cutting Instrument
Use of worn off and dull instruments should be avoided. Damaged cutting edges cause vibration and reduced cutting efficiency.
Use of dull instruments encourages the dentist to use excessive operating pressure, which results in increased temperature. This can result in thermal injury to pulp.
EFFECT OF CHEMICAL IRRITANTS ON PULP
The pulp is subjected frequently to chemical irritation from materials generally used in dentistry. Various filling materials produce some irritation ranging from mild-to-severe, as do various medicaments used for desensitization or dehydration of the dentin.
Properties of a material that could cause pulpal injury are its cytotoxic nature, acidity, heat evolved during setting and marginal leakage (Fig. 13.6).
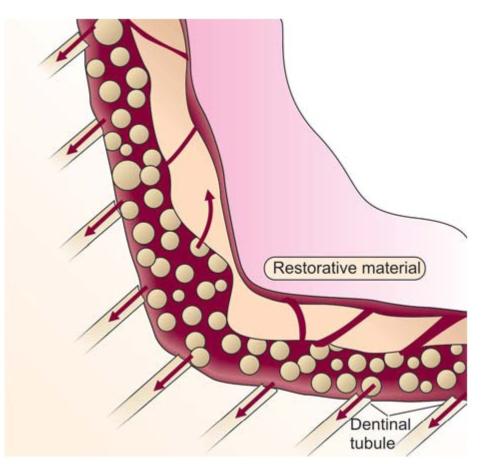
Fig. 13.6: Pathways of marginal leakage
Factors Influencing the Effect of Restorative Materials on Pulp
• Acidity
0 Absorption of water from dentin during setting
• Heat generated during setting
Poor marginal adaptation leads to bacterial penetration
• Cytotoxicity of material.
PULP PROTECTION PROCEDURES
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses



