CHAPTER 13 Periodontology
PERIODONTIUM
Periodontium consists of gingival tissues, periodontal ligament (PDL), cementum, alveolar bone. Functions as attachment mechanism, shock absorber, line of defense against external agents; attaches the tooth to its bony housing (alveolus), provides resistance to forces of mastication, speech, and deglutition, maintains body surface integrity by separating the external and internal environment, adjusts for structural changes associated with wear and aging through continuous remodeling and regeneration, and defends against external harmful factors.
Periodontal Diseases and Risk Factors
Tobacco Use Risk
Endocrine Disorder Risk
CLINICAL STUDY
| Age | 25 YRS | SCENARIO |
| Sex |  Male Male  Female Female |
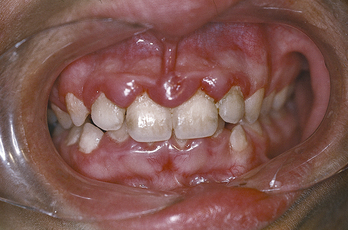
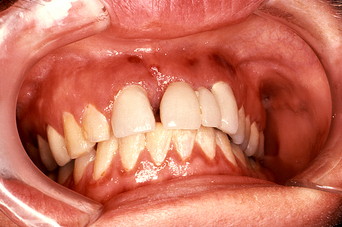
The patient, whom the dental office has been seeing regularly every 6 months for oral prophylaxis, presents with pocket depths that have increased from 3 to 4 mm and a bleeding score of 60%, according to the Ainamo and Bay bleeding index. Signs of gingival inflammation are present in the form of marginal erythema, generalized bulbous interdental papillae, and rolled margins. This finding is unusual for the patient because she has always exhibited meticulous oral hygiene. Moreover, dental biofilm and calculus are not present in noticeable quantities during this visit. |
| Height | 5′10″ | |
| Weight | 220 LBS | |
| BP | 120/82 | |
| Chief Complaint | “I gave up smoking and still my gums are a mess. Is it my being pregnant?” | |
| Medical History |
Nutritional Deficiency Risk
Poor nutrition lowers resistance to periodontal disease, which makes deficient individuals MORE at risk for infection and severe forms of periodontitis. In United States, nutritional deficiencies are found MOST commonly among elderly, lower socioeconomic groups, drug and alcohol abusers. Food consistency also has been recognized as contributing factor to accumulation of dental biofilm and thus development of periodontal disease. Poor nutrition can be modified with proper diet.
Adverse Drug Reaction Risk
HIV/AIDS Status Risk
CLINICAL STUDY
| Age | 38 YRS | SCENARIO |
| Sex |  Male Male  Female Female |
Patient has a chronic cough that he notes has persisted for several months. The extraoral examination reveals bilateral generalized lymphadenopathy. Intraorally, several large ulcerations that are red and raw are noted on the hard palate. Additionally, a thick white coating appears on portions of the hard palate and all of the soft palate, extending into the pharynx; when the coating is wiped off with gauze, raw inflamed tissue is exposed. The gingival tissues have a definite red band along the facial gingival margins of the maxillary arch; however, no bleeding is detected. |
| Height | 6′4″ | |
| Weight | 185 LBS | |
| BP | 105/68 | |
| Chief Complaint | “My mouth hurts so bad that I can’t eat. And I have not been feeling well lately.” | |
| Medical History |
Neutrophil Abnormality Risk
ETIOLOGY OF PERIODONTAL DISEASE
Defense Mechanisms of Oral Cavity
Inflammatory Response
Clinical Signs of Inflammation
Immune Response
Dental Biofilm
Dental biofilm (dental plaque) is a living, highly organized, and complex microbial ecosystem composed of more than 300 species of bacteria embedded in a gelatinous matrix. Classified as either supragingival or subgingival. Microflora associated with each type of periodontal disease classification as noted in the Human Oral Microbiome Database (HOMD) are listed in each subcategory, as well as Table 13-1. Presence of dental biofilm (and associated calculus) is the MOST common reason for gingivitis (NOT more obscure causes such as vitamin C deficiency).
| Microorganism | Gram stain reaction, motility | Associations |
|---|---|---|
| Aggregibacter (previously Actinobacillus) actinomycetemcomitans (Aa) | Gram negative, nonmotile | Chronic periodontitis (less than with Pg) and aggressive periodontitis, both localized and generalized; can invade tissue |
| Tannerella forsythensis (Tf) (previously Bacteroides forsythus [Bf]) | Gram negative, nonmotile | Early stages of gingivitis and chronic periodontitis |
| Campylobacter rectus (Cr) | Gram negative, motile | Chronic periodontitis |
| Porphyromonas gingivalis (Pg) | Gram negative, nonmotile | Chronic periodontitis (most prevalent) and generalized aggressive periodontitis |
| Prevotella intermedia (Pi) | Gram negative, nonmotile | Gingivitis with pregnancy and chronic periodontitis |
| Treponema denticola (Td) | NA, motile | Chronic periodontitis; can invade tissue |
Bacteria-Mediated Tissue Destruction
Etiology: Oral Contributing Factors
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


 •
•