Nonextraction Class II Correction
Ram S. Nanda, Tarisai C. Dandajena, Ravindra Nanda
Nonextraction treatment has gained in popularity in the orthodontic community since the second half of the twentieth century. This is due to the paradigm shift from focusing on the dentition to appraising the whole face. The careful selection of patients and timing of treatment are essential to the success of nonextraction treatment. When planning nonextraction treatment, we opt to use early treatment, redirection of growth, saving leeway space, guidance of eruption, and mechanics that aim to achieve distal movement of the maxillary molars. For a successful outcome, it is necessary before the initiation of treatment to take into consideration the type of malocclusion, facial type, required arch perimeter, individual growth, and motivation of the patient.
Class II, Division 1 malocclusion has been described as the most frequent treatment problem in orthodontic practice. It is estimated that about 35% of American children have Class II malocclusions. Distal movement of the maxillary first molars is a common goal in the treatment of the Class II molar relationship and in the resolution of tooth size–arch length discrepancy in the maxillary arch.
Early treatment is the key to successful treatment of Class II malocclusions. During the 1940s and 1950s Kloehn1 suggested the use of headgear during the transitional dentition to correct molar relations. In the 1960s Ricketts et al.2 promoted the bioprogressive philosophy, which used utility arches, quad helix, and cervical facebow headgear among several other innovative appliance systems. However, the real impetus behind nonextraction treatment was the realization that for far too long orthodontists had focused on the placement of the denture on the basal bone without sufficient regard to the facial integument. Research findings on long-term retention of treated dentitions revealed that relapse was common in both extraction and nonextraction treatment modalities. Cetlin and Ten Hoeve3 showed stable results for nonextraction treatment of patients with severe malocclusions. The thickness of facial soft tissue integument varies among individuals and its growth pattern is specific to individuals throughout their lifespan and not just during the period of active growth.4 In view of these findings, the nonextraction treatment modality has become a treatment of choice for select groups of patients.
Patient Selection
Patients need to be carefully selected for nonextraction treatment. Prospective patients to be treated using maxillary molar distalization techniques should exhibit a Class II dental relation or a minor skeletal Class II relation. A Class II relationship with mesial migration of maxillary molars due to premature loss of the primary molar is preferred. The patient should have minimal or no mandibular arch length discrepancy, preferably with mesofacial or brachyfacial types, and potential remaining growth. A low mandibular plane angle is most suitable because in high angle the distal movement of molars will tend to open the bite due to the extrusive force component. Even a full Class II relationship can be corrected if treated earlier. Recently, Kim et al.5 have shown that an occlusion established at an early age is more likely to be maintained despite the differential growth of the jaws.
A variety of appliances has been used, including ones that require patient cooperation and ones that do not.
Biomechanical Principles
The adequate force for distal movement of the molars is in the range of 150 to 250 g. The type of movement can be either translation or controlled tipping followed by uprighting. Translation movement requires the force to pass through the center of resistance (see Chapter 4). Therefore, when using any type of appliance, it is necessary to evaluate the force system of that appliance and to be informed about the side effects. Anchorage considerations include extrusion of molars and mesial movement of the anterior segment. To obtain the maximum benefit the distal resistance (the presence of second or third molars), growth in the tuberosity region, and functional interferences should be checked.
Treatment Modalities for Maxillary Molar Distalization
Several treatment modalities exist for the distal movement of the maxillary molars. These can be with either fixed or removable appliances, and intraoral or extraoral. The extraoral approach can use cervical, occipital, or high-pull headgear. The intraoral mechanics can be inter-arch or intra-arch. Of the inter-arch appliances, the Herbst, Twin Force bite corrector, Jasper jumper, and SAIF spring constitute fixed functional appliances that do not require patient compliance. Class II elastics with the jig and bimetric arch (Wilson appliance) require patient compliance. The transpalatal arch, coil springs, repelling magnets, K-loop,7 pendulum, Jones jig, and distal jet are intra-arch appliances. These appliances can be used as single entities or combined with another appliance. Some of these appliances are discussed below.
Headgear
Kingsley8 first introduced the extraoral method of applying traction to the maxillary arch to retract maxillary incisors. Later, Angle9 described and illustrated the headgear he used in the treatment of patients with Class II, Division 1 malocclusion. Both Kingsley and Angle used astonishingly modern-looking appliances, apparently with reasonable success. At the beginning of the twentieth century, the introduction of intermaxillary elastics resulted in the discontinuation of extraoral anchorage. This was not due to its ineffectiveness, but rather because it was considered an unnecessary complication.
By 1920 Angle and his followers were convinced that Class II and III elastics not only moved teeth but also caused significant skeletal changes, stimulating the growth of one jaw while restraining the other. If intraoral elastics could produce a true stimulation of mandibular growth while simultaneously restraining the maxilla, there would be no reason either to ask a patient to wear an extraoral appliance or to initiate treatment while waiting for the permanent teeth to erupt.
When cephalometric evaluations became available in the 1940s, they did not support the idea that significant skeletal changes occurred in response to intraoral forces. In 1936 Oppenheim10 strongly advocated extraoral anchorage therapy. Later, Kloehn1 demonstrated impressive results with headgear in the early treatment of Class II malocclusion. He stated that, during the transitional dentition, cervical traction can retard or even halt the forward growth of the maxilla and assist in moving maxillary teeth distally to correct developing Class II relationships.
While the distal movement of the molars by headgear may not be questionable, the changes that take place within the temporomandibular joint (TMJ) complex have not been well explained. Animal studies have shown remodeling of the condyle-glenoid fossa complex: apposition in the posterior compartment and resorption in the anterior compartment.11–13 Cephalometric studies have shown little or no change in the size of the mandible with the use of functional appliances such as headgear. It is possible that the lateral cephalogram is not sensitive enough to isolate these changes. The orthopedic forces applied by headgear cannot be ignored, however.
Extraoral traction has some demonstrable important advantages. These include maximum anchorage, ability to adjust the force levels, and control of bodily or tipping movement. It can assist in correcting transverse deficiencies by expanding the inner bow. The extrusive component of the cervical headgear will allow for bite opening in deep bite patients. If vertical control is a concern in a high-angle patient, a high-pull facebow headgear will control the extrusive force component.
There are limitations in the use of extraoral traction, of which the need for patient compliance is perhaps the most important. Besides compliance, the type of force delivered by the appliance is intermittent, with tooth movement usually being slower. We have found that prolonged use of headgear can delay the eruption of maxillary second molars or even lead to their impaction. This may not be a problem if treatment is initiated at the appropriate age of 9 years and for a limited time. In such cases the second molars need to be monitored if treatment is completed prior to their eruption. Extraction of the second molars may be considered if the presence of the third molars is radiographically documented. Despite these limitations, extraoral traction is perhaps one of the most effective ways to obtain distal movement of maxillary molars and a successful nonextraction treatment plan.
A decision to extract the second molars may be made in severe Class II cases where maximum retraction of the first molars is required. As mentioned, radiographic documentation for the presence of the third molars is important. Figure 12-1 documents a case in which extraction of the maxillary second molars was performed prior to their eruption. A mandibular lip bumper engaged to the mandibular first molar bands was used to align and unravel the minor mandibular crowding. The maxillary premolars were allowed to passively drift back. Retraction of the anterior segment, however, required active mechanics and this was accomplished using a T-loop. Class II elastics were used for 1 month. During this process the headgear was used as anchorage and the patient wore it only at bedtime.
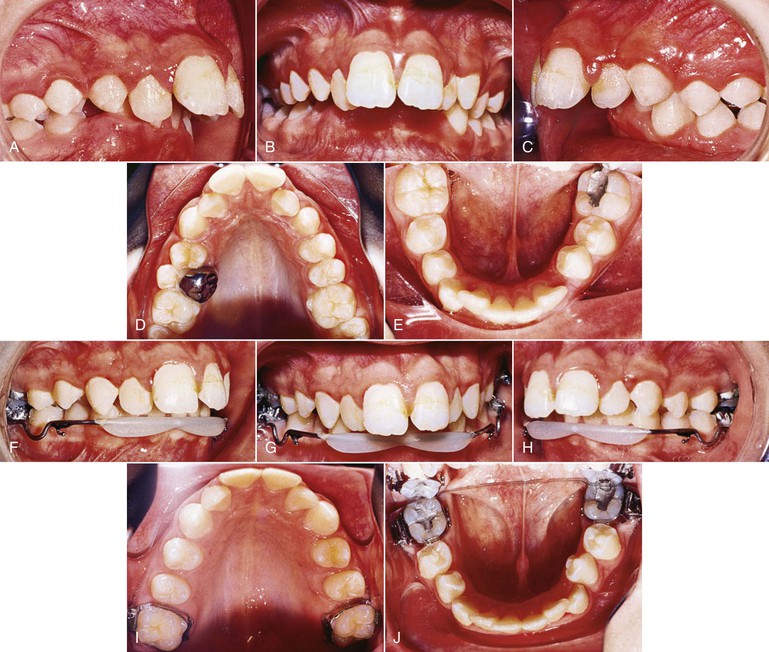
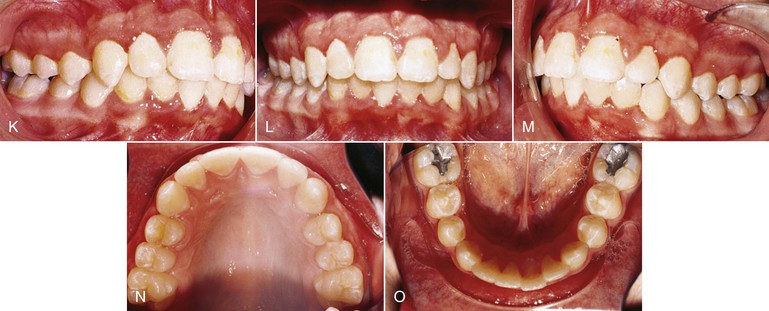
Figure 12-1 Headgear treatment. A–E, Pre-treatment intraoral photographs. A stainless steel crown is present on the exfoliating maxillary left second primary molar. F–J, Progress photographs show the lip bumper in place. K–O, Intraoral photographs 1 month post-treatment. Total treatment time was 23 months.
The headgear may be used effectively in cases of asymmetrical Class II correction. In such cases there is asymmetrical adjustment of the outer bow, one side being longer than the other.14,15 The longer arm of the outer bow will be placed on the side where correction of the Class II molar relationship is desired. Asymmetrically positioning the center of the outer bows while the arms are kept the same length may not achieve the same results as altering the lengths of the outer bows. This is because in the first instance the force applied will pass through the center, while in the latter instance there is an asymmetrical distribution of the moments. The greater moment is applied to the longer side.14,15 Of importance, however, is the need for patient compliance.
Care should be taken to adjust the facebow so as to achieve the desired result. In open bite, for example, care should be taken to avoid extrusion of the molars, while in cases of low mandibular plane angle extrusion of the molars may be a desired consequence. In such patients, then, application of the force above the center of resistance with the strap pulling down and backward will produce extrusion with distal movement.16 Figure 12-2 shows the various movements that can be obtained using the facebow headgear depending on the point of force application.16
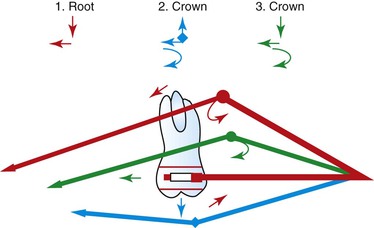
Figure 12-2 Forces and moments generated by the facebow headgear. 1, Force is above the center of resistance—the result is extrusion, mesial moment, and distal movement of the root. 2, Force is below the center of resistance in an upward direction—the effect is distal crown movement, clockwise moment, and an intrusive effect. 3, Force is below the center of resistance in a downward direction—the effect is extrusion, distal crown movement, and clockwise moment.
Vertical Holding Appliance
Some clinicians and investigators have sought ways to augment the extraoral traction. One method is the combined use of a vertical holding appliance (VHA)17,18 and high-pull headgear. The VHA (Fig. 12-3) has been recommended for treatment of high-angle patients where there is an important need to control the vertical dimension. It is fabricated from a 0.040-inch wire with a helix just distal to each maxillary first molar. Two more helices are placed at the center of the appliance, and these are separated by a V-bend to which is molded an acrylic button the size of a dime. The most mesial portion of this appliance (i.e., the acrylic button) should lie on a line that connects the mesial margins of the maxillary first molars. The button should also be 2- to 5-mm away from the palate. The VHA achieves the treatment objectives by way of an intrusive and distally directed force. The result is intrusion and distal movement of the molars. This is a fixed functional appliance since the forces are achieved from the functional activity of the tongue. In a study conducted at the University of Oklahoma,19 excellent results were achieved using the VHA compared to other methods.
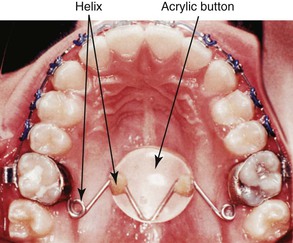
Figure 12-3 Vertical holding appliance (VHA). The first set of helices is positioned distal to the maxillary first molar and the second set is under the acrylic but not inside it. Only the V-bend attaches the 0.040-inch wire to the acrylic.
Though initially recommended for use in combination with headgear, we have noted that the VHA on its own is useful for correction of Class II malocclusion. Figure 12-4 documents a patient whose initial treatment plan was for treatment with a straight-pull facebow headgear, but she declined to use it. The patient was put under observation for 6 months while the VHA was cemented to the maxillary first molars. A fixed lingual arch (FLA) was also cemented to the mandibular arch for maintenance of the leeway space. Even though the leeway space may not always be available,19 the FLA can be used to control the vertical dimension during the growth period.20 After 6 months, correction of the Class II malocclusion was observed. No other appliance was used during this period.
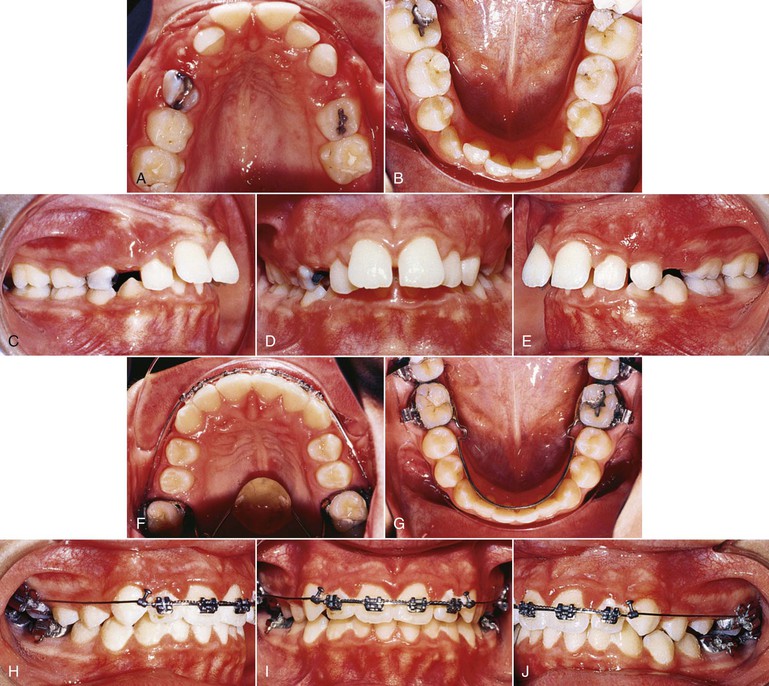
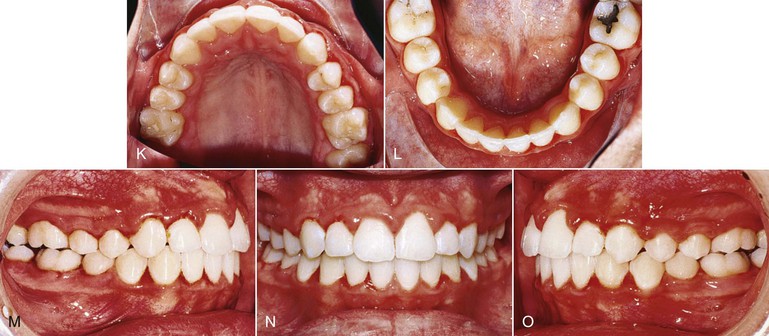
Figure 12-4 Class II, Division 1 malocclusion treated with a vertical holding appliance (VHA). A–E, Pre-treatment intraoral photographs of a Class II, Division 1 subdivision left malocclusion. F–J, Progress photographs showing a VHA cemented to the maxillary first molars and a fixed lingual arch (FLA) cemented to the mandibular first molars. These photographs were taken 6 months after delivery of the VHA and FLA. K–O, Final records at completion of treatment.
Although the forces generated by the VHA have not been measured, measurement of the forces applied to the transpalatal arch (TPA) from the tongue20 suggest that these forces may reach very high levels considering the size of the Nance button to which the 0.040-inch wire is attached. Chiba et al.21 noted that maximum pressure was applied to the TPA during deglutition when the appliance was engaged to the maxillary second molars. Also, this pressure was at its maximum when the TPA was positioned 6-mm from the palate.
Cervical Facebow with Removable Maxillary Plate
Cetlin has proposed the treatment of Class II relationships using a combination of TPAs (Fig. 12-5), cervical headgear, and a removable maxillary plate with auxiliary springs. This treatment modality requires correction of maxillary molar rotations (which in Class II are usually rotated mesiolingually) prior to distal movement and then distalization. The derotation of the molars in a distobuccal direction may produce a space gain of as much as 2- />
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


