CHAPTER 12 Diagnosis and Treatment Planning
Clinical Examination
Objectives of Prosthodontic Treatment
As was pointed out in Chapter 1, failure of removable partial dentures can usually be attributed to factors that result in poor stability. These can result from inadequate diagnosis and failure to properly evaluate the conditions present. This results in failure to prepare the patient and the oral tissues properly before the master cast is fabricated. The importance of the examination, the consideration of favorable and unfavorable aspects relative to movement control, and the importance of planning the elimination of unfavorable influences cannot be overemphasized (see Chapter 2).
Oral Examination
Sequence for Oral Examination
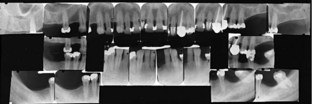
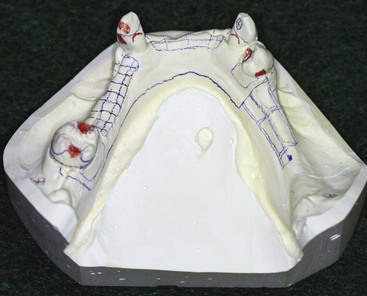
Diagnostic Casts
The impression for the diagnostic cast is usually made with an irreversible hydrocolloid (alginate) in a stock (perforated or rim lock) impression tray. The size of the arch will determine the size of the tray to be used. The tray should be sufficiently oversized to ensure an optimum thickness of impression material to avoid distortion or tearing on removal from the mouth. The technique for making impressions is covered in more detail in Chapter 15.
Purposes of Diagnostic Casts
Mounting Diagnostic Casts
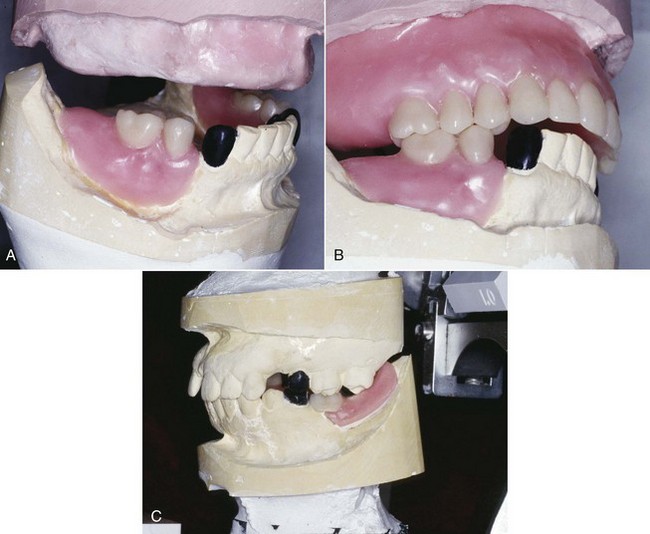
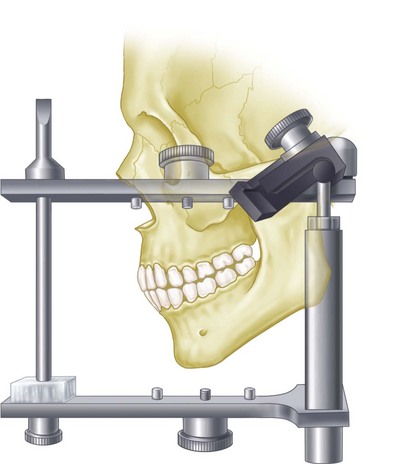
For diagnostic purposes, casts should be related on an anatomically appropriate articulator to best understand the role occlusion may have in the design and functional stability of the removable partial denture. This becomes increasingly important as the prosthesis replaces more teeth. If the patient presents with a harmonious occlusion and the edentulous span is a tooth-bound space, simple hand articulation is generally all that is required. However, when the natural dentition is not harmonious and/or when the replacement teeth must be positioned within the normal movement patterns of the jaws, the diagnostic casts must be related in an anatomically appropriate manner for diagnosis. This means placement of the maxillary cast in a position relative to the opening axis on the articulator, which is similar to the position of the maxilla in relation to the temporomandibular joint of the patient (Figure 12-6). The mandibular cast is then placed beneath the maxillary cast in a horizontal position dictated by mandibular rotation without tooth contact, at a minimal vertical opening.
The Glossary of Prosthodontic Terms* describes an articulator as a mechanical device that represents the temporomandibular joints and jaw members, to which maxillary and mandibular casts may be attached. Because the dominant influence on mandibular movement in a partially edentulous mouth is the occlusal plane and the cusps of the remaining teeth, an anatomic reproduction of condylar paths is probably not necessary. Still, movement of the casts in relation to one another as influenced by the occlusal plane and the cusps of the remaining teeth, when mounted at a reasonably accurate distance from the axis of condylar rotation, permits a relatively valid analysis of occlusal relations. This is more anatomically accurate than a simple hinge mounting.
Sequence for Mounting Maxillary Cast to Axis-Orbital Plane
The initial steps allow recording of the maxilla–temporomandibular joint (TMJ) relationship:
The next steps allow transfer of the recorded relationship to the articulator:
Casts are prepared for mounting on an articulator by placing three index grooves in the base of the casts. Two V-shaped grooves are placed in the posterior section of the cast and one groove in the anterior portion (Figure 12-7).
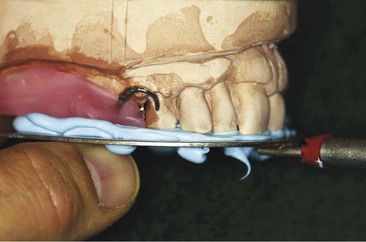
For purposes of illustration, a facebow using the external auditory meatus as the posterior reference point, the Whip-Mix Facebow technique (DB 2000, Whip-Mix Corp, Louisville, KY), will be shown. The facebow fork is covered with a polyether, polyvinyl siloxane or a roll of softened baseplate wax with the material distributed equally on the top and on the underneath side of the facebow fork. Then the fork should be pressed lightly on the diagnostic casts with the midline of the facebow fork corresponding to the midline of the central incisors (Figure 12-8). This will leave imprints of the occlusal and incisal surfaces of the maxillary casts and occlusion rim on the softened baseplate wax and is an aid in correctly orienting the facebow fork in the patient’s mouth. The facebow fork is placed in position in the mouth, and the patient is asked to close the lower teeth into the wax to stabilize it in position. It is removed from the mouth and chilled in cold water and then replaced in position in the patient’s mouth. An alternative method of stabilizing the facebow fork and recording bases is to enlist the assistance of the patient.
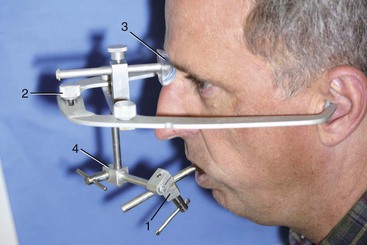
If an earpiece facebow is to be used, the patient should be reminded that the plastic earpieces in the auditory canals will greatly amplify noise. With the facebow fork in position, the facebow toggle is slipped over the anterior projection of the facebow fork (Figure 12-9). The patient can assist in guiding the plastic earpieces into the external auditory meatus. The patient can then hold the arms of the facebow in place with firm pressure while the operator secures the bite fork to the facebow. This accomplishes the radius aspect of the facebow transfer.
An auxiliary device called a cast support is available; it is used to support the facebow fork and the maxillary cast during the mounting operation (Figure 12-10). With this device, the weight of the cast and the mounting stone are supported separately from the facebow, thus preventing possible downward movement resulting from their combined weight. The cast support is raised to supporting contact with the facebow fork after the facebow height has been adjusted to the level of the orbital plane. Use of some type of cast support is highly recommended as an adjunct to facebow mounting.
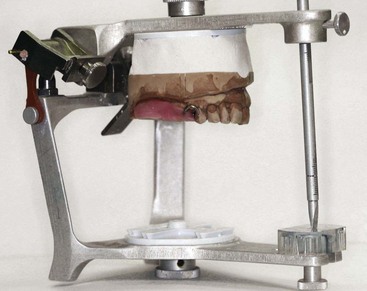
The keyed and lubricated maxillary cast is now attached to the upper arm of the articulator with the mounting stone, thus completing the facebow transfer (Figure 12-11). Not only will the facebow have permitted the upper cast to be mounted with reasonable accuracy, it also will have served as a convenient means of supporting the cast during mounting. Once mastered, its use becomes a great convenience rather than a time-consuming nuisance.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses