CHAPTER 9 Denture Base Considerations
Functions of Denture Bases in Control of Prosthesis Movement
The denture base supports the artificial teeth and consequently receives the functional forces from occlusion and transfers functional forces to supporting oral structures (Figure 9-1). This function is most critical for the distal extension prosthesis, as functional stability and comfort often relate directly to the ability for this transfer of forces to occur without undue movement.
Distal Extension Partial Denture Base
In a distal extension partial denture, denture bases other than those in tooth-supported modifications must contribute to the support of the denture. Such support is critical to the goal of minimizing functional movement and improving stability of the prosthesis. Although the abutment teeth provide support for the distal extension base, as the distance from the abutment increases, support from the underlying ridge tissues becomes increasingly important. Maximum support from the residual ridge may be obtained by using broad, accurate denture bases, which spread the occlusal load equitably over the entire area available for such support. The space available for a denture base is determined by the structures surrounding the space and by their movement during function. Maximum support for the denture base therefore can be accomplished only by using knowledge of the limiting anatomic structures and of the histologic nature of the basal seat areas, accuracy of the impression, and accuracy of the denture base (Figure 9-2). The first two of these support features relate to the gross size and cellular characteristics of the residual ridge tissues. These are highly variable between patients, and consequently not all residual ridges can provide the same quality of support. Therefore the ability to control functional displacement of the distal extension base is a determination that is unique for individual patients.
The snowshoe principle, which suggests that broad coverage furnishes the best support with the least load per unit area, is the principle of choice for providing maximum support. Therefore support should be the primary consideration in selecting, designing, and fabricating a distal extension partial denture base. Of secondary importance (but to be considered nevertheless) are esthetics, stimulation of the underlying tissues, and oral cleanliness. Methods used to accomplish maximum support of the restoration through its base(s) are presented in Chapters 15 and 16.
Boucher, writing on the subject of complete denture impressions, described these forces as follows:
The molding of the soft tissues around the polished surfaces of denture bases helps to perfect the border seal. Also, it forms a mechanical lock at certain locations on the dentures, provided these surfaces are properly prepared. This lock is developed automatically and without effort by the patient if the impression is made with an understanding of the anatomic possibilities.*
Methods of Attaching Denture Bases
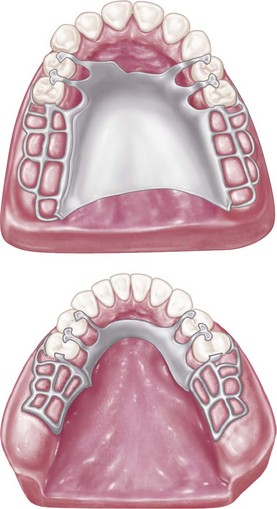
Acrylic-resin bases are attached to the partial denture framework by means of a minor connector designed so that a space exists between the framework and the underlying tissues of the residual ridge (Figure 9-3). Relief of at least a 20-gauge thickness over the basal seat areas of the master cast is used to create a raised platform on the investment cast on which the pattern for the retentive frame is formed (Figure 9-4). Thus after casting, the portion of the retentive framework to which the acrylic-resin base will be attached will stand away from the tissue surface sufficiently to permit a flow of acrylic-resin base material beneath its surface.
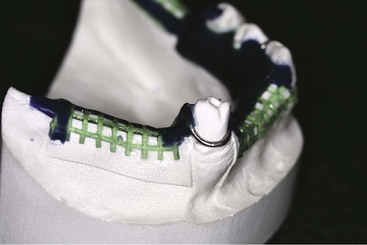
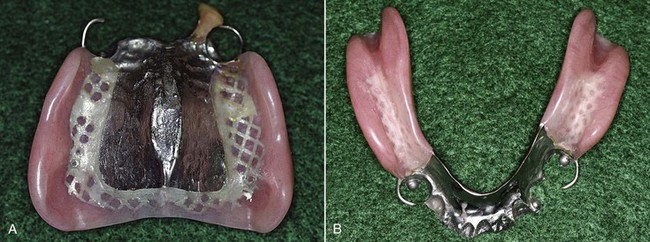
Figure 9-4 Unlike the minor connector designs in Figure 9-3, the designs used for this prosthesis have a plastic mesh pattern. Although such designs can be reinforced to be more rigid, the bulk of the connector itself may contribute to weakening of the resin base. A more open type of minor connector seems preferable.
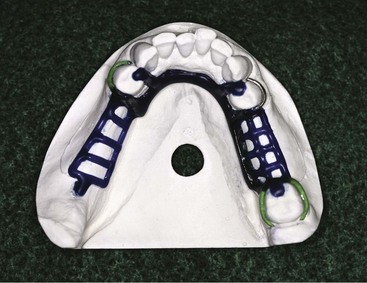
The use of plastic mesh patterns in forming the retentive framework is generally less satisfactory than a more open framework (see Figure 9-4). Less weakening of the resin by the embedded framework results from use of the more open form. Pieces of 12- or 14-gauge half-round wax and 18-gauge round wax are used to form a ladderlike framework rather than the finer latticework of the mesh pattern. The precise design of the retentive framework, other than that it should be located both buccally and lingually, is not as important as its effective rigidity and strength when it is embedded in the acrylic resin base. It should also be free of interference with future adjustment, should not interfere with arrangement of artificial teeth, and should be open enough to avoid weakening any portion of the attached acrylic-resin. Designing the retentive framework for denture bases by having elements located buccal and lingual to the residual ridge not only will strengthen the acrylic-resin base but also will minimize distortion of the base created by the release of inherent strains in the acrylic-resin base during use or storage of the restoration (Figure 9-5).
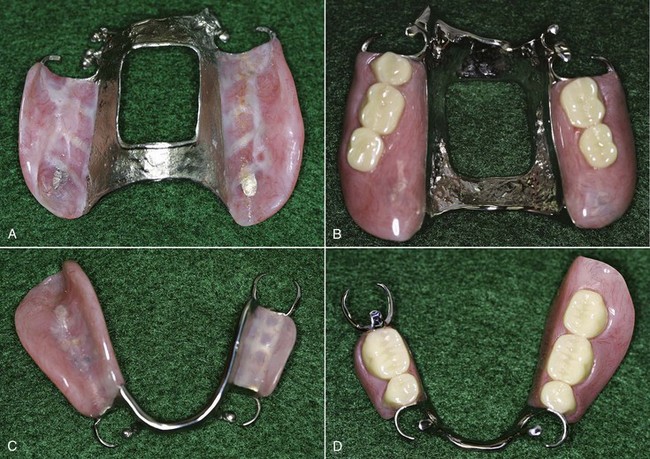
Metal bases are usually cast as integral parts of the partial denture framework. Mandibular metal bases may be assembled and attached to the framework with acrylic-resin (Figure 9-6).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses