11
When Should an Orthodontist Seek the Advice of an Endocrinologist?
Summary
A variety of dental abnormalities should prompt referral to an endocrinologist. A single central incisor and/or delayed dentition and a small chin are suggestive of possible growth hormone deficiency and accompanying hypopituitarism. Alternatively, widely spaced teeth, an enlarged tongue, and a prominent lower jaw (which may be associated with significant tall stature) may indicate acromegaly/gigantism due to growth hormone excess. Delayed or premature eruption of teeth in association with symptoms of hypo- or hyperthyroidism, with or without an enlarged thyroid gland, should prompt an endocrine referral. A diagnosis of ossifying fibroma of the mandible or maxilla with hypercalcemia raises concerns for hyperparathyroidism-jaw tumor syndrome. Consultation with an endocrinologist should also be obtained if deciduous teeth are lost prematurely with the root of the tooth still intact, since this may be indicative of hypophosphatasia. Dental abscesses in association with rickets raise concerns about X-linked hypophosphatemic rickets, whereas radiodensity of the maxilla and/or mandible may be suggestive of osteopetrosis. Fibrous dysplasia of the maxilla or mandible may be a component of McCune–Albright syndrome. Patients with diabetes should be monitored closely for periodontal disease. Maintaining contact with an endocrinologist is important to optimize diabetes control as an important step in preventing gum disease. When a high-arched palate and crowded teeth are noted in a young girl with short stature and any other clinical characteristics of Turner syndrome, a referral to an endocrinologist should be made. In addition, hyperpigmented gingivae in a patient with unusual skin hyperpigmentation may be a sign of primary adrenal insufficiency.
Introduction
Much is now known about the influence of hormones on orthodontic treatment. Hormones exert their influences in a variety of ways: endocrine (hormones acting on remote tissues), paracrine (hormones acting on nearby tissues), and autocrine (hormones acting on the tissues that secrete them). Orthodontic tooth movement and bone remodeling are closely linked and depend on both systemic and local hormone actions. The modeling and remodeling necessary for orthodontic tooth movements are part of a continuous process where mature bone is removed (bone resorption) and new bone is formed (bone formation). Bone resorption and formation are dependent on hormones including parathyroid hormone (PTH), 1,25 (OH)2 vitamin D, insulin-like growth factor 1 (IGF-1), and thyroid hormones.
Many endocrinological disorders have dental and oral manifestations as characteristic features. Recognizing these disorders is important in order to facilitate proper diagnosis and orthodontic therapy. This chapter is aimed at promoting communication between endocrinologists and orthodontists in the identification and management of growth- and bone metabolism-related endocrinopathies, and details the most common endocrine disorders with orthodontic or oral manifestations. Table 11.1 provides an overview of the conditions discussed in the chapter, their etiologies, and their main oral/dental manifestations.
Table 11.1 Endocrine disorders with dental/oral manifestations
| Condition | Etiology | Dental/oral manifestations |
| Growth hormone deficiency | Variable genetic etiology, most idiopathic | Delayed dentition, small mandible, midfacial hypoplasia, single central incisor |
| Acromegaly/gigantism | Most commonly due to a pituitary adenoma, can be seen in association with McCune–Albright syndrome and neurofibromatosis type 1 | Widely spaced teeth, prominent lower jaw, crossbite, coarse facial features |
| Thyroid disease | Variable, congenital versus acquired | Delayed or premature eruption of teeth, gum disease, large tongue |
| Hyperparathyroidism-jaw tumor syndrome | HRPT2 gene mutations | Ossifying fibroma of the mandible or maxilla |
| Hypophosphatasia | ALPL gene mutations | Premature loss of primary teeth |
| Nutritional rickets | Associated with calcium, phosphate, or vitamin D deficiency | Enamel hypoplasia |
| Delayed dentition | ||
| Increased susceptibility for caries | ||
| 1-α hydroxylase deficiency rickets | CYP27B1 mutations | Hypoplastic enamel with yellowish to brownish discoloration |
| Large pulp chambers and short roots | ||
| X-linked hypophosphatemic rickets | PHEX gene mutations | Defective dentin leading to recurrent dental abscesses |
| Fibrous dysplasia | GNAS1 gene mutations | Well-defined radiolucent bony lesions with ground-glass appearance in maxilla or mandible |
| Diabetes | Type 1 diabetes is autoimmune mediated and polygenic, type 2 diabetes is associated with obesity and is polygenic; most genetic mechanisms responsible for both type 1 and type 2 diabetes are unknown | Gingivitis and periodontitis; the latter can lead to early tooth loss |
| Primary adrenal insufficiency | Variable, congenital versus acquired | Hyperpigmented gingivae |
| Turner syndrome | Complete or partial loss of one of the X chromosomes | High-arched palate, crowding of teeth, mandibular retrognathia |
Growth Hormone Deficiency
Growth hormone deficiency (GHD) can either be isolated or seen in conjunction with other pituitary hormone abnormalities. Growth hormone, which is produced by the pituitary gland under regulation by the hypothalamus, is necessary for normal growth and development in children and for maintaining proper body fat distribution, muscle and bone health in adults. GHD can be either congenital or acquired. Although most instances of GHD are idiopathic, other causes include central nervous system (CNS) anatomical abnormalities involving the hypothalamic–pituitary axis, brain tumors, CNS surgery, trauma and infection, and radiation therapy to the brain.
Clinical and Biochemical Findings
GHD is commonly accompanied by delayed eruption of both primary and permanent teeth. Children with untreated GHD tend to have smaller facial heights and widths and smaller head circumferences than their age-matched peers (Segal et al., 2004). Growth hormone is necessary for both maxillary and mandibular growth, especially mandibular growth. Children with GHD tend to have a disparity in size between the mandible and maxilla and often exhibit a retrognathic mandible and crowding of teeth. The characteristic feature of GHD is linear growth delay. Laboratory findings include low insulin-like growth factor 1 (IGF-1 or somatomedin-C) level and low growth hormone levels on pharmacological stimulation testing. A referral to an endocrinologist should be considered in a child with delayed dentition, a small jaw, or a single central incisor, especially if slow growth or short stature is noted.
Diagnosis
The diagnosis of GHD relies on clinical and biochemical features. When a diagnosis of GHD is made, brain magnetic resonance imaging (MRI) is usually performed to assess the pituitary gland and rule out an underlying CNS abnormality.
Management
Treatment of GHD is with growth hormone therapy given in the form of daily subcutaneous injections. Although this therapy does not affect tooth formation (Ito et al., 1993), it will impact the timing of orthodontic interventions. Therefore, it is important for the treating endocrinologist and orthodontist to maintain good communication. Growth hormone therapy increases facial height, with a lesser effect on facial width, and may affect jaw alignment (Segal et al., 2004). Overtreatment with growth hormone can cause mandibular overgrowth. Orthodontic intervention when done in conjunction with growth hormone replacement therapy can resolve micrognathia associated with GHD to an extent. In a case report, Tsuboi et al. (2008) suggested that catch-up growth in the craniofacial structures (with increases in Z-scores) occurs alongside increases in stature during orthodontic treatment carried out concurrently with growth hormone therapy.
A single central incisor has also been described in isolated GHD and GHD in association with additional pituitary hormone deficiencies (Artman and Boyden, 1990; Hamilton et al., 1998). It is also the hallmark of the solitary median maxillary central incisor (SMMCI) syndrome (Hall, 2006), which is described in detail in Chapter 7. Thus, when a single central incisor is detected on examination, the treating dentist should elicit a history of short stature or growth delay and a referral to an endocrine clinic and craniofacial center should be considered for further investigations and management.
Growth Hormone Excess
Excessive pituitary production of growth hormone results in characteristic clinical features. In a growing child, the condition is referred to as gigantism and is associated with abnormally tall stature. When growth hormone excess develops in adulthood, the term acromegaly is used. The most common cause of gigantism and acromegaly is a pituitary adenoma, a benign tumor of the pituitary gland (Eugster and Pescovitz, 1999). Patients with suspected acromegaly, based on clinical features, should be referred to an endocrinologist.
Clinical Features
Common facial features of acromegaly include a protruding lower jaw (prognathism) due to mandibular bone overgrowth, an enlarged tongue, coarse facial features with a prominent forehead, widening of the maxilla, widely spaced teeth and a skeletal Class III relationship (Figure 11.1). Additional features include significant tall stature, especially when the disease onset is in childhood, large hands and feet, excessive sweating, muscle weakness, and thick skin. When the tumor is large, compressive symptoms can result in headaches and visual disturbances.
Figure 11.1 Widely spaced teeth, prominent lower jaw, and coarse facial features in a child with gigantism.

Diagnosis
The diagnosis of growth hormone excess is made using a combination of baseline IGF-1 levels, the response of growth hormone levels to an oral glucose tolerance test, and pituitary imaging. Occasionally, enlargement of the sella turcica may be seen on skull films. Chang et al. (2005) described the case of a patient with gigantism due to a pituitary adenoma who presented to an orthodontic office for correction of anterior crossbite due to mandibular prognathism. Skull films demonstrated an enlarged sella turcica in all dimensions along with deepening of its floor in routine cephalometric analysis. Generally, however, diagnosis of pituitary tumor is based on MRI rather than plain X-ray analysis.
Treatment
Treatment may consist of resection of the pituitary lesion and/or therapy with somatostatin analogs. After the condition is under control, orthognathic surgery can be considered for correction of occlusion and profile. Patients need to be monitored for recurrence. Yagi et al. (2004) described a case of an acromegalic patient who had surgical–orthodontic correction after his acromegaly had been controlled with drugs for 5 years following a transsphenoidal hypophysectomy. Unfortunately, during the retention period, an MRI revealed recurrence of the lesion, resulting in higher IGF-1 levels and slight mandibular prognathic changes.
Thyroid Disease
The thyroid gland produces two hormones, calcitonin and thyroxine. Calcitonin is a minor hormone in bone metabolism, which works opposite to PTH and decreases serum calcium levels. Calcitonin therapy has been reported to be useful for osteoporosis and giant cell granulomas of the jaw. However, its utility is limited due to possible allergic reactions and tachyphylaxis with multiple doses. No disease related to calcitonin excess or deficiency in humans has yet been described. Therefore, the remainder of this discussion will be about thyroid hormones.
Thyroxine (T4) is a prohormone that is converted to its active form triiodothyronine (T3). This active hormone influences the activity and metabolism of all cells, and it plays an important role in physical development and growth. Thyroid disease can be congenital or acquired. Most common etiology for acquired thyroid disease is autoimmune. Hashimoto thyroiditis is most commonly associated with hypothyroidism, whereas Graves disease is the most common cause of hyperthyroidism.
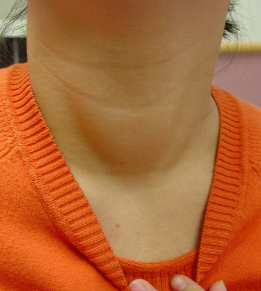
Both hypothyroidism and hyperthyroidism can affect dental health, as can the treatment for thyroid cancer. Persons with either hypo- or hyperhyroidism may also have a goiter (enlarged thyroid gland) palpable on examination (Figure 11.2), which should prompt a referral to an endocrinologist. Premature or delayed tooth eruption in a child should also alert the treating dentist to the possibility of thyroid disease.
Figure 11.2 Enlarged thyroid gland (goiter) in a child with hyperthyroidism.
Clinical Findings
Common symptoms of hypothyroidism are fatigue, increased sleepiness, dry skin and brittle hair, cold intolerance, mild weight gain, and constipation. In children, growth may be slowed, depending on severity of hypothyroidism. Children with hypothyroidism may have a wide variety of dental problems, including malocclusion, delayed eruption of primary and permanent teeth, a prominent tongue and swollen gingivae, and an increased risk of caries and gingival disease. Adults with hypothyroidism may have an enlarged tongue, delayed postoperative wound healing, and defects in taste and smell.
Hyperthyroidism is associated with symptoms of weight loss, difficulty in sleeping, and a decline in school or work performance. Bulging of the eyes (exophthalmos) is characteristic of Graves disease. Children with hyperthyroidism may experience premature tooth eruption. The most common forms of thyroid cancers are treated with high doses of radioactive iodine. This treatment can cause gingival pain and swelling, and increased salivation.
Diagnosis
The diagnosis of thyroid disease is made based on clinical and laboratory findings. The presence of a goiter, particularly with palpable nodularity, should prompt thyroid function testing (usually measurement of thyroid-stimulating hormone (TSH) and thyroxine levels [T4 or free T4]) and referral for endocrine evaluation. An elevated TSH level in association with low thyroxine levels is diagnostic of primary hypothyroidism whereas a low TSH level in association with an elevated thyroxine level usually indicates primary hyperthyroidism.
Management
Treatment of hypothyroidism is with thyroid hormone replacement. Treatment of hyperthyroidism depends on the etiology and may include radioactive iodine, anti-thyroid medications, and/or surgery. High levels of thyroxine (either from primary hyperthyroidism or from ingestion of too much thyroxine) may result in increases in osteoclastic activity and faster tooth movement rates (Shirazi et al., 1999). Close collaboration with an endocrinologist is preferred so that the thyroid hormone levels are monitored and controlled while orthodontic forces are applied for achieving optimal results.
Hyperparathyroidism-Jaw Tumor Syndrome
Parathyroid hormone is secreted by the parathyroid glands and stimulates bone resorption, primarily through its effects on vitamin D metabolism. PTH also reduces renal clearance of calcium and increases intestinal calcium absorption. In primary hyperparathyroidism, autonomous production of PTH from the parathyroid glands leads to increased serum calcium levels. Secondary hyperparathyroidism is seen when PTH secretion is increased because of hypocalcemia. Orthodontic tooth movement can be stimulated by exogenous PTH in a dose-dependent manner when the jaw is exposed to continuous PTH, either by systemic infusion or by local delivery every other day in a slow-release formulation (Soma et al., 1999). Rarely, hyperparathyroidism can be associated with ossifying fibromas as part of the hyperparathyroidism-jaw tumor syndrome.
A painless mass in the mandible or maxilla could represent an ossifying fibroma, a benign fibrous tumor with local aggressive behavior. As mentioned above, ossifying fibromas are associated with the hyperparathyroidism-jaw tumor syndrome. This is a rare autosomal dominant syndrome caused by inactivating mutations of the tumor suppressor gene HRPT2 (Carpten et al., 2002). It is characterized by multiple parathyroid tumors occurring at an early age. These tumors lead to development of hyperparathyroidism, and also ossifying fibromas of the mandible and/or maxilla, and less frequently, a variety of renal lesions and uterine tumors. When ossifying fibromas are suspected, a careful family history should be taken, focusing on history of hypercalcemia and hyperparathyroidism, which is important in making decisions regarding further investigations and management.
Clinical and Biochemical Findings
Symptoms of hypercalcemia are often subtle but include increased thirst and urination, nausea, vomiting, constipation, weakness, restlessness, confusion, and altered mental status. In hyperparathyroidism, serum calcium levels are elevated in association with low serum phosphorus levels. An ossifying fibroma presents as a bony, hard, non-tender mandibular swelling.
Diagnosis
Diagnosis is based on clinical, biochemical, radiological and histological findings. Radiographically, the lesions are either completely radiolucent or mixed, depending on the amount of calcification, or are completely radiopaque and surrounded by a radiolucent rim. In each type, there is a sclerotic border around the lesion. Histologically, the tumor consists of cementum-like or bony masses distributed in a highly cellular fibrous stroma.
Treatment
Ossifying fibromas are treated surgically. Large lesions, particularly of the maxilla, are often aggressive and require radical surgery. Small lesions can be treated with conservative excision. After curettage, nearly a third of mandibular lesions will recur. To minimize the likelihood of recurrence, en bloc or partial jaw resections are preferred. Gurol et al. (2001) reported successful orthognathic surgery following presurgical orthodontic treatment for correction of a retrognathic mandible in a 17-year-old girl with an ossifying fibroma.
Hypophosphatasia
Hypophosphatasia is a rare metabolic disease, with an estimated incidence of 1:100 000 (Mulivor et al., 1978). A history of premature tooth exfoliation should raise concerns for hypophosphatasia, which results from a mutation in the ALPL (alkaline phosphatase, liver/bone/kidney) gene encoding the tissue-nonspecific alkaline phosphatase enzyme (TNSALP) (Mornet and Simon-Bouy, 2004). TNSALP is important for normal bone and tooth mineralization. Five clinical forms are described: perinatal (lethal), infantile, childhood, adult, and odontohypophosphatasia. Children with the perinatal, infantile, and childhood forms can present with severe skeletal manifestations of under-mineralized bone, including frequent fractures. In odontohypophosphatasia, clinical manifestations are limited to the teeth. In a child with suspected hypophosphatasia, it is important for the dentist to inquire about a history of bon/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


