Chapter 11 Oral implications of infection in compromised patients
The term ‘medically compromised’ is often misused. The definition of a medically compromised patient is one who by virtue of their medical condition, or its treatment, is susceptible to infection and other serious complications. Conditions which cause patients to be medically compromised can either be congenital or acquired. Medical compromise can be due to a whole variety of factors, some of which are illustrated in Table 11.1. The term ‘immunocompromised’ refers specifically to congenital or acquired alterations of the immune system, which may render an individual susceptible to infection. The number of immunocompromised individuals is increasing rapidly, mostly because of the AIDS pandemic, but also through intervention therapy (drugs which deliberately modify the immune system). A good example of the latter is deliberate suppression of the immune system with drugs to prevent rejection during and following solid organ transplantation. The oral microflora in immunocompromised patients is changed either by colonization with exogenous microorganisms which are not normally found in the mouth, or by the occurrence of opportunistic infection. It used to be believed that any person who was immunocompromised had to be given prophylactic antibiotics to prevent infection after surgery. This is not necessary unless there is a proven degree of impairment of immune defences which renders them susceptible to infection. The extent to which an immunocompromised patient is susceptible to infection can be measured by a variety of blood tests to assess the function of their immune system. These include simple tests on the number and proportion of their immunological cells (predominantly white cells), their function, or their degree of abnormality. Only where there is a proven loss of functional protective immunity is there a necessity to give prophylactic antimicrobials before surgery (Ch. 8).
Table 11.1 Orofacial infections that may occur in medically compromised patients
| Disorder | Example | Orofacial infection |
|---|---|---|
| Endocrine disorders | Diabetes mellitus | Oral fungal infections |
| Respiratory disorders | Asthma | Oral fungal infections |
| Neurological disorders | Epilepsy | Gingival hyperplasia and periodontal disease |
| Neoplastic disease | Oral carcinoma | Dental caries and mucositis following radiotherapy |
| Chronic infection | Tuberculosis | Oral tuberculosis |
| Immunological disorders | HIV and AIDS | Oral viral and fungal infections |
| Haematinic deficiencies | Anaemia | Angular cheilitis and oral fungal infections |
The status of the teeth and oral soft tissues is often a reflection of systemic health. Thus, opportunistic orofacial infection may be the presenting initial feature of systemic disease. In this chapter, the types of orofacial infection that are seen in medically compromised patients as a result of the presence of underlying disease or as a result treatment will be considered.
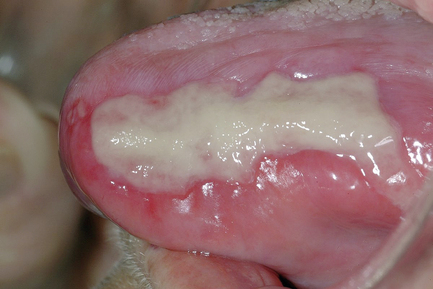
Post-irradiation mucositis
Another of the consequences of irradiation of the oral region is non-specific inflammation of the oral mucosa, often called mucositis (Fig 11.1). This can be extensive and cause considerable pain with difficulties in feeding. Symptoms may be severe enough to influence the patient to abandon the radiation treatment. At first it was thought that radiation mucositis was due to infection by Candida spp., and other yeasts. However, provision of antifungal therapy has no effect, suggesting that yeasts are not causing the condition. More extensive sampling of the mucosa has shown that the microflora associated with mucositis is mainly composed of Gram negative aerobic and facultatively anaerobic bacteria such as Escherichia coli, pseudomonads, Klebsiella spp, and Acinetobacter spp.. Irradiation mucositis can be largely alleviated by selective decontamination of the oral cavity before and during irradiation therapy by applying topically a combination of non-absorbable antimicrobials onto the tissues to be protected. The usual combinations of antimicrobials are polymixin and tobramycin, and an antifungal is added to prevent yeast overgrowth. Two antimicrobials are used in order to prevent the selection of resistance in Gram negative bacteria. This combination can be used to ameliorate the effects of the mucositis.
Staphylococcal mucositis
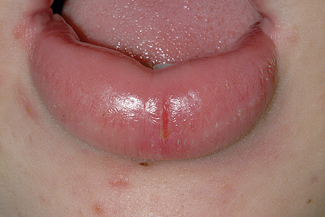
Recent surveys of data from oral samples processed in microbiology laboratories have shown that Staphylococcus spp. are frequently isolated. The predominant species isolated is Staphylococcus aureus with a minority of these being methicillin-resistant (MRSA). Many of these isolations have been obtained from patients who are debilitated, or are terminally ill. In addition, staphylococci have been isolated from orofacial granulomatosis, in particular within fissures of swollen lips (Fig. 11.2). The presenting features of orofacial granulomatosis are identical to those of Crohn’s disease, which is a chronic inflammatory condition of the gut. There is debate as to how frequently staphylococci infect or colonize the mouth. Recently, it has been proposed that there is a discrete condition called staphylococcal mucositis which occurs in debilitated individuals.
Pyostomatitis vegetans
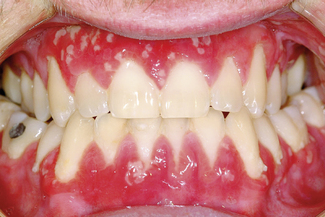
This condition is associated with the presence of active inflammatory bowel disease, in particular, ulcerative colitis or Crohn’s disease. The oral mucosa is diffusely inflamed, with fissured ulcers separating papillary projections (Fig. 11.3). Histological examination reveals suprabasal separation of the epithelium with the formation of eosinophilic abscesses. The severity of pyostomatitis vegetans often mirrors the bowel disease activity. Interestingly, the provision of metronidazole can relieve oral symptoms. Healing occurs when the underlying inflammatory bowel disorder is brought under control.
Cancrum oris (noma, gangrenous stomatitis)
This is a severe form of necrotizing periodontal disease, and is seen occasionally in developing countries, in particular, sub-Saharan Africa (Ch. 6). The sufferer is characteristically less than 10 years of age, malnourished and has a history of a recent viral infection, such as measles (Ch. 10). The initial lesion spreads into the cheek, face and neck causing extensive tissue loss. Treatment is with a combination of antibiotics, such as benzylpenicillin with metronidazole, but each combination should include agents active against both Gram negative and Gram positive microorganisms.
Xerostomia
Xerostomia means literally dry mouth and can be caused by a variety of conditions or treatments (Table 11.2). One of the consequences of xerostomia is overgrowth of dental plaque, with acidogenic oral streptococci and lactobacilli predominating within the biofilm. This can induce a dramatic increase in dental caries if teeth are present. Xerostomia predisposes to the development of mucositis and opportunistic Candida infections of the oral mucosa.
| Drug therapy (in particular antidepressants) |
| Sjögren’s syndrome (immunological destruction of salivary tissues) |
| Damage to salivary glands following radiotherapy |
| Undiagnosed or poorly controlled diabetes |
| Dehydration |
| Congential absence of salivary glands |
Gingival hyperplasia and immunosuppressive agents
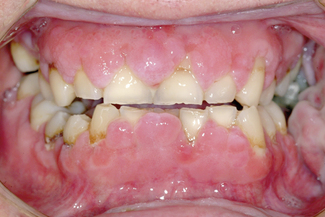
Following organ transplantation it is necessary to take immunosuppressive agents to prevent the immune system causing rejection of the transplant. One of the curious consequences of taking these antirejection agents is that the gingivae enlarge due to overgrowth of fibrous tissue (Fig. 11.4). The gingival overgrowth is worse if the oral hygiene of the mouth is poor. No plaque bacteria have been associated with this condition, which was thought to be directly due to the systemic action of the immunosuppressive agents. If the patient is treated with low doses of macrolide antimicrobials (e.g. azithromycin), then the overgrowth can be prevented or reduced. This evidence supports the contention that gingival hyperplasia is an infective inflammatory process but the infecting bacteria have still to be identified.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses