Chapter 11
Miscellaneous Lesions
Aim
This chapter aims to outline the non plaque-induced periodontal lesions and manifestations of systemic diseases that do not readily fall under the descriptive headings used in the previous 10 chapters. These lesions present primarily as incidental or intentional radiological findings, as gingival bleeding that is inconsistent with local irritants, as para-gingival swellings or annular lesions.
Outcome
At the end of this chapter the reader should have a clear insight into the nature, diagnosis and management of lesions that are discussed therein.
Introduction
Table 11-1 summarises the non-radiological lesions to be discussed. Tables 11-2 to 11-4 list those lesions normally detected radiologically and consistent with the general approach taken within this text, categorised by radiological appearance. The approach taken is similar to that of Langlais, Langeland and Nortjé in Diagnostic Imaging of the Jaws, which is recommended for further reading. Radiological features of periodontitis are not discussed, and those lesions of the soft tissues that can appear on radiographic films are also beyond the scope of this chapter. Only those lesions and conditions likely to present to the periodontal clinician rather than the radiologist will be discussed briefly.
| Category | Condition | Sub-Classification | Discussed or Refer Reader |
| Uncontrolled/ un-explained gingival bleeding | Myelodysplasia | Primary | discussed |
| Secondary | discussed | ||
| Clotting factor deficiencies | Factor VIII | discussed | |
| Factor IX | discussed | ||
| Idiopathic thrombocytopenic discussed purpura (ITP) | discussed | ||
| Platelet pool storage disease | discussed | ||
| Acute leukaemia | discussed | ||
| Chronic leukaemia | discussed | ||
| Thrombocytopaenia | Secondary to liver disease | discussed | |
| Drug-induced | discussed | ||
| HIV-associated | discussed | ||
| Benign familial thrombocytopaenia | discussed | ||
| Aplastic anaemia | discussed | ||
| Thrombasthenia | discussed | ||
| Patients on warfarin | discussed | ||
| Para-gingival swellings | Osteomas | discussed | |
| Gardner’s syndrome | discussed | ||
| Mandibular/maxillary tori | discussed | ||
| Annular lesions | Erythema migrans | discussed | |
| Erythema multiforme | Stevens Johnson syndrome | discussed |
| Radiological Categorisation | Condition | Sub-group | Discussed or Refer Reader |
| Root resorption | Internal root resorption | reader referred | |
| External root resorption | Cervical Infra-cervical |
discussed | |
| Inter- and peri-radicular radiolucencies | Scleroderma (systemic sclerosis) | discussed | |
| Periapical cemental dysplasia | discussed | ||
| Lateral developmental periodontal cyst (Botyroid cyst) | discussed | ||
| Lateral inflammatory periodontal cyst | discussed | ||
| Gingival cyst | discussed | ||
| Incisive canal cyst | discussed | ||
| Solitary bone cyst | reader referred | ||
| Median mandibular cyst | reader referred | ||
| Squamous odontogenic tumour | discussed | ||
| Ameloblastoma | Classical Unicystic Peripheral Malignant |
discussed | |
| Ameloblastic fibroma | discussed | ||
| Histiocytosis-X | Unifocal (solitary eosinophilic granuloma) | ||
| Inter- and periradicular radiopacities | Periapical osteosclerosis (sclerosing osteitis) | discussed | |
| Condensing osteitis | discussed | ||
| Hypercementosis | discussed | ||
| Cementomas | Cementoblastoma | discussed | |
| Periapical cemental dysplasia | discussed | ||
| Gigantiform cementoma | discussed | ||
| Cementicles | discussed | ||
| Ossifying fibroma | discussed |
| Radiological Categorisation | Condition | Sub-group | Discussed or Refer Reader |
| Well circumscribed radiolucencies | Odontogenic keratocyst | discussed | |
| Inflammatory cysts | Periapical | discussed | |
| Peri-implant | discussed | ||
| Neural sheath tumours | Neurilemmoma | discussed | |
| Schwannoma | discussed | ||
| Neurofibroma | discussed | ||
| Neurofibromatosis | discussed | ||
| Multi-locular radiolucencies | Odontogenic keratocyst and Gorlin-Goltz syndrome | discussed | |
| Botyroid cyst (lateral developmental periodontal cyst) | discussed | ||
| Ameloblastoma | Polycystic | discussed | |
| Malignant | discussed | ||
| Odontogenic myxoma | discussed | ||
| Giant cell tumour of bone (central giant cell granuloma) | discussed | ||
| Arterio-venous malformation | discussed | ||
| Aneurysmal bone cyst | discussed | ||
| Central haemangioma | reader referred | ||
| Sturge Weber syndrome | Arterio-venous malformations | discussed | |
| Cherubism | discussed | ||
| Odontogenic fibroma | reader referred | ||
| Ossifying fibroma | Calcifying/ossifying fibrous epulis | discussed | |
| Poorly defined radiolucent lesions | Osteomyelitis | discussed | |
| Osteoradionecrosis | Sterile Septic |
discussed | |
| Intraosseous carcinoma | discussed | ||
| (Epidermoid carcinoma) | |||
| Gingival carcinoma | Squamous cell | discussed | |
| Cuniculatum | discussed | ||
| Mucoepidermoid carcinoma | reader referred | ||
| Clear cell carcinoma | reader referred | ||
| Ameloblastic carcinoma | discussed | ||
| Metastatic tumour | Adenocarcinoma of lung | reader referred | |
| Prostate carcinoma | reader referred | ||
| Breast carcinoma | reader referred | ||
| Renal carcinoma | reader referred | ||
| Melanoma | reader referred | ||
| Fibrosarcoma | reader referred | ||
| Ewings sarcoma | reader referred | ||
| Radiolucent lesions as presentations of disseminated disease | Histiocytosis-X | Progressive (disseminated or Letterer-Siwe disease) | discussed |
| Multifocal (Hand-Schuller-Christian syndrome) | discussed | ||
| Multiple myleoma | discussed | ||
| Non-Hodgkins lymphoma | discussed | ||
| Burkitt’s lymphoma | reader referred | ||
| Leukaemia | discussed | ||
| Generalised radiolucencies | Hypophosphatasia | Neonatal (Lethal) | discussed |
| Infantile | discussed | ||
| Childhood | discussed | ||
| Adult | discussed | ||
| Pseudo-hypophosphatasia (Odontohypophosphatasia) |
discussed | ||
| Hyperparathyroidism | Brown tumours | discussed | |
| Sickle cell anaemia | discussed | ||
| β-thalassaemia | reader referred | ||
| Radiolucent lesions with radiopacities | Periapical cemental dysplasia | discussed | |
| Calcifying odontogenic cyst | discussed | ||
| Calcifying epithelial odontogenic tumour | discussed | ||
| Adenomatoid odontogenic tumour | discussed | ||
| Ameloblastic fibroadenoma | reader referred | ||
| Odontomes | Compound | discussed | |
| Complex | discussed |
| Radiological Categorisation | Condition | Sub-group | Discussed or Refer Reader |
| Focal radioopacities | Garrè’s osteomyelitis | reader referred | |
| Hyperostosis | reader referred | ||
| Osteoma | discussed | ||
| Osteoblastoma | reader referred | ||
| Osteoclastoma | reader referred | ||
| Osteosarcoma | discussed | ||
| Osteogenic sacroma | reader referred | ||
| Chondroma | reader referred | ||
| Chondroblastoma | reader referred | ||
| Chondrosarcoma | reader referred | ||
| Generalised radiopacities | Gardner’s syndrome | discussed | |
| Osseous dysplasia | reader referred | ||
| Sclerosing osteomyelitis | discussed | ||
| Fibrous dysplasia | discussed | ||
| Albright’s syndrome | discussed | ||
| Paget’s disease | discussed | ||
| Osteopetrosis | Albers-Schönberg disease | discussed | |
| Hyperostosis | discussed |
Uncontrolled/Unexplained Gingival Bleeding
When patients present with gingival bleeding that is not consistent with levels of plaque or inflammation, underlying systemic disease should be suspected and appropriate investigations undertaken.
Myelodysplasia
The myelodysplastic syndromes (MDS) are rare haematological disorders of the myeloid cell lineages. They have an incidence of 4:100,000, are heterogeneic in nature and thought to be part of the same spectrum of disorders that give rise to acute myeloid leukaemia (AML). Previously called ‘preleukemia’, MDS has been diagnosed following persistent herpes labialis, severe oral mucosal ulceration and unexplained or spontaneous gingival bleeding, which was inconsistent with plaque levels (Chapple et al, 1999). The incidence of MDS appears to be increasing, and due to the high mortality rates associated with this group of disorders, it is important that the dental surgeon, who may be the first person to whom patients with MDS present, is aware of this group of disorders. Presentation is normally in patients over 60 years of age.
Clotting Factor Deficiencies
Clotting factor deficiencies that may give rise to excessive gingival bleeding include:
-
Von-Willebrand Factor deficiency (important for platelet adhesion).
-
Factor II.
-
Factor VII.
-
Factor VIII (haemophilia). Many haemophiliacs now self-manage by injection of recombinant factor VIII.
-
Factor IX (congenital factor IX disease, also called Christmas disease or haemophilia B).
-
Factor X.
-
Factor XII deficiency (Hageman factor).
Idiopathic Thrombocytopenic Purpura (ITP)
ITP is a chronic autoimmune condition of insidious onset without any identifiable or associated illness. It is a chronic condition that typically affects young and middle aged adults, with a female: male ratio of 3:1. In 30% of adults it is persistent and appears resistant to most forms of treatment. The pathogenesis involves increased platelet destruction by autoantibodies to platelet membrane antigens (glycoprotein 11b/111a).
Platelet Pool Storage Disease
This is a mild congenital bleeding disorder, generally managed by Desmopressin acetate (DDAVP) medication. It is associated with:
-
Glanzmann’s thrombasthenia – a condition caused by lack of a protein required for platelet aggregation, bleeding might be severe.
-
Bernard-Soulier syndrome – a congenital disorder where platelets lack receptors to adhere to vessel walls. Bleeding may also be severe with this disorder.
Acute Leukaemia
This is discussed in Chapter 8.
Chronic Leukaemia
See Chapter 8.
Thrombocytopaenia
Thrombocytopaenia is by definition a platelet deficiency, the defining level being <150,000 platelets per ml of blood. In clinical terms, control of haemorrhage does not normally become a problem in non-surgical periodontal therapy unless platelet levels fall below 60,000 per ml. There may be many underlying causes of thrombocytopaenia and these include:
-
Advanced liver disease.
-
HIV-associated thrombocytopaenia.
-
Secondary to immunosuppressant and cytotoxic drugs.
-
Idiopathic thrombocytopaenic purpura (ITP).
-
Platelet pool storage disease.
-
Other auto-immune diseases.
-
Wiskott-Aldrich syndrome.
Aplastic Anaemia
This is a rare condition that is associated with reduced haemopoetic tissue and a pancytopaenia. Gingival bleeding and advanced periodontal bone loss have been reported.
Thrombasthenia
See Glanzmann’s thrombasthenia above.
Patients on Warfarin
Warfarin is the most commonly employed anticoagulant used in patients with a history of:
-
Cerebro-vascular accident (stroke).
-
Myocardial infarction.
-
Thyrotoxicosis with associated cardiac arrhythmias.
Warfarin is a competitive antagonist of vitamin K, which is required for the production in the liver of Factors II, VII, IX and X. These factors are utilised in the coagulation cascade. Warfarin affects the prothrombin time (a measure of the extrinsic coagulation pathway), which is measured in a standardised way as the International Normalised Ratio (INR). An INR of 1.0 is normal, but an increasing ratio is associated with reduced coagulation. A growing body of opinion suggests that provided the INR is ≤ 4 and, local haemostatic measures are employed, periodontal and minor oral surgical procedures can be carried out with minimal post-operative haemorrhage. It is, therefore, less likely that warfarin doses may need to be adjusted in such patients. However, certain drugs may potentiate the action of warfarin and these include:
-
Penicillin V.
-
Amoxicillin.
-
Miconazole (including topical applications).
-
Erythromycin.
-
Metronidazole.
-
Fluconazole.
If bleeding does not respond to local measures in patients taking warfarin, the use of tranexamic acid is recommended. Tranexamic acid is a non-physiological inhibitor of fibrinolysis and an extremely effective haemostatic agent when used as a mouthwash (5%, 10mls as a rinse for two minutes and then spit out). It can be used four times daily for five to seven days, but avoid food and drink for one hour after rinsing.
Para-Gingival Swellings
Osteomas
Clinical appearance
-
Solitary or multiple well-circumscribed swellings (Fig 11-1).
-
Bony hard.
-
Surface epithelium is intact (no ulceration).
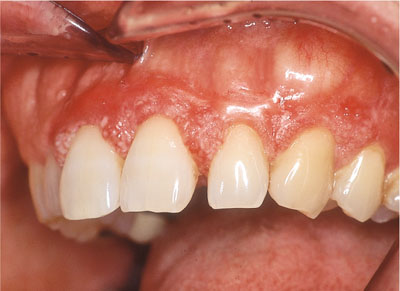
Fig 11-1 Well circumscribed benign osteoma affecting the UL3 region.
Clinical symptoms
-
Painless swelling.
Aetiology
These are benign slow growing tumours of mature bone, usually diagnosed in adult life.
Involvement of non-gingival sites
Multiple osteomas of the jaw are a feature of Gardner’s syndrome, a rare autosomal dominant condition. The syndrome also includes:
-
Polyposis coli (high incidence of malignant transformation).
-
Sebaceous cysts of the skin.
-
Multiple fibrous tumours of skin.
-
Multiple supernumerary teeth.
-
Multiple impacted permanent teeth.
Differential diagnosis
-
Torus palatinus or mandibularis.
-
Osteoblastoma.
-
Osteochondroma (usually in children).
-
Ossifying fibroma.
-
Ameloblastoma.
-
Fibrosarcoma.
Clinical investigation
-
Radiology.
-
Biopsy.
Management
No treatment unless aesthetic or functional problems have arisen due to the size of the osteoma. In the latter case, surgical re-contouring may be indicated.
Gardner’s Syndrome
See above.
Mandibular Tori
Tori are examples of bony ‘exostoses’, which are benign outgrowths of bone. Normally tori are developmental but they may arise following chronic stimulation as reactive exostoses. The torus palatinus clasically arises in the midline of the palate and the torus mandibularis arises lingual to the mandibular premolar teeth (Fig 11-2). No treatment is indicated unless pre-prosthetic surgery is deemed necessary.
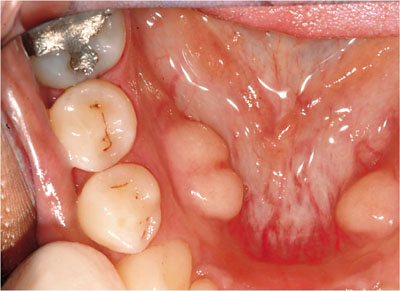
Fig 11-2 Classical mandibular tori.
Annular Lesions
Erythema Migrans
Clinical appearance
Erythema migrans may arise in several oral mucosal sites, but usually involves the tongue, where prevalence figures are approximately 2% (Fig 11-3). The term describes red patches, said to look like a map, which vary in size and location, often with a yellow margin surrounding areas of depapillation.
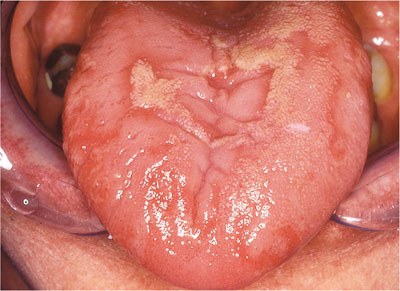
Fig 11-3 Erythema migrans.
Clinical symptoms
-
Usually asymptomatic.
-
Soreness of the tongue, especially with salty or spicy foods.
- />
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


