CHAPTER 10 Surgical Procedures
Introduction
As a dental nurse, you must have the knowledge and understanding of the procedures required to:
The dental nurse may assist the clinician undertaking dento-alveolar surgery, which may involve:
Consent
An example of a patient information sheet is given in Box 10.1. To read more about patient consent, see Subchapter 3.2.
Surgical procedures
Soft Tissue Surgery
A range of instruments are used for soft tissue surgery.
The disposable surgical scalpel blades used are:
Mucoperiosteum: the combined term for the mucous membrane and the periosteum that covers the bone (see Subchapter 4.1).
Cutting diathermy and electrosurgery
These procedures should be avoided in patients with artificial cardiac pacemakers.
Artificial cardiac pacemaker: this is a medical device that regulates the heart beat. It is placed in people whose natural heart beat is not fast enough or in those who have a problem with the system that conducts the heart beat from the atria to the ventricles (see Subchapter 4.1). The pacemaker consists of electrodes that are placed in contact with the heart muscles and which send out electrical signals to the heart.
Cryosurgery
This procedure uses freezing to destroy tissue.
Indications
Laser surgery
Lasers can be used for surgery but can also damage normal tissues, especially the eyes. The hard laser, especially the carbon dioxide laser, is the most useful (see Subchapter 1.1).
Surgery Involving Hard Tissues (Bone and Teeth)
Bone and teeth are usually cut with rotating instruments (burs) in a surgical handpiece. This involves the production of heat, so simultaneous cooling by constant running sterile water or sterile saline (irrigation) is important. Air-rotors are less commonly used as they can contaminate wounds unless using a sterile coolant, and occasionally cause surgical emphysema (see Chapter 16). Laser and ultrasonic cutting are uncommonly used. Piezosurgery is a new but expensive technique that cuts only hard tissues, increasingly used in apical and implant surgery as the danger of damage to nerves or arteries or the sinus membrane is less. However, this kind of surgery can generate significant heat, and cutting is slower than with many high-speed drills.
Wound Closure
Incisions are usually an integral part of surgery. The wound thus created needs to be closed so that it heals by primary intention. The would is closed usually with cyanoacrylate tissue adhesive or tapes (e.g. Steri-Strip), or sutures (stitches) (Box 10.2). This results in a small line of scar tissue, which is the goal whenever a wound is closed. In some circumstances, an open wound is left to heal by secondary intention. In the mouth it is then protected by a dressing such as Coepak. Wounds in bone are sometimes protected by BIPP (bismuth iodoform paraffin paste), or Whitehead’s varnish (compound iodoform paint).
BOX 10.2 Closing a Wound
Skin Tapes
Sutures
Technique
Surgical operations: safeguards
Operating on the Wrong Patient
Prevention
Operating on the Wrong Side or Area
Causes
Prevention
The role of a dental nurse in oral surgery
Before the Procedure
| Instrument | Purpose |
|---|---|
| Scalpel blade (Nos 11,12,15) | To cut the flap |
| Scalpel handle (e.g. Swann Morton) | |
| Mitchell’s trimmer | To raise the flap |
| Periosteal elevator (e.g. Howarth’s) | To raise the flap and protect soft tissues |
| Surgical handpiece | To remove bone or cut tooth |
| Surgical selection of burs | |
| Retractors: flap; cheek; tongue | To retract flap for visibility to operative site, and protect tissues |
| Surgical aspirator | To remove saliva, blood, water and debris |
| Irrigation syringe | To irrigate the site with sterile saline or water |
| Suture | To reposition and fix mucoperiosteal flap |
| Needle holders | To hold the suture needle |
| Rat-toothed tissue dissecting forceps | To hold the flap while suturing |
| Suture scissors | To cut sutures |
| Gauze swabs | |
| Cotton wool rolls |
Extraction of teeth (exodontia)
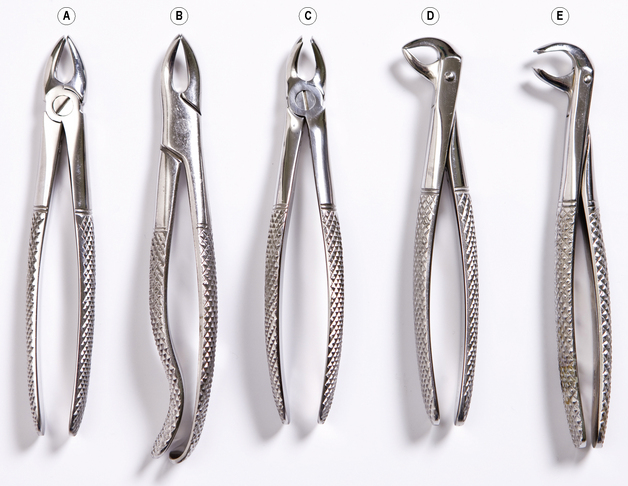
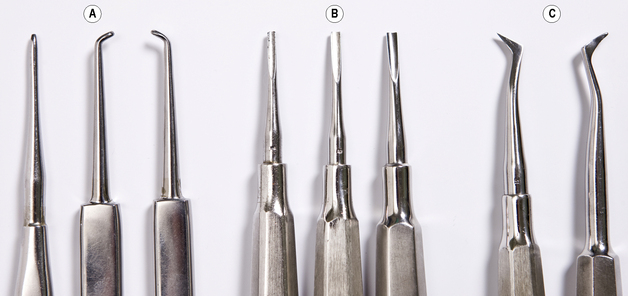
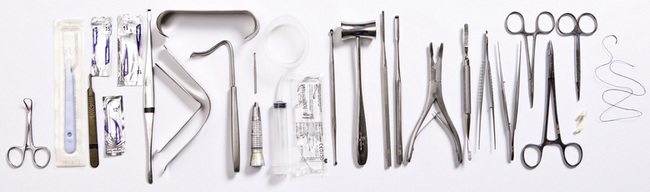
Instruments Used
Figures 10.1–10.3 show a selection of forceps and elevators used for extraction of teeth, both straightforward and impacted teeth. Figure 10.4 shows a selection of other surgical instruments.
Extraction of Deciduous Teeth
There is seldom a case for the removal of only one deciduous tooth, unless it:
Extraction of Permanent Teeth
Checks Required Before Extraction of a Tooth
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses