Chapter 10 Metal–ceramic crowns
Indications for metal–ceramic full coverage crowns
If a tooth requires a full coverage indirect restoration and there is a need for an aesthetic restoration, a metal–ceramic crown can be considered. However, all-ceramic restorations may be more appropriate in patients with extremely high aesthetic demands and these are increasingly being used by some clinicians. There are also special circumstances that require specific modifications to the standard metal–ceramic crown detailed throughout this chapter. Metal–ceramic restorations can be waxed-up or milled to provide space for a movable component of a fixed prosthesis (Figure 10.1; see also Chapter 19) or a rest for a removable partial denture (see Chapter 8). These must not be confined to ceramic as this can lead to catastrophic fracture and failure. In addition, guide planes and undercuts to aid the retention of a removable prosthesis can be incorporated into the restoration.
Metal–ceramic full coverage crowns
Metal–ceramic crowns consist of:
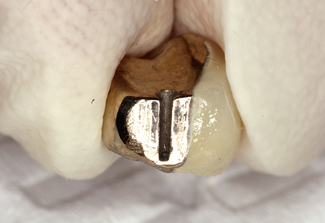
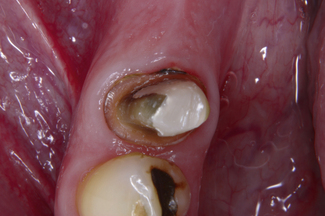
The rationale for this restoration is to combine the strength of a metal substructure with the aesthetic qualities of dental porcelain. However, tooth preparation for a full coverage metal–ceramic restoration is destructive of tooth substance (Figure 10.3) as clearance needs to be created not only for the metal but also for the opaceous ceramic and the dentine and enamel effect veneering ceramics. To provide sufficient strength the metal substructure should normally be between 0.3 and 0.7 mm thick; ideally this should be at least 0.5 mm thick with a greater thickness on the occlusal surface.
The metals
The metal–ceramic bond
The ceramic
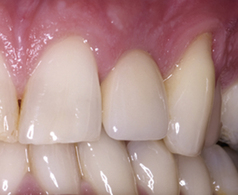
The types of dental porcelain available are discussed in Chapter 11 and are used to provide the aesthetic component of these restorations. Usually glass ceramics are used for metal–ceramic restorations; these ceramics must be thermally compatible with the specific alloy being used. The difference in coefficient of thermal expansion between the ceramic and metal is important; if the difference is too great, stresses will be introduced into the ceramic, leading to crazing, cracking and ceramic fracture. Ideally, the coefficient of thermal expansion of the metal should be slightly higher than that of the ceramic (see compression bonding above). The thickness of the veneering ceramic should allow the dental technician to match the colour of the restoration to the desired shade (Figure 10.4). However, it should not be more than about 1 mm thick as the ceramic has a relatively low flexural strength and may fracture if not adequately supported by the metal framework, although newer ceramics have improved physical properties.
Advantages of metal–ceramic full coverage crowns
Disadvantages of metal–ceramic full coverage crowns
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses