Chapter 10
Business Implications
Aims
The aims of this chapter are to consider the impact of quality in the context of the business of dentistry.
Outcome
The reader should appreciate the business benefits of implementing quality improvements in general dental practice.
Introduction
General practice is a business enterprise that has identified a need and organises internal and external resources to meet that need in a clinically effective and ethically sound manner. Profitability is one indicator of how well the task has been carried out. Inherent in this is the need to understand the requirements of the patient and to have available the range of clinical products, techniques, facilities and services to meet those requirements.
These should be delivered in a consistent way, preferably exceeding patient expectations. Patient satisfaction is part of a cyclic process that is summarised in Fig 10-1.
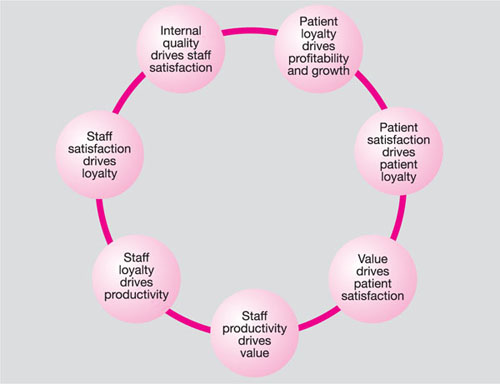
Fig 10-1 The multi-linkages of the service-profit chain.
Delivering Value
It was Walter A. Shewhart, the originator of the PDCA cycle, as discussed in Chapter 5, who noted that: “Price has no meaning without a measure of the quality being purchased.”
Quality and cost are intimately related and value is the combination of the quality of a product and the cost at which that level of quality is achieved (Fig 10-2, Fig 10-3).
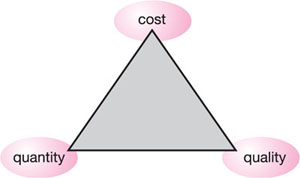
Fig 10-2 Value for money triangle.
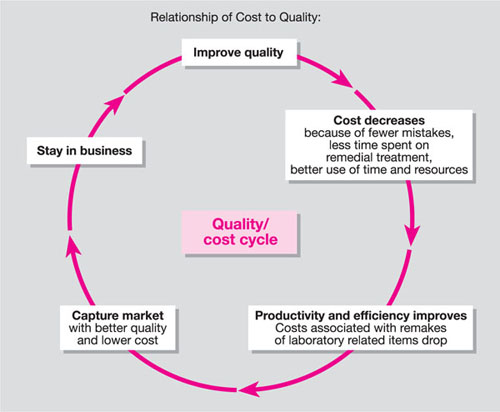
Fig 10-3 The relationship of cost to quality. Adapted from: W. Edwards Deming. Out of the Crisis: Relationship of Cost to Quality. MIT press, 1986.
We have established in earlier chapters that it is difficult for patients to measure the technical quality, and that patients will rely on indicators which will assist them in evaluating that quality.
In discussing the cost and quality of clinical treatments with our patients, we frequently refer to content quality. From this technical/content perspective, high value clinical care results from the most efficient expenditure of resources to achieve an established high level of clinical quality. Also, most dentists would agree that to achieve higher quality would often involve incurring additional costs – laboratory fees being just one example.
CQI theory takes a different, somewhat counter-intuitive argument that suggests that high quality can result in lower costs, within certain limits. To illustrate the principal, we need to review five areas:
-
Quality waste.
-
Productivity.
-
Maximalism versus optimalism in the face of limited resources.
-
The effect of improving the best clinical outcome that can be achieved through the application of new technology, new medications, or new techniques.
-
Lifestyle factors and the role of preventive dentistry.
Quality Waste
Low quality results when a process fails. For example, a failure in the process of recording an accurate impression of teeth prepared to receive a conventional bridge will result in an ill-fitting fixed prosthesis. The outcome brings with it a series of high costs. This bridge must now be discarded and all of the resources that went into its fabrication – in the practice and in the laboratory – are wasted. The process of impression taking may have failed for a number of reasons – Ishikawa’s cause and effect diagram is a useful tool here – but one reason may be the difficulty of obtaining a homogenous mix of the impression material.
We need to ask some key questions:
-
Who pays for the discarded bridge?
-
Additional resources must be allocated to correct the deficiency. Who pays for the new work?
-
The patient may be dissatisfied with the outcome and may elect to have the treatment elsewhere. What is the cost to the reputation of the practice of a dissatisfied patient? It costs far more to attract a new patient than it costs to retain an existing one.
-
What has been the cost of the time that must be spent on dealing with the dissatisfied patient and further discussions with the laboratory?
The conclusion is self-evident – a low quality process has led directly to higher end costs. Philip Crosby describes this as quality waste; it represents the resources that are consumed when the output fails to meet quality expectations. The cost of poor quality is discussed in more detail later in this chapter.
Productivity
Low productivity occurs when an alternative approach will achieve the same quality using fewer resources. It differs from maximalism which achieves higher quality but at an increasingly unfavourable cost.
Optimalism and Maximalism
There are occasions in clinical practice where gains in quality may not justify the increase in practice resources both from a patient and practitioner perspective. If this is the case, clinicians will attempt to achieve an optimal level of quality for the resources consumed – which may be measured in terms of the price to the patient. In other words, they will try and maximise value, but may not achieve the ultimate quality outcome. This is optimalism and is a necessary approach when resources are finite.
From an ethical standpoint, healthcare professionals should not be placed in the position of limiting content quality on the basis of cost. Many, if not all, dentists would welcome an environment where the best possible/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


