Chapter 1
The First Step: the Endodontic Treatment
Aim
To describe the principles of root canal treatment and their impact on the subsequent restoration of the tooth.
Outcome
After reading this chapter, the reader should have a clearer understanding of the role of microbial infection in periapical disease, the rationale for each stage of root canal treatment, and the importance of a suitable post-endodontic restoration. The reader should also appreciate the impact of each stage of root canal treatment on the subsequent restoration of the tooth.
Introduction
The purpose of root canal treatment is to prevent apical periodontitis in teeth with irreversible pulpitis and to heal apical periodontitis in teeth with infected, necrotic pulp spaces. Root canal treatment allows teeth to remain in healthy, pain-free function in the dental arch, and to justify confidence and expenditure in respect of a definitive long-term restoration.
The dentine-pulp complex is protected by a hard, impermeable outer casing of enamel. Once these barriers are breached by, for example, caries, operative dentistry, tooth surface loss or trauma, the underlying permeable dentine-pulp complex becomes susceptible to microbial, chemical and/or physical injury. Injury may occur as a result of noxious stimuli reaching the pulp indirectly via patent dentinal tubules, or directly if the pulp becomes exposed to the mouth. The pulp tissue within the root canal space will become inflamed and ultimately necrotic, allowing microbial infection to progress. Eventually, this will lead to the development of periapical disease.
Patients with pain of dental origin may present with signs of pulpitis or apical periodontitis. Once a diagnosis of irreversible pulpitis or apical periodontitis has been made, the tooth should be assessed according to the guidelines in Chapter 8, and the treatment options of extraction versus root canal treatment and subsequent restoration discussed with the patient. When discussing treatment options, it is essential to advise that root canal treatment is not an end in itself, and that post-endodontic restorative treatment will be required to restore the tooth back to function and aesthetics. It should be stressed that the timing, nature and quality of the coronal restoration may have a critical bearing on endodontic success and tooth survival. Only then can an informed decision be made on the most suitable treatment for the tooth in question.
Stages of Root Canal Treatment
Root canal treatment can be broken down into stages:
-
preoperative assessment and preparation
-
preparation of the pulp space (including access and instrumentation/ disinfection)
-
sealing the pulp space
-
provision of a sealing and protective coronal restoration.
Restoration should be considered as an integral element in the package of endodontic care.
The prognosis of endodontic treatment is dependent on a systematic approach. Each stage must be successfully completed before embarking on the next if consistently predictable results are to be achieved.
Preoperative Assessment and Preparation
Once the diagnosis has been confirmed, it is essential that the prognosis of the tooth is determined. Restorability must first be established, taking into account both the quantity, quality and location of coronal tissue, and the periodontal status. Carefully “walking” a periodontal probe around the gingival margin of the tooth will highlight the presence of significant features such as vertical fractures, which may have a serious impact on restorability and treatment planning. It is common for teeth that require endodontic treatment to be heavily restored or broken down and infected. Caries must be removed to prevent leakage and minimise the risk of microbe-laden carious dentine entering the root canal space during treatment (Fig 1-1).
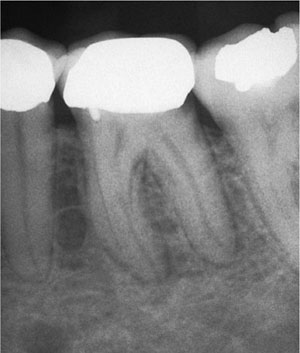
Fig 1-1 Radiographic signs of caries at the distal margin of a lower molar crown. The crown must be removed to fully excavate caries and assess restorability before root canal treatment can commence.
Ideally, there should be a minimum of 2 mm of sound supragingival tooth tissue around the circumference of the tooth for subsequent restoration with a cuspal coverage restoration (Fig 1-2). If there is any doubt in respect to the prosthodontic restorability (see Chapter 8), the existing restoration should be completely removed to reveal the extent and location of residual sound tooth tissue (Fig 1-3). It is essential to inform the patient and secure their consent prior to embarking on this type of exploratory treatment. If the tooth is found to be unrestorable, an informed decision should be made to extract rather than attempt a heroic restoration.
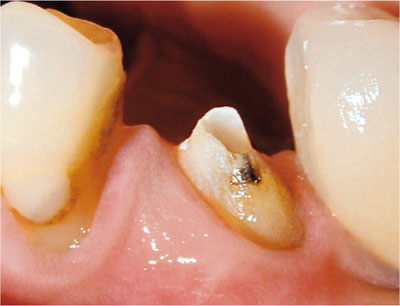
Fig 1-2 At least 2 mm of supragingival coronal tooth tissue should be present on all tooth surfaces for optimal restorative prognosis after root canal treatment.
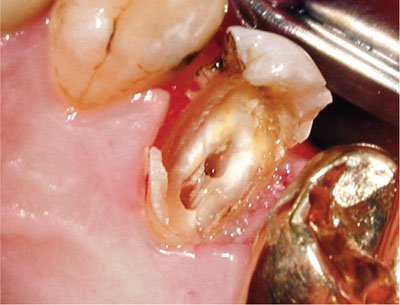
Fig 1-3 Removal of the failing restoration and caries revealed that this premolar tooth was unrestorable. It was extracted and replaced with an implant.
Complete removal of the existing restoration is advisable in a range of circumstances. This may reveal hidden fracture lines, which may not have been identified by external examination or periodontal probing (Fig 1-4).
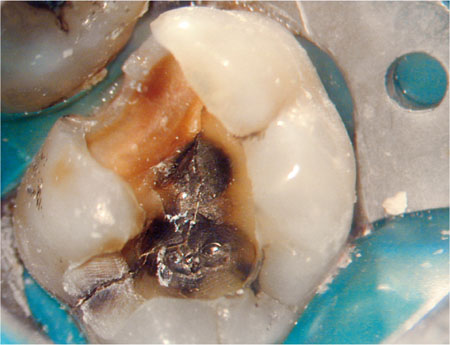
Fig 1-4 Fracture lines indicating that this tooth will require a cuspal coverage restoration very soon after endodontic treatment.
Such careful exploration may be time and effort well spent, determining not only the restorability of a tooth but also:
-
The type and design of the post-endodontic restoration required.
-
How soon after endodontic treatment a definitive restoration should be placed.
-
Whether cusp reduction, the placement of a well-fitting copper ring, orthodontic band or a provisional crown is required to prevent cuspal fracture during and immediately after root canal treatment (Fig 1-5). Extracoronal support of this sort may also be required to allow a secure, well-sealing rubber dam to be placed.
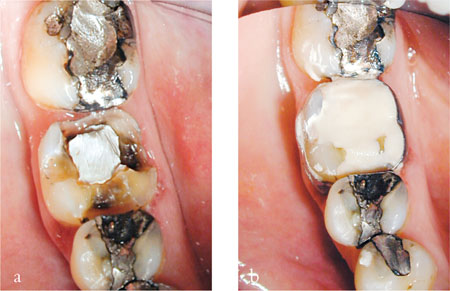
Fig 1-5 (a) Restorations in this lower molar tooth have been removed. (b) The remaining buccal cusps have been braced with an orthodontic band filled with a glass-ionomer cement.
Crowns must be removed prior to root canal treatment if significant coronal leakage or caries are suspected, or are detected once the tooth is accessed (Fig 1-6a). Root canal treatment can be more challenging if a decision is made to access the pulp through a crown, as the anatomical landmarks of the tooth may be masked by the extracoronal restoration. This may lead to difficulties in identifying the root canal entrances, the inadvertent removal of excessive sound dentine (Fig 1-6b) or even perforation. In all of these situations, the risks should be assessed and an informed decision made to remove the crown before treatment is commenced.
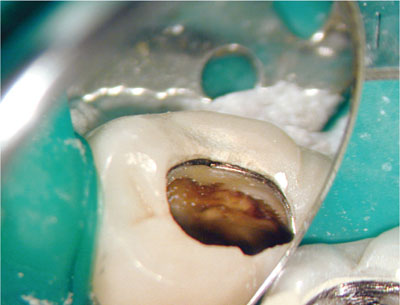
Fig 1-6 (a) Access cavity preparation in this lower molar has revealed a significant amount of caries which was not detected on preoperative radiographs. The crown must be removed for caries excavation and assessment of restorability.
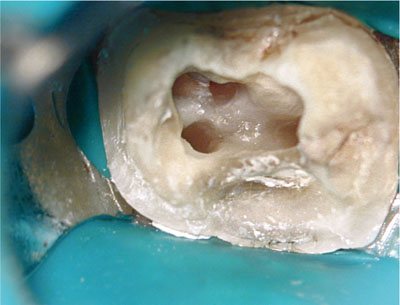
Fig 1-6 (b) Removal of existing crowns assists in the location and preparation of canals.
Even if, as a consequence, a decision is made to work through a crown, it is always wise to advise the patient that circumstances may dictate that the crown is removed during treatment and that a new crown may be required once the treatment has been completed.
Endodontic treatment must be carried out under a rubber dam (Box 1-1) (Fig 1-7). Good illumination and the use of magnification are essential to carry out root canal treatment to a consistently high standard. Similar conditions are also required for the stages of restoration using an adhesive approach.
Box 1-1 Functions of a rubber dam
Protects the patient from risks of swallowing or inhalation of endodontic instruments and materials.
Eliminates bacterial contamination of the root canal space from saliva.
Prevents leakage of irrigants into the oral cavity.
Improves visibility for operator by retraction of soft tissues (cheek, tongue).
Improves comfort for patients.
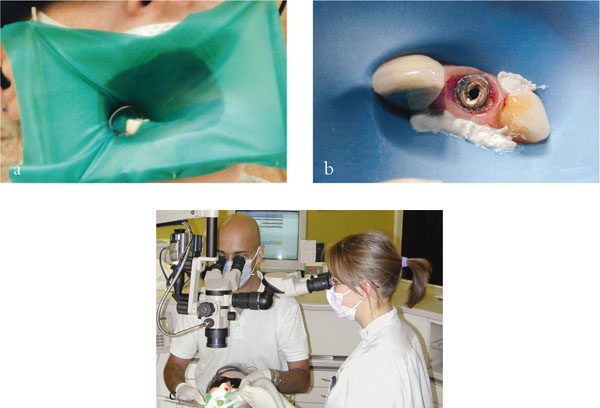
Fig 1-7 (a) A rubber dam is mandatory when carrying out endodontic treatment. (b) The split dam technique may be used to isolate teeth which cannot be easily isolated, OraSeal© is used to plug any gaps between the gingivae and rubber dam. (c) Good illumination and the use of magnification are essential.
Preparation of the Root Canal Space
Preparation of the root canal space can be divided into two stages; firstly, access cavity preparation and, secondly, instrumentation and disinfection of the root canal space.
Access cavity preparation
The aim of access cavity preparation is to identify the root canal entrances for subsequent instrumentation and disinfection of the root canal space. Access cavity preparation can be one of the most challenging and frustrating aspects of endodontic treatment, but it is the key to successful treatment. Inadequate access may complicate canal location and negotiation, and impact on the prognosis by compromising debridement, disinfection and sealing of the root canal space. It may contribute also to instrument separation and canal aberrations (e.g. transportation and ledging), which may impair infection control and ultimately lead to treatment failure.
It is unusual for access cavities to follow precisely the classic outline forms of young, previously unrestored teeth, as commonly illustrated in endodontic textbooks. The dimensions of the pulp chamber and location of the root canal entrances will be influenced by the amount and position of secondary and tertiary dentine deposition in response to caries, restoration, leakage and tooth surface loss over the course of a tooth’s life. These cumulative insults may have a dramatic, and not necessarily chronological effect, on the size and shape of the pulp chamber (Fig 1-8a–c).
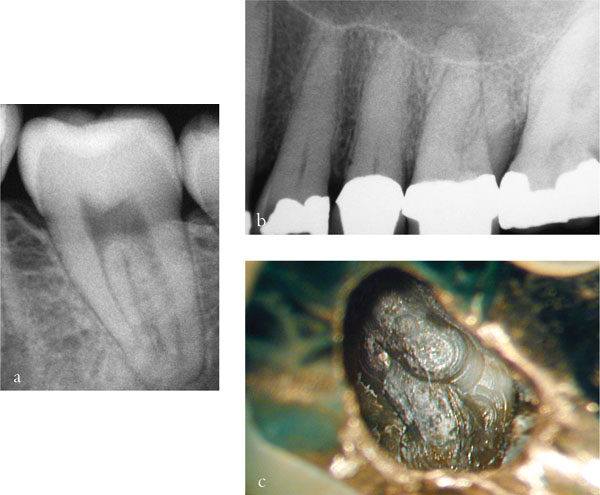
Fig 1-8 (a) Full exposure of the pulp chamber and patent canals should result in uncomplicated negotiation and preparation.
(b) The pulp chamber and canals of the upper left first permanent molar appear to be completely sclerosed.
(c) Removal of the crown may improve the likelihood of identifying canal entrances.
The objectives of access cavity preparation are to:
-
remove the entire roof of the pulp chamber to allow the coronal pulp tissue to be eliminated
-
produce a smooth-walled preparation with no dentine overhangs
-
prevent damage to the floor of the pulp chamber
-
allow straight-line access of instruments into the main root canals
-
preserve as much sound coronal tooth tissue as possible within the constraints presented by the other objectives (Fig 1-9).
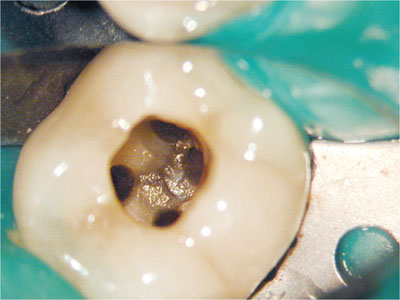
Fig 1-9 Minimally prepared access.
Instrumentation and disinfection of the root canal space
The aims of this stage of endodontic treatment are to:
-
debride and disinfect the root canal space
-
prepare a suitable root canal shape for subsequent three-dimensional sealing (obturation) with root filling material
-
preserve as much structurally important tooth tissue as possible, consistent with the other factors.
Micro-organisms exist both within the main root canal space and in a biofilm coating the complex ramifications of the root canal. The operator can rarely see, let alone enter and fully debride the root canal space with instruments (Fig 1-10). Instrumentation (debridement) removes material from some areas of the root canal wall and opens up the pulp space with its ramifications for deep exchange of antimicrobial irrigants and medicaments (disinfection). Instrumentation should create a root canal which is three-dimensionally tapered from apex to coronal entrance, and follows closely the outline of the root surface. This taper will facilitate the eventual sealing (obturation) of the root canal space.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


